Treatment of Gingival Enlargement
Paulo M. Camargo, Fermin A. Carranza, Flavia Q. Pirih and Henry H. Takei
The treatment of gingival enlargement is based on an understanding of the cause and underlying pathologic changes of this condition (see Chapter 16). Gingival enlargements are of special concern to the patient and the dentist because they pose problems that involve plaque control, function (including mastication, tooth eruption, and speech), and aesthetics. Because gingival enlargements differ with regard to cause, the treatment of each type is best considered individually.
Drug-Associated Gingival Enlargement
Gingival enlargement has been associated primarily with the administration of three different types of drugs: anticonvulsants, calcium channel blockers, and the immunosuppressant cyclosporine. Chapter 16 provides a comprehensive review of the clinical and microscopic features and the pathogenesis of gingival enlargement induced by these drugs. There is more limited evidence that other drugs may also induce gingival enlargement, albeit at a lower prevalence and with a lesser severity.5
The examination of cases of drug-induced gingival enlargement reveals the overgrown tissues to have two components: fibrotic, which are caused by the drug, and inflammatory, which are induced by bacterial plaque. Although the fibrotic and inflammatory components present in the enlarged gingiva are the result of distinct pathologic processes, they almost always are observed in combination. The role of bacterial plaque in the overall pathogenesis of drug-induced gingival enlargement is not clear. Some studies indicate that plaque is a prerequisite for gingival enlargement,12 whereas others suggest that the presence of plaque is a consequence of its accumulation caused by the enlarged gingiva.
Treatment Options
First, consideration should be given to the possibility of discontinuing the drug10,13 or changing the medication. These possibilities should be examined with the patient’s physician. Simple discontinuation of the offending drug is usually not practical, but its substitution with another medication may be an option. If any drug substitution is attempted, it is important to allow for a 6- to 12-month period to elapse between discontinuation of the offending drug and the possible resolution of gingival enlargement before a decision to implement surgical treatment is made.
Alternative medications to the anticonvulsant phenytoin include carbamazepine8 and valproic acid, both of which have been reported to induce gingival enlargement to a lesser degree.
For patients who are taking nifedipine, which has a reported prevalence of gingival enlargement of up to 44%, other calcium channel blockers such as diltiazem or verapamil may be viable alternatives; their reported prevalences of inducing gingival enlargement are 20% and 4%, respectively.4,11,18 In addition, consideration may be given to the use of another class of antihypertensive medications rather than calcium channel blockers, because none of these drugs are known to induce gingival enlargement.
Drug substitutions for cyclosporine are more limited. Tracolimus is another immunosuppressant that has been used with organ transplant recipients.25 The incidence of gingival enlargement in patients receiving tacrolimus therapy is approximately 65% lower than that of individuals who are receiving cyclosporine.2 Clinical trials have also shown that the substitution of cyclosporine with tacrolimus results in a significant decrease in the severity of gingival enlargement as compared with patients who are kept on cyclosporine therapy.14,23,28 In another study,16 the same drug substitution resulted in a strong decrease in or the complete resolution of gingival enlargement in more than 70% of the patients who initially presented with cyclosporine-induced gingival enlargement. Therefore, the dental practitioner should consult with the treating transplantation physician to investigate the possibility of a change in immunosuppressant therapy as one of the steps in the treatment of cyclosporine-induced gingival enlargement. Patients who take cyclosporine in combination with a calcium channel blocker tend to present an overall lower prevalence of and less severe gingival enlargement if the anti-hypertensive drug is amlodipine as compared with nifedipine.15
The administration of the antibiotic azithromycin has been shown to decrease the severity of gingival enlargement induced by the administration of cyclosporine. A 3-day course of systemic azithromycin significantly decreased gingival enlargement, and the effect was observed as early as 7 to 30 days after the initiation of antibiotic therapy.27 The use of azithromycin to decrease cyclosporine-induced gingival enlargement resulted in significantly greater changes than those observed with an improvement in oral hygiene.21 The topical administration of azithromycin in the form of a toothpaste also decreased the severity of cyclosporine-induced gingival enlargement.2
Second, the clinician should emphasize plaque control as the first step in the treatment of drug-induced gingival enlargement. Although the exact role played by bacterial plaque is not well understood, evidence suggests that good oral hygiene, chemotherapeutics,24 and the frequent professional removal of plaque decrease the degree of gingival enlargement and improve overall gingival health.10,12,26 The presence of drug-induced enlargement is associated with pseudopocket formation, frequently with abundant plaque accumulation, which may lead to the development of periodontitis; meticulous plaque control therefore helps to maintain attachment levels. In addition, adequate plaque control may help to prevent the recurrence of gingival enlargement in surgically treated cases.
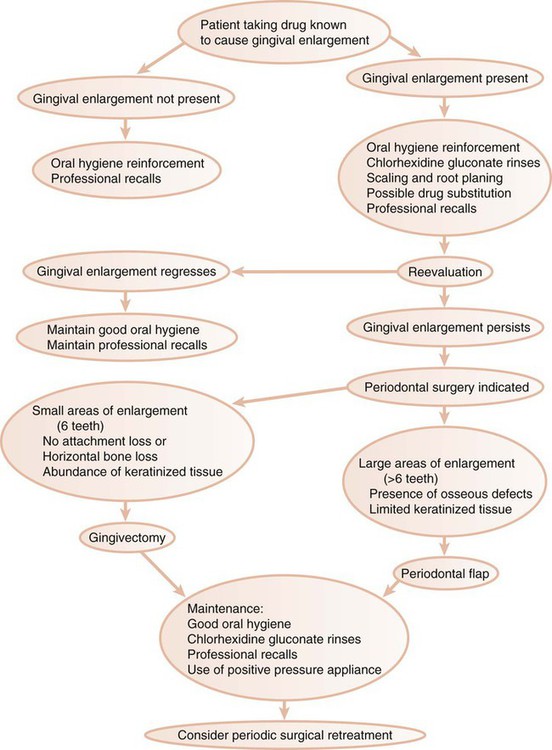
Figure 58-1 presents a decision tree that outlines the sequence of events and options for the treatment of drug-induced gingival enlargement.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses