Armamentarium
|
History of the Procedure
The great golden age anatomist Galen was uncertain of the role of peripheral nerves and initially did not distinguish them from tendons. Subsequently he sectioned the recurring laryngeal nerve in pigs to demonstrate peripheral nerve action. Injuries to peripheral nerves were poorly understood due to the nondiscrete nature of these injuries. However, in his 1795 treatise, John Haighton reported that “an animate machine differs from an inanimate one in nothing more conspicuously than in its power of repairing its injuries.” He identified the need for peripheral nerve continuity to preserve diaphragmatic function. His experiments on dogs, apparently after division of the vagus nerve in the neck (although he called it the VIII nerve), demonstrate the apparent ability of peripheral cranial nerves to undergo repair. He sectioned one side, both sides, and both sides in sequence over weeks to demonstrate not only the action of the peripheral nerve, but also its ability to undergo repair. His drawings of dissections completed in functionally restored animals demonstrate the spontaneous repair of peripheral nerves.
The first description of technique for reanastomosis of peripheral nerve neurotmesis is likely that of Gabriel Ferrara of Venice in 1608. The first successful modern peripheral nerve repairs were performed during hand surgery for traumatic neurotmesis. In 1973 Millesi emphasized the importance of fascicular alignment and perineural suturing to achieve favorable results in hand surgery. The results of hand surgery demonstrated the proof of motor and sensory recovery after neurotmesis could be obtained in humans.
Modern peripheral trigeminal nerve surgery was hampered by the development of access techniques and the irregular nature of referral for these sensory injuries which, compared to motor injuries of the hand, did not create as much disability for most. However, the presence of anesthesia dolorosa ineffectively treated with nerve ablation and the vexing issue of lingual nerve anesthesia and dysesthesia prompted surgeons in the 1970s to develop techniques for repair. Hausamen et al. demonstrated a technique for the inferior alveolar nerve with interpositional grafting. Phillip Worthington, Ralph Merrill, Bruce Donoff, Tony Pogrel, and John Gregg, among others, pioneered the advancement of these techniques in contemporary surgical practice. Today large outcome studies demonstrating functional sensory recovery have established the utility of direct repair and interpositional grafting of peripheral trigeminal nerve injuries.
History of the Procedure
The great golden age anatomist Galen was uncertain of the role of peripheral nerves and initially did not distinguish them from tendons. Subsequently he sectioned the recurring laryngeal nerve in pigs to demonstrate peripheral nerve action. Injuries to peripheral nerves were poorly understood due to the nondiscrete nature of these injuries. However, in his 1795 treatise, John Haighton reported that “an animate machine differs from an inanimate one in nothing more conspicuously than in its power of repairing its injuries.” He identified the need for peripheral nerve continuity to preserve diaphragmatic function. His experiments on dogs, apparently after division of the vagus nerve in the neck (although he called it the VIII nerve), demonstrate the apparent ability of peripheral cranial nerves to undergo repair. He sectioned one side, both sides, and both sides in sequence over weeks to demonstrate not only the action of the peripheral nerve, but also its ability to undergo repair. His drawings of dissections completed in functionally restored animals demonstrate the spontaneous repair of peripheral nerves.
The first description of technique for reanastomosis of peripheral nerve neurotmesis is likely that of Gabriel Ferrara of Venice in 1608. The first successful modern peripheral nerve repairs were performed during hand surgery for traumatic neurotmesis. In 1973 Millesi emphasized the importance of fascicular alignment and perineural suturing to achieve favorable results in hand surgery. The results of hand surgery demonstrated the proof of motor and sensory recovery after neurotmesis could be obtained in humans.
Modern peripheral trigeminal nerve surgery was hampered by the development of access techniques and the irregular nature of referral for these sensory injuries which, compared to motor injuries of the hand, did not create as much disability for most. However, the presence of anesthesia dolorosa ineffectively treated with nerve ablation and the vexing issue of lingual nerve anesthesia and dysesthesia prompted surgeons in the 1970s to develop techniques for repair. Hausamen et al. demonstrated a technique for the inferior alveolar nerve with interpositional grafting. Phillip Worthington, Ralph Merrill, Bruce Donoff, Tony Pogrel, and John Gregg, among others, pioneered the advancement of these techniques in contemporary surgical practice. Today large outcome studies demonstrating functional sensory recovery have established the utility of direct repair and interpositional grafting of peripheral trigeminal nerve injuries.
Indications for the Use of the Procedure
Peripheral trigeminal nerve injury can result from mechanical injury to the affected nerve after facial trauma or surgical intervention ( Figure 16-1 ). Mandible and zygomatico-orbital fractures commonly injure afferent V3 and V2, respectively. Removal of impacted mandibular third molars, mandibular fracture, mandibular tumors, and placement of dental implants commonly affect V3. In addition to mechanical injuries, chemical nerve injury of the trigeminal nerve results from endodontic medicaments, amide local anesthetics, and antiseptics such as alcohol. Thermal injury to the trigeminal nerve can occur from electrocautery, heat from rotary instruments, or warm gutta-percha ( Figure 16-2 ). Ischemic injury may occur due to endoneural injection of epinephrine, radiation therapy, or infarction of the peripheral nerve vas neurosum.
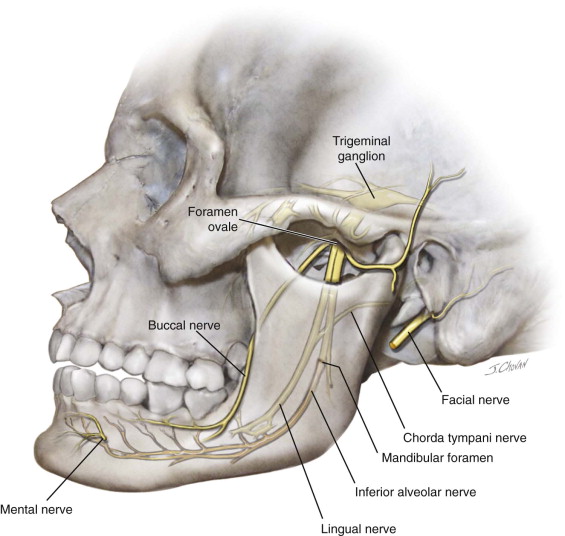
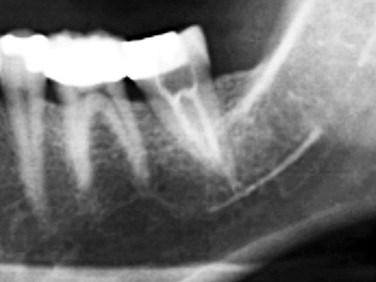
Injuries to the sensory branches of the trigeminal nerve result in afferent defects characterized by alterations or absence of sensation. The alterations in sensation can be noxious or painful, or they may be innocuous, with mild tingling or just dullness.
Neuropathic pain may be associated with peripheral nerve injuries of branches of the trigeminal nerve. All injuries to the sensory branches of the trigeminal nerve result in afferent defects characterized by alterations or absence of sensation. Although in many cases there is simply a diminution of sensation, these alterations in sensation can be noxious or painful. Surgical management of hypoesthesia or anesthesia is an established method, whereas procedures for dysesthesia are less well defined, and recommendations for surgical management have not been as well characterized.
Over the course of surgical and nonsurgical treatment, the improvement of patients to the point of elimination of pain applies only to a small minority. Despite these shortcomings, treatment is capable of reducing the impact of pain from an unbearable burden on the patient’s well-being to a tolerable condition with substantial improvements in quality of life. For patients with well-defined injuries and those with nociceptive inflammatory components, the prognosis is better yet with surgical intervention.
A variety of definitions of these conditions are used and are consistent with the characterization of neuropathic pain in a patient with a trigeminal nerve injury. The following definitions and clinical presentations are noted.
-
Hypoesthesia: A diminution of sensation, compared to a control stimulus, with the absence of pain. In such patients, sharp may feel dull. The patient produces errors in two-point and directional stimuli. No areas of anesthesia are present, and the findings are due either to decreased neural density (e.g., incomplete repair) without neurotmesis or to neuropraxia and thus are transient.
-
Anesthesia: The absence of sensation with the absence of pain to any stimulus. These patients often treat the anesthetic part as a foreign body (e.g., a bolus). Hypersalivation, dysarthria, dysphagia, and speech articulation issues, among others, are noted when the perception of an absent body part is noted. This typically is due to neurotmesis, which may be physical separation, neuroma in continuity, lateral adhesive neuroma, kinking of the nerve, or some other impingement or infarction of the nerve.
-
Elicited neuropathic pain:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


