Armamentarium
|
History of the Procedure
The development of the classic Le Fort I osteotomy used in orthognathic surgical correction of the maxilla evolved through the contributions of many surgeons. The first description of an osteotomy of the maxilla was published by von Langenbeck in 1859, and he used this approach to access nasopharyngeal polyps. In 1867, Cheever performed a bilateral hemimaxillary down-fracture known as the “double operation,” which resembled a Le Fort I osteotomy, to remove nasopharyngeal pathology. After Le Fort’s classic publication and description of the natural fracture lines of a maxillary fracture in 1901, Wassmund was the first to describe the classic Le Fort I operation in 1921, although he did not mobilize the osteotomy during the surgery, preferring to use orthopedic traction postoperatively. Auxhausen, in 1934, performed a complete Le Fort I osteotomy with intraoperative mobilization and repositioning for open-bite correction. Despite contributions from Schuchard, Moore and Ward, and Converse, difficulties with techniques for separation of the maxilla from the pterygoid plate region, bleeding, and relapse made predictable surgery difficult. Not until 1965, when Obwegeser suggested more complete mobilization and tension-free stabilization of the maxilla, did the routine use of the Le Fort I osteotomy fully evolve. The importance of orthodontic collaboration during treatment was recognized, and studies by Bell further defined stability, bone healing, and revascularization following Le Fort I osteotomy. With the introduction of plate osteosynthesis by Horster in 1980 and Drommer and Luhr in 1981, the operation evolved to become a routine surgery for dentofacial correction. Multiple nuances of the classic surgery have been described, but the basic principles of a viable vascular pedicle, complete mobilization, and stable fixation are paramount for success.
History of the Procedure
The development of the classic Le Fort I osteotomy used in orthognathic surgical correction of the maxilla evolved through the contributions of many surgeons. The first description of an osteotomy of the maxilla was published by von Langenbeck in 1859, and he used this approach to access nasopharyngeal polyps. In 1867, Cheever performed a bilateral hemimaxillary down-fracture known as the “double operation,” which resembled a Le Fort I osteotomy, to remove nasopharyngeal pathology. After Le Fort’s classic publication and description of the natural fracture lines of a maxillary fracture in 1901, Wassmund was the first to describe the classic Le Fort I operation in 1921, although he did not mobilize the osteotomy during the surgery, preferring to use orthopedic traction postoperatively. Auxhausen, in 1934, performed a complete Le Fort I osteotomy with intraoperative mobilization and repositioning for open-bite correction. Despite contributions from Schuchard, Moore and Ward, and Converse, difficulties with techniques for separation of the maxilla from the pterygoid plate region, bleeding, and relapse made predictable surgery difficult. Not until 1965, when Obwegeser suggested more complete mobilization and tension-free stabilization of the maxilla, did the routine use of the Le Fort I osteotomy fully evolve. The importance of orthodontic collaboration during treatment was recognized, and studies by Bell further defined stability, bone healing, and revascularization following Le Fort I osteotomy. With the introduction of plate osteosynthesis by Horster in 1980 and Drommer and Luhr in 1981, the operation evolved to become a routine surgery for dentofacial correction. Multiple nuances of the classic surgery have been described, but the basic principles of a viable vascular pedicle, complete mobilization, and stable fixation are paramount for success.
Indications for the Use of the Procedure
The Le Fort I osteotomy is indicated when repositioning of the maxilla will aid in the correction of hard or soft tissue deformities or functional disorders of the maxillofacial region. Dentofacial abnormalities of this region include maxillary deficiency, excess, malposition, or asymmetry, all of which can result in a broad range of functional issues including masticatory and swallowing difficulty, speech pathology, myofascial pain dysfunction (MPD), temporomandibular joint dysfunction (TMD), obstructive sleep apnea, malocclusion, dental/periodontal disease, and psychosocial issues.
Maxillary dentofacial disorders can generally be broken down into four diagnostic categories: horizontal, vertical, transverse, and combination abnormalities. Horizontal deficiencies most commonly involve maxillary horizontal hypoplasia and require advancement surgery. Vertical disorders of the maxilla may include both vertical hyperplasia and hypoplasia and require impaction or downward movement of the maxilla. Transverse disorders commonly include transverse deficiency, and less commonly transverse excess, requiring widening or narrowing of the maxilla. Combination maxillary disorders may occur in any plane and often have a corresponding disorder in the mandible. Apertognathia is frequently a combination deformity that presents with maxillary transverse deficiency, maxillary horizontal hypoplasia, and an anterior or posterior vertical abnormality.
Limitations and Contraindications
The stability of the osteotomized maxilla often depends on many factors including surgical technique, bone quality and contact, rigid fixation, and the severity of surgical repositioning. The previously operated maxilla may require an additional presurgical diagnostic workup to optimize clinical outcomes and prevent well-documented intraoperative or postoperative complications. Specific movements are known to have a higher degree of relapse (e.g., posterior maxillary downgrafting) than others. Ideal repositioning may be difficult to achieve in severe deformities. Aside from well-known general medical comorbidities (uncontrolled diabetes mellitus, immune compromise, bone and joint disease, etc.), specific contraindications of the Le Fort I osteotomy include uncontrolled periodontal disease, skeletal immaturity, and progressive dentofacial deformities, especially those with temporomandibular joint etiology (resorption or hyperplasia). A relative contraindication in the skeletally immature patient includes the Le Fort I osteotomy performed in a growing patient, in which anteroposterior (A-P) growth of the maxilla ceases postoperatively due to nasal septal separation from the upper jaw. Final A-P positioning must be estimated if surgery is performed in growing patients since vertical growth of the maxilla and A-P and vertical growth of the mandible continue postoperatively, possibly resulting in a secondary malocclusion.
Technique: Le Fort I Osteotomy
A standard nasoendotracheal intubation is indicated. The nasoendotracheal tube is stabilized with a head wrap, with the tube coming off the forehead region, away from the operative region. The patient is draped in a sterile fashion in a supine position, preferably in a reverse Trendelenburg position. Hypotensive anesthesia with the systolic blood pressure below 100 mm Hg is recommended.
Step 1:
Reference Point
Although some clinicians use internal markings, external reference markers have been shown to be more accurate. A stable extraoral reference point is established with a 0.035-inch K-wire placed in the nasion. The wire is drilled until stable or up to 1 cm in depth and then shortened to 3 to 4 mm above the skin surface. A caliper is used to measure the vertical distance from the K-wire to the brackets of the central incisor teeth, and these measurements are recorded. Adjustment of any dental prematurities noted during model surgery are made with a round diamond bur at this time.
Step 2:
Surgical Exposure
Local anesthesia with vasoconstrictor is infiltrated labially and buccally from the pterygoid plate region, forward to the midline bilaterally. A horizontal incision is made with a #15 blade or needle-tip electrocautery, extending from first molar to the contralateral first molar, 3 to 4 mm above the mucogingival junction. Retraction is maintained with down-turned Obwegeser retractors, and the superior mucoperiosteal flap is elevated with a #9 Molt periosteal elevator. The anterior nasal spine, piriform rim, infraorbital foramen, lateral maxillary wall, and zygomaticomaxillary junction are exposed. Exposure of the posterior maxillary wall and pterygomaxillary junction is next performed with a Molt periosteal elevator, placed parallel to the maxillary teeth and advanced posteriorly below periosteum until the pterygomaxillary junction is encountered. The nasal/septal mucosal dissection is performed after the bilateral maxillary osteotomies have been completed and involves elevation of the nasal mucosa with a curved freer elevator to the posterior palatine bone ( Figure 38-1 ).
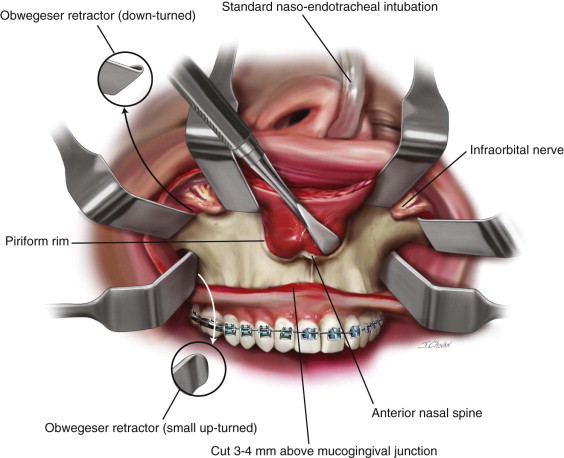
Step 3: Bony Osteotomies
Lateral Osteotomies
A 701 straight fissure bur or reciprocating saw creates the lateral maxillary osteotomy from the lateral nasal rim to the zygomatico-maxillary junction. The osteotomy starts 3 to 4 mm above the nasal floor and is carried to the depth of the maxillary sinus, back to the pterygomaxillary junction, approximately 30 to 35 mm above the bracket on the first molar tooth. Cuts are made at least 5 mm above the roots of the teeth and can be made higher as needed. A vertical step at the first molar is carried inferiorly for 5 to 10 mm (step osteotomy permits grafting in the zygomaticomaxillary buttress area subsequently, if required), and then it is continued in a horizontal plane to the posterior maxilla ending in front of the pterygomaxillary junction ( Figure 38-2, A ).
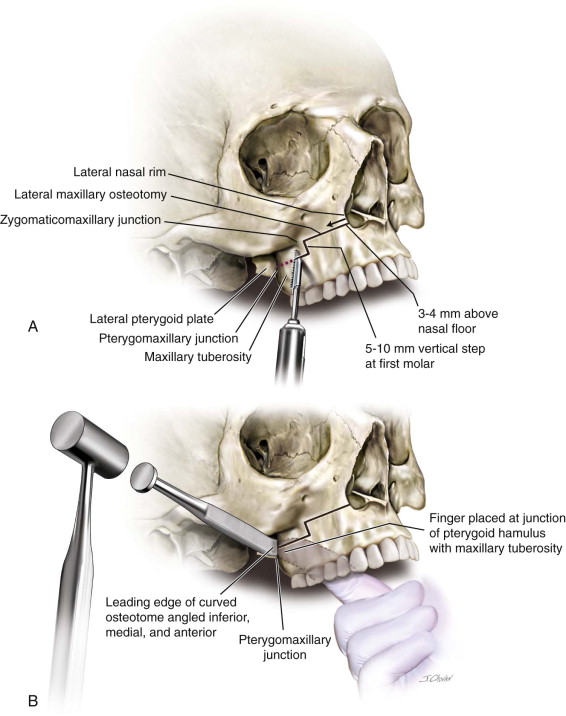
Pterygoid Plate Separation
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


