Pathologic Tooth Migration
A Case Report*
Pathologic tooth migration (PTM) is a common complication of moderate-to-severe periodontitis.1,2 The prevalence of PTM among periodontal patients has been reported to range from 30.03% to 55.8%. It occurs most frequently in the anterior region, but posterior teeth can also be affected. There are many types of pathologic tooth migration: diastema, extrusion, rotation, facial flaring, and drifting into edentulous spaces. Some of the important factors are poor periodontal support as the result of periodontal disease and the eventual loss of teeth, which changes the forces exerted on the remaining dentition. Later, if the missing teeth are not replaced, especially the first molars, the maxillary incisors are forced labially and laterally, which leads to the extrusion of the anterior teeth and the resulting diastema. Teeth mobility increases, and the second and third molars tilt mesially, which results in a reduced vertical dimension. This can also lead to an anterior overbite, and the mandibular incisors occlude near or on the palatal gingival margin of the maxillary anterior dentition.
Case Report
The patient’s complaints were as follows:
• A reduced ability to bite because of increased tooth mobility in the maxillary anterior area
Oral Examination
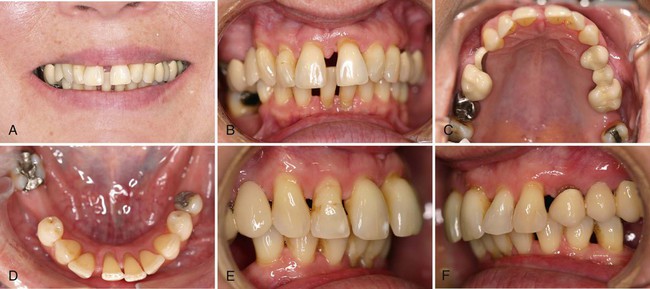
There were symptoms of PTM in the anterior region (Supplement A Figure 51-1). Diastemas were present between the maxillary incisors, as well as the mandibular dentition. The patient confirmed that in the past the position of her anterior teeth was normal and that her teeth “were all touching.” The maxillary and mandibular incisors displayed extrusion, rotation, and facial flaring. There was a pronounced anterior overbite.
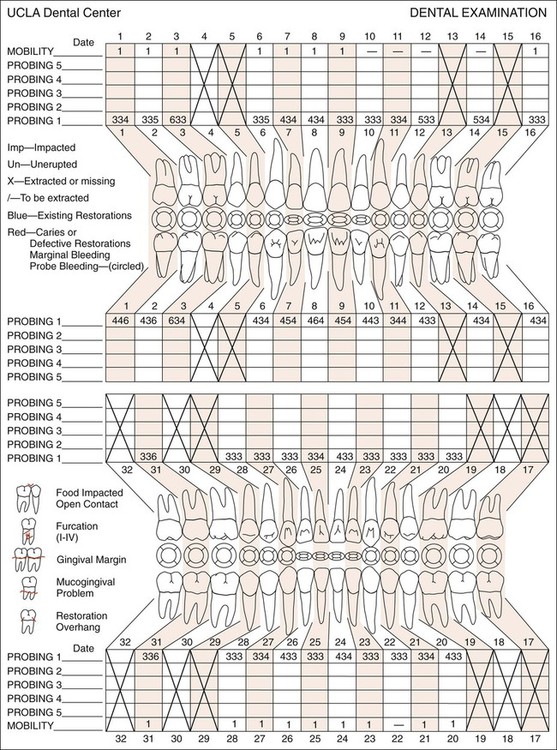
Periodontal Assessment
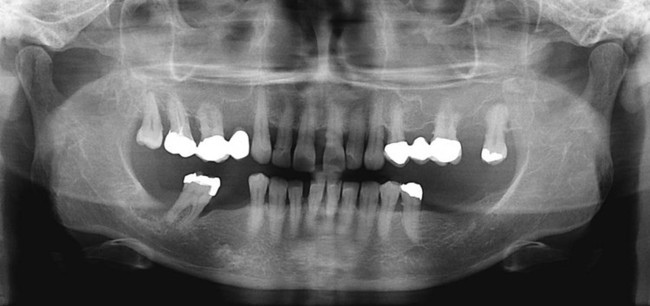
To assess the extent of the periodontal disease, a full periodontal examination was accomplished. The examination included pocket probing and evaluation of gingival recession and tooth mobility. Supplement A Figure 51-2 indicates the extensive periodontal involvement of the maxillary arch. Periodontal pockets that involved the interdental and lingual areas ranged from 4 to 6 mm. The majority of the anterior teeth presented recession that measured 2 mm. Increased mobility was noted for most teeth, especially tooth #31. Most of the furcations were class I.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses