Armamentarium
|
Revision cleft surgery can present unique reconstructive challenges that sometimes are more difficult to treat than those of the initial cleft deformity. The surgeon is frequently asked to manage postsurgical problems, even though he or she may have had little or nothing to do with the primary procedure. Additionally, once the lip and nose have been poorly positioned in infancy, growth can further compound the deformity. Palate surgery that results in large areas of denuded bone postoperatively can also result in growth restriction in both the sagittal and transverse planes. Improper muscle positioning or reconstruction in either the lip or palate repair can leave the patient with both esthetic and functional deficits that impair the individual’s self-esteem. Cleft surgeons must be students of the various protocols and techniques of past years, in addition to newer procedures, so that they can meet the unique revision challenges posed by scarring and compromised blood supply in patients who have undergone previous surgery.
Indications, Limitations, and Contraindications to Use of the Procedure
The appearance and function of the repaired lip and nose are largely determined by the primary repair during infancy. The simultaneous construction of functional nasal and labial muscles dictates the growth and development of the underlying facial skeleton and the appearance of the lip. The esthetic form of the lip and nose is the result of a carefully designed skin incision, muscle and cartilage dissection, and both oral and nasal muscle repair during the initial surgery. Of the multiple skin incisions that have been used, the geometric triangular and quadrangular incisions violate the subunits of the upper lip. The anatomic subunit repair and the advancement rotation, along with its modifications, more accurately replicate normal anatomic structures and are the most amenable to revision. Additional disadvantages of the geometric repairs include the tendency to create a long lip that can be difficult to correct secondarily and difficulty converting the geometric incision to a more anatomically appropriate skin incision if revision eventually is required.
The habilitation of cleft lip and palate consists of a series of procedures, the timing of which depends on chronologic and developmental milestones throughout life. Therefore, the lip and nose repair, which often is the first of many interventions, sets the tone for many of the procedures that follow. Much attention is paid to the lip in the primary repair; however, nasal positioning, especially the sagittal and vertical position of the ala/nostril sill, may have broader implications for future revision efforts. It is also important to keep in mind that the staged reconstruction of these patients is a stepwise process, and that careful consideration must be given to each procedure and its downstream effects on growth and subsequent procedures.
Although the construction of the labial and nasal muscular rings guides the eventual appearance and symmetry of the lip and nose, the individual’s innate ability to heal and scarring tendencies also play a key role in the esthetic appearance of the repair. Infection, postsurgical trauma, and technical error can contribute to suboptimal results.
The underlying skeletal platform must be considered when lip revision is planned because the presence or absence of a bony maxillary-alveolar cleft or maxillary hypoplasia greatly affects the appearance of the nasolabial structures as the child grows. Regardless of attempted soft tissue correction and camouflaging techniques, facial harmony can be accomplished only when the hard tissue cleft and hypoplasia have been addressed. Therefore, it is recommended that, depending on the age of the child and the degree of skeletal dysplasia, major soft tissue revisions be deferred until bone grafting or a Le Fort osteotomy has been accomplished, when possible. Occasionally, severe soft tissue problems and impaired self-esteem mandate earlier intervention, with the understanding that further revisional surgery may be required in the future.
When trying to determine whether a subtotal or total revision of the lip is required, the surgeon must have an understanding of the initial deformity and the goals of primary surgery. An understanding of the secondary deformity and its global functional and esthetic implications also is crucial. Tissue fillers (autologous, allogenic, and alloplastic), Z -plasties, and simple scar revisions can be used to address minor height mismatches of the white roll, vermilion notching, or vermilion fullness when the muscle is otherwise functional and united across the cleft. If applied inappropriately, however, these “minor” procedures may serve only to accentuate the deformity, increase scarring, or leave the patient well short of a complete correction. Total revision of the lip and nose should be considered if there are significant issues with lip height or symmetry or nasal symmetry, substantial vermilion/white roll mismatches, or a dehiscent orbicularis oris. Reopening the lip may be advantageous in that it provides an excellent opportunity (and additional access) to address residual nasal and septal deformities or turbinate issues. In some cases, the total revision can be performed with maxillary bone grafting. When there is significant damage and scarring to the cleft adjacent tissue, especially with the bilateral cleft lip, the surgeon may need to recruit nearby tissue to reconstitute the philtrum and reconstruct the oral muscular ring.
Analysis/problem list:
- •
Type of primary repair
- •
Underlying skeletal deficiency (bony cleft or maxillary hypoplasia)
- •
Soft tissue deficiency
- •
Presence of asymmetry
- •
Condition of the muscle
- •
Skin problems (soft tissue landmarks and scar assessment)
- •
White roll
- •
Wet-dry line
- •
- •
Degree of nasal asymmetry
Indications, Limitations, and Contraindications to Use of the Procedure
The appearance and function of the repaired lip and nose are largely determined by the primary repair during infancy. The simultaneous construction of functional nasal and labial muscles dictates the growth and development of the underlying facial skeleton and the appearance of the lip. The esthetic form of the lip and nose is the result of a carefully designed skin incision, muscle and cartilage dissection, and both oral and nasal muscle repair during the initial surgery. Of the multiple skin incisions that have been used, the geometric triangular and quadrangular incisions violate the subunits of the upper lip. The anatomic subunit repair and the advancement rotation, along with its modifications, more accurately replicate normal anatomic structures and are the most amenable to revision. Additional disadvantages of the geometric repairs include the tendency to create a long lip that can be difficult to correct secondarily and difficulty converting the geometric incision to a more anatomically appropriate skin incision if revision eventually is required.
The habilitation of cleft lip and palate consists of a series of procedures, the timing of which depends on chronologic and developmental milestones throughout life. Therefore, the lip and nose repair, which often is the first of many interventions, sets the tone for many of the procedures that follow. Much attention is paid to the lip in the primary repair; however, nasal positioning, especially the sagittal and vertical position of the ala/nostril sill, may have broader implications for future revision efforts. It is also important to keep in mind that the staged reconstruction of these patients is a stepwise process, and that careful consideration must be given to each procedure and its downstream effects on growth and subsequent procedures.
Although the construction of the labial and nasal muscular rings guides the eventual appearance and symmetry of the lip and nose, the individual’s innate ability to heal and scarring tendencies also play a key role in the esthetic appearance of the repair. Infection, postsurgical trauma, and technical error can contribute to suboptimal results.
The underlying skeletal platform must be considered when lip revision is planned because the presence or absence of a bony maxillary-alveolar cleft or maxillary hypoplasia greatly affects the appearance of the nasolabial structures as the child grows. Regardless of attempted soft tissue correction and camouflaging techniques, facial harmony can be accomplished only when the hard tissue cleft and hypoplasia have been addressed. Therefore, it is recommended that, depending on the age of the child and the degree of skeletal dysplasia, major soft tissue revisions be deferred until bone grafting or a Le Fort osteotomy has been accomplished, when possible. Occasionally, severe soft tissue problems and impaired self-esteem mandate earlier intervention, with the understanding that further revisional surgery may be required in the future.
When trying to determine whether a subtotal or total revision of the lip is required, the surgeon must have an understanding of the initial deformity and the goals of primary surgery. An understanding of the secondary deformity and its global functional and esthetic implications also is crucial. Tissue fillers (autologous, allogenic, and alloplastic), Z -plasties, and simple scar revisions can be used to address minor height mismatches of the white roll, vermilion notching, or vermilion fullness when the muscle is otherwise functional and united across the cleft. If applied inappropriately, however, these “minor” procedures may serve only to accentuate the deformity, increase scarring, or leave the patient well short of a complete correction. Total revision of the lip and nose should be considered if there are significant issues with lip height or symmetry or nasal symmetry, substantial vermilion/white roll mismatches, or a dehiscent orbicularis oris. Reopening the lip may be advantageous in that it provides an excellent opportunity (and additional access) to address residual nasal and septal deformities or turbinate issues. In some cases, the total revision can be performed with maxillary bone grafting. When there is significant damage and scarring to the cleft adjacent tissue, especially with the bilateral cleft lip, the surgeon may need to recruit nearby tissue to reconstitute the philtrum and reconstruct the oral muscular ring.
Analysis/problem list:
- •
Type of primary repair
- •
Underlying skeletal deficiency (bony cleft or maxillary hypoplasia)
- •
Soft tissue deficiency
- •
Presence of asymmetry
- •
Condition of the muscle
- •
Skin problems (soft tissue landmarks and scar assessment)
- •
White roll
- •
Wet-dry line
- •
- •
Degree of nasal asymmetry
Techniques
Long Upper Lip
The long upper lip is infrequently seen with the predominance of advancement rotation repairs performed today; in fact a short lip is far more common. Excessive lip length was primarily a problem of triangular and quadrangular repairs, but it can also be encountered with other techniques. The long lip can be a difficult problem to correct, requiring horizontal excision of tissue at the supravermilion level or in the subalar region. The scars left by these revisions can be camouflaged by the white roll and the alar crease, respectively, although they are less than optimal in appearance. The asymmetric long lip can be even more challenging, requiring a complete revision of the original repair, possibly along with one of the aforementioned tissue excisions applied unilaterally. The surgeon must also be sure that the appearance of a long upper lip is not actually hypoplasia of the maxilla with inadequate incisor display. In this instance, the solution lies not in a soft tissue revision, but rather in appropriate positioning of the maxilla by means of a Le Fort osteotomy.
Reduction of Lip Height
Subalar or supravermilion excisions can be used to adjust the height of the lip for excessive lip length. Either form of excision can be combined with philtrum modifications as needed, and both types generally require the removal of both skin and muscle. Subalar and supravermilion excisions can be designed symmetrically or asymmetrically to address specific length issues.
Tight Upper Lip/Mutilated Philtrum
The tight upper lip can stem from overly aggressive soft tissue excision at the time of primary or secondary repair, or it can be the result of a protuberant premaxilla. The appearance of tissue deficiency can be further accentuated by maxillary hypoplasia or a full lower lip. Further lip revision that includes soft tissue excision may serve only to enhance the problem unless nearby tissue is recruited in the form of an Abbe flap. This pedicled cross-lip flap, based on the inferior labial artery, adds width and appropriate bulk while reducing the width differential between the upper and lower lip. The Abbe flap also may be of value when the prolabial tissue has been severely damaged by scarring. Before a reconstruction such as this is undertaken, it is best to have the maxilla or premaxilla already in the appropriate skeletal position.
Abbe Flap
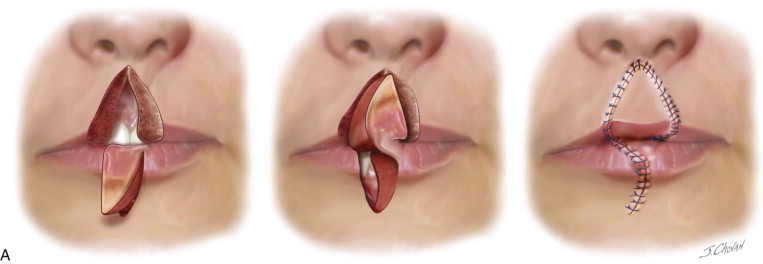
When the philtrum region has been affected by scarring or when there is a significant full-thickness tissue deficiency of the upper lip, a pedicled Abbe flap can be designed based on the inferior labial arterial pedicle of the lower lip. The flap and the inset defect can be customized based on the recipient site requirements for height and esthetics ( Figure 57-1, A ).
- •
The upper lip incision can be designed to allow downward rotation of the lateral lip elements. It can involve a full-thickness excision of damaged or scarred tissue.
- •
A full-thickness shield, “ W ,” or rectangular-shaped flap is designed in the lower lip, including the skin, vermilion, and mucosa.
- •
One side of the flap remains pedicled at the vermilion, based on the labial artery that runs within the muscle of the vermilion.
- •
The flap is rotated 180 degrees.
- •
Inset is accomplished by a three-layer closure (mucosa, followed by muscle and skin).
- •
The donor site is closed similarly.
- •
The pedicle is divided after 14 days, and the remainder of the flap is trimmed and inset.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses