Armamentarium
|
History of the Procedure
Posterior cranial vault remodeling is used primarily to treat infants and children with cranial deformities secondary to sagittal or lambdoid synostosis. Virchow first defined the term craniosynostosis in 1851. In its most basic form, craniosynostosis is a malformation in which one or more sutures of the cranial vault are prematurely fused. Virchow noted that this synostosis of the skull restricted growth perpendicular to the direction of the involved suture and promoted compensatory cranial overgrowth parallel to it.
The earliest recorded surgical attempts to treat craniosynostosis were performed by Lannelongue in Paris in 1890 and shortly thereafter, in 1892, by Lane in San Francisco. Strip craniectomies were performed on fused sagittal sutures to alleviate compression within the cranial vault. Synostosis treatment evolved considerably over the ensuing years and was revolutionized by the innovative techniques introduced by Tessier et al. in 1967. Later, in 1972, Rougerie et al. applied Tessier’s concepts of simultaneous suture release and cranial vault reshaping in infants, and in 1977, Whitaker et al. described a more formal anterior cranial vault remodeling and orbital reshaping procedure for unilateral coronal synostosis.
The current treatment for infants and children with moderate to severe deformities secondary to synostosis revolves around comprehensive open treatment with suture release, in conjunction with cranial remodeling to allow the brain to grow without restriction and to establish more normal contours of the craniofacial complex. In most cases, an intracranial approach is used to perform cranial vault and orbital osteotomies, which are reshaped and advanced to establish an ideal age-appropriate morphology.
History of the Procedure
Posterior cranial vault remodeling is used primarily to treat infants and children with cranial deformities secondary to sagittal or lambdoid synostosis. Virchow first defined the term craniosynostosis in 1851. In its most basic form, craniosynostosis is a malformation in which one or more sutures of the cranial vault are prematurely fused. Virchow noted that this synostosis of the skull restricted growth perpendicular to the direction of the involved suture and promoted compensatory cranial overgrowth parallel to it.
The earliest recorded surgical attempts to treat craniosynostosis were performed by Lannelongue in Paris in 1890 and shortly thereafter, in 1892, by Lane in San Francisco. Strip craniectomies were performed on fused sagittal sutures to alleviate compression within the cranial vault. Synostosis treatment evolved considerably over the ensuing years and was revolutionized by the innovative techniques introduced by Tessier et al. in 1967. Later, in 1972, Rougerie et al. applied Tessier’s concepts of simultaneous suture release and cranial vault reshaping in infants, and in 1977, Whitaker et al. described a more formal anterior cranial vault remodeling and orbital reshaping procedure for unilateral coronal synostosis.
The current treatment for infants and children with moderate to severe deformities secondary to synostosis revolves around comprehensive open treatment with suture release, in conjunction with cranial remodeling to allow the brain to grow without restriction and to establish more normal contours of the craniofacial complex. In most cases, an intracranial approach is used to perform cranial vault and orbital osteotomies, which are reshaped and advanced to establish an ideal age-appropriate morphology.
Indications for the Use of the Procedure
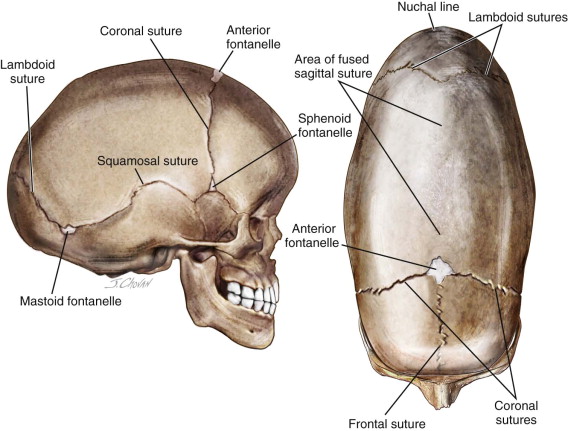
Posterior cranial vault remodeling is indicated for correction of cranial malformation associated with sagittal suture synostosis or lambdoid suture synostosis. When planning the time and type of surgical intervention, the surgeon must take into account future craniofacial growth and development and the maintenance of a normal appearance. Diagnosis of craniosynostosis is based on clinical and radiographic evaluation. The clinical examination involves palpating the skull for any areas of movement, ridging, and the presence or absence of the anterior or posterior fontanelles. A high-resolution computed tomography (CT) scan and three-dimensional (3D) reconstruction of the craniofacial complex are routinely used to evaluate the extent and location of involved sutures and to plan any surgical treatment ( Figure 44-1 ).
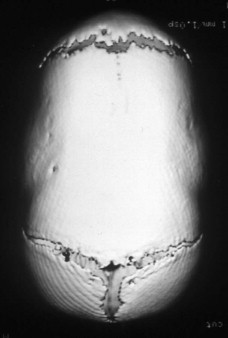
In patients with sagittal suture synostosis, the skull typically has an anterior-posterior elongation with a compensatory narrowing in the transverse dimension ( Figure 44-2 ). This is the most common form of cranial vault synostosis, accounting for approximately 50% of cases of nonsyndromic, single-suture synostosis in the United States. Children show different degrees of cranial deformity, depending on the extent of sutural involvement. They present with involvement of the anterior, the posterior, or the entire sagittal suture. When the posterior half of the sagittal suture is synostosed, the posterior two thirds of the cranial vault is reshaped with the patient in the prone position. If the entire sagittal suture is synostosed, the child usually is treated in a staged manner, first undergoing posterior vault reconstruction and then anterior vault and orbital reconstruction 6 to 8 weeks later.
Lambdoid synostosis results in flatness of the affected ipsilateral parietal-occipital region. Clinically, the location of the ear canal and external ear are more posterior and inferior on the ipsilateral side compared to the contralateral side. This is more noticeable when the patient is examined from the superior aspect and relatively inconspicuous from frontal or profile views. Posterior plagiocephaly secondary to lambdoid synostosis must not be mistaken for positional or deformational plagiocephaly secondary to infant positioning or molding. With positional plagiocephaly, the ipsilateral ear and forehead are positioned anteriorly and the ear is not inferiorly displaced, as it is with true lambdoid fusion. The overall incidence of true unilateral lambdoid synostosis is less than 3% of all isolated synostosis cases in the United States. In the surgical treatment of this deformity, the patient’s dysmorphic posterior vault is remodeled bilaterally, with the patient in the prone position, to a more symmetric and ideal age-appropriate shape.
Brain volume expansion in the normally developing child almost triples during the first year of life. If unimpeded brain growth is to occur, open sutures at the level of the cranial vault must expand outward during this phase of growth. When premature suture closure is combined with continued development, the growth potential of the brain may be physically limited. Surgical intervention, with suture release and cranial vault reshaping, is undertaken to restore normal intracranial volume.
Restricted cranial volume secondary to craniosynostosis can also result in elevated intracranial pressure (ICP). Normal ICP is defined as 0 to 15 mmHg; elevated ICP occurs when the pressure exceeds 15 mmHg. Renier et al. measured the ICP in 121 children and found that elevated ICP occurred in 42% of children with multisuture involvement and in 13% with single-suture involvement. They also noted a decrease in ICP after corrective surgery. If elevated ICP goes untreated for a prolonged period, detrimental effects on brain function may result; therefore, increased ICP is an important indicator for surgical treatment. Children should also be monitored for additional ophthalmologic sequelae. Untreated elevated ICP can lead to papilledema and optic nerve atrophy, possibly resulting in complete or partial loss of vision.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


