Introduction
Good oral hygiene is a challenge for orthodontic patients because food readily becomes trapped around the brackets and under the archwires, and appliances are an obstruction to mechanical brushing. The purpose of this study was to compare plaque removal efficacy of 3 toothbrush treatments in orthodontic subjects.
Methods
This was a replicate-use, single-brushing, 3-treatment, examiner-blind, randomized, 6-period crossover study with washout periods of approximately 24 hours between visits. Forty-six adolescent and young adult patients with fixed orthodontics from a university clinic in Germany were randomized, based on computer-generated randomization, to 1 of 3 treatments: (1) oscillating-rotating electric toothbrush with a specially designed orthodontic brush head (Oral-B Triumph, OD17; Procter & Gamble, Cincinnati, Ohio); (2) the same electric toothbrush handle with a regular brush head (EB25; Procter & Gamble); and (3) a regular manual toothbrush (American Dental Association, Chicago, Ill). The primary outcome was the plaque score change from baseline, which we determined using digital plaque image analysis.
Results
Forty-five subjects completed the study. The differences in mean plaque removal (95% confidence interval) between the electric toothbrush with an orthodontic brush head (6% [4.4%-7.6%]) or a regular brush head (3.8% [2.2%-5.3%]) and the manual toothbrush were significant ( P <0.001). Plaque removal with the electric toothbrush with the orthodontic brush head was superior (2.2%; P = 0.007) to the regular brush head. No adverse events were seen.
Conclusions
The electric toothbrush, with either brush head, demonstrated significantly greater plaque removal over the manual brush. The orthodontic brush head was superior to the regular head.
Good levels of oral hygiene are difficult to achieve in patients with fixed orthodontic appliances because the appliances are an obstruction to mechanical brushing, and food readily becomes trapped around the brackets and under the archwires. Effective mechanical removal of plaque and accumulated food debris throughout patients’ long treatment times is a special challenge to patients with these appliances; and it is perhaps even more critical for them relative to the nonorthodontic population to achieve high levels of daily plaque removal by effective brushing to prevent dental caries and periodontal disease.
A common aim of toothbrush manufacturers is to provide design features that can improve plaque removal efficacy. Although an impressive array of different models of manual and electric toothbrushes is available for patients, a recent systematic review by the Cochrane Collaboration demonstrated that oscillating-rotating electric toothbrushes consistently reduced plaque more than did manual brushes in both the short and long terms. Most toothbrush models, and the associated comparative clinical studies in the literature, however, have focused on nonorthodontic populations. Since many people in the general population have fixed orthodontic appliances (more than 5 million in the United States in 2006 according to the American Association of Orthodontists) and experience difficulties in achieving high levels of plaque control, there is an obvious need for brushes with appropriate design features to aid in plaque removal and for these potential advances to be assessed in comparative clinical studies.
Assessing plaque levels in patients with orthodontic appliances has been problematic because standard methods are based on subjective categorical scales and are not necessarily sensitive enough for measuring the surface area of the plaque and its irregular accumulation around the appliances. Recently, however, objective area-based plaque image techniques have been developed that offer advantages over more traditional methods. One such technique is the digital plaque imaging analysis (DPIA) developed by Sagel et al. This methodology has already been used for evaluating antiplaque chemotherapeutics, has shown excellent reproducibility in patients without orthodontic appliances, and has been successfully adapted by Klukowska et al for measuring plaque levels in patients with fixed orthodontic appliances.
The aim of this study in adolescents and young adults with fixed orthodontic appliances was to evaluate, with the DPIA methodology, the plaque removal efficacy of an oscillating-rotating electric toothbrush with a specially designed orthodontic brush head compared with a regular brush head and a regular manual toothbrush.
Material and methods
To be enrolled in this study, the subjects were required to be in good general health, at least 12 years of age, with fixed orthodontic appliances in both arches, and with a minimum of 8 natural front teeth with facial scorable surfaces. All subjects enrolled in the study were patients from the Department of Orthodontics at the University Medical Center of the Johannes Gutenberg-University Mainz in Mainz, Germany. The subjects were required to have evidence of prebrushing overnight plaque (approximately 10% plaque coverage) based on DPIA at the screening visit. In addition, the subjects were instructed to refrain from using nonstudy toothbrushes, dentifrices, mouth rinses, tooth-whitening products, and floss for the study duration, except during the washout periods between each visit, when they used their usual toothbrush. The subjects also agreed not to participate in any other oral or dental clinical study for the duration of this study. Subjects were excluded if there was evidence of neglected dental health.
The study, which took place in 2009, was approved by the Freiburger Ethik-Kommission International (Germany, code 08/2687) before the start of the trial. Each subject and the subject’s guardian gave signed informed consent, and each subject’s medical history was reviewed before study entry. Full details of the protocol can be found by contacting the Freiburger Ethik-Kommission International.
The DPIA system was similar to that described by Klukowska et al. It consisted of a high-resolution digital camera (digital model HC2500 3CCD; Fuji, Tokyo, Japan) fitted with a lens (Fujinon A4 × 7.5 BMD; Fuji; f2.8; 7.5-30 mm) with a linear polarizer to permit cross-polarized light. A long-wave ultraviolet flash (model FX60 fitted with cutoff filters at 265 nm; Balcar, Rungis, France) provided the lighting. The unit was connected to a computer, which recorded and analyzed the images. Before daily use, the system was calibrated to ensure proper operation. For each examination period, the room was darkened to prevent reflections. Patients disclosed their plaque with fluorescein solution by rinsing for 10 seconds with 25 mL of phosphate buffer, then rinsing for 1 minute with 5.0 mL of 1240 ppm fluorescein in phosphate buffer, and then rinsing 3 times for 10 seconds with 25 mL of phosphate buffer.
All images were captured within 2 minutes of disclosure to minimize fluorescence variation. The subjects were asked to place cheek retractors and to position their chin on a chin rest in front of the camera in a standardized way. The incisal edges of the front teeth were slightly opened (about 2 mm) and centered in the camera. For each subject, a digital image of the maxillary and mandibular anterior facial tooth surfaces was captured. The images were masked (masking included up to 12 anterior teeth if all present, excluding the brackets) and analyzed using Optimas software (version 6.5.1; Media Cybernetics, Silver Spring, Md). After that, an objective classification rule was developed (using least squared distance pixel classification) to recognize all key elements (classes) in the image: teeth and plaque (light and dark) on the teeth. All images in the data base were analyzed with automated batch classification, and the percentage of plaque coverage on the teeth was calculated as described previously.
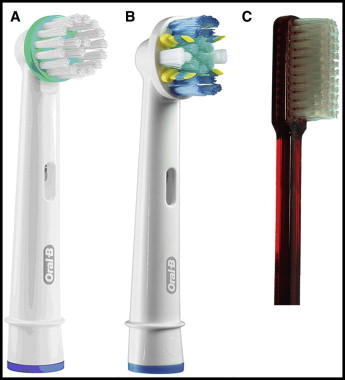
This study was a replicate-use, single-brushing, 3-treatment, examiner-blind, randomized, 6-period (visit) crossover design with washout periods of approximately 24 hours between visits. The 3 brushes compared in this study were the Oral-B Triumph (oscillating-rotating action) electric toothbrush (Procter & Gamble, Cincinnati, Ohio), with either the orthodontic brush head (OD17) or the FlossAction regular brush head (EB25; Procter & Gamble), and a manual toothbrush (ADA brush; American Dental Association, Chicago, Ill; Fig 1 ). Nine treatment sequences, each with 6 treatment periods (eg, ACBBCA, BACCAB, CBAABC, ABBACC, where A, B, and C represent the 3 brush treatments), determined the order in which the brushes were assigned to the subjects for the periods in each sequence (approximately 5 subjects per sequence). The sequences were randomly assigned using a computer-generated randomization plan prepared before the study. Kits containing the treatment products were assigned by site staff outside the view of the investigator (C.E.) to ensure blinding. The study sponsor and all study personnel, except those involved in product distribution, were blinded to treatment until the study concluded and the data base was finalized and locked.
At an initial (acclimation) visit (visit 1), the subjects disclosed their plaque with fluorescein as described above, and the subject’s plaque level was assessed using the DPIA. Subjects who qualified according to the inclusion and exclusion criteria were given the acclimation kit containing the electric toothbrush handle, both brush heads, and a dentifrice (Blendax Antibelag; Procter & Gamble, Gross-Gerau, Germany), and received verbal and written brushing instructions. Those brushing instructions were based on standard manufacturer’s brushing instructions and tailored for patients with fixed orthodontic appliances used in the Department of Orthodontics at the University Medical Centre Mainz. The subjects were instructed to brush the buccal surfaces of their teeth so that the brush could reach the tooth area above and below the brackets. They were told to guide the brush, slightly angled (45° angle), slowly in the interdental space and in the spaces between the brackets and the teeth with rotary movements of the brush head, so that the bristles reached into these critical areas. Then the subjects brushed using the electric toothbrush handle, half of the mouth for 1 minute with the orthodontic brush head (OD17) and the other half of the mouth for another minute with the regular brush head (EB25). During brushing with each brush, the subjects were observed without intervention.
The subjects were instructed to use their acclimation products at home in place of their usual toothbrush for regular brushing (2 minutes); they were required to use the products for approximately 4 days and to alternate the brush heads at each brushing (morning and evening). They were asked to switch back to their usual toothbrush along with the acclimation toothpaste 48 hours before the start of period 1 (visit 2). They were also asked to continue to use their usual toothbrush and acclimation toothpaste between treatment visits. The subjects were also instructed to perform their last oral hygiene in the evening (not later than 11 pm ) before the day of each scheduled afternoon study visit and asked to refrain from eating, drinking, chewing gum, or smoking for 4 hours before their appointment time.
At visit 2, the subjects’ plaque was disclosed as described above, and a prebrushing DPIA image was taken. The subjects were randomly assigned to 1 of the 9 treatment sequences and then instructed to brush (2 minutes for the electric toothbrush as described above and 2 minutes with the modified Bass brushing technique for the manual toothbrush following the standard hygiene instructions for patients with fixed orthodontic appliances used at the Department of Orthodontics of the University Medical Centre Mainz) with their brush (and marketed toothpaste) assigned for that treatment period. After brushing their teeth, the subjects redisclosed the plaque with fluorescein, and a postbrushing DPIA image was taken. The subjects were rescheduled for their next treatment visit and reminded to continue to use their usual toothbrush and acclimation toothpaste between study visits. Periods 2 through 6 (visits 3-7) had the same procedures as did period 1. All data were collected at the Department or Orthodontics at the University Medical Center of the Johannes Gutenberg University Mainz.
Statistical analysis
Based on plaque removal data from a previous DPIA orthodontic study (with a root mean squared error of 6.8), 40 completed subjects in a 3-treatment, 6-period crossover study should give a 2-tailed alpha of 0.05 with 80% power to detect a difference between treatments of at least 3.1%. Accordingly, approximately 45 subjects were to be randomized into the study. All data were analyzed using SAS software (version 8.2; SAS Institute, Cary, NC). The DPIA scores (ie, plaque levels as percentages of tooth area coverage) were averaged on a per-subject basis so that each subject had one DPIA score before brushing and another score after brushing in each of the 6 treatment periods. The difference in scores (baseline minus postbrushing) was calculated for each subject for each treatment period. These differences were analyzed for treatment differences using a mixed model analysis of covariance for a crossover design with terms in the model for subjects (random effect), treatment, period, and carryover (potential effect from treatment used in previous period), with the average prebrushing (baseline) score as the covariate. Since the carryover term was not significant ( P = 0.291), the final crossover model did not include the carryover term. The adjusted mean plaque removal scores for each treatment were also analyzed for statistical significance from zero using a t test on the adjusted treatment mean score differences from the analysis of covariance. Treatment comparisons were 2 sided, and all statistical tests had a significance level of 0.05.
Results
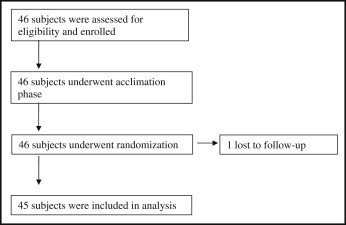
A total of 46 subjects were enrolled and randomized into 1 of the 9 treatment sequences. One subject was lost to follow-up before the second study visit, and 45 subjects completed the study. See Figure 2 for participant flow. Baseline demographics for each group are shown in Table I .
| Age (y) | Mean | Range | SD |
| 14.6 | 12-25 | 2.4 | |
| Sex | Frequency (n) | Percentage (%) | |
| Female | 17 | 37 | |
| Male | 29 | 63 | |
| Race | Frequency (n) | Percentage (%) | |
| Asian Indian | 1 | 2.2 | |
| Asian Oriental | 5 | 10.9 | |
| White | 40 | 86.9 | |
| Baseline DPIA | Mean (%) | ||
| Power/regular | 45.52 | ||
| Power/orthodontic | 46.45 | ||
| Manual | 46.08 |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


