CHAPTER 20
Dental Implant Repositioning by Osteotomy in the Esthetic Zone
A step back can be incautious too.
—Wieslaw Brudzinski
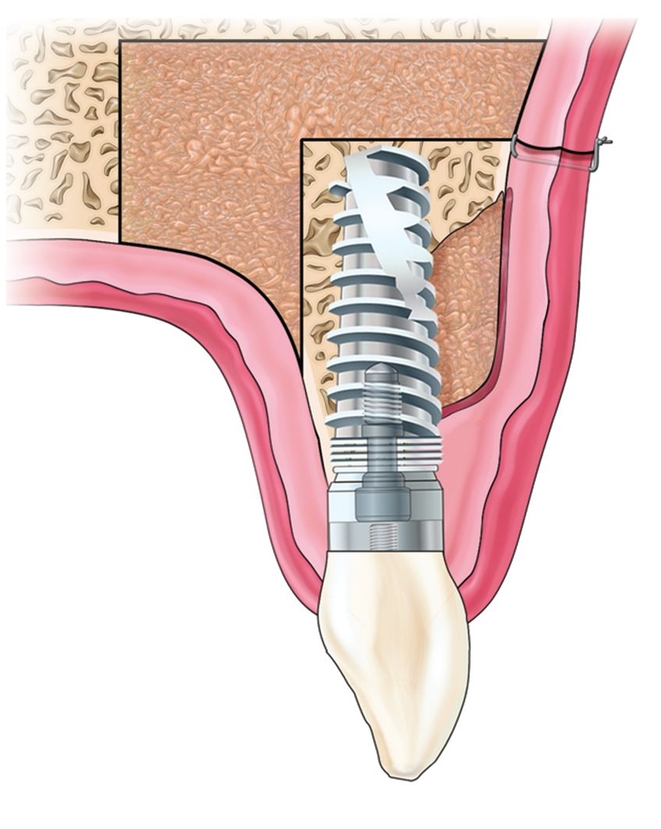
Implant placement following dental extraction with immediate provisional restoration has often led to late-term gingival recession, resulting in an unesthetic, relatively long crown.1,2 When dehiscence of the facial surface of the implant occurs, the restoration presents as a dark shadow beneath the soft tissue.3 If the dehiscence is severe, screw threads become exposed, and a chronic peri-implant infection may develop.4 The natural progression of a chronically infected implant is further bone loss that can extend circumferentially around the implant and involve supporting bone of adjacent teeth.5 When bone loss progresses, subpapillary bone is lost, and soft tissue ablation with papillary loss generally follows.6,7
The choice of treatment in these situations, especially when they arise in the esthetic zone, is controversial and unclear.8 Many clinicians choose to perform various salvage procedures such as resubmergence of the implant after disinfection with citric acid, followed by bone or soft tissue grafting.9–11 Other clinicians prefer to remove the implant and bone graft the site to develop a foundation for implant retreatment.12,13 Apical repositioning flaps have been used in attempts to cover exposed implant surfaces, but these measures are generally unsuccessful.14–16
 Treatment Algorithm
Treatment Algorithm
When peri-implant bone loss is severe and chronic infection is present, each treatment alternative represents a very difficult course of treatment with a high incidence of failure. The question arises: What should be done and under what criteria? No definitive parameters have been established; in particular, no systematic approach has been developed to determine what is most important and what is least important in retreatment of an esthetically failed dental implant restoration. This chapter proposes a decision tree algorithm that ranks criteria, that is, pertinent questions regarding treatment for a “failed” implant restoration in the presence of osseointegration.
Application
These questions serve as a decision tree that establishes whether or not bodily movement of an implant in the esthetic zone can be accomplished (Fig 20-1). The diagnostic parameters that must be assessed include the degree of osseointegration, the extent of implant malpositioning, the depth of the implant platform, the presence of facial bone integrity, the proximity to adjacent subpapillary bone, the presence of apical bone above the implant, and the existence of adequate interarch space. All criteria must be judged to be favorable before the implant can be repositioned vertically by an osteotomy procedure.
Although the algorithm provides a rationale for surgical repositioning of an implant, the decision to proceed with an osteotomy should not be taken lightly; there is already a significant complication present that can be compounded further by an osteotomy procedure that is difficult to perform even for those who are experienced with single-tooth osteotomy surgery. A complete loss of the osteotomy segment caused by poor surgical technique would probably require iliac bone graft reconstruction or grafting with bone morphogenetic protein 2 as well as other secondary procedures. For these reasons, orthognathic surgeons have avoided single-tooth osteotomies because the blood supply is easily disturbed when limited to palatal flap vascularity.
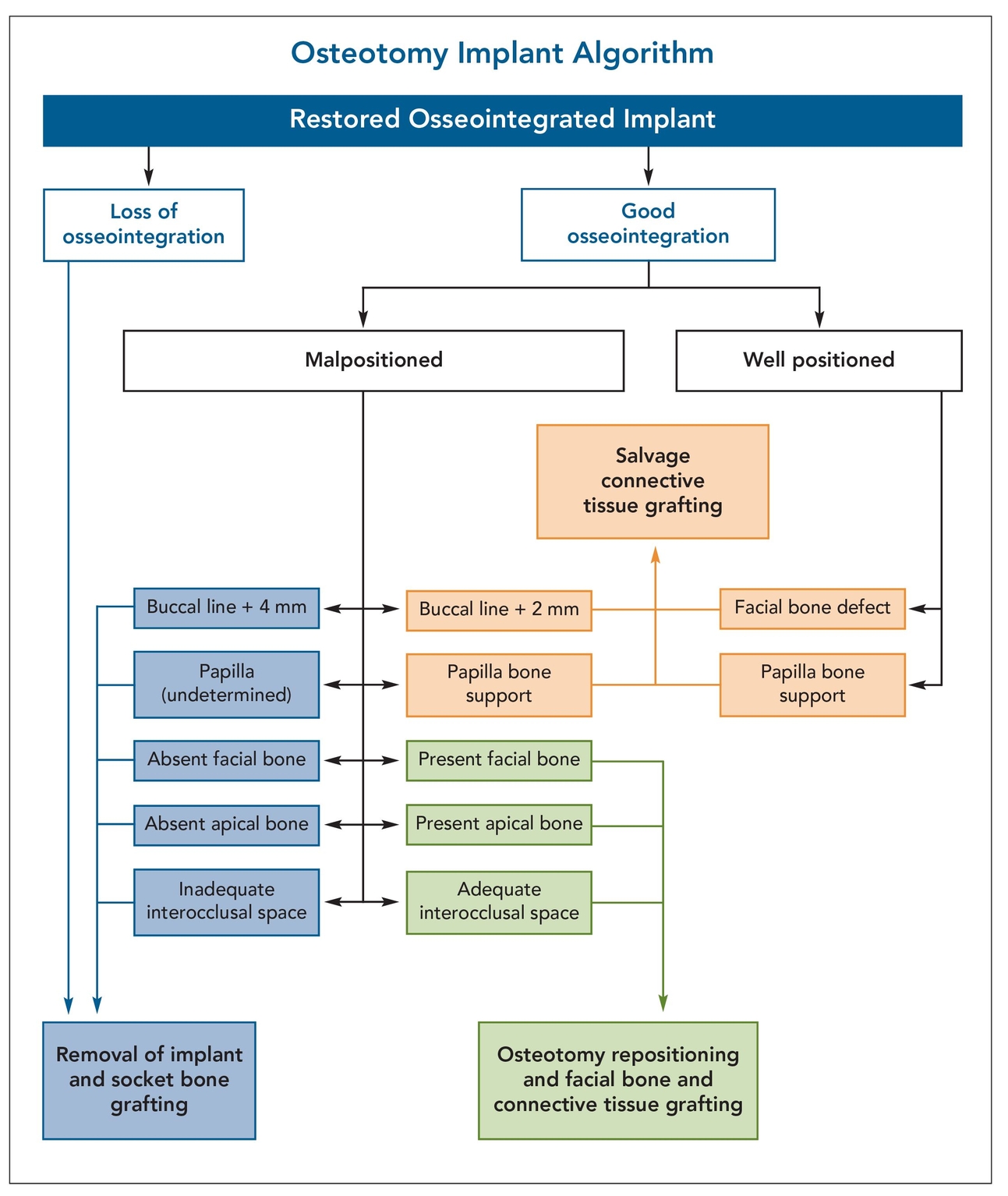
Fig 20-1 The treatment algorithm regarding whether to reposition or remove an unesthetically placed implant involves seven questions to determine if conditions favor the success of osteotomy repositioning.
 Case Report
Case Report
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


