Implants
Byron W. Benson and Vivek Shetty
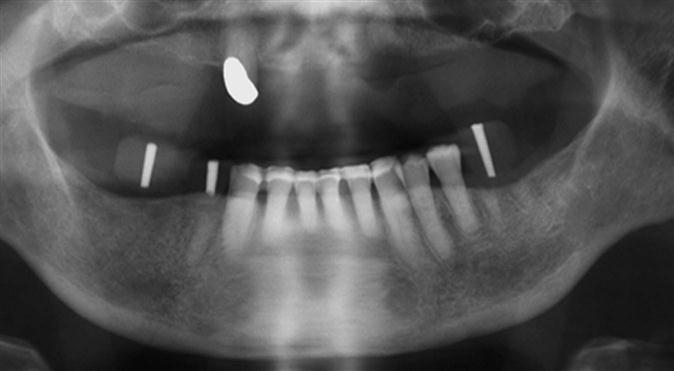
Few advances in dentistry have been as remarkable as the use of dental implants (Fig. 33-1) to restore orofacial form and function. Implant technology has enabled the dentist to help patients regain the ability to chew normally and function without embarrassment. With the application of precise surgical and restorative techniques, implant-facilitated restorations provide a predictable and successful rehabilitation of patients with a broad spectrum of prosthodontic needs. The predictable results of contemporary implant systems derive in part from increasingly sophisticated imaging techniques and software programs used in all phases of implant treatment. These imaging modalities contribute information for every stage of the treatment, from presurgical diagnosis and treatment planning, through surgical placement and postoperative assessment of the implant, to the prosthetic restoration and long-term maintenance phase.
Acceptance of dental implantology as an integral part of conventional practice requires the general dentist to be knowledgeable of implant imaging techniques and their clinical application. With the exception of occasionally used subperiosteal, blade, and transosteal implant systems, dental implants used today are almost exclusively root-form devices (see Fig. 33-1) embedded within the jaw bone (endosseous implants). This chapter focuses on current imaging concepts and describes the applications and value of imaging techniques in the various stages of contemporary implant dentistry.
Diagnostic Imaging
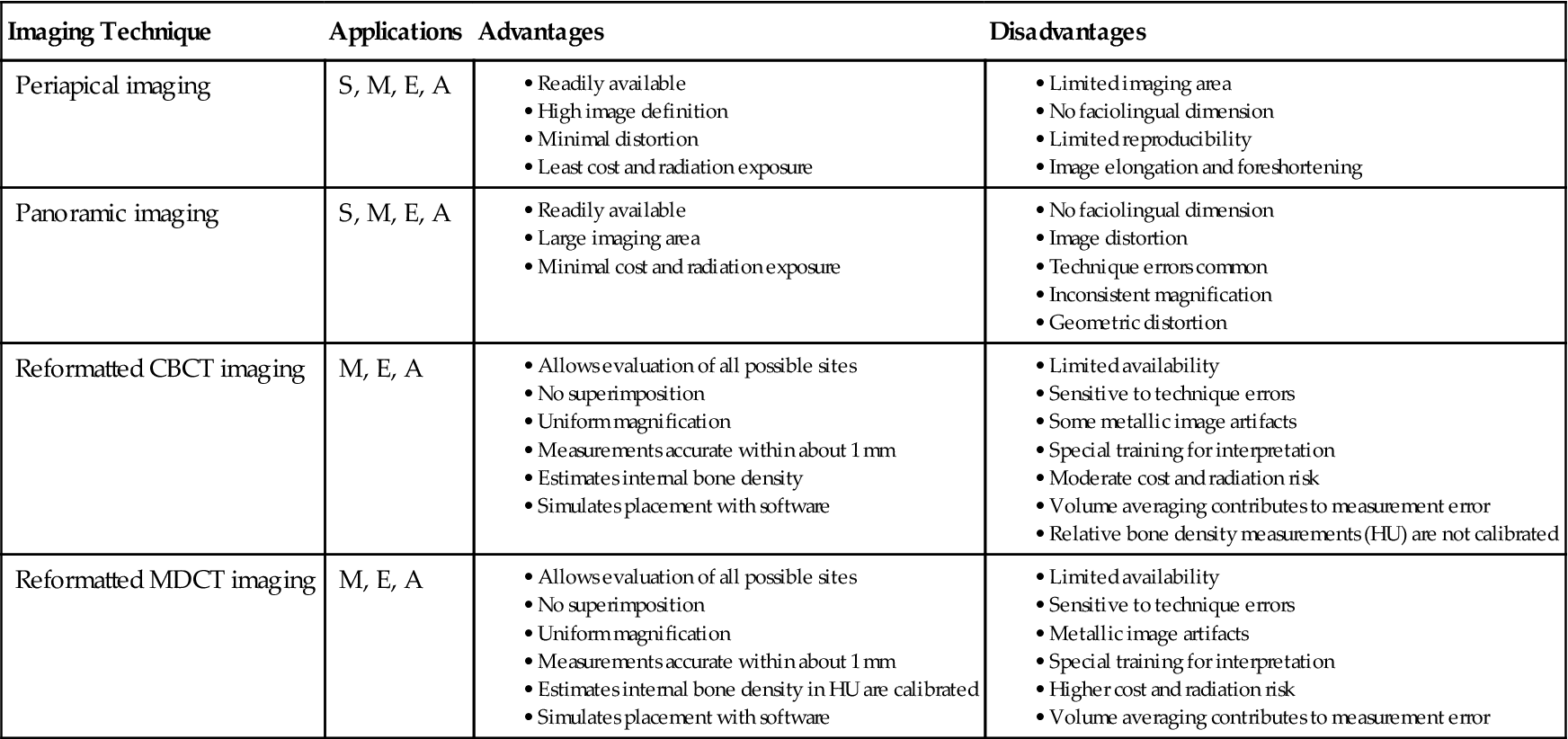
Commonly used two-dimensional imaging, such as panoramic and periapical images, is generally useful and cost-effective for patient selection and initial assessment. However, these modalities lack the cross-sectional visualization or interactive image analysis that can be obtained with the more sophisticated imaging techniques now available. Numerous imaging techniques can be applied to various phases of implant case management (Table 33-1). The selection of a specific imaging technique should be based on the examination best suited to provide the information required by the implant team—the restorative dentist, surgeon, and radiologist (Table 33-2).
TABLE 33-1
| Stage of Treatment | Radiographic Procedures |
| Initial examination | |
| Preoperative site specific | |
| Postoperative |
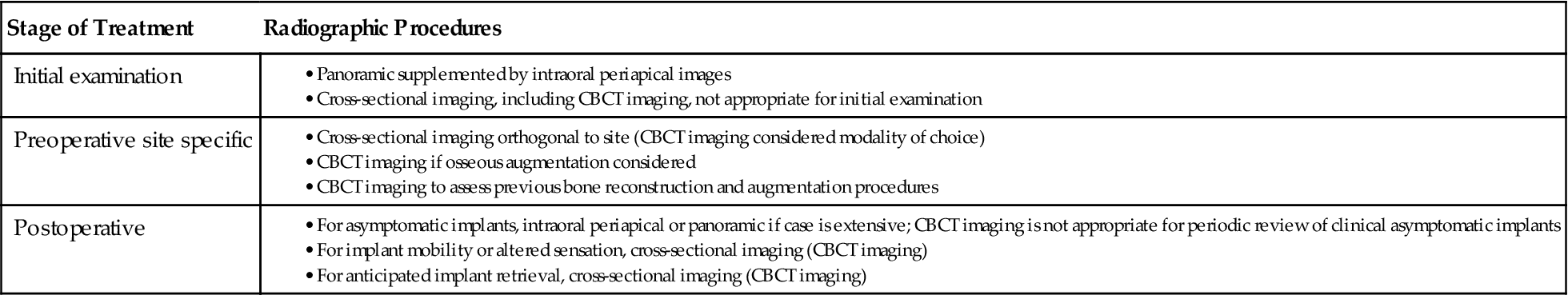
CBCT, Cone-beam computed tomographic.
From Tyndall DA, Price JB, Tetradis S, et al: Position statement of the American Academy of Oral and Maxillofacial Radiology on selection criteria for the use of radiology in dental implantology with emphasis on cone beam computed tomography, Oral Surg Oral Med Oral Pathol Oral Radiol 113:817–826, 2012.
Imaging Techniques
The ideal imaging technique for dental implant care should have several essential characteristics, including the ability to visualize the implant site in the mesiodistal, faciolingual, and superoinferior dimensions; the ability to allow reliable, accurate measurements; a capacity to evaluate trabecular bone density and cortical thickness; a capacity to correlate the imaged site with the clinical site; reasonable access and cost to the patient; and minimal radiation risk. Usually a combination of imaging techniques is used. Available imaging techniques include intraoral (film and digital), cephalometric, and panoramic imaging; cone-beam computed tomographic (CBCT) imaging; and multidetector computed tomographic imaging (MDCT). A review of these imaging techniques as applied to dental implant case management is provided here.
Intraoral Imaging
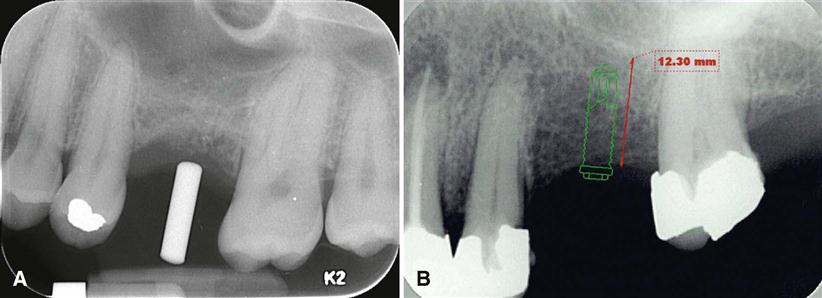
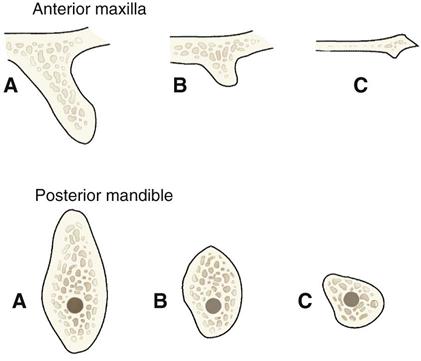
Intraoral images may be acquired on film or as digital images. Periapical and occlusal radiographs provide images with superior resolution and sharpness. Periapical radiographs commonly are used to evaluate the status of adjoining teeth and remaining alveolar bone in the mesiodistal dimension. They also have been used for determining vertical height, morphology, and bone quality (bone density, amount of cortical bone, and amount of trabecular bone). Although readily available and relatively inexpensive, periapical radiography has geometric and anatomic limitations. When teeth are present, images are typically made with the paralleling technique, creating an image with minimal foreshortening and elongation (Fig. 33-2). Because of variations in the morphology of the residual edentulous alveolar ridge (Fig. 33-3), the ridge may not have the same “long axis” as a tooth. The position of the image receptor may not result in an accurate display of the height of the alveolar ridge as a result of image foreshortening or elongation. Also, placing the image receptor either superior or inferior enough to capture an image of the entire maxillary or mandibular ridge can prove to be challenging. Reportedly, 25% of mandibular periapical radiographs do not demonstrate the mandibular canal. In cases in which the canal is identifiable, only 53% of measurements from the alveolar crest to the superior wall of the mandibular canal are accurate within 1 mm.
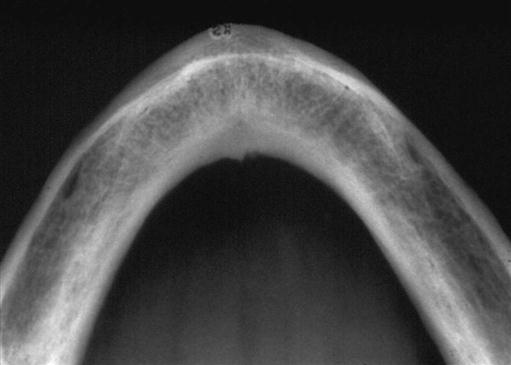
Because periapical images are unable to provide any cross-sectional information, occlusal radiographs may be used occasionally to determine the faciolingual dimensions of the mandibular alveolar ridge (Fig. 33-4). Although useful, the occlusal image records only the widest portion of the mandible, which typically is located inferior to the alveolar ridge. This image may give the clinician the impression that more bone is available in the cross-sectional (faciolingual) dimension than actually exists. The occlusal technique is not useful in imaging the maxillary arch because of anatomic limitations.
Lateral and Lateral-Oblique Cephalometric Imaging
Lateral cephalometric imaging provides an image of known magnification (usually 7% to 12% for midline structures) that documents axial tooth inclinations and the dentoalveolar ridge relationships in the midline of the jaws. The soft tissue profile also is apparent on this film and can be used to evaluate profile alterations after prosthodontics rehabilitation. However, this projection can provide a cross-sectional view of only the maxillary and mandibular midline. Images of nonmidline structures are superimposed on the contralateral side, complicating the evaluation of other implant sites. Occasionally, lateral-oblique cephalometric radiographs are used with one side of the mandibular body positioned parallel to the film cassette. Image magnification on these views is unpredictable because the body of the mandible is not the same distance from the film as is the rotation center of the cephalostat (used to calculate object-receptor distance for image magnification values). Thus, measurements made from these images are unreliable. In general, cephalometric images have significant limitations but may be useful in the placement of some implants near the midline for overdentures.
Panoramic Imaging
Although the resolution and sharpness of panoramic radiographs are less than those of intraoral radiographs, panoramic projections provide a broader visualization of the jaws and adjoining anatomic structures. Panoramic units are widely available, making this imaging technique useful and popular as a screening and assessment instrument for preliminary estimations of crestal alveolar bone and cortical boundaries of the mandibular canal, maxillary sinus, and nasal fossa (Fig. 33-5).
Information acquired from panoramic images must be applied judiciously because this technique has significant limitations as a definitive presurgical planning tool. Angular measurements on panoramic radiographs tend to be accurate, but linear measurements are not. Image size distortion (magnification) varies significantly between images acquired on different panoramic units and even within different areas of the same image. Vertical measurements are unreliable owing to foreshortening and elongation of the anatomic structures because the central ray of the x-ray beam is perpendicular neither to the long axis of the anatomic structures nor to the plane of the image receptor. The negative vertical angulation of the x-ray beam also causes lingually positioned objects, such as mandibular tori, to be projected superiorly on the film, resulting in an overestimation of vertical bone height. The anatomic vertical axis varies within the image, particularly in nonmidline areas. Compared with contact radiographs of dissected anatomic specimens, only 17% of panoramic measurements between the alveolar crest and superior wall of the mandibular canal were found to be accurate within 1 mm.
Similarly, dimensional accuracy in the horizontal plane of panoramic radiographs is highly dependent on the position of the structures of interest relative to the central plane of the image layer. The horizontal dimension of images of structures located facial or lingual to the central plane but still within the image layer tends to be minified or magnified, respectively. The degree of horizontal size distortion is difficult to ascertain on panoramic radiographs because the shape of the image layer is configured to a population average, and the anatomic morphology of only a few individuals conforms totally to that image layer. Horizontal image magnification with panoramic radiographs ranges from 0.70 to 2.2 times the actual size, which some manufacturers report as a 1.25 average magnification (at the central plane of the image layer). Errors in patient positioning can further exacerbate measurement error in the horizontal dimension. The deficient dimensional accuracy of the two-dimensional panoramic image is further limite/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses