General Chairside, Radiation Health and Safety, and Infection Control
General Chairside
1. In the Universal or Standard tooth numbering system, which letter represents the maxillary left primary second molar?
2. Which classification of carious lesions form on the occlusal surfaces or the buccal and lingual grooves of posterior teeth?
3. The more fixed attachment of the muscle that is usually the end attached to the more rigid part of the skeleton is the:
4. Which of the following teeth would not be found in the deciduous dentition?
5. What does this charting symbol indicate?

6. What does this charting symbol indicate?

7. On a cephalometric analysis, the abbreviation Na stands for:
8. If the charting conditions indicate that there is a furcation involvement, some type of symbol will be placed:
a. at the apical area of the tooth
b. on the occlusal surface of the tooth
9. What does this charting symbol indicate?
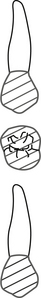
10. What does this charting symbol indicate?

11. What does this charting symbol indicate?
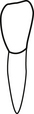
12. What does this charting symbol indicate?
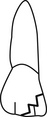
13. Which surgical procedure describes a hemisection?
a. removal of the apical portion of the root
b. removal of diseased tissue through scraping with a curette
c. removal of the root and crown by cutting through each lengthwise
d. removal of one or more roots of a multirooted tooth without removing the crown
14. How should a properly positioned dental assist be seated?
a. on the same plane as the dentist
b. 2 to 4 inches above the dentist
15. Using Black’s classification of cavities, what class are caries along the cervical of a tooth?
16. An ML restoration on tooth #9 is classified as a _________ restoration.
17. Which instrument is used to remove subgingival calculus?
18. Forceps are used in this portion of the clamp while placing the rubber dam.
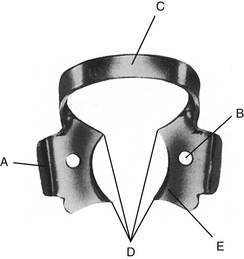
19. Which classification of motion should the dentist and the dental assistant eliminate to increase productivity and decrease stress and body fatigue?
20. Which is an accurate statement regarding the placement of an oral evacuator tip?
a. Place the HVE tip as far into the distal of the arch as possible.
b. Always use the pen grasp to avoid stress on the hand.
c. Place the angle of the HVE tip in a downward position to pick up maximum fluids.
d. The assistant should place the HVE tip first, and then the operator should place the handpiece.
21. If a left-handed operator is preparing tooth #14 for a crown, where does the dental assistant place the bevel of the high-velocity evacuator?
a. parallel to the buccal surface of the tooth being prepared
b. distal to the left maxillary tuberosity from the buccal side
c. parallel to the lingual surface of the tooth being prepared
d. distal to the left maxillary tuberosity from the lingual side
22. Which of the following statements is not a concept of four-handed dentistry?
a. Place the patient in the supine position.
b. The operator and assistant should sit as close to the patient as possible.
c. Use preset tray setups with instruments placed in sequence of use.
23. Which type of handpiece can operate both forward and backward and can be used with a variety of attachments?
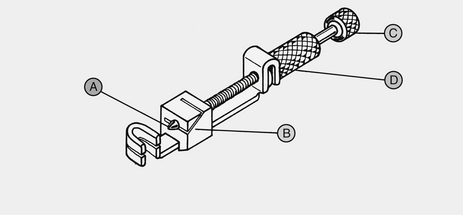
24. When a Tofflemire matrix band retainer is used, which of the knobs or devices would be used to adjust the size or loop of the matrix band to fit around the tooth and loosen the band for removal?
25. What is the purpose of a barbed broach?
26. Which instrument would be used to remove debris or granulation tissue from a surgical site?
27. Which of the following statements is true regarding the use of a universal matrix band and retainer?
a. The matrix retainer and wedge are both placed on the buccal surface.
b. The matrix retainer is placed on the buccal surface, and the wedge is placed from the lingual at the proximal surface involved.
c. The matrix retainer is placed on the lingual surface, and the wedge is placed from the buccal at the proximal surface involved.
d. It is not necessary to use a wedge with a Tofflemire matrix band and retainer.
28. A dental team is restoring an MOD preparation on tooth #4 with amalgam. Which item is not required to place this type of restoration?
29. An orthodontic positioner is designed to:
30. Which of these instruments would not be a choice when placing a gingival retraction cord?
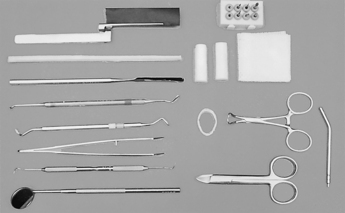
31. From the photograph, what is the procedure for which this tray would be used?
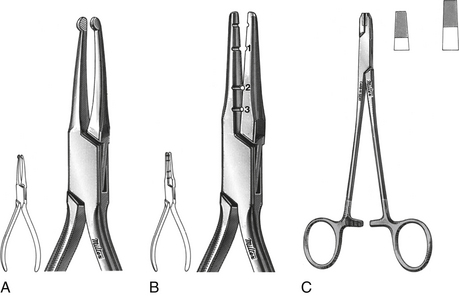
32. The instruments shown from left to right are:
a. three-pronged pliers, posterior band remover, ligature pin, and ligature cutter
b. Howe pliers, wire bending pliers, and ligature tying pliers
c. bird beak pliers, contouring pliers, and Weingart utility pliers
33. Which of the following is not a postoperative instruction to control bleeding after a surgical procedure?
a. Bite on two folded gauze for at least 30 minutes after the procedure is completed.
b. If bleeding continues and does not stop, call the dental office.
c. Restrict strenuous work or physical activity for the remainder of the day.
34. What is the endodontic test in which the dentist applies pressure to the mucosa above the apex of the root and notes any sensitivity or swelling?
35. The process by which the living jawbone naturally grows around an implanted dental supports is known as:
36. The treatment used as an attempt to save the pulp and encourage the formation of dentin at the site of the injury is a(n):
37. The removal of the coronal portion of an exposed vital pulp is a(n):
38. The instrument used to adapt and condense gutta-percha points into the canal during endodontic treatment is:
39. The surgical removal of diseased gingival tissues is called:
40. A(n) __________is a dentist with a license in the specialty of dentistry who provides restoration and replacement of natural teeth and supporting structures.
41. Periodontal pocket depth is charted at ____ points on each tooth during a baseline charting procedure.
42. A periodontal pocket marker is similar in design to a ______.
43. A(n) ___________ is an additive bone surgery that includes the reshaping and contouring of the bone.
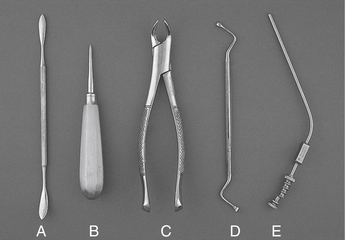
44. From the instruments shown below, select the periosteal elevator.
45. Using Black’s classification of cavities, a pit and fissure lesion on the occlusal surface of molars and premolars is considered a Class _____ cavity.
46. Using Black’s classification of cavities, a lesion found on the mesial or distal surfaces of incisors and canines is considered a Class _____ restoration or cavity.
47. Which orthodontic pliers are used in fitting bands for fixed or removable appliances?
48. Which of the following rotary instruments would cut fastest and most efficiently?
49. In selecting a shade for a composite restoration, under which of the following conditions should the shade be selected?
a. Select before tooth preparation and dry the tooth thoroughly.
b. Select with operating light in place before tooth preparation.
50. When cleaning a dental handpiece, it is important to:
a. follow the handpiece manufacturer’s directions thoroughly
b. follow the sterilizer manufacturer’s directions thoroughly
51. A(n) __________ procedure is performed to remove defects and to restore normal contours in the bone.
52. Which of the following is not a measurement used in constructing a complete denture?
53. All of the following are categories of restorations except:
54. ____________ sealants __________ require mixing as they cure when they are exposed to UV light.
55. When adjusting a crown after cementation, the dentist most likely would use a(n) ______.
56. The procedure performed to remove subgingival calculus and to remove necrotic tissue from the periodontal pocket is referred to as __________:
57. Why would a dentist use an intraoral camera?
a. to take a patient’s picture for the dental chart
b. to demonstrate periodontal pocket depths
58. To minimize leakage, what would the operator do to the rubber dam around each isolated tooth?
59. What are the attachments used for support or retention of a three-unit bridge called?
60. Which portion of the bridge replaces the missing tooth?
61. Which instrument would be passed to the operator to smooth the interproximal box on a prepared MO amalgam?
62. Which of the following would be considered a contraindication for a patient receiving a fixed bridge?
63. The surgical removal of the apex of an endodontically treated tooth is what procedure?
64. What is the common name for the #110 pliers?
65. Before surgery, a patient is explained the procedure and then signs an authorization for treatment. What is this process called?
66. A patient who is said to be “tongue tied” would have what type of procedure?
67. The water-to-powder ratio generally used for an adult maxillary impression is ____ measures of water and _____ scoops of powder.
68. If using a self-cure composite resin system, what will occur if the containers are cross-contaminated?
a. It will cause the material to harden.
b. It will prevent the material from hardening.
69. Which statement is incorrect regarding tooth conditioner?
a. The conditioning agent forms a mechanical bond with the enamel.
b. The conditioning agent is flooded onto the surface and rubbed vigorously.
c. The conditioning agent is generally applied with special applicators provided by the manufacturer.
d. The conditioning agent is rinsed from the tooth after a recommended time to stop the etching process.
70. Which of the following materials would not be used to take a final impression for the creation of a prosthetic device?
71. A porcelain fused to a metal crown would be designed so the porcelain would always be on which surface?
72. A glass ionomer material may be used for all of the following except a(n):
73. If the room temperature and humidity are very low while mixing a final impression material, the setting time may be:
74. A porcelain fused to a metal crown is being seated. The assistant will mix the cement to a _____________ or ____________ consistency.
75. A posterior tooth with a deep preparation may require a base that is designed to prepare pulpal defense by functioning as a(n):
76. IRM (intermediate restorative material) is used primarily for:
77. A patient has a fractured amalgam on 29DO. Time in the doctor’s schedule does not permit placement of a permanent restoration. Which of the following statements is correct as to the type of dental cement and the consistency that would be used in this clinical situation?
a. temporary cement to a secondary consistency
b. final cement to a secondary consistency
78. A reproduction of an individual tooth on which a wax pattern may be constructed for a cast crown is a(n):
79. Which food can be compared to a reversible hydrocolloid?
80. An alginate impression has been taken to prepare a set of diagnostic models. Which of the following statements is false as it relates to handling the impression? Alginate impressions __________.
a. should be stored for as short a period as possible
b. expand when stored in water
c. shrink when stored in air with low humidity
d. can be stored in 100% relative humidity without serious dimensional changes for up to 24 hours
81. A broken removable denture prosthesis can be repaired:
a. at home by the patient with an OTC kit
b. at home by the patient with superglue
82. A removable denture prosthesis can be cleaned in the dental office by all of the methods listed below except:
a. immersion in an ultrasonic cleaner with a special denture cleaning solution
b. brushing with a denture brush
c. removing calculus with hand instruments
d. with routine prophylaxis instruments and brushes in the patient’s mouth
83. A patient is seen early in the morning. The record indicates she has diabetes. She mentions she had not yet had breakfast but took all of her medications before the appointment. As the appointment progresses, it is noted that she is perspiring, seems not able to focus on conversation, and is increasingly anxious. These symptoms are an indication of:
84. Which of the following statements is not true as it relates to a patient’s respiration?
a. If a patient knows the breaths are being monitored, he or she will usually change the breathing pattern.
b. For children and teenagers, the respiration rate is higher than that of an adult.
c. A person’s respiration normally is not noticeable unless he or she is having trouble taking a breath.
d. Respirations are normally higher in counts per minute than the pulse rate.
85. What is the respiration pattern for a patient in a state of tachypnea?
86. What is the respiration pattern for a patient who is hyperventilating?
87. In an emergency the staff member should feel for the pulse of a conscious patient at which artery?
88. If a patient displays symptoms of hyperglycemia and is conscious, what is the first thing you should ask the patient?
a. “What time did you awaken this morning?”
c. “How many fingers do you see?” while holding up your fingers.
89. Which of the following are the recommended guidelines for cardiopulmonary resuscitation?
a. access, breathing, and circulation,
b. access, breathing, circulation, and defibrillation
90. Which of the following conditions is not a potential medical contraindication to nitrous oxide?
91. What substance is added to a local anesthetic agent to slow down the intake of the agent and increase the duration of action?
92. The type of anesthesia achieved by injecting the anesthetic solution directly into the tissue at the site of the dental procedure is known as ___________.
93. General anesthesia is most safely administered in a:
94. Which of the following refers to an allergic response that could threaten the patient’s life?
95. How should the staff respond if a patient is having a grand mal seizure?
a. Stand back and let the seizure run its course.
b. Place the patient in an upright and seated position.
96. In which situation is nitroglycerin placed under the tongue of a patient?
97. MyPlate is an outline of what to eat each day. The smallest segment of the plate concept represents which food source?
98. How are foods that contain sugars or other carbohydrates that can be metabolized by bacteria in plaque categorized?
99. Organic substances that occur in plant and animal tissues are _______, and essential elements that are needed in small amounts to maintain health and function are _________.
100. Dry mouth is also known as ______________.
101. _____________is more prominent in older adults who have experienced gingival recession.
102. Which factor would not contribute to xerostomia in a patient?
103. Which of the following would not be suggested as an intervention for the prevention of dental caries?
104. A caries risk assessment test is used to determine the _________.
a. number of mutans streptococci and lactobacilli present in the saliva
105. Inflammation of the supporting tissues of the teeth that begins with __________ can progress into the connective tissue and alveolar bone that supports the teeth and become _______________.
106. A dietary food analysis includes a diary of everything a patient consum/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


