Armamentarium
|
History of the Procedure
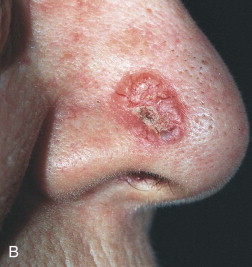
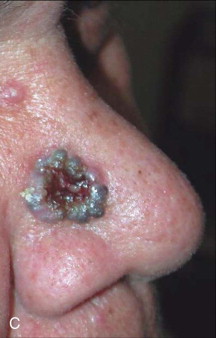
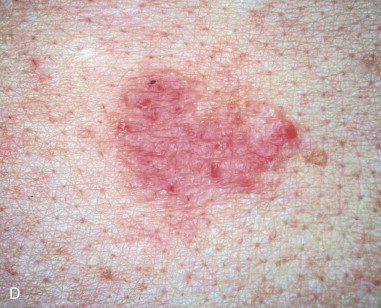
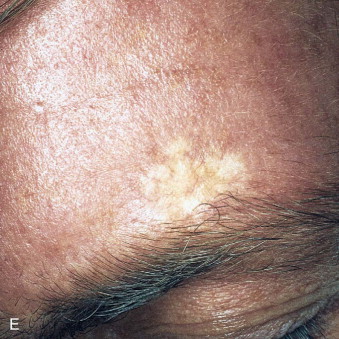
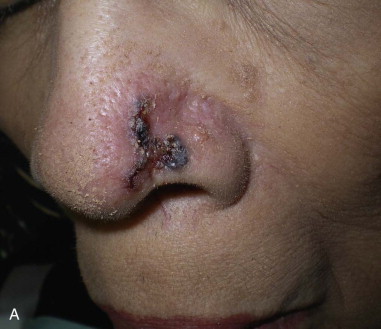
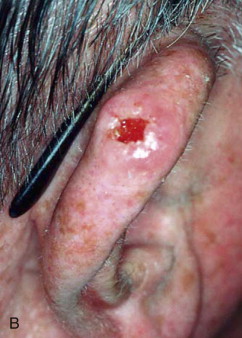
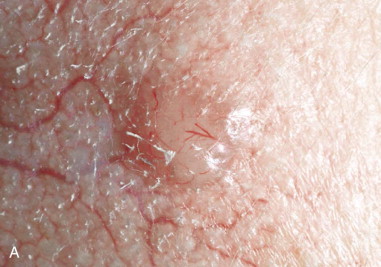
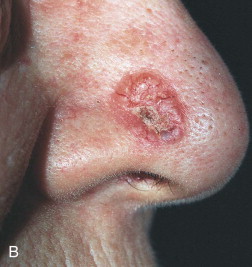
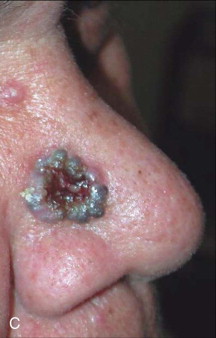
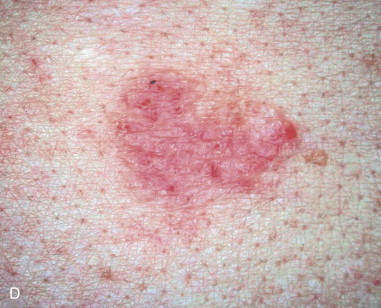
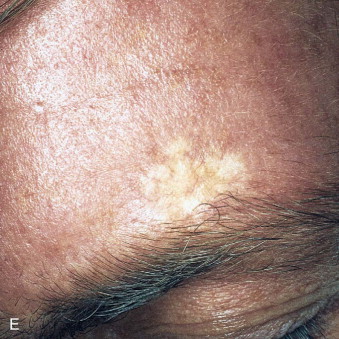
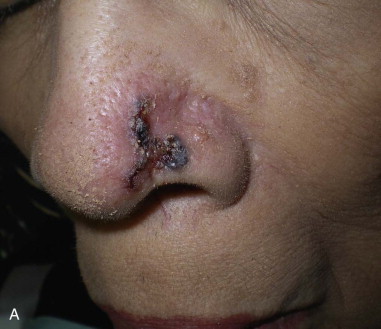
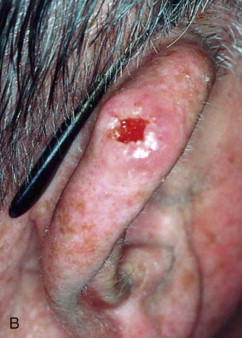
Skin cancer is the most common malignancy of humans, and its incidence continues to rise despite increased awareness of the disease among both practitioners and the general public. Nonmelanoma skin cancer (NMSC), primarily squamous cell carcinoma (SCC) and basal cell carcinoma (BCC), is estimated to account for nearly 2 million new cancer cases per year, representing 95% of all skin cancers ( Figures 94-1 and 94-2 ). The incidence of NMSC has been rising at a rate of 5% per year, and it is estimated that 1 in 6 Americans develop skin cancer during their lifetime. Although the incidence of NMSC is high, the 5-year survival remains above 95%, with most deaths occurring from metastatic SCC. The overall incidence of metastatic disease in BCC is very low (0.0028% to 0.1%); favored sites include regional lymph nodes, the liver, lungs, bone, and skin. SCC more frequently develops metastatic disease, with an overall rate of 2% to 6% for the primary lesion and 24% to 45% for recurrent SCC. The presence of metastatic disease reduces the 5-year survival rate to only 34%; therefore, complete removal of disease at the time of initial surgery is essential.
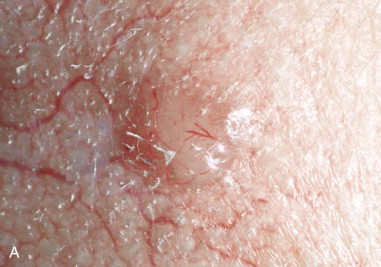
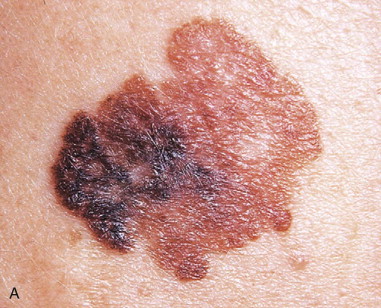
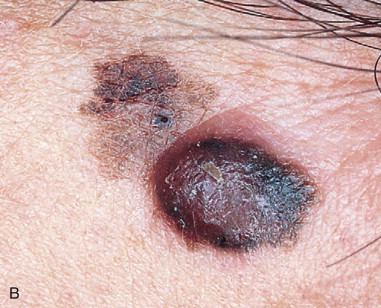
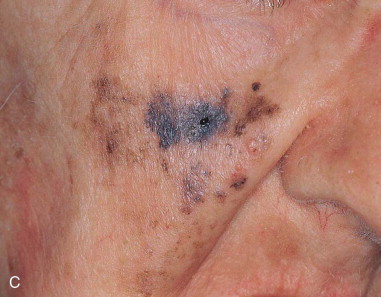
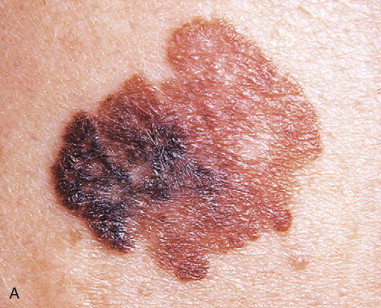
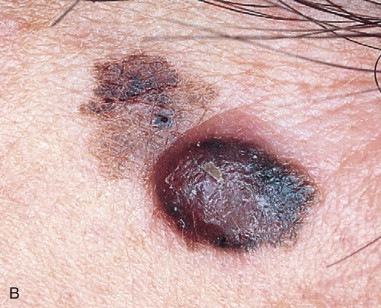
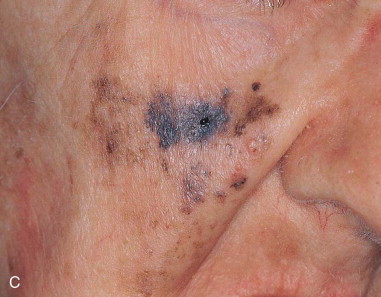
Melanoma accounts for 75% of skin cancer–related deaths, but for only 5% of all skin neoplasms ( Figure 94-3 ). Approximately 80,000 new cases of melanoma skin cancer are diagnosed per year in the United States, and the patient’s age at diagnosis is younger than for most cancers. This makes melanoma the most common cancer diagnosis in women 20 to 29 years of age.
Surgical excision of facial skin malignancy continues to be the gold standard treatment and is the procedure most often performed by oral and maxillofacial surgeons and other surgical specialists. Other treatment modalities, such as cryotherapy, curettage and electrodessication, Mohs micrographic surgery, and laser treatment are available, and when used for specific indications by individuals well trained in the technique, they have similar rates of success. It should be noted that not every technique can be used for all lesions in all patients, and factors such as the histologic diagnosis, lesion size, patient comorbidities, and lesion site play a role in treatment planning. Although this chapter focuses on the standard surgical excision of lesions, the discussion of this procedure would not be complete without mentioning alternative treatment modalities.
Standard surgical excision is the most common treatment modality among plastic, ear, nose, and throat, and oral and maxillofacial surgeons, and the cure rate ranges from 93% to 95%. Surgical excision is advantageous because it allows for tissue diagnosis and assessment of completion of excision through frozen sections (if used) and final specimen histologic analysis. In addition, the cosmetic outcome often is superior, regardless of whether immediate or delayed closure is performed, especially for lesions amenable to primary closure. Excision is also the standard technique for removal of cutaneous melanomas, because Mohs surgery remains a highly controversial treatment technique for this malignancy. Disadvantages of standard surgical excision include the patient’s perception of increased invasiveness, time, and potential increased expense.
In both SCC and BCC, a margin of 4 mm for lesions less than 2 cm has been shown to provide tumor-free margins in 97% and 96% of cases, respectively. For BCC, it is important to distinguish between histologic subtypes. The morpheaform BCC is well known for its significant subclinical extension, and therefore a minimum 7-mm to 1-cm margin or consideration for Mohs surgery is advisable. For nodular, pigmented, or superficial BCC, a margin of 2 to 3 mm for small lesions (less than 1 cm) is adequate. Some authors divide this group of small lesions into those less than 5 mm and those 5 mm to 1 cm, with recommended margins of 2 mm and 3 to 4 mm, respectively. For lesions greater than 1 cm, a 5- to 7-mm margin is used, and lesions greater than 2 cm should include a 1-cm margin with strong consideration for delayed reconstruction until final pathology is available or margins are shown to be clear by perioperative frozen sections. Alternatively, referral for Mohs micrographic surgery should be considered. In SCC, lesions of less than 1 cm can be excised with a 5-mm margin, provided there is no perineural invasion and the lesion is not poorly differentiated. These adverse histologic features are indications for Mohs surgery and/or consideration of wider margins. Advanced SCC lesions with poor differentiation, invasion of adjacent structures, large size (greater than 2 cm), or recurrence often require 1- to 2-cm margins for tumor clearance. Finally, SCC originating in an area of radiation, chronic ulceration, or burn injury is a more aggressive tumor with an increased rate of metastatic disease and should be treated accordingly.
For in situ melanoma a 5-mm margin should be included; lesions 0.5 to 1 mm thick require a 1-cm margin; and melanoma 1 to 2 mm thick necessitates a 1- to 2-cm margin. Lesions greater than 2 mm thick must be treated with 2-cm margins. The necessary margin for lesions greater than 4 mm in depth (stage T4) has not been adequately studied, and early reports have failed to prove decreased local recurrence, disease-free results, or overall survival benefit to margins greater than 2 cm for these lesions.
History of the Procedure
Skin cancer is the most common malignancy of humans, and its incidence continues to rise despite increased awareness of the disease among both practitioners and the general public. Nonmelanoma skin cancer (NMSC), primarily squamous cell carcinoma (SCC) and basal cell carcinoma (BCC), is estimated to account for nearly 2 million new cancer cases per year, representing 95% of all skin cancers ( Figures 94-1 and 94-2 ). The incidence of NMSC has been rising at a rate of 5% per year, and it is estimated that 1 in 6 Americans develop skin cancer during their lifetime. Although the incidence of NMSC is high, the 5-year survival remains above 95%, with most deaths occurring from metastatic SCC. The overall incidence of metastatic disease in BCC is very low (0.0028% to 0.1%); favored sites include regional lymph nodes, the liver, lungs, bone, and skin. SCC more frequently develops metastatic disease, with an overall rate of 2% to 6% for the primary lesion and 24% to 45% for recurrent SCC. The presence of metastatic disease reduces the 5-year survival rate to only 34%; therefore, complete removal of disease at the time of initial surgery is essential.
Melanoma accounts for 75% of skin cancer–related deaths, but for only 5% of all skin neoplasms ( Figure 94-3 ). Approximately 80,000 new cases of melanoma skin cancer are diagnosed per year in the United States, and the patient’s age at diagnosis is younger than for most cancers. This makes melanoma the most common cancer diagnosis in women 20 to 29 years of age.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses