Chapter 5
TREATMENT AND FEE PLANNING
Treatment planning is one of the most important and possibly most neglected areas in the management of patients with failed, extensive restorations.
The advantages of setting time aside for planning for treatment and calculating fees are as follows:
- The dentist becomes realistic as to how much time is required to plan such complex treatment.
- The dentist is made to realise that somebody has to pay for this time;
- The dentist may decide to bear this cost himself, but it is costing somebody.
- Proper thought can be given to the sequence of treatment.
- Sufficient time can be allocated for each appointment.
- Intervals between appointments can be calculated.
- Since treatment follows a planned sequence, the appointment book can be carefully programmed and the practice run in a controlled and predictable manner.
- Everybody understand the time commitment necessary for treatment.
- It is possible to accurately estimate fees (the system of multiplying the expected laboratory fee by three is irrational and erratic in effect).
Careful treatment planning is absolutely essential in the management of these patients. If the reader is unwilling to accept this discipline or is unrealistic about the time required for treatment planning, the primary value of this text is lost.
System
Two cards are used, 25.5 cm x 20.5 cm (Greenbrook Dental Supplies Ltd). The treatment planning card is blue, the fee calculation card pink (Figs 5-1a+b).
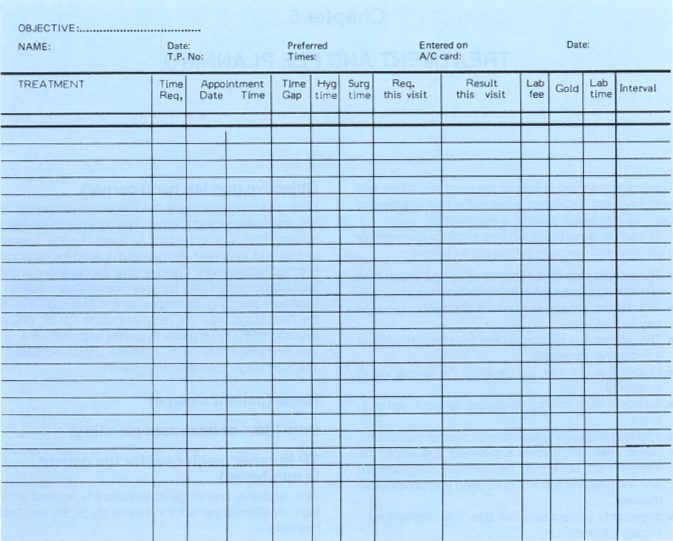
Fig. 5-1a Treatment planning card. A new card is filled in for every stage of treatment. See pages 121–126 for more details.
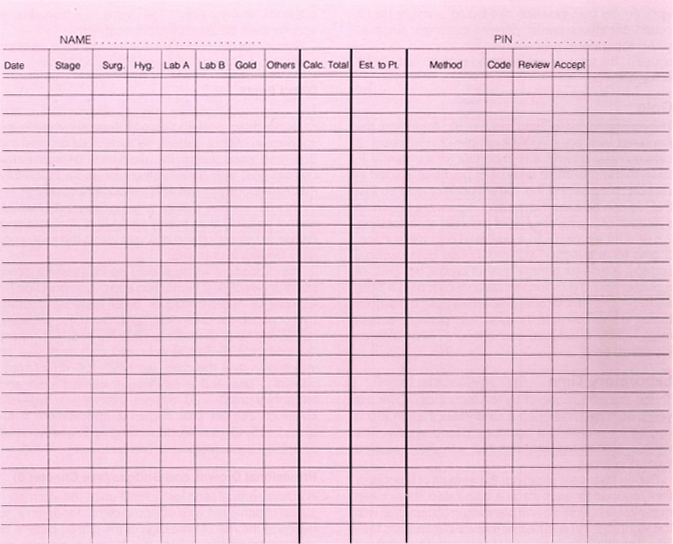
Fig. 5-1b Estimate/Fee calculation card. Each stage of treatment which may consist of several treatment planning cards, is entered. The fee per time unit is entered and the number of hours entered beneath it. The total fee is calculated for each column and the total calculated. The estimate to the patient is then entered. For further details see pages 126–128.
Treatment Planning Card
Each of the headings on the treatment planning card will be considered individually:
Objective (top left hand corner)
When planning treatment, the first aim is to determine the objectives for each stage. The details can be filled in later, but it is important to map out the overall direction of treatment. A new card is used for each set of primary objectives. For example, the objective at the initial appointment may be: examination, consultation, treatment planning, correspondence. The objective of the next stage may be: remove bridge 13–23, place provisional bridge plus six hygienist appointments. The next stage may be: re-evaluate, adjust occlusion. The next stage: definitive bridgework, 13–23.
Name (patient’s name)
Date (date of treatment planning)
TP Number (each card for the patient is numbered)
One, and only one stage of treatment is entered on a card. Additional cards for the same stage are used as required.
Preferred Times (times/days preferred by patient for appointments)
Treatment
Once the objectives have been decided upon, each stage is planned appointment by appointment. The appointments are listed and for each appointment, all appropriate procedures are listed. A question often asked is “How do you know what you will find?”, or “How long should the next appointment be?”. The answer is, if you don’t know what you will find, sufficient time must be allowed for the worst possible finding, so that the patient leaves the surgery in a stable state. If less time is actually taken, then so be it. However, when insufficient time is allowed, problems may arise not only for the patient under treatment, but also for the dentist who is likely to be stressed, and, in consequence, for subsequent patients.
If different treatment possibilities are required for each particular stage, they can each be entered with their appropriate times. It is better to make appointments based on the longest possible times needed and then to shorten them as this becomes possible. In a busy practice it is harder to find time, than to reduce it. In a quiet practice the time is easily available, so why allocate too little?
Time Required
For each appointment the times necessary to perform the various procedures are noted and added together to give the appropriate duration of that appointment. It is quite salutary to work out how much time is actually required, as opposed to the time one thinks should be allocated. As stated earlier, frequently, the chairside assistant has a better idea of the time requirements than the dentist.
It cannot be overstressed – time is an enemy. If insufficient time is allocated, problems occur, compromises are made, “botch-ups” propagated and the patient, the dentist and the subsequent patients all suffer.
Appointment, Date, Time
These will be entered in the appointment book by the secretary when the appointments are made.
Time Gap
This is the time interval required between successive appointments and is dependent upon, for example, the time required for laboratory work or the time interval between hygienist appointments.
Hygienist Time
The total hygienist time noted on this card is calculated and entered at the base of the column.
Surgery Time
Similarly, the total surgery (that is, dentist) time is entered.
Required this Visit
This lists the major requirements for this visit, such as: mounted study casts; three unit ceramometal bridge; technician – half an hour – for example for pouring casts or staining crowns. If this were a consultation appointment with, for example, an endodontist, a letter of referral and radiographs would be required at this visit.
Result this Visit
This lists the items resulting from the visit, usually requiring laboratory work. For example: impressions, soldering pickup, jaw registrations.
Lab Fee
This relates to the fees estimated for outside laboratory work (in my own practice this would primarly be for cobalt chromium partial denture castings, since all other laboratory procedures are carried out “in house”). The total is estimated and entered at the base of the column.
Gold
The estimated fee for gold can be calculated from the Required Visit column, for example: 2 cast posts, 3 ceramometal crowns. It is important for the dentist to know the approximate amount of gold that is used in various castings and the current price of gold so that this fee can be calculated. Calculations are based on averages of 2 gms per unit of provisional restoration, 2.5 gms for a crown with a porcelain occlusal surface, 3 gms for a ceramometal crown with gold occlusal surface, 3 gms for a three quarter crown, 3.5 gms for a gold crown, 2 gms for a small core cast onto a post, and 3 gms for a molar core cast onto a post. It is slightly better to overestimate the gold fee, patients accept more readily a reduced final account rather than an increased one!
Laboratory Time
This is the time required by the technician. Over the years we have developed a card index system which can be transfered to a computer based system. The various procedures are itemized with their required laboratory times.
During treatment planning, the amount of laboratory time required for each stage is calculated. It has taken many years of working and planning in conjunction with the technician, to ensure that these estimates are realistic. The total laboratory time is calculated and entered at the base of the column in a similar manner to hygienist time and dentist time.
Interval
The time span allocated for laboratory work must be realistic. It is foolish to program 60 hours of laboratory work with a time interval of 10 days, since there would be little time abailable for anything other than that particular piece of work. Also, during that 10 days the dentist is prevented from undertaking treatment involving technical services, this leads to problems with appointment scheduling within the practice. It would be far more sensible, therefore, to spread the 60 hours over 20 days, thereby allowing for work on other patients. At the same time the question of safety must be raised how safe is it for the patient if there is a whole month between one stage of treatment and the next? Wherever possible, it is best to leave the patient in a stable state at the end of each appointment, so that the danger of an emergency or a change in tooth or jaw positions is minimized. The ways in which this is achieved will be discussed subsequently.
Sometimes it is important that the interval is as short as possible. Commonly occuring examples are:
Direct Posts
The usual sequence for this is: appointment in the morning; direct post and core fabricated in the mouth; impression of core pattern; no temporization, cast the post and core during the day; later on same day cement post with definitive cement and a laboratory made temporary crown with temporary cement.
This avoids the risk of a temporary post, which cannot possibly fit as evenly as the final post, exerting undue stress on localized points within the root, possibly leading to cracking.
The procedure which should be followed for direct posts is: direct post fabrication and overimpression (in alginate or hydro-colloid or other material. If using hydrocolloid, the core must be in DuraLay, not wax); half to one hour, depending upon the post, to prepare the post-hole, build the post and core and take an impression over the core; lab time – 30–45 minutes; interval – one and a half hours; cement post and temporary crown – 30 minutes; interval – 0; hygienist clean off cement plus hygienist appointment if required – 15–45 minutes, depending upon whether a full arch provisional restoration has been recemented.
Provisional Crowns and Bridges (see Chapter 8)
Following preparation for multiple units, initial temporization is achieved with plastic crowns. Frequently, to minimize the risk of breakage of the plastic crowns or another emergency, these are followed, as soon as possible, by provisional restorations. These are made from a semi-precious cast substructure covered with plastic.
An Example of an Initial Treatment Plan (Fig 5-1c)
Objective
Examination, Consultation, Three Hygienist Appointments, Treatment Plan, Correspond.
The details are as follows:
TP Number 1
Treatment 1: examination, full mouth radiographs, impressions, jaw registration, face bow.
Time Required: one hour.
Required this Visit: technician – quarter of an hour to pour casts.
Result this Visit: impressions for mounted diagnostic casts.
Lab Time Required: 30 minutes.
Interval: laboratory timed so that mounted casts will be ready for visit 6.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


