Gingival Disease in Childhood
Clarice S. Law, Daniela R. Silva, Donald F. Duperon and Fermin A. Carranza
After first reviewing anatomic and physiologic changes in the periodontium and dentition, this chapter presents the gingival changes associated with childhood and adolescence. Periodontal diseases during these early periods of life are presented in the chapters that address the respective diseases (see Chapters 11, 23 to 25).
Periodontium of the Primary Dentition
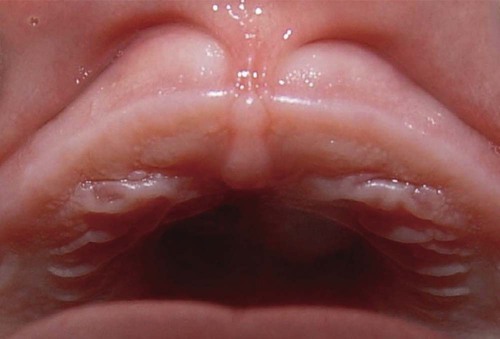
In the edentulous infant, the gingival tissues present with thick gingival mucosa and segmentations that correspond with the primary buds (Figure 18-1). A high labial frenum attachment is a normal finding in almost 85% of infants, which may diminish in size with normal development.58 During the primary dentition stage, the normal gingiva continues to be somewhat different from that found in adults. The tissues are pale pink, but they are pink to a lesser degree than the attached gingiva of adults, because the thinness of the keratinized layer causes the underlying vessels in children to be more visible.41 Stippling appears at about 3 years of age and has been reported in 56% of children between ages 3 and 10 years, with little differences between maxillary and mandibular arches or between boys and girls throughout childhood11 (Figure 18-2).
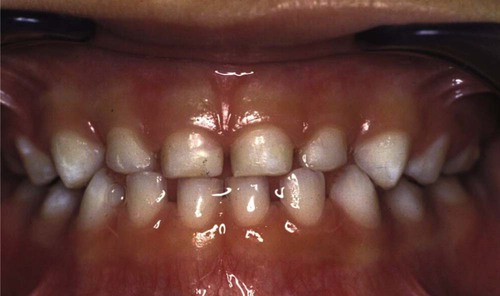
Gingival sulcular depth is shallower in the primary dentition than in the permanent dentition. Probing depths range from 1 mm to 2 mm, with an increase in depth from anterior to posterior.9,25,60
The attached gingiva varies in width anteroposteriorly, with a range of 3 mm to 6 mm. On the buccal surfaces, the width decreases from anterior to posterior, with some data indicating a narrowing over the canines (Figure 18-3). The lingual attached gingiva shows an inverse relationship, with an increase in width from anterior to posterior.25 The gingival width normally increases with age as children transition from the primary to the permanent dentition.5,9,15,60 Interestingly, the junctional epithelium is thicker in the primary dentition than in the permanent dentition,10 which is thought to reduce the permeability of the tissues to bacterial toxins.
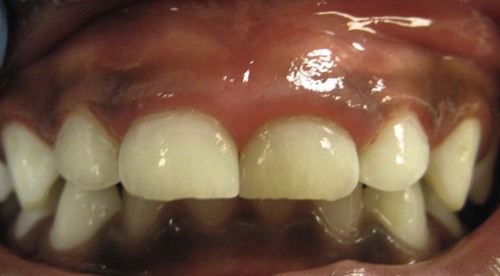
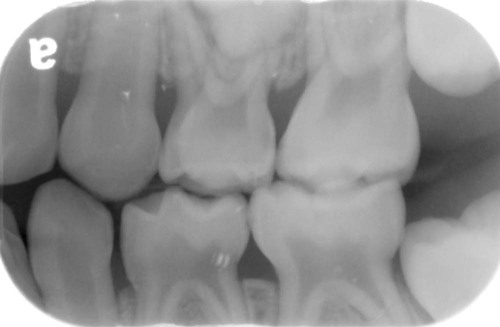
Radiographically, the lamina dura is prominent in the primary dentition, with a wider periodontal space than in the permanent dentition. The marrow spaces of the bone are larger, and the crests of the interdental bony septa are flat, with bony crests within 1 mm to 2 mm of the cementoenamel junction26 (Figure 18-4).
Periodontal Changes Associated With Normal Development
Tooth Eruption
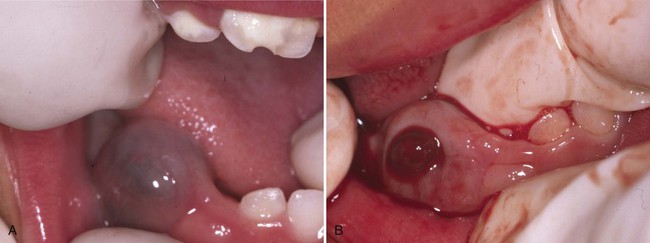
Before the eruption of a primary or permanent tooth, the gingiva reveals a bulge that is firm and pink or blanched as a result of the underlying tooth crown. An eruption cyst may occasionally be evident. This fluctuant mass may be filled with blood, and it generally presents as a bluish or deep red enlargement of the gingiva over the erupting tooth (Figure 18-5, A). The most common sites of these cysts are the primary first molars and the permanent first molars. Many resolve without treatment, but they may be marsupialized if they are painful or interfere with occlusion (Figure 18-5, B).14
Teething
The effect of primary tooth eruption on infant health has been debated for centuries, but there is little scientific evidence regarding the diagnosis and management of the teething child. The period associated with the eruption of the primary teeth in infants can be difficult and stressful for both the child and the parents. The timing of primary incisor eruption (i.e., 5 to 12 months old) coincides with the diminution of the passive humoral immunity conferred by the transfer of maternal antibodies via the placenta and the establishment of the child’s own immunity.17,54 Pain is a common feature of teething as reported by parents and some health care providers. However, it is not the tooth that causes the pain but rather the follicle, which is a rich source of eicosanoids, cytokines, and growth factors and which results in a localized inflammatory response.54,57
Most medical and dental professionals agree that teething does not cause life-threatening illness, but they disagree about which symptoms may be associated with tooth eruption. A summary of the studies and systematic reviews of symptoms related to teething most commonly include decreased appetite, biting, drooling, gum rubbing, irritability, sucking, and abnormal temperature.24,27,37,38,45,52,54,57,64,65 However, there is no evidence that any of the aforementioned symptoms can be diagnostic of teething in a child without excluding the possibility of other systemic diseases.
Primary Tooth Exfoliation
As with tooth eruption, the process of tooth exfoliation involves changes in the periodontium. The depth of the gingival sulcus increases as the junctional epithelium migrates down the resorbing root of an exfoliating tooth.8,10 Microscopically, minor traumatic changes may demonstrate compression, ischemia, and the hyalinization of the periodontal ligament.48 There may be changes in the permeability and integrity of the junctional epithelium, thereby making the exfoliating tooth more susceptible to inflammation.10
Other Developmental Issues
Relation of Periodontal Status to Malocclusion.
Data indicate an association between abnormal tooth position and gingivitis.20 Crowding in the mixed dentition can often make plaque and food removal more difficult, thereby leading to an increased incidence of gingivitis. Severe changes may include gingival enlargement, discoloration, occasional ulceration, and the formation of deep pockets or pseudopockets. Generally, gingival health can be restored with orthodontic correction, but a failure to align the teeth does not necessarily have an effect on periodontal disease later in life.20
Mucogingival Problems.
The prevalence of mucogingival problems and recession in children ranges from 1% to 19%, depending on the criteria used to assess the condition.32 Evidence suggests that some mucogingival problems may start during the primary dentition as a consequence of developmental aberrations in eruption and deficiencies in the thickness of the periodontium.41,42 A high frenum attachment may also be a factor in the development of mucogingival problems if there is excess tension at the marginal tissues.51,61 During the mixed dentition, recession is most often found on the facial aspect of mandibular permanent incisors secondary to rotations or labial positioning related to space problems. Although erupting permanent lower incisors often show minimal attached gingiva, gingival width often increases as the teeth erupt and stimulate bone development15 (Figure 18-6).
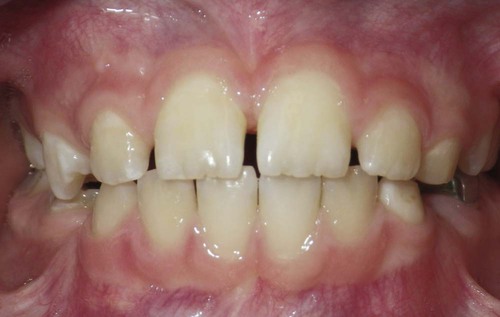
The maxillary canine region is also prone to localized gingival recession. Late-erupting canines in a crowded dentition may be displaced buccally, erupting into or near unattached gingiva or mucosa and increasing the risk of insufficient gingival tissue width and recession. Recession may also be associated with an anterior open bite as a result of the labial inclination of the teeth.35 Orthodontic treatment and realignment may be necessary to protect the integrity of the attached gingiva.
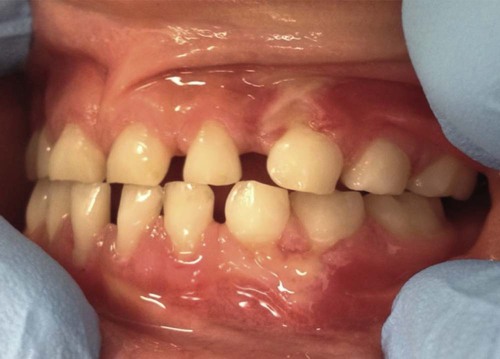
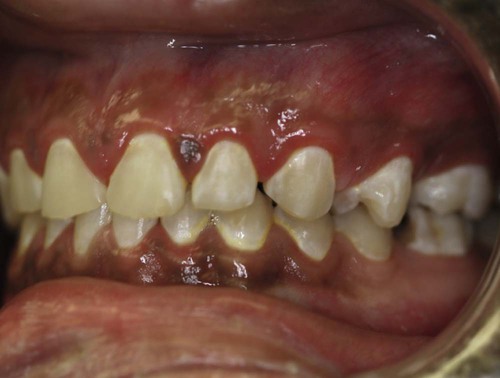
Mucogingival problems can also result from factitious habits, like self-inflicted trauma from a fingernail (Figure 18-7) or excessive toothbrushing by either the parent or the child. Because the width of the attached gingiva increases with age, any of these problems may resolve spontaneously, thereby suggesting a cautious approach to treatment with judicious monitoring instead of immediate surgical intervention.15,53
Gingival Diseases of Childhood
Plaque-Induced Gingival Disease
Gingivitis is extremely common among children and adolescents, and it affects up to 70% of children who are more than 7 years old.16,46 Inflammation is generally limited to the marginal gingiva (Figure 18-8), with undetectable loss of bone or connective tissue attachment in most cases. Although gingivitis does not always progress to periodontitis, the management of gingival disease in children and adolescents is important, because periodontitis is always preceded by gingivitis.46
In children as in adults, the primary cause of gingivitis is dental plaque, which is related to poor oral hygiene. The relationship between plaque and the gingival index, however, is weak and remains unclear.8,37,40 Although gingivitis is highly prevalent in children, its severity is generally less intense than what is found in adults.10 Similar oral hygiene conditions produce less severe forms of disease among children as compared with adults.46
As children age, their tendency to develop gingivitis increases.10 The prevalence of disease is lowest during the preschool years and increases throughout childhood, peaking during puberty. However, increases in the degree of gingival inflammation do not fully correlate with the amount of plaque, thereby suggesting the influence of other factors.
Clinical Features.
The most prevalent type of gingival disease in childhood is chronic marginal gingivitis (see Figure 18-8). The gingival tissues exhibit changes in color, size, consistency, and surface texture that are similar to those of chronic inflammation in the adult. Red, linear inflammation is accompanied by underlying chronic changes, including swelling, increased vascularization, and hyperplasia. Bleeding and increased pocket depth are not found as often in children as in adults, but they may be observed if severe gingival hypertrophy or hyperplasia occur.8,46
Chronic gingivitis in children is characterized by a loss of collagen in the area around the junctional epithelium and an infiltrate that consists mostly of lymphocytes, with small numbers of polymorphonuclear leukocytes, plasma cells, monocytes, and mast cells. Lesions generally have relatively few plasma cells, and they resemble the early nondestructive, nonprogressive lesions that are seen in adults. Furthermore, gingivitis in children differs from adult gingivitis in that the response is dominated by T lymphocytes, with few B lymphocytes and plasma cells in the infiltrate. This difference could explain why gingivitis in children rarely progresses to periodontitis.33,34,40,55 Gingival histology in children also demonstrates other unique features that may contribute to a decreased tendency to progress to severe gingivitis. The junctional epithelium of the primary dentition tends to be thicker than in the permanent dentition,10 which is thought to reduce the permeability of the gingival structures to bacterial toxins that initiate the inflammatory response.
Calculus.
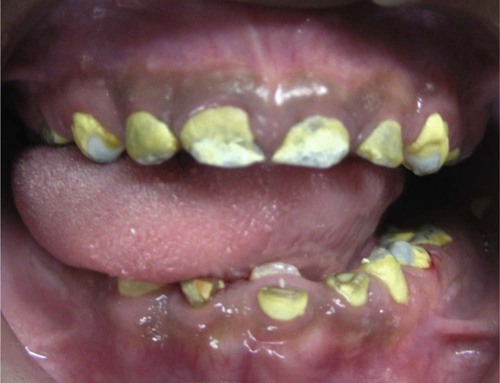
Calculus deposits are uncommon in infants and toddlers, but they may increase with age. About 9% of 4- to 6-year-old children exhibit calculus deposits. By the age of 7 to 9 years, 18% of children present with calculus deposits, and, by the age of 10 to 15 years, 33% to 43% have some calculus formation.66 Within the category of special needs patients, children with cystic fibrosis66 or chronic kidney disease39 have a higher incidence of calculus deposits, which may be caused by increased calcium and phosphate concentrations in their saliva. Children who are fed exclusively with gastric or nasogastric tubes show significant calculus buildup as a result of a lack of function and increased oral pH (Figure 18-9).23
Microbiology of Disease.
Because the intensity of gingival disease increases as a child develops into adulthood, it is important to understand the microbiology of disease, which is discussed more fully in Chapter 8. Interestingly, the composition of the oral microflora changes as the child matures.10 Yang and colleagues67 analyzed samples of dental plaque in children and reported that 71% of 18- to 48-month-old children were infected with at least one periodontal pathogen. Sixty-eight percent were infected with Porphyromonas gingivalis, and 20% exhibited Bacteroides forsythus (Tannerella forsythia).67 A moderate correlation also has been found between B. forsythus in children and periodontal disease in their mothers. B. forsythus also has been associated with gingival bleeding in children.
In a similar study, 60% of children between the ages of 2 and 18 years had detectable levels of P. gingivalis in their plaque, and 75% showed similar levels of Actinobacillus actinomycetemcomitans. The presence of P. gingivalis was most strongly associated with the progression of gingivitis and the onset of periodontitis in healthy children.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses