Gastrointestinal and pancreatic disorders
Key Points
• Dysphagia can signify serious disease
• Coeliac disease is common and often unrecognized
• Inflammatory bowel diseases are serious and may lead to cancer
The Oesophagus
The oesophagus has the single important function of carrying food, liquids and saliva from the mouth to the stomach, achieved by an automatic process of coordinated contractions of its muscular lining (peristalsis), termed deglutition (swallowing). Deglutition involves a complex and coordinated process initiated by sensory impulses from stimulation of receptors on the fauces, tonsils, soft palate, base of the tongue and posterior pharyngeal wall to the brainstem primarily through cranial nerves VII, IX and X. Cricopharyngeal sphincter opening is reflexive and starts when the bolus reaches the posterior pharyngeal wall before reaching this sphincter. The efferent (motor) function of swallowing is mediated by cranial nerves IX, X and XII. Swallowing has three phases; the first is voluntary, the others are involuntary:
■ Phase one is collection and swallowing of the masticated food bolus.
■ Phase two is passage of food through the pharynx into the oesophagus.
Swallowing and respiration are inextricably linked. Neurological damage, such as from a stroke, can lead to disturbed swallowing (dysphagia) and the risk of aspiration into the lungs.
The oesophagus is generally examined by endoscopy. The current ‘gold standard’ examination of swallowing is videofluoroscopy but this is time-consuming and carries a small radiation risk.
Reflux Oesophagitis (Gastro-Oesophageal Reflux Disease)
General aspects
Gastro-oesophageal reflux disease (GORD) is the term used to describe a backflow of acid from the stomach into the oesophagus. One of the most common kinds of dyspepsia, GORD is predisposed to by gastrointestinal disorders (e.g. high acidity of gastric contents; impaired gastro-oesophageal motility) or extragastrointestinal conditions (obesity, stooping, large meals, smoking, alcohol). Although it was at one time considered to be a result of hiatus hernia (diaphragmatic hernia), the relationship between the symptoms and appearances on barium swallow is inconsistent. Hiatal hernias are found in about 25% of all people over age 50 – particularly in women and those who are overweight. They form at the opening (hiatus) in the diaphragm where the oesophagus joins the stomach. The muscle tissue around the hiatus weakens, allowing the upper stomach to herniate through the diaphragm into the chest cavity. Most hernias cause no symptoms but larger ones may allow food and acid to regurgitate into the oesophagus, which can cause chest pain (‘heartburn’).
Clinical features
The usual symptom is an uncomfortable burning sensation behind the sternum, most commonly felt after a meal (‘heartburn’). Acid taste is common. Rare complications may include stricture and iron-deficiency anaemia.
General management
Diagnosis can be confirmed by oesophageal pH monitoring. Conditions to differentiate include candidal oesophagitis, or chemical burns from acids or alkalis, non-steroidal anti-inflammatory drugs (NSAIDs), potassium chloride or tetracyclines. Symptoms can often be effectively relieved by losing weight, raising the head of the bed by at least 10 cm at night and taking frequent small meals with antacids. Proton-pump inhibitors such as omeprazole or lansoprazole are effective but H2-blockers (cimetidine, ranitidine) are often used.
Dental aspects
Gastric contents can have a pH as low as 1 and regurgitation, if chronic, can thus cause dental erosion, typically of the palatal aspects of the upper anterior teeth and premolars; this may be worse if there is impaired salivation. Some patients are convinced that other oral symptoms or diseases are caused by ‘acid’ but, apart from the few genuine cases with persistent regurgitation of gastric contents, this is no more than a folk myth, probably fostered by advertisements for antacids. Other causes of erosion include anorexia nervosa, bulimia (Ch. 27) and alcoholism (Ch. 34).
Post-Cricoid Web
The association of post-cricoid dysphagia, upper oesophageal webs and iron-deficiency anaemia is known as the Paterson–Brown-Kelly syndrome in the UK and the Plummer–Vinson syndrome (PVS) in the USA. The term sideropenic dysphagia has also been used, since the syndrome can feature iron deficiency (sideropenia) but no anaemia. Postulated aetiopathogenic mechanisms include iron and nutritional deficiencies, genetic predisposition and autoimmune factors. The improvement in dysphagia after iron therapy provides evidence for an association between iron deficiency and post-cricoid dysphagia. Moreover, the decline in Paterson–Brown-Kelly syndrome seems to parallel an improvement in nutritional status, including iron supplementation. However, population-based studies have shown no relationship between post-cricoid dysphagia and anaemia or sideropenia.
If a web is suspected, endoscopy should be carried out carefully under direct vision through the upper oesophageal sphincter. The web typically appears as a thin mucosal membrane covered by normal squamous epithelium. Although reports are inconsistent, patients with Paterson–Brown-Kelly syndrome seem to be at greater risk for hypopharyngeal, oesophageal and oral cancers. Patients with Paterson–Brown-Kelly syndrome usually respond well to iron therapy, diet modification and, if necessary, oesophageal dilatation.
Cancer of the Oesophagus
General aspects
Oesophageal cancer is usually squamous cell carcinoma in the upper and middle part of the oesophagus, or adenocarcinoma in the lower third. It is more frequent in older people and in men. Risk factors are shown in Box 7.1.
Clinical features
Early oesophageal cancer usually causes few or no symptoms but later features may include dysphagia, weight loss, pain (in the throat or back, behind the sternum or between the shoulder blades), hoarseness, chronic cough, vomiting or haemoptysis (coughing up blood).
Metastases are typically in the lymph nodes, liver, lungs, brain and bones.
General management
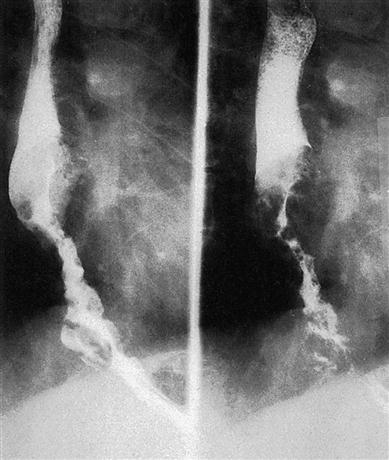
Diagnosis is confirmed by chest radiography, barium swallow (Fig. 7.1), oesophagoscopy (endoscopy), computed tomography (CT), magnetic resonance imaging (MRI) and biopsy. Bone scan and bronchoscopy may be needed.
Surgery is the most common treatment (oesophagectomy). Laser therapy or photodynamic therapy is sometimes used. A stent may be used for palliation; alternatively, a plastic tube or part of the intestine is used to reconnect with the stomach. Radiation therapy may be used alone or with chemotherapy as primary treatment or to shrink the tumour before surgery.
Dental aspects
Patients who have had oesophageal cancer have a greater chance of developing a second cancer in the head and neck area. Paterson–Brown-Kelly syndrome may be associated with a high risk of oral cancer. Rare patients have tylosis and oral leukoplakia.
The Stomach and Intestines
Common features of gastrointestinal disorders include nausea and vomiting, diarrhoea and constipation, though none of these is specific and all have a wide range of causes (Ch. 4).
The Stomach
Gastric products include hydrochloric acid (secreted by parietal cells), pepsin (secreted by chief or peptic cells) and intrinsic factor (secreted by parietal cells). Gastric mucus contains several glycoproteins, which, with bicarbonate, are produced by surface cells and protect the mucosa against erosion.
Hydrochloric acid secretion is stimulated by: hypoglycaemia and mediators including acetylcholine (muscarinic-type receptor); gastrin (from G cells) and synthetic analogues of gastrin (pentagastrin); and histamine (from histaminocytes). Hydrochloric acid secretion is inhibited from higher centres and by low gastric pH and hormones – cholecystokinin, gastric inhibitory peptide (GIP) and secretin (Table 7.1).
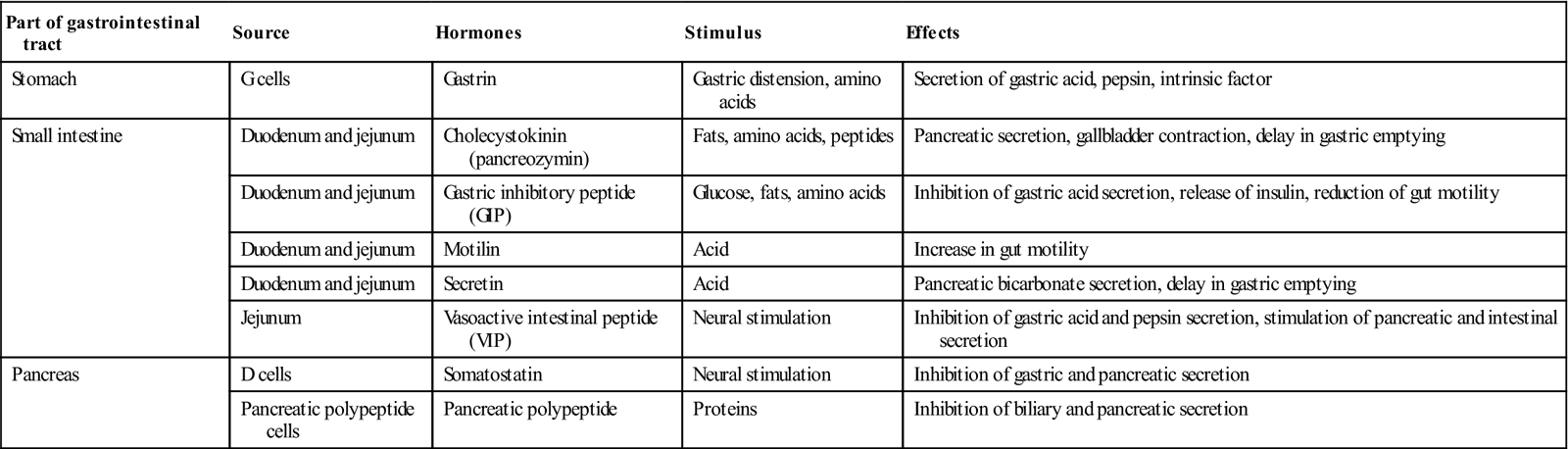
Table 7.1
< ?comst?>
| Part of gastrointestinal tract | Source | Hormones | Stimulus | Effects |
| Stomach | G cells | Gastrin | Gastric distension, amino acids | Secretion of gastric acid, pepsin, intrinsic factor |
| Small intestine | Duodenum and jejunum | Cholecystokinin (pancreozymin) | Fats, amino acids, peptides | Pancreatic secretion, gallbladder contraction, delay in gastric emptying |
| Duodenum and jejunum | Gastric inhibitory peptide (GIP) | Glucose, fats, amino acids | Inhibition of gastric acid secretion, release of insulin, reduction of gut motility | |
| Duodenum and jejunum | Motilin | Acid | Increase in gut motility | |
| Duodenum and jejunum | Secretin | Acid | Pancreatic bicarbonate secretion, delay in gastric emptying | |
| Jejunum | Vasoactive intestinal peptide (VIP) | Neural stimulation | Inhibition of gastric acid and pepsin secretion, stimulation of pancreatic and intestinal secretion | |
| Pancreas | D cells | Somatostatin | Neural stimulation | Inhibition of gastric and pancreatic secretion |
| Pancreatic polypeptide cells | Pancreatic polypeptide | Proteins | Inhibition of biliary and pancreatic secretion |
< ?comen?>< ?comst1?>
< ?comst1?>
< ?comen1?>
Gastric acid secretion in response to various stimuli can be assessed by passing a nasogastric tube and measuring the volume, pH and acid concentration of the aspirate. The response to a meal is regulated by complex hormonal and neural (vagal) mechanisms (see Table 7.1).
Peptic ulcer
General aspects
An ulcer is a break in the continuity of an epithelial surface. Peptic ulcer disease (PUD) develops in or close to acid-secreting areas in the stomach (gastric ulcer) or proximal duodenum (duodenal ulcer). It affects up to 15% of the population, mostly men over the age of 45 years.
Helicobacter pylori, a spiral bacterium that lives in the stomach and duodenum, is the most common contributory cause to peptic ulcers. In the developed world, some 20–50% of normal adults are infected, but the figure is much higher in poor socioeconomic circumstances. Few carriers have disease, but H. pylori can cause increased gastric acid secretion, loss of the mucous protective layer, increased secretion of pepsinogen and increased gastrin release. H. pylori survives in the mucous lining, and resists gastric acid via the enzyme urease, which converts urea (abundant in the stomach from saliva and gastric juices) into bicarbonate and ammonia – both strong bases. This reaction of urea hydrolysis is important for the diagnosis of H. pylori by the ‘breath test’. H. pylori has another defence, in that the immune response cannot reach it, and the polymorphs may release their destructive superoxide radicals on to the stomach-lining cells, causing gastritis and perhaps eventually a peptic ulcer. H. pylori is found in the mouth, especially the gingival sulcus, and believed to be transmitted orofaecally. It is possible that H. pylori could be transmitted from the stomach to the mouth through gastro-oesophageal reflux and then be transmitted through oral contact.
PUD is also associated with raised gastrin levels, as in Zollinger–Ellison syndrome (a gastrin-producing tumour; high serum calcium provokes gastrin release) and chronic renal failure (poor gastrin metabolism). Other factors that predispose to peptic ulceration include NSAIDs, corticosteroids, smoking, alcohol, diet and stress. There are genetic influences: first-degree relatives have a threefold risk and there is an association with blood group O.
Clinical features
The main feature of PUD is epigastric pain, often relieved by ant-acids. Many of those affected have no symptoms and the first sign may be one of the complications – haemorrhage, perforation or pyloric obstruction (stenosis) with vomiting.
General management
Patients less than 45 years old who present with typical ulcer symptoms should be screened for H. pylori. Four tests are used to detect the bacterium:
■ Blood test for antibodies to H. pylori – shows past or present infection
■ Urea breath test – shows H. pylori infection
■ Stool antigen test – tests for the presence of H. pylori antigens in faeces (stool)
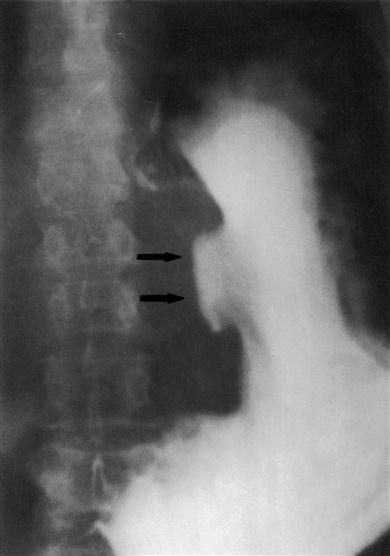
Studies of gastric acid or serum gastrin levels may be helpful and, if gastric outlet obstruction is suspected, a barium meal may be diagnostic-ally useful (Fig. 7.2). Management of PUD involves conservative measures: dietary modification (frequent small meals with no fried foods); smoking cessation; alcohol moderation; and treatment of any H. pylori. Individuals who are H. pylori-positive should be given ‘triple therapy’, usually for 7 days, to eradicate infection. This normally is effective in over 90% with little risk of relapse and consists of a proton-pump inhibitor (esomeprazole, lansoprazole, omeprazole, pantoprazole or rabeprazole) and antibiotics (amoxicillin, clarithromycin and metronidazole). An additional reason to treat H. pylori infection is that it may lead to gastric cancer or mucosa-associated lymphoid tissue (MALT) lymphomas.
PUD that is H. pylori-negative is usually associated with NSAID use. Drugs that block histamine (H2) receptors, such as cimetidine and ranitidine, are therefore used to reduce gastric acid secretion. Prostaglandin analogues such as misoprostol promote healing in PUD and are indicated in patients from whom NSAIDs cannot be withdrawn. Surgery is usually reserved for those with complications; gastric ulcers may be managed by antrectomy with gastroduodenal anastomosis or partial gastrectomy, while duodenal ulcers are managed with vagotomy and pyloroplasty (rarely).
Dental aspects
Gastric acid regurgitation can cause severe dental erosion (perimylolysis), typically of the palatal aspects of the upper anterior teeth and premolars. H. pylori may be transmitted in saliva but dental health-care professionals do not appear to be at particular risk from infection. There are conflicting findings as to whether dental plaque or dentures are an important reservoir for H. pylori and significant in transmission of the organism. There may be an association with halitosis.
Gastric surgery may result in attacks of hypoglycaemia. After resection, deficiencies of vitamin B12, folate or iron may cause ulcers, sore tongue or angular stomatitis. Drugs such as aspirin and other NSAIDs and corticosteroids that cause gastric irritation, or promote bleeding, and should not be given to patients with peptic ulcers.
Labial vascular anomalies may be associated with PUD.
Oral adverse effects from medications may include:
■ dry mouth from proton-pump inhibitors, pirenzepine and sucralfate
Antacids impede absorption of ciprofloxacin, erythromycin, metronidazole and tetracyclines. Cimetidine and omeprazole may delay clearance of lidocaine and benzodiazepines but the effect is rarely clinically significant.
Cancer of the stomach
General aspects
Stomach cancer, usually adenocarcinoma, is common. Men are affected nearly twice as often as women. The aetiology of gastric cancer is unclear (Box 7.2).
Clinical features
Early symptoms of gastric cancer may closely mimic those of peptic ulcer – indigestion or vague upper abdominal pain. Later, there may be anorexia, loss of weight, nausea, vomiting, haematemesis or melaena (black and tarry stools with blood). Anaemia may develop. The tumour spreads locally later and leads to pain, and may obstruct the intestine to cause vomiting, or the bile duct to cause jaundice. Metastases are mainly to liver, peritoneum (causing ascites), lungs, bones or brain.
General management
The lesion may show on barium imaging and the diagnosis is usually confirmed by gastroscopy and biopsy, but is often delayed by the lack of early symptoms.
Most patients are treated by surgery but frequently this is only palliative. The prognosis is poor, with about a 7% 5-year survival rate (Ch. 22).
Dental aspects
Anaemia or obstructive jaundice may complicate dental treatment. Oral effects of anaemia (glossitis, ulcers, angular stomatitis) can be an initial sign. It is important to remember that iron deficiency usually results from chronic haemorrhage, in a male often from the gastro-intestinal tract, and then sometimes due to an ulcer or neoplasm in the stomach or large bowel.
Orofacial metastases from gastric carcinoma are rare, usually in the body of the mandible, and may cause swelling, pain, paraesthesia, loosen-ing of teeth or sockets that fail to heal; they may be found as ragged radiolucent areas, sometimes with tooth root resorption. Occasionally, metastases may be first detected in a lower cervical (supraclavicular, or Virchow) lymph node, usually on the left side (Troisier sign).
The Small Intestine
The small intestine is the main site of food digestion, which depends on intestinal and pancreatic enzymes acting on food previously exposed to salivary amylase, gastric acid and pepsin. This is where food absorption chiefly occurs.
Iron and folate are absorbed in the duodenum, most other substances in the jejunum. Bile salts facilitate the absorption of fats and the fat-soluble vitamins (A, D, E and K). Gastric intrinsic factor from the stomach parietal cells is needed for vitamin B12 absorption, which occurs in the terminal ileum.
Small intestine disease causes malabsorption, with diarrhoea or steatorrhoea (fatty stools), sometimes abdominal discomfort, and deficiency states leading to lassitude, weakness, loss of weight or failure to thrive, and anaemia.
Diseases of the small intestine of most significance include coeliac disease and Crohn disease. Other causes of problems include surgery, infestations and drugs. For example, olmesartan can cause a sprue-like disease (diarrhoea, weight loss and villous atrophy, which resolves after discontinuation of the drug).
Coeliac disease
Coeliac disease (CD; gluten-sensitive enteropathy; coeliac sprue, non-tropical sprue) is the most common genetic disease in Europe, where up to 1 in 250 people have it. It is rare in Africans, Chinese or Japanese. CD is strongly associated with genes on chromosome 6, on a genetic background of HLA-DQw2 or DRw3, and may have a familial tendency.
CD is a hypersensitivity or toxic reaction of the small intestine mucosa to the gliadin component of gluten (prolamine), a group of proteins found in all forms of wheat (including durum, semolina, spelt, kamut, einkorn and faro), related grains (rye, barley, triticale) and possibly oats. Ingestion of gluten causes destruction of jejunal villi (villous atrophy) and inflammation, leading to malabsorption. Coeliac disease may be associated with autoimmune disorders (Box 7.3). Other food sensitivities or lactose intolerance may also be associated.
Clinical features
CD is one of the great mimics in medicine. It may present at any age and many affected individuals are asymptomatic, but CD can result in malabsorption (leading to growth retardation, vitamin and mineral deficiencies, which may in turn lead to anaemia, osteomalacia, bleeding tendencies and neurological disorders), abdominal pain, steatorrhoea and behavioural changes (Fig. 7.3). Intestinal lymphomas arise in about 6% of individuals.
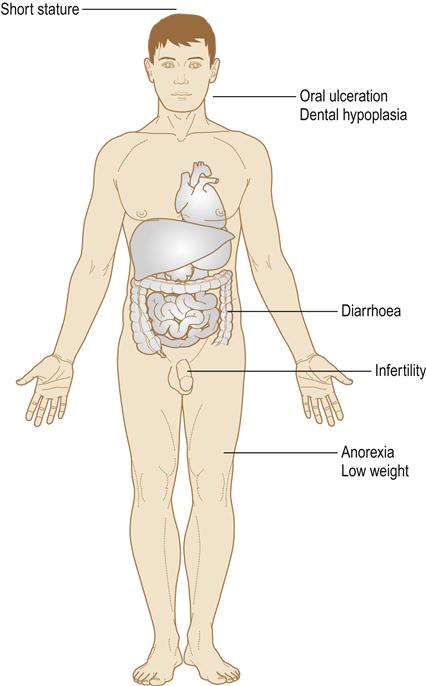
General management
It is important to diagnose CD and/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses