Armamentarium
|
History of the Procedure
The idea of plate osteosynthesis is more than 100 years old. In 1886, surgeon Carl Hansmann became the first to develop and present a procedure for subcutaneous fixation of bone fragments with a plate and screw system. He therefore is regarded as the inventor of plate osteosynthesis. First, he surgically exposed the fracture. Then he replaced and splinted the fragments with narrow, nickel-coated metal strips that had holes to receive screws. The steel screws were also nickel coated and had a conical screw thread, as do screws used in wood but not in metal. Both the plate and the screws stuck out of the wound and were removed 4 to 8 weeks later. Sir William A. Lane used screws and plates for fracture treatment in 1893. To gain a better fixation of the plates, he used conical screw heads, which fitted exactly into the conical holes of the plates. Two years later he reported corrosion of the material during the healing process. The Belgian surgeon Albin Lambotte established the term osteosynthesis. He is considered the father of modern internal and external splinting because he invented external fixation and various screws and plates made from aluminum, brass, copper, and silver. Sherman improved Lambotte’s screws and plates by applying vanadium steel and self-tapping machine threads. The screw tips received a cutting notch. Thus, the screw itself could cut a bone thread as it was inserted into the bone. This increased the screw’s hold. These systems of osteosynthesis often showed severe corrosion, metallosis, broken plates, and loose screws. This resulted in impaired healing, which brought the whole procedure into question. The plates constructed by Lane and Sherman could not be substituted because there was no better material available.
In addition to compression osteosynthesis, another procedure of plate osteosynthesis was established in the late 1960s. With miniplates, the path of static compression was avoided in favor of a dynamic compression. Plate osteosynthesis in the upper face and midface was not possible until the plates could be down-sized to miniplates.
Plate osteosynthesis is a breakthrough in maxillofacial surgery. The main advantage is that the patient does not need to undergo weeks of intermaxillary fixation. The introduction of noncorrosive materials, such as Vitallium and titanium, increased biocompatibility. The development of various system sizes, with screws as small as 0.8 mm in diameter, helps to extend the range of applications and patients’ convenience. Miniplate osteosynthesis in the upper face and midface was introduced by Champy and Loddé in 1976.
Because of its biocompatibility and mechanical properties, titanium is used as the standard material. Some disadvantages of titanium are a possible second surgery to remove the material, hot and cold irritation, bone growth inhibition in infants, migration and loosening of the screws, and interferences in imaging procedures. For these reasons, biodegradable osteosynthetic materials were developed more than 30 years ago. Mechanical properties, biocompatibility, and degradation time vary from system to system. The amount of inserted material and the polymers themselves (i.e., their molecular weight and crystallinity) determine the material’s in situ characteristics. The material most commonly used, besides polyglycolide (PGA), is polylactic acid (PLA), which exists in two enantiomers, l -lactic acid (PLLA) and d -lactic acid (PDLA). Increasing the amount of the D-form (PDLA) in a plate reduces crystallinity in a mix with PLLA, thus forming the amorphous poly- d , l -lactide (PDLLA). The degradation time of the available resorbable osteosynthesis systems ranges from 1 to more than 5 years.
Today, three-dimensional (3D) implants and custom-made devices represent the next step in reconstruction of the midface and upper face.
History of the Procedure
The idea of plate osteosynthesis is more than 100 years old. In 1886, surgeon Carl Hansmann became the first to develop and present a procedure for subcutaneous fixation of bone fragments with a plate and screw system. He therefore is regarded as the inventor of plate osteosynthesis. First, he surgically exposed the fracture. Then he replaced and splinted the fragments with narrow, nickel-coated metal strips that had holes to receive screws. The steel screws were also nickel coated and had a conical screw thread, as do screws used in wood but not in metal. Both the plate and the screws stuck out of the wound and were removed 4 to 8 weeks later. Sir William A. Lane used screws and plates for fracture treatment in 1893. To gain a better fixation of the plates, he used conical screw heads, which fitted exactly into the conical holes of the plates. Two years later he reported corrosion of the material during the healing process. The Belgian surgeon Albin Lambotte established the term osteosynthesis. He is considered the father of modern internal and external splinting because he invented external fixation and various screws and plates made from aluminum, brass, copper, and silver. Sherman improved Lambotte’s screws and plates by applying vanadium steel and self-tapping machine threads. The screw tips received a cutting notch. Thus, the screw itself could cut a bone thread as it was inserted into the bone. This increased the screw’s hold. These systems of osteosynthesis often showed severe corrosion, metallosis, broken plates, and loose screws. This resulted in impaired healing, which brought the whole procedure into question. The plates constructed by Lane and Sherman could not be substituted because there was no better material available.
In addition to compression osteosynthesis, another procedure of plate osteosynthesis was established in the late 1960s. With miniplates, the path of static compression was avoided in favor of a dynamic compression. Plate osteosynthesis in the upper face and midface was not possible until the plates could be down-sized to miniplates.
Plate osteosynthesis is a breakthrough in maxillofacial surgery. The main advantage is that the patient does not need to undergo weeks of intermaxillary fixation. The introduction of noncorrosive materials, such as Vitallium and titanium, increased biocompatibility. The development of various system sizes, with screws as small as 0.8 mm in diameter, helps to extend the range of applications and patients’ convenience. Miniplate osteosynthesis in the upper face and midface was introduced by Champy and Loddé in 1976.
Because of its biocompatibility and mechanical properties, titanium is used as the standard material. Some disadvantages of titanium are a possible second surgery to remove the material, hot and cold irritation, bone growth inhibition in infants, migration and loosening of the screws, and interferences in imaging procedures. For these reasons, biodegradable osteosynthetic materials were developed more than 30 years ago. Mechanical properties, biocompatibility, and degradation time vary from system to system. The amount of inserted material and the polymers themselves (i.e., their molecular weight and crystallinity) determine the material’s in situ characteristics. The material most commonly used, besides polyglycolide (PGA), is polylactic acid (PLA), which exists in two enantiomers, l -lactic acid (PLLA) and d -lactic acid (PDLA). Increasing the amount of the D-form (PDLA) in a plate reduces crystallinity in a mix with PLLA, thus forming the amorphous poly- d , l -lactide (PDLLA). The degradation time of the available resorbable osteosynthesis systems ranges from 1 to more than 5 years.
Today, three-dimensional (3D) implants and custom-made devices represent the next step in reconstruction of the midface and upper face.
Indications for the Use of the Procedure
The aim in modern bone surgery is rapid reestablishment of form and function. The reduction of fractures of the midface and upper face must resemble the form in height, width, depth, and projection. The blood supply of the fragments and the surrounding tissue should be maintained or reestablished. Further considerations are the occlusion and nasal and orbital function. Functionally stable internal fixation is indicated in multiple or comminuted fractures, panfacial fractures, defect fractures, wide open fractures, and dislocated midface fractures. A relative indication for internal fixation is patient noncompliance with conservative treatment. With polytrauma, patients absolutely need early fracture treatment. Sufficient stability prevents infection and secondary reconstructive surgery.
Due to the resorbable properties of osteosynthetic materials, the stiffness in particular is inferior to that of titanium plates. It is recommended that resorbable plates be used in non-load-bearing areas only, such as the cranium or midface. Therefore, they preferably are used for craniofacial surgery in growing patients.
Limitations and Contraindications
The level of stability needed depends on the fracture pattern. Adequate stability is not necessarily maximum stability. There are absolute and relative indications for the treatment of facial fractures. The decision on conservative or surgical treatment depends on the fracture pattern and on the condition and situation of the patient. Stable, simple, and closed fractures can be treated conservatively.
Today, mostly self-tapping screws are used in fracture surgery, which saves the time-consuming extra step of cutting a thread into the bone. Self-drilling screws also are available. These are suited for bones with a thin cortical layer, which makes them useful in the upper facial and midfacial region. The fixation of large segments with self-drilling screws is possible. In trauma cases, it can be difficult to position self-drilling screws in small bone fragments without breaking the fragments.
The mechanical properties of resorbable osteosynthetic material contraindicate its use in load-bearing areas.
Technique: Rigid Internal Fixation of the Midface and Upper Face
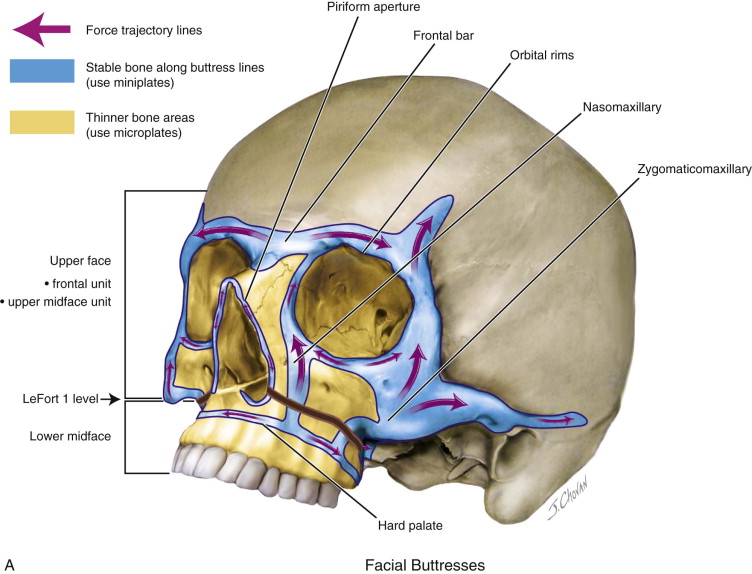
The face is divided into upper and lower halves by the Le Fort I level. The upper face consists of the frontal unit and the upper midfacial unit. The lower midfacial unit reaches from the Le Fort I level to the occlusal plane. The frontal unit forms the upper face and contains the frontal and temporal bones, the supraorbital rims, the orbital roofs, and the frontal sinus. The midfacial unit consists of the maxilla, the zygomas, the nasoethmoid complex, the internal orbits, and the infraorbital rims. The facial skeleton is composed of a solid bone framework ( Figure 71-1, A ). Paper-thin bone stretches between its buttresses, which are stable enough for the fixation with miniplates with screws.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses