Bone grafting
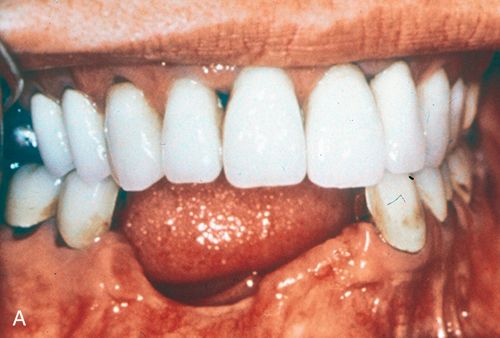
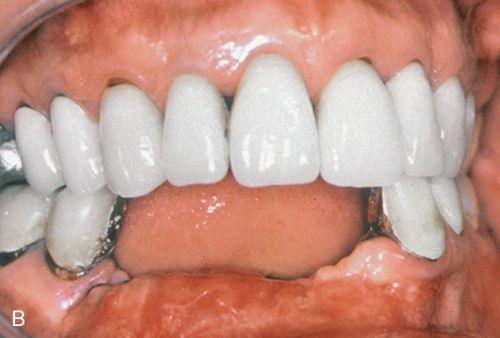
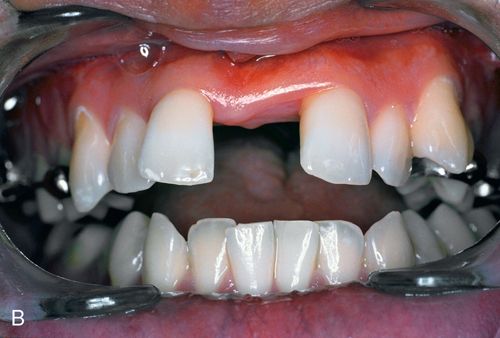
Minor bone grafts or bone substitutes can be used to augment a regional defect in the alveolus, such as a bony undercut or narrow ridge that may have resulted from buccal plate collapse after tooth extraction (Fig. 18-2 A,B) or from traumatic bony avulsion.
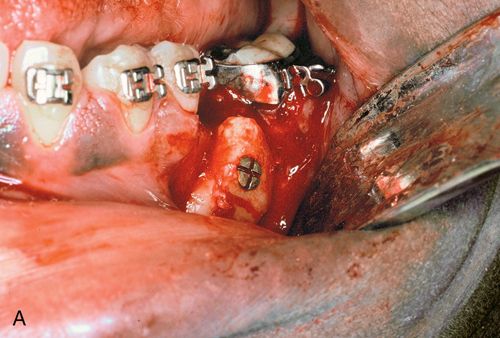
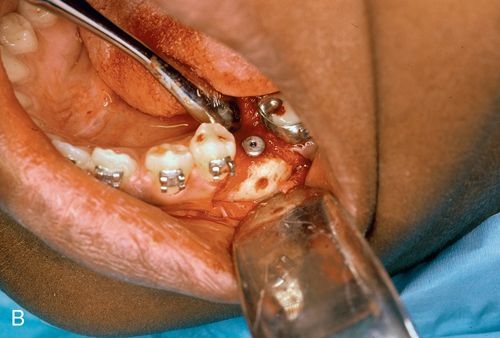
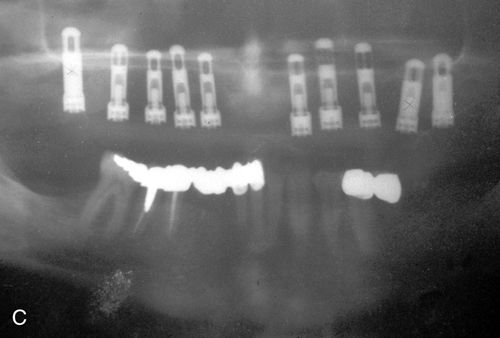
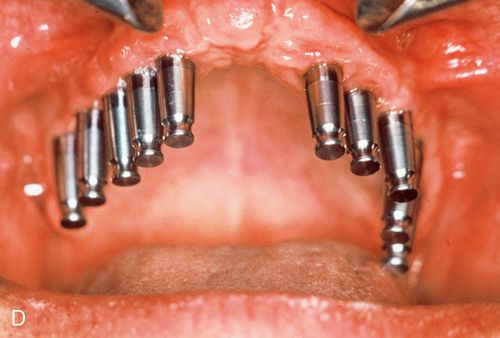
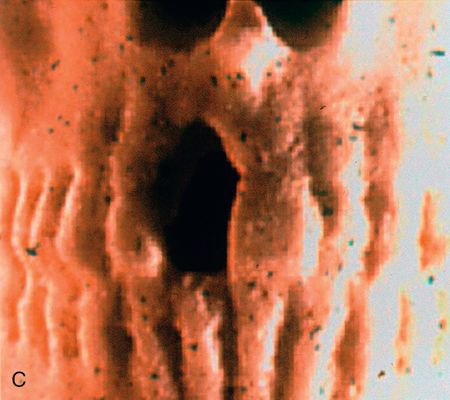
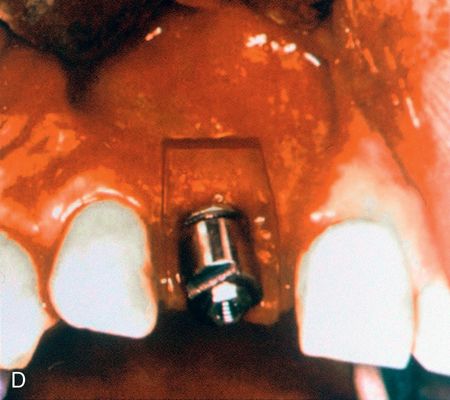
After a period of consolidation of the graft, an endosteal titanium fixture can be placed. Particulate bone grafts also can be placed within the maxillary sinus (sinus lift), enabling the dentist to restore implant fixtures distal to the maxillary canine/bicuspid area with a fixed splint7 (Fig. 18-2 C,D). Larger grafts can restore the alveolar height of the complete maxillary or mandibular arches.
Bone grafts are classified as either autologous or homologous (allogenic). Autologous grafts are harvested from the patient and transplanted into the defect. Donor sites can be close to the surgical site (chin and maxillary tuberosity) or distant (calvarium, iliac crest, or tibial plateau). The advantage of the intraoral source, aside from proximity, is the minimal morbidity associated with this type of graft harvest. Disadvantages include the paucity of marrow rich in osteoprogenitor cells and the limited amount of bone available for transplantation.8
When the requirement for bone is more significant (e.g., for bilateral sinus augmentations or full-arch onlay grafting), the iliac crest is the preferred site for harvesting the large amounts of corticocancellous bone needed.9 Up to 100 mL of bone can be harvested from the posterior iliac bone.10 The tibial plateau is another good source of cancellous bone. Approximately 25 mL of bone can be harvested from this source. Although immediate sequelae, such as pain and gait disturbance, are common, long-term donor site morbidity is very rare. Calvarial bone grafts are mainly cortical in nature and are usually reserved for reconstruction of the midface, nasal, and orbital areas.11
Homologous (allogenic) bone is obtained from human cadavers. The material is processed by human tissue banks to remove the antigenic and potentially infectious material (e.g., hepatitis, human immunodeficiency virus) and sterilized with ethylene oxide or gamma irradiation before packaging. Banked bone is available in lamellar strips, corticocancellous blocks, bone chips, and bone powder. The powder form also is available in a demineralized preparation. This process is believed to increase the concentration of an osseoinductive protein, bone morphogenic protein (BMP), which is present in the nonmineralized moiety.12 In general allogenic bone grafts are used to restore small defects or act as graft “expanders” when mixed with autologous bone harvested intraorally. The advantage of this type of grafting material is that it is readily available, thus eliminating the need for a surgical donor site and the associated morbidity. The major disadvantage is the risk of transmission of a disease for which no screening is currently available.
Bone graft substitutes, such as resorbable or nonresorbable hydroxyapatite and other bioactive ceramic granules, can also fill minor contour defects and, to a lesser degree, expand autologous grafts.13 Although these materials are considered osteophilic, they are not completely replaced by native bone and are not considered to produce good implantation sites. Again the advantage of this material is that it is readily available. The disadvantage is that the material is replaced by bone only on its surface. It generally is not recommended for sinus lifts or significant ridge augmentation in preparation for implant placement.
Alveolar distraction
Alveolar bone distraction recently was introduced as an alternative to bone grafting for ridge augmentation of traumatically induced, limited alveolar defects (Fig. 18-3 A,B). Specially designed expansion devices are used to slowly “distract” an osteotomized bone segment to restore the lost alveolar height.
Once this has been achieved and the regenerate has been allowed to consolidate, the distractors are replaced with endosteal fixtures that will osseointegrate and support a cosmetic prosthesis, which will then have a more acceptable crown to root (fixture) ratio.14 A similar technique is now used to distract the anterior mandibular alveolus in patients with atrophic mandibles to create a more favorable site for the placement of endosteal fixtures.15 Changes in the design of alveolar distractors will allow these devices to play a dual role of distractor/implant fixture without having to change the hardware at the completion of the distraction (Fig. 18-3 C,D).
Skeletofacial procedures
Malalignment of the basal and tooth-supporting alveolar structures often result in facial “disharmony” and suboptimal function and appearance. Maxillary and mandibular osteotomies commonly are used to correct dento-skeletofacial deformities.
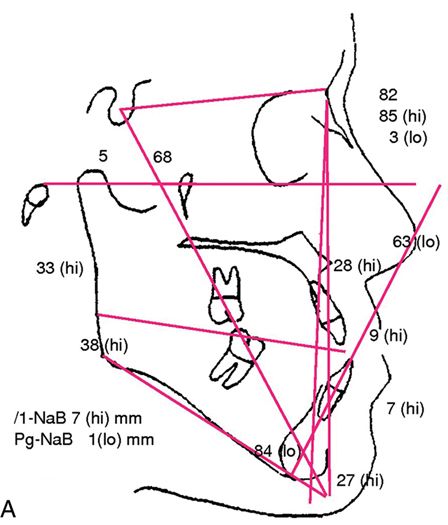
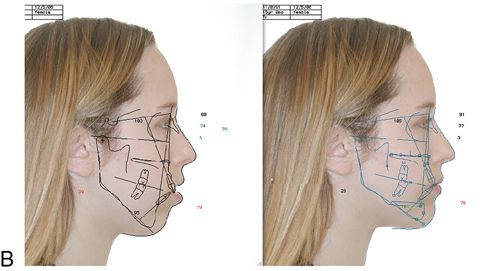
The first step in the evaluation of a patient suspected of having a dento-skeletofacial deformity is a thorough clinical exam, good quality extraoral and intraoral photographs, and cephalometric radiographs or a cone beam CT scan (CBCT). The lateral cephalogram can be traced manually or digitized and processed with treatment planning software and a personal computer (Fig. 18-4 A,B).
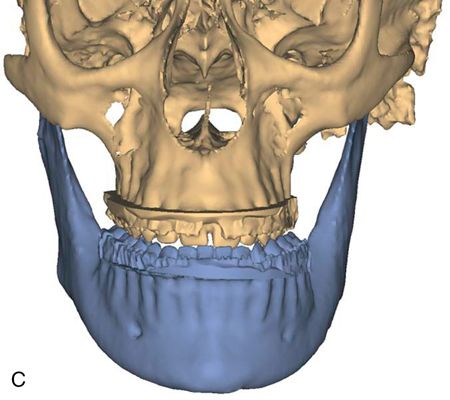
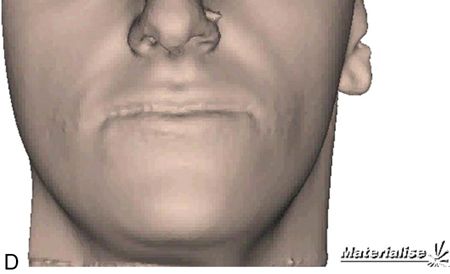
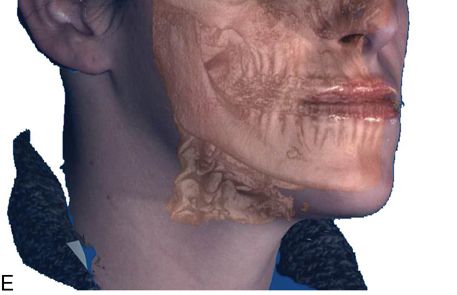
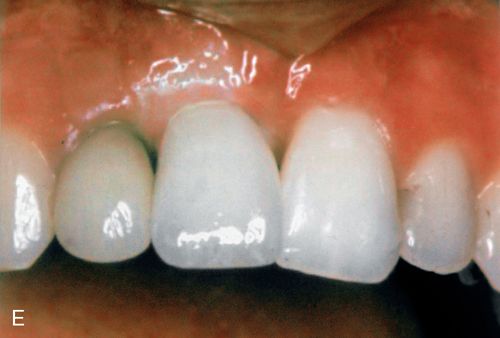
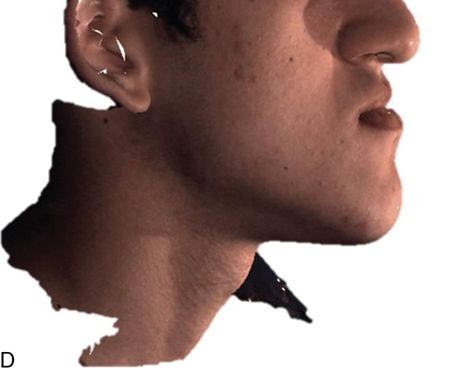
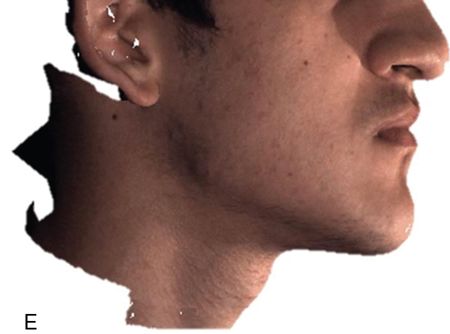
For more complex asymmetries, the Digital Imaging and Communications in Medicine (DICOM) files obtained from the cone beam CT can be used to generate a virtual three-dimensional (3D) cast of the patient’s facial skeleton and overlying soft tissue mask (Fig. 18-4 C,D). For a more realistic soft tissue representation, a 3D photograph obtained using a special camera can be overlaid on the soft tissue mask (Fig. 18-4 E) and used to demonstrate the facial changes that can be expected from the movement of the osteotomized bony segments.
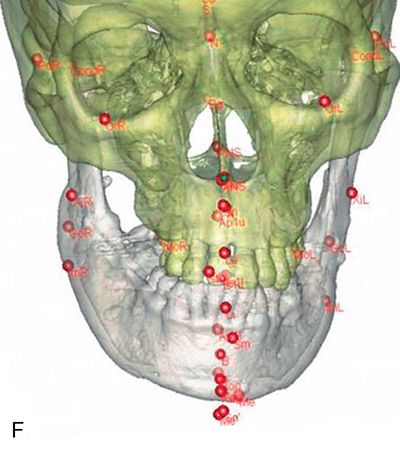
The virtual skeletal cast can then be digitized using conventional cephalometric landmarks and analyzed to generate a problem list. Unlike 2D cephalometry, a number of these landmarks will be subdivided into right and left components to take into account the asymmetry between the two points (ramus height or occlusal cant) (Fig. 18-4 F). Once the diagnosis and problem list are generated, a treatment plan is formulated and the proposed osteotomies can then be simulated by creating virtual objects using the planning software’s cutting tools. The segments are then repositioned three dimensionally to the desired position (Fig. 18-5 A-C). The soft tissue predicted change is calculated using a complicated mathematical algorithm that allows the surgeon and patient to visualize the projected soft tissue changes (Fig. 18-5 D).
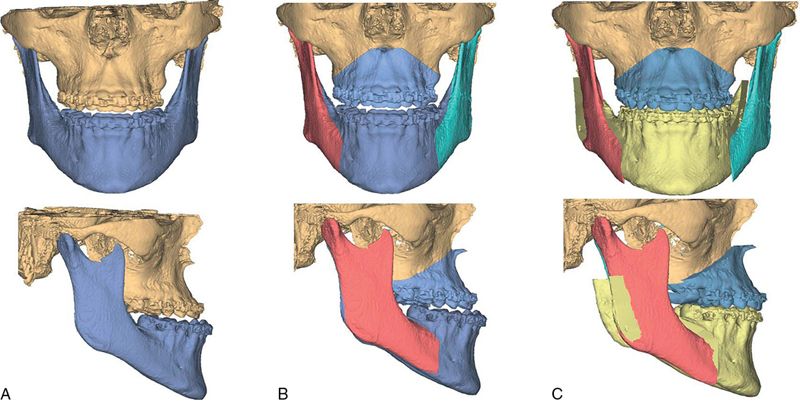
Computer-assisted design and computer-assisted manufacturing (CAD/CAM)-generated intermediate and definitive splints can also be designed and produced using the planning software and used intraoperatively to help execute the planned procedures (see Fig. 18-1).
Computer-assisted treatment planning is not only a very effective, time-saving technique for the planning of complex maxillomandibular osteotomies, but is also a powerful communication tool. It allows the surgeon to discuss the proposed procedure with the patient using interactive, visual images. It also allows a demonstration of the virtual outcome of the proposed surgery. However, clinical results that do not reproduce the predicted simulation may lead to patient dissatisfaction, with possible legal implications (for a complete discussion, see Chapter 27). Therefore all discussions with the patient should include a disclaimer that the simulation must be viewed as an aid in visualizing the treatment result, which in no way implies a guarantee of the surgical result.
Most dento-skeletofacial deformities are three dimensional. They must be evaluated and treated in the anteroposterior, vertical, and transverse planes.
Anteroposterior deformities include prognathism, or excessive growth of the jaw in a horizontal plane. Mandibular prognathism (Fig. 18-6 A), such as is seen in a Class III skeletal malocclusion, is more common than maxillary or bimaxillary (maxilla and mandible) prognathism.
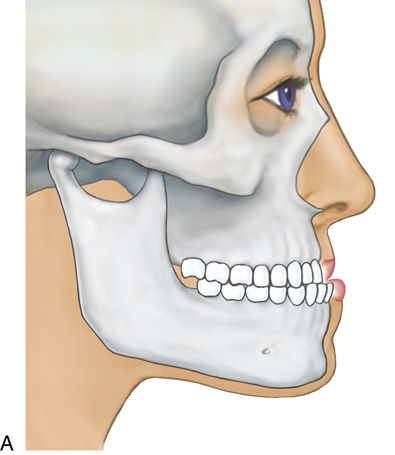
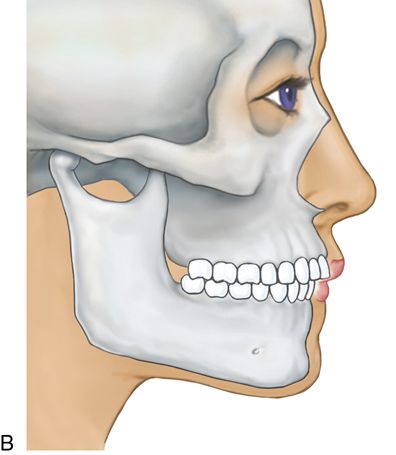
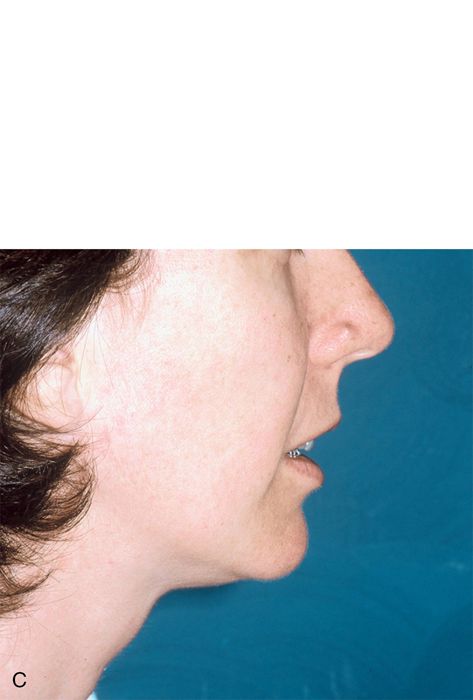
Retrognathism is an underdevelopment of the jaw in the horizontal plane (Fig. 18-6 B). Both the maxilla and mandible may be affected (Fig. 18-6 C).
Retrogenia is an underprojected chin, and progenia is an overprojected chin. These deformities are surgically corrected with maxillary or mandibular osteotomies. See the sections on Maxillary Surgery and Mandibular Surgery.
Vertical deformities include vertical maxillary excess (VME), an excessive downward growth of the maxilla that results in a “gummy” smile and a “long face” with a narrow alar base and retrodisplaced mandible, caused by the counterclockwise mandibular rotation prompted by this excessive growth (Fig. 18-7 A).
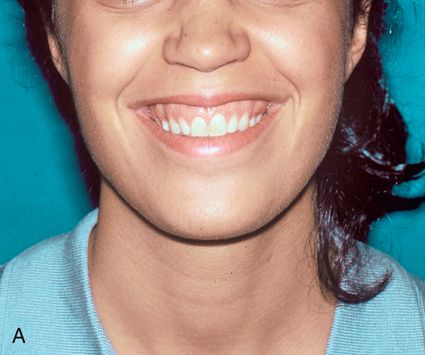
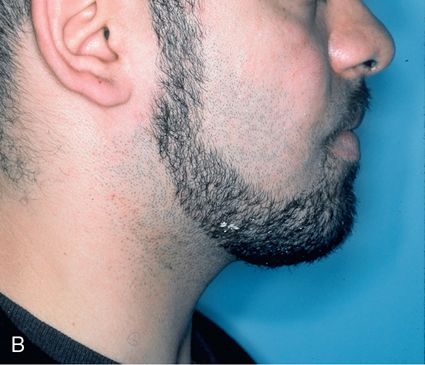
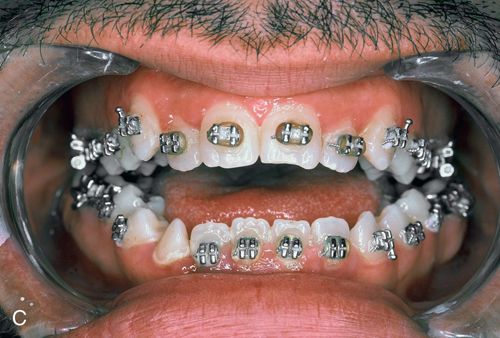
The lip to tooth ratio at rest is excessive (>4 mm) and is accompanied by lip incompetence (the patient is unable to passively oppose the lips without straining the perioral musculature [orbicularis oris and mentalis]). When growth excess is limited to the posterior maxilla, an anterior open occlusion (apertognathia) will result, further accentuating the relative mandibular retrognathia (Fig. 18-7 B,C).
Isolated (apertognathia) with occlusal contacts limited to the second molars, anterior maxillary hyperplasia is rare and usually is caused by an overgrowth of the anterior alveolus in a patient with a severe mandibular retrognathia (Class II, division I). Mandibular vertical excess usually is limited to the anterior mandible and can be corrected surgically by means of a horizontal osteotomy with the resection of a bony “wedge.” Maxillary vertical excess is treated with a Le Fort I osteotomy, removal of a wedge of bone, repositioning, and stabilization of the maxilla (Fig. 18-8 A).

Maxillary vertical deficiency, another vertical deformity, is also corrected with a Le Fort I osteotomy. In this situation, the placement of a wedge of bone (grafting) between the upper facial skeleton and the repositioned maxilla becomes necessary before stabilization (fixation) (see Fig. 18-8 A). Transverse deformities usually result in a constricted arch form with overcrowding and tooth malalignment. The treatment goal is the expansion of the alveolar segment to correct the tooth/arch-length discrepancy. In the maxilla, a palatal expansion device can be used. Surgically assisted palatal expansion is based on the concept of distraction osteogenesis and relies on the creation of lateral maxillary wall and midpalatal osteotomies (Fig. 18-8 B).
After a few days (the latency period), the expander is activated and begins a controlled distraction of the callous at the osteotomy site. Once the expansion is complete, the regenerate bone is allowed to consolidate before the teeth can be moved into the neoalveolar segment. In patients in whom the transverse deformity is not caused by a tooth/alveolar discrepancy and the orthodontist is unable to align the dental units over the alveolar segment, a multiple-segment Le Fort I osteotomy with interpositional bone grafting can be done to correct the transverse problem. A similar procedure can be performed to expand the mandibular arch with an internal bone/tooth-borne distraction device and a midline mandibular osteotomy to expand the mandibular alveolus.16 This device has now been approved for clinical use.
The deformities described in the preceding can involve both the maxilla and the mandible and may also be associated with facial asymmetries such as laterognathia or facial canting in patients of hemifacial atrophy or hypertrophy (congenital) or condylar hyperplasia (acquired). Temporomandibular joint pain and dysfunction and the resulting masticatory and swallowing difficulties often are associated with dento-skeletofacial deformities and should alert the practitioner to investigate for a malocclusion or jaw malposition. Recognition of the underlying condition and appropriate referral can increase the patient’s confidence in the practitioner’s ability to provide comprehensive care.
Once the workup has been completed and a problem list has been formulated, the surgeon selects the surgical procedures designed to correct the deformity and discusses the risks and benefits of each procedure with the patient. If the patient agrees with the proposed treatment, the general practitioner and orthodontist optimize the patient’s dentition in preparation for the surgical procedure. Dental and periodontal diseases must be either eradicated or controlled before the surgery. The goal of preoperative orthodontics is to level and align the dental units over the alveolus and coordinate the opposing dental arches. The fixed orthodontic appliances will also be used for maxillomandibular fixation at the time of surgery.
Surgical procedures
Mandibular surgery
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


