The Anxious or Fearful Dental Patient
Even after years of experience, many practitioners find that treating fearful/anxious dental patients is stressful. Part of the stress comes from the manner in which patients express their dental fear. The anxious patient may blurt out, “Don’t take it personally, but I hate going to the dentist.” Some fearful patients appear angry and hostile, whereas others are furtive and withdrawn both groups may be distrustful. Not only is such patient behavior unsettling to the dentist, but it may also significantly limit his or her ability to treat the patient’s dental problems. This chapter is designed to help the practitioner understand the problem of dental fear and to deal with it more effectively. This chapter familiarizes the reader with (1) the nature and scope of the problem; (2) the characteristics of fearful patients; (3) methods to evaluate, diagnose, and plan treatment for fearful patients; and (4) suggestions on how to deliver dental care to fearful individuals, including pharmacologic interventions when necessary.
NATURE AND SCOPE OF THE PROBLEM
In present times, the media often portray fear as a commonplace reaction to dental treatment. Many practitioners are offended by this portrayal, but the fact remains that fear of the dentist is a common phenomenon and is universally recognized. Little wonder that some (but not all) patients are so forthright with their own fearful dental stories.
Several studies confirm that dental anxiety and fear are common among people in the U.S. and other countries.1,2 About 50% of U.S. adults report some dental fear, with 8% to 11% being fearful enough that going to a dentist at all is problematic. In a Seattle area survey, 20% of respondents were classified as having high fear of dentistry.3 Smith and Heaton reviewed 19 articles involving more than 10,000 adults in the United States and concluded that the rate of dental anxiety and/or fear has remained stable during the past 50 years.4 Francis and Stanley drew from multiple sources and estimated the prevalence of dental phobia (an extreme form of fear) in Australian adults to be 10% to 14%.5 Surveys in Iceland, Taiwan, and Japan show at least some dental fear among 21%, 50%, and 82% of the adult respondents, respectively.6–8 Studies of children have shown a global variation in the prevalence estimates of dental anxiety between 3% and 43%.9 Methods used to collect dental fear data vary widely across studies, making direct comparisons of fear rates between countries problematic. Nonetheless, dental fear appears to be a problem internationally and affects the use of dental services in all countries from which data are available.
Many fears are not regarded as socially acceptable. The presence of dental fear, however, is widely accepted and carries little social stigma. This may make it easier for patients to rationalize and justify their own dental fear and hence maintain their own fearful and avoidant behavior. Given the international prevalence and universal acceptance of dental fear, it is impossible for the dentist anywhere to avoid fearful patients. Consequently, it is worth the clinician’s time and energy to learn to effectively treat fearful patients.10
Impact on Society
The large numbers of fearful dental patients and their associated behavior have an impact on the greater society.11 For the reported 14% of patients who delay having dental treatment because of their fear, the consequences can be unnecessary pain and suffering. Society then pays through lost workdays and diminished productivity of its members.12 Current estimates are that between 15% and 33% of the U.S. public experience dental-related disability days. In a study of 2600 employed people, 25% reported an episode of work loss in the past 12 months related to a dental problem.13
Impact on the Dental Team
About 14% of the public report canceling or failing to appear for dental appointments because of fear. The cost of missed or unfilled appointments becomes a financial issue for the dentist. This increased cost for dental practitioners in turn influences the cost of dental care for other patients in the practice. In addition, even when fearful patients do appear for their appointment, they often require more staff time and attention. Interactions with fearful patients may result in a reduction in job satisfaction. The patient’s fearful behavior may result in more stress and fatigue for the practitioner and less satisfaction among staff members as well. Dental fear may also result in reduced patient compliance, and therefore a diminished likelihood of treatment success for both patient and dentist.
Impact on the Patient
Dental fear has its greatest impact on the individual patient.14,15 The physical and psychological effects are significant, and the emotional toll on the millions of affected individuals is inestimable. In some families, several generations of individuals have suffered ill health, oral infection, acute and chronic dental pain, loss of oral function, and loss of self-esteem all because of dental anxiety.
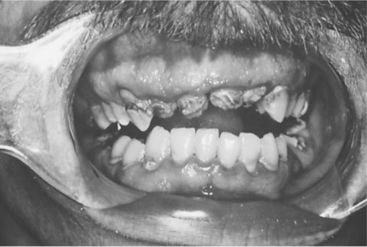
Some patients are embarrassed by their fear and may seek to hide it by avoiding going to the dentist altogether. On the other hand, if patients do mount the courage to schedule an appointment, they may fail to appear or avoid scheduling certain types of appointments (e.g., root canal therapy or surgery). This avoidance puts the patient at risk for failing to understand the symptoms he or she is experiencing, overestimating or underestimating their seriousness, and making it difficult to know when to seek help. Fearful patients may also have difficulty in making well-reasoned treatment decisions about their dental care needs. Some dentists may charge a fee for missed appointments, thus further increasing the financial burden of care. Delayed or nonexistent maintenance and preventive care frequently results in the need for more complex care, often at increased cost. If the patient delays too long, he or she must bear the burden of the greater cost for emergency care (Figure 13-1). The fearful patient is at risk for poor oral health, a lowered quality of life, and a substantial financial obligation.16,17
CHARACTERISTICS OF DENTAL ANXIETY, FEAR, AND PHOBIA
Anxiety is both a physical and emotional response to an anticipated experience that the individual perceives as threatening in some way. In some instances, the anxiety is generalized with a poorly defined focus. In its most extreme form, anxiety may significantly limit the individual’s ability to function in everyday life. Pathologic anxiety requires psychiatric intervention and is discussed in Chapter 14. When the dentist observes symptoms of extreme generalized anxiety, patients should be referred to an appropriate health care provider.
Fear is an emotional response to a genuine threat or danger. In its extreme form, fear of any stimulus can interfere with the ability to perform daily tasks. When the fear of a particular stimulus dominates the individual’s life, it is described as a phobia, also discussed in Chapter 14. Sometimes such fears become generalized to multiple stimuli. For example, dental fear is generalized to overall fear in 20% of the phobic population. Dental phobia is a special case of dental fear characterized as a consistent and persistent fear that interferes with one’s social or role functioning and often leads to avoidance of dental treatment of almost any type. Mental health workers may make a distinction between anxiety, fear, and phobias, but for most patients, the terms are used interchangeably.
Researchers in the field have been able to identify some circumstances and events that contribute to dental anxiety in susceptible patients. Children who received restorative or surgical dental treatment as 9-year-olds are more likely to report dental anxiety as 12-year-olds than are children who received regular treatment.18 Adult patients whose fears developed during childhood and early adolescence are less trusting and more hostile toward the dentist than other patients. Among adults, anxiety is often associated with the patient’s current assessment of the dentist’s likelihood to inflict pain.19 Evidence suggests that when the patient no longer fears pain, dental fear declines. Studies also show that relatively brief dental treatment may result in the incubation of dental fear that may manifest at a later time. Longer episodes of treatment, including spending time building trust and encouraging good oral self-care behaviors, may actually lessen the likelihood of dental fear. Therefore, brief emergency treatment appointments with such patients should be avoided.20 The implications of this research for the dentist are that special care should be taken in managing the distress and pain of adolescents who are irregular careseekers and who will require invasive dental procedures. Additional time spent with the patient, establishing rapport, providing the patient with a degree of personal control over the pace of treatment delivery, and fully informing the patient may lessen the likelihood of dental fear developing at a later date.
Fearful dental patients often report they are frightened by certain dental stimuli.21 The feared object or objects may include the needle, office sounds, the drill, or even the smell of the office.22 Patients also may report distrust of dental personnel and fear of catastrophe, such as a heart attack or choking during treatment. Such patients may have generalized anxiety about other life events as well. For many patients, the underlying fear is fear of pain.23,24 In fact, even among routine patients, fear of pain can be high.25
Emotional arousal increases the likelihood that patients will process the information they hear from the dentist and staff less carefully.26 As a result, anxious patients cannot be counted on to pay close attention to the details of a message about their care. Instead the anxious patient may pay closer attention to superficial and peripheral stimuli that reinforce negative stereotypes about dental treatment. The implications of this phenomenon are that the dental team must be attentive to the verbal and nonverbal messages with a fearful patient. An abrupt or “short” command to the patient may be interpreted as an admonition. The patient may also misinterpret nonverbal messages, such as perceiving the appearance of the physical surroundings (presence of “sharp” instruments) as threatening. The patient may focus on items in the environment that reinforce the perception of being in a frightening place, including anything that appears disorganized or not sterile.
Anxiety and Pain Perception
It is commonplace for dentists to downplay the degree of pain experienced by their patients. For some patients, the use of a local anesthetic may be sufficient to make them comfortable during treatment but for others it is not. Pain is a complex experience.27 The International Association for the Study of Pain defines pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage.”28 But the sensation of pain as it is experienced by a patient is more than a simple reflection of the amount of tissue damage that has occurred. Pain is always subjective and includes biological, psychological, and social dimensions. Sessle proposed that orofacial pain may be more complex than pain in other regions of the body because of the “special emotional, biologic, and psychologic meaning” it holds for the person.29 In addition, sensory nerves are heavily concentrated in the oral cavity, increasing the likelihood that all individuals are acutely aware of what is happening in their mouths.
Evidence suggests that anxiety lowers the pain threshold.30 However, there is also some evidence that anxiety and fear may have differential effects on pain reactivity. In a landmark experiment, Rhudy and Meager showed that experimentally induced anxiety led to increased pain reactivity whereas high levels of fear led to decreased pain.31 Whether the dental setting produces fear or anxiety is not clear, but within the dental care context, patients may have worried for days about a scheduled treatment, resulting in elevated levels of autonomic arousal and high levels of anxiety. This elevated arousal may produce heightened levels of plasma catecholamines, which in laboratory studies have been shown to lower the pain threshold and tolerance.32 It is not surprising then that many highly anxious patients show elevated levels of pain reactivity during dental treatment as compared with less anxious patients.33 Clinicians should therefore anticipate that anxious patients will experience more sensory and affective distress during dental treatment than less anxious patients and treat them accordingly (see the What’s the Evidence? box).34
Anxiety and Pain Memory
Anxiety appears to play a role in the level of pain that dental patients remember. Negative emotions, such as anxiety, become stronger predictors of the pain memory than the actual pain intensity. One study35 asked patients to recall their perception of pain during root canal treatment at 1 week after treatment and again 18 months later. All patients had an accurate recall of the pain level at the 1 week interval, but at 18 months, the patients with a higher level of anxiety remembered the pain as being greater than was actually recorded at the time of the time of the treatment. Experimental pain research has shown that the recall of pain intensity is reasonably accurate immediately after a painful experience and after a short delay of about 2 weeks. But after 6 months, the memory of pain delivered within a stressful context becomes exaggerated, with women recalling more pain than men.36 Moreover, exaggerated pain memories can alter brain pathways, further sensitizing the individual to painful stimulation.37 These findings illustrate the importance of anxiety management at the time of dental treatment to minimize the patient’s long-term recollection of the aversiveness of dental treatment and their anticipation of pain at future visits.
Gender Differences in Pain Response
There is considerable interest in gender differences in both clinical and experimental pain reporting. Several reviews and meta-analyses show that men are somewhat more pain tolerant than women.38 The differences, however, are often small,39 and the findings are not always consistent.40,41 Several explanations for the reported differences have been made, including the possibility that social learning encourages women to acknowledge painful stimuli, whereas men are expected to hide pain.42,43 Gender-specific hormones have also been implicated. For women, differences in the phase of the menstrual cycle are believed to influence pain sensitivity. A meta-analysis of experimental pain showed that during the follicular phase of their menstrual cycle women show the greatest tolerance and highest pain threshold. Research suggests that certain forms of analgesia may be differentially effective in women and men, but these differences are not universal.44–46 So it is not practical for the dentist to try to select an anxiolytic strategy or technique based on the gender of the patient. The best current wisdom is that there are large individual differences in the biological, psychological, and social mechanisms that underlie the human pain experience, and these individual differences are much more significant determinants of pain perception than is gender. As such, patients respond to dental pain and anxiety in unique ways, and a single approach to pain management in the dental office cannot be expected to work for all or even a majority of patients regardless of gender.
ETIOLOGY
The cause of dental fear is complex and multifactorial.47 Although dental fear may appear at any age, current data suggest that most fears begin in the preteen years. Direct conditioning and modeling play important roles in the development of fear in children who have a family history of dental fear. Such a history is predictive of early-onset dental anxiety.48 Adolescent-onset patients are more likely to exhibit high levels of generalized anxiety. These fears may lessen with maturity and after positive experiences with the dentist.49 For some patients, however, dental fear persists into adulthood. Evidence suggests that those who maintain their fear into adulthood tend to overpredict the level of pain they will experience during dental treatment. This overprediction of pain is often associated with a high level of anxiety during the treatment.50 Although the data show that this group of patients may or may not report more pain during treatment, their anxiety may make it difficult to correct their expectations.51 Thus the vicious cycle of anxiety-pain-fear persists, with little opportunity for the patient or the dentist to disrupt the cycle.
About 27% of fearful patients develop their fear as adults. Adult-onset dental fear seems to be associated with multiple severe fears and, in some cases, may be indicative of psychiatric problems. The perception of a lack of personal control during the dental appointment can contribute to dental fear.52,53 Some theorists have suggested that dental fear may be constant in spite of improved dental technology because many patients find that during dental treatment, they can exert very little personal control over what will happen to them. Patients may perceive their inability to speak and their supine position below the level of the dentist equivalent to helplessness. In a society in which some people seem to feel they are losing control of their lives, the loss of personal control during dental treatment can become symbolic of life in general. Several studies show that when this perceived lack of control is coupled with a heightened desire for control, patients are at risk for high levels of dental stress and pain.54,55 Whether this need for control is the result of negative experiences with the dentist at an early or at a more advanced age is not clear. It is clear, however, that patients who want control and believe that they will not have it expect high levels of pain and experience and remember more pain than other patients. The resulting dental treatment is likely to be stressful for both the dentist56 and patient.
In general, patients younger than 40 years of age are more fearful than those who are over 40, but no differences among socioeconomic groups or racial/ethnic groups have been demonstrated. Females are more fearful than males, but the differences between men and women are not so great that dentists should assume that male patients will not be fearful.57 Research shows that women demonstrate higher dental anxiety in association with root canal therapy than do men.58 Men may appear more stoic than women because women find it more socially acceptable to be overt about their distress. The clinical significance of this finding is that dentists may underestimate the amount of pain their male patients experience.59
There is increasing evidence that women with high levels of dental fear are more likely to have a history of sexual/physical abuse than other women. The current estimate of childhood sexual abuse in the general U.S. population is 5.8% to 34% for women and 2% to 11% for men, which is considered by many to be a conservative estimate.60,61 The sheer numbers of patients who have experienced sexual abuse suggest that dentists frequently treat sexually abused patients, and a greater understanding of the impact of abuse on dental attitudes and reactions may help both the patient and dentist to form an effective treatment partnership. For instance, a study of sexually abused European women who were categorized as to whether they had been exposed to sexual touching, intercourse, or oral penetration showed that women in the oral penetration group scored significantly higher on dental fear than women in the other two groups.62 In addition, women with a history of childhood sexual abuse and high levels of dental fear considered interpersonal factors related to the dentist as more important than did women with high levels of dental fear but without a history of childhood sexual abuse. These interpersonal factors included not believing that the dentist can be trusted and the absence of a sense of control.63
Not surprisingly, psychological distress, including the tendency to catastrophize upcoming events, was greater among women with an abuse history compared with other women.64 Unfortunately, knowing that there can be a relationship between sexual abuse and dental anxiety does not usually help the dentist in managing the anxiety. Raising the issue of physical abuse, even when done with the utmost tact and sensitivity, can be embarrassing for both parties (especially if the inference is wrong), can be psychologically traumatizing for the patient, and can irreparably harm the dentist-patient professional relationship. If there is clinical evidence of ongoing physical abuse, then the issue must be broached. Otherwise, unless the patient raises it, the dentist is usually best served not delving into the question. If, however, all other strategies for managing the anxiety have been tried and none have been met with success, and if the dentist has reason to believe that the patient’s dental anxiety has roots in underlying psychological problems that may have their origin with physical or sexual abuse, this avenue can be pursued. But if so, it must be with the guidance and counsel or via direct referral to a mental health specialist with experience and training in dealing with abuse.
RECOGNITION AND DIAGNOSIS OF DENTAL ANXIETY
Several directly observable behaviors can be used to identify the fearful patient. Often patients will volunteer information about dental fear without being asked. It is important for the dentist not to become defensive. A statement such as “Why do you feel that way?” may be interpreted as confrontational and may make it difficult to build a therapeutic relationship with the patient. Instead, comments such as “I understand that you are concerned about receiving dental care. Please tell me more about your concerns,” allows the patient to elaborate without having to justify his or her feelings.
It is usually possible to observe a patient before or during the appointment and to recognize fearfulness. Fearful patients often have enlarged pupils and sweaty or cold hands, and are extremely fidgety in the chair. They may either talk excessively or not want to talk at all. When a patient behaves in such a way, it is wise to say, “You seem uneasy, is there anything I can do to help you be more comfortable?” Ignoring the patient’s fear does not help the patient relax, and the patient may interpret the dentist’s behavior as callous. Moreover, it is easier to treat the patient if the dentist has more specific information about the patient’s concerns.
Patients may exhibit indirect indicators of their dental fear. Dental assistants and front desk personnel are often in an excellent position to observe these indirect indicators. Patients who chronically cancel appointments and reschedule may be struggling with their fear of dental treatment. Similarly, patients who fail to appear or who are chronically late may also be fearful patients. For patients exhibiting these behaviors, a question such as, “I see that you frequently have trouble getting here for your appointment. Are you nervous about receiving dental care?” allows the patient to either acknowledge the fear or to identify other barriers the dentist should know about. In either case, the information helps the dentist make better decisions about future dental care.
Standardized Indices
When any or all of the above clues are apparent, it may be advantageous to quickly administer one of several available surveys to establish the patient’s level of dental fear. Kleinknecht’s Dental Fear Survey consists of 20 items, has good psychometric properties, can be completed in less than 10 minutes in the waiting room, and can be quickly scored and interpreted.65–67 Other instruments that have shown good predictive utility are the Corah Anxiety Scale68–70 and the Iowa Dental Control Index54,71–73 (Boxes 13-1 to 13-3).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses