and Melih Motro2
(1)
Faculty of Dentistry Department of Orthodontics, University of Marmara, Istanbul, Turkey
(2)
Henry M. Goldman School of Dental Medicine Department of Orthodontics & Dentofacial Orthopedics, Boston University, Boston, Massachusetts, USA
Cleft lip and palate treatment is a long journey for the patient, family, and also the team that is involved in the treatment that starts from the first day of birth and continues till the late adolescence. The first shock the parents live the first day they meet their baby turns to questions and worries. In this moment, health-care professionals should have the ability to calm down the parents, assure them their baby is a great gift as any other baby is, and direct them to an adequate cleft team to be sure that they will have the right journey map for the future.
Cleft lip and palate is defined as the nonfusion of the upper lip and/or the roof of the mouth (hard and/or soft palate), which appears as a gap in the affected structures. Studies report 1–7 per thousand babies have a cleft lip or a cleft palate, or both. Most cleft lip and palate (%66.9) occur with a cleft palate. Unilateral clefts are more common than bilateral clefts; females are more likely to get cleft palate, and males are more likely to have cleft lip and palate together.
All the detailed treatment modalities will not be included in this book. However, a brief information concerning the treatment applied will be provided.
Main Cleft Types
The cleft lip may vary from a small defect to complete cleft extending to the nasal floor. Usually, these clefts are associated with alveolar clefts also. However, isolated alveolar clefts can be seen without the lip cleft as well. If the baby has the palatal cleft involved as well, then the cleft can be categorized as a complete cleft.
Unilateral Incomplete Cleft Lip
It is characterized by vertical separation of the lip. However, the cleft area does not reach the nasal area. They have either an intact nasal sill or a Simonart band (Fig. 2.1).
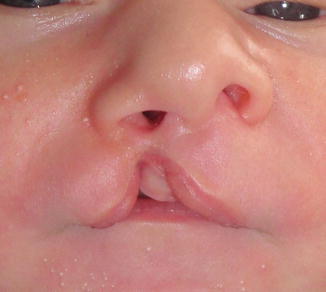

Fig. 2.1
Unilateral incomplete cleft lip
Unilateral Complete Cleft Lip and Palate
It is characterized by complete vertical separation of the lip, including the nostril sill and alveolus. No Simonart band is followed. The position of the alveolar segments and the width of the alveolar cleft are also important factors when defining the cleft and therefore the treatment approach. Alveolar segments can be wide, narrow, collapsed, or not collapsed. According to the width and collapse rate of the segments, presurgical orthopedic treatment approaches can be used to align the arch shape and increase the columellar height of the nose, resulting in decreased tension in lip repair and benefits in final nasal anatomy (Fig. 2.2).
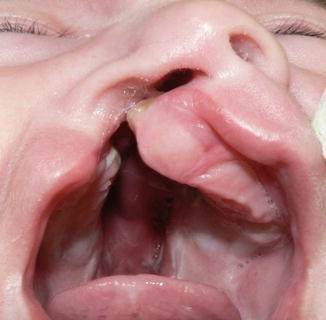

Fig. 2.2
Unilateral complete cleft lip and palate
Bilateral Complete Cleft Lip and Palate
In this type of cleft, the premaxilla is not in alignment with the lateral alveolar segments due to the lack of connection with the lateral palatal shelves. Premaxilla is usually overprojected and may show rotation. Lateral shelves, on the other hand, are usually collapsed to the midline because of the lack of intact connection with the premaxilla (Fig. 2.3).
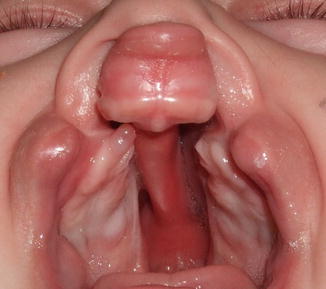

Fig. 2.3
Bilateral complete cleft lip and palate
Mostly, the anterior nasal spine is congenitally missing or underdeveloped, resulting in the recession of the footplates, which leads to broad flat nasal tip and typical absent columella.
The patients born with cleft lip and palate go through lots of surgeries from the beginning of their lives. At the first months of their life, usually in the third month, they undergo a lip surgery (Semb et al. 2005). However, before the lip surgery, some nonsurgical approaches aim to bring both sides of the lip and prolabium together to ease further lip surgery by reducing the strain that possibly occur after the surgery. In these approaches, babies wear a plate that both eases sucking and brings the alveolar segments closer orthopedically (Santiago et al. 1998). At the same time, with part extending to the nose, it also helps to raise the nose tip by increasing the columellar length. The main purpose of lip surgery is both giving the baby an esthetically pleasing appearance and at the same time a good functionality to help sucking. Till then, the baby is fed with special feeders. Usually, these feeders have liquid flow control, and they are used with severe feeding problems. Feeding is also provided with the assistance of feeding plates after the lip surgery, till the palatal closure is performed. There is no general agreement about the right time for palatal surgery. However, the current consensus is that palatal repair should be performed around 18 months of age before meaningful speech develops.
Palatal Repair
Palatal repair is performed with several aims:
1.
To close defect and have anatomically intact functional palatal
2.
To help normal speech production and
3.
To reduce dentoalveolar deformities
There are many techniques used by different practitioners, such as
-
von Langenbeck technique
-
Veau–Wardill–Kilner pushback technique
-
Bardach two-flap technique
-
Furlow double opposing Z-plasty
-
Two-stage palatal repair
-
Alveolar extension palatoplasty (AEP)
-
Primary pharyngeal flap
-
Intravelar veloplasty
-
Vomer flap
-
Buccal myomucosal flap
However, the mostly used techniques are von Langenbeck, Veau–Wardill–Kilner, Bardach two-flap, and Furlow double opposing Z-plasty techniques.
von Langenbeck Technique (Fig. 2.4)
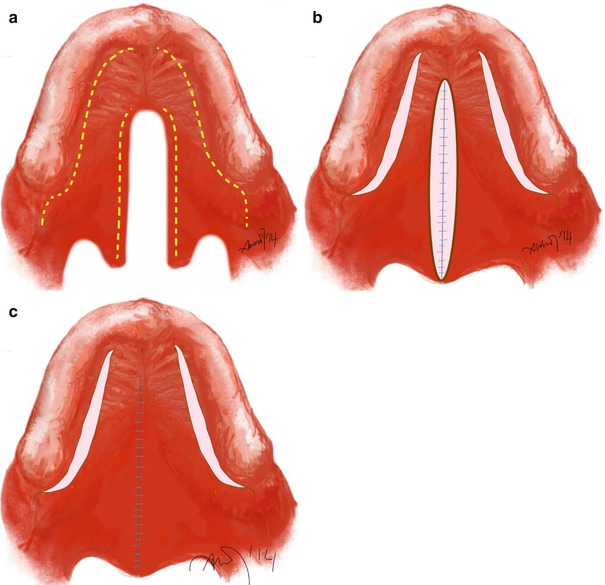
Fig. 2.4
von Langenbeck technique for palatal closure. (a) Incision lines along the oral side of the cleft edges and along the posterior alveolar ridge from the maxillary tuberosities to the anterior level of the cleft. (b) Bipedical mucoperiosteal flaps are risen. (c) Flaps are mobilized medially and sutured along the midline. Illustrated by Dr. Ali Murat Kokat
This method was introduced in 1861 by Bernard von Langenbeck. It uses mucoperiosteal flaps for the hard palate repair. The flap is left attached to the alveolar margin, and the incisions are made through the cleft edges to release the mucoperiosteum. Additional lateral relaxing incisions are also involved to relieve tension in the midline repair (Agrawal 2009; Fisher and Sommerlad 2011).
Veau–Wardill–Kilner Pushback Technique (Fig. 2.5)
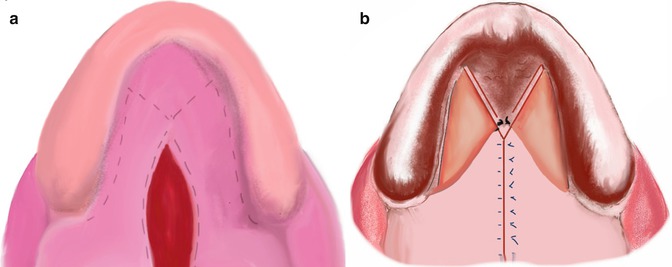
Fig. 2.5
Veau–Wardill–Kilner technique. (a) Incision lines. (b) Mucoperiosteal flaps raised and the oral mucosa is sutured – note that nasal mucosa and oral mucosa are sutured separately – open wound surfaces are left for secondary healing. Illustrated by Dr. Ali Murat Kokat
This technique adopts V–Y procedure. As a result, mucoperiosteal flap and the soft palate are positioned posteriorly. It was believed that the palatal lengthening would improve the speech outcome. However, some studies show that it is not the case. This technique also has the disadvantage of increased maxillary growth restriction and large anterior fistulas due to raw area left for secondary healing after the pushback of the flap (Agrawal 2009; Fisher and Sommerlad 2011).
Bardach Two-Flap Technique (Fig. 2.6)
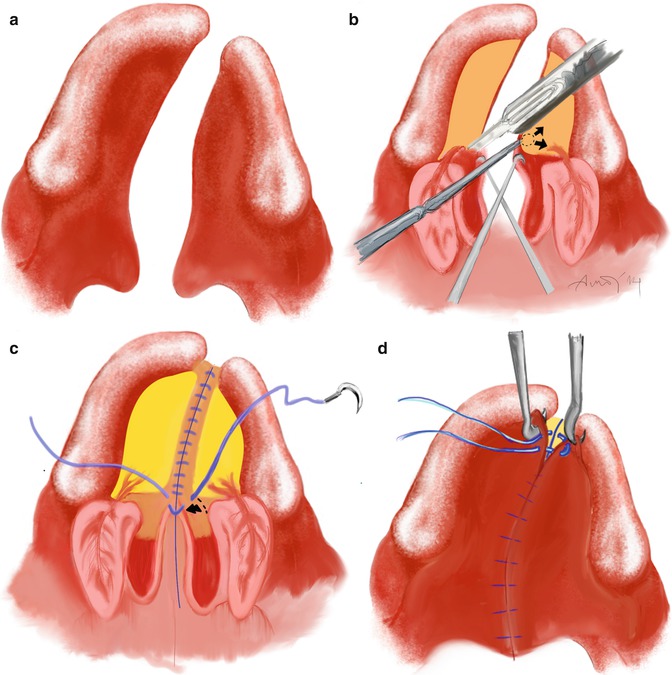
Fig. 2.6
Bardach two-flap technique. (a) Incision along palatal side of the alveolus and along the edges of the cleft is performed. (b) Palatal mucosa dissected and pushed posteriorly – nasal mucosa dissected off the hard palate. (c) Nasal mucosa is sutured against vomer mucosa as far as possible than nasal mucosa on the palatal side are sutured to each other to obtain full closure. (d) Oral mucosa is sutured from back to front. Illustrated by Dr. Ali Murat Kokat
It is similar to von Langenbeck technique. However, the lateral releasing incisions are extended toward the alveolar margins. Therefore, the flap bases extend posteriorly to the palatine pedicles. This method allows closure without tension.
Furlow Double Opposing Z-Plasty (Fig. 2.7)
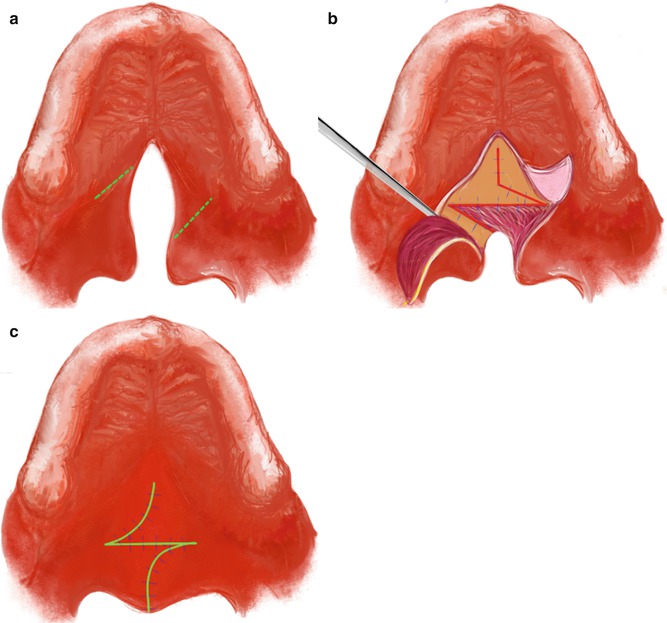
Fig. 2.7
Furlow technique. (a) Two incision opposite to each other end at the hamulus of each side. (b) Two flaps raised with the palatal muscle. (c) Z plasty flaps are transposed and sutured. Illustrated by Dr. Ali Murat Kokat
It is a single-stage palatoplasty, where palatal muscles are overlapped by the transposition of the Z-flaps. Z-plasty results in the lengthening of the soft palate because of its geometry. Therefore, this technique can also be used for the treatment of velopharyngeal incompetence. Lateral tightening can be considered as the main disadvantage of the technique. However, this problem can be overcome by lateral relaxing incisions (Agrawal 2009; Fisher and Sommerlad 2011; Furlow 1986).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


