Necrotizing Ulcerative Periodontitis
Necrotizing ulcerative periodontitis (NUP) may be an extension of necrotizing ulcerative gingivitis (NUG) into the periodontal structures that leads to periodontal attachment and bone loss. Alternatively, NUP and NUG may be different diseases. To date, there is little evidence to support the progression of NUG to NUP or to establish a relationship between the two conditions as a single disease entity. However, numerous clinical descriptions and case reports of NUP clearly demonstrate many clinical similarities between the two conditions. Until a distinction between NUG and NUP can be proved or disproved, it has been suggested that NUG and NUP be classified together under the broader category of necrotizing periodontal diseases, although with differing levels of severity.1,19
NUG has been recognized and described in the literature for centuries.22 The features of NUG are presented in Chapter 10.
The term necrotizing ulcerative periodontitis was first adopted at the 1989 World Workshop in Clinical Periodontics.3 It was changed from the 1986 term necrotizing ulcerative gingivoperiodontitis, which represented the condition of recurrent NUG that progresses to a chronic form of periodontitis that includes attachment and bone loss. The adoption of NUP as a disease entity occurred in 1989 when there was a heightened awareness and an increase in the number of necrotizing periodontitis cases being diagnosed and described in the literature. Specifically, more cases of NUP were being described among immunocompromised patients, especially those who were human immunodeficiency virus (HIV) positive or who had acquired immunodeficiency syndrome (AIDS). In 1999, the subclassifications of NUG and NUP were included as separate diagnoses under the broader classification of “necrotizing ulcerative periodontal diseases.”1
Clinical Features
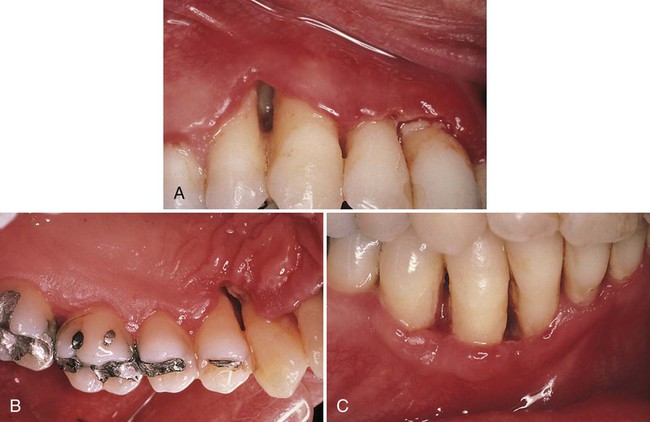
The distinguishing feature of NUP is the destructive progression of the disease, which includes periodontal attachment and bone loss. Deep interdental osseous craters typify periodontal lesions of NUP (Figure 24-1). However, “conventional” periodontal pockets with deep probing depth are not found, because the ulcerative and necrotizing nature of the gingival lesion destroys the marginal epithelium and connective tissue, thereby resulting in gingival recession. Periodontal pockets are formed because the junctional epithelial cells remain viable and can therefore migrate apically to cover areas of lost connective-tissue attachment. The necrosis of the junctional epithelium in patients with NUG and NUP creates an ulcer that prevents this epithelial migration, and a pocket cannot form. Advanced lesions of NUP lead to severe bone loss, tooth mobility, and ultimately tooth loss. In addition to these manifestations, as previously mentioned, patients with NUP may present with oral malodor, fever, malaise, or lymphadenopathy.
Microscopic Findings
In a study involving the use of transmission electron microscopy and scanning electron microscopy of the microbial plaque overlying the necrotic gingival papillae, Cobb and colleagues4 demonstrated striking histologic similarities between NUP in HIV-positive patients and previous descriptions of NUG in HIV-negative patients. Microscopic examination revealed a surface biofilm composed of a mixed microbial flora with different morphotypes and a subsurface flora with dense aggregations of spirochetes (i.e., the bacterial zone). Below the bacterial layers were dense aggregations of polymorphonuclear leukocytes (PMNs) (i.e., the neutrophil-rich zone) and necrotic cells (necrotic zone). The biopsy technique used in this study did not allow for the observation of the deepest layer and thus was not able to identify the spirochetal infiltration zone, which is classically described in NUG lesions. In addition to the NUG-like microscopic features of NUP described in this study, high levels of yeasts and herpes-like viruses were observed. This latter finding is most likely indicative of the conditions afforded to opportunistic microbes in the immunocompromised host (i.e., HIV-positive patients).
Patients with Human Immunodeficiency Virus/Acquired Immunodeficiency Syndrome
Gingival and periodontal lesions with distinctive features are frequently found in patients with HIV infection and AIDS. Many of these lesions are atypical manifestations of inflammatory periodontal diseases that arise during the course of HIV infection and as a result of the patient’s concomitant immunocompromised state. Linear gingival erythema, NUG, and NUP are the most common HIV-associated periodontal conditions reported in the literature.20 Chapter 19 provides detailed descriptions of these and other atypical periodontal diseases that occur in the patient with HIV.
NUP lesions found in patients with HIV or AIDS can present with features similar to those seen in HIV-negative patients. Alternatively, NUP lesions in patients with HIV or AIDS can be much more destructive and frequently result in complications that are extremely rare among patients without HIV or AIDS. For example, periodontal attachment and bone loss associated with NUP in an HIV-positive patient may be extremely rapid. Winkler and colleagues30 described cases of NUP in HIV-positive patients with teeth that lost more than 90% of periodontal attachment and 10 mm of bone over a 3- to 6-month period. Ultimately, many of these lesions resulted in tooth loss. Other complications reported in this population included the progression of the lesions to involve large areas of soft-tissue necrosis, with the exposure of bone and the sequestration of bone fragments. This type of severe, progressive lesion with extension into the vestibular area and the palate is referred to as necrotizing ulcerative stomatitis (see Figure 19-31).
The reported prevalence of NUP among patients with HIV infection varies.6,13,20,22 Riley and colleagues23 described only two cases of NUP in 200 HIV-positive patients (1%), whereas Glick and colleagues13 found a prevalence of 6.3% for NUP cases in a prospective study of 700 HIV-positive patients. Variations in reported findings may be related to differences in the populations studied (e.g., intravenous drug users versus homosexuals versus patients with hemophilia) and differences in the immune statuses of the study subjects.
Necrotizing forms of periodontitis appear to be more prevalent among patients with more severe immunosuppression.20,21 Case reports have depicted NUP as a progressive extension of HIV periodontitis (i.e., chronic to necrotic progression).24 Glick and colleagues13,14 found a high correlation between the diagnosis of NUP and immunosuppression in HIV-positive patients. Those patients who presented with NUP were 20.8 times more likely to have CD4+ counts of less than 200 cells/mm3 as compared with HIV-positive patients without NUP. The authors consider a diagnosis of NUP to be a marker of immune deterioration and a predictor of the diagnosis of AIDS.13 Others have suggested that NUP may be used as an indicator of HIV infection in undiagnosed patients. Shangase and colleagues27 reported that a diagnosis of NUG or NUP in systemically healthy, asymptomatic South-African patients was strongly correlated with HIV infection. Of patients presen/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses