The Definitive Phase of Treatment
The definitive phase of care forms the core of virtually every treatment plan. Exceptions are made for those patients whose needs are limited to preventive services only, and those currently in a disease control plan for whom a definitive treatment cannot yet be delineated. For patients whose oral health needs do not warrant a disease control phase, all active restorative, periodontal, and orthodontic therapy is addressed in the definitive phase. For those patients whose oral health has necessitated special disease control measures, the definitive phase that follows may include elective surgical and endodontic procedures; orthodontic therapy; single tooth restorations not completed in the control phase; implants; any definitive tooth replacement; and any additional, more extensive therapy required for periodontal disease.
For the patient with complex oral needs, significant changes in oral health or attitude may have occurred since the first oral examination. Therefore, before engaging in definitive phase treatment, the practitioner should affirm that the following requisites have been met.
DEFINITIVE PHASE TREATMENT OPTIONS
Most definitive treatment falls into one of the categories listed in Box 8-1.
Clinical situations and treatment options for those situations are presented for each topic. The list of possible therapies that could be included in a discussion of the definitive phase is substantial and continues to grow with the introduction of new materials and techniques. The aim of this chapter is to suggest the range of options available for representative situations.
In general, the discussion that follows reflects the spectrum of today’s practice of general dentistry. For each topic, professional and patient modifiers that influence and shape the decision-making process are discussed. Tables in many sections summarize the discussion, restating the conditions to be treated, listing relevant treatment options, and providing brief suggestions regarding when each is recommended. For more in-depth coverage of specific areas, several excellent texts are available for each of the clinical disciplines of dentistry covering diagnosis, treatment planning, and therapy (see Suggested Readings).
PERIODONTAL THERAPY
A better understanding of the pathogenesis of periodontal diseases has led to new therapeutic approaches in addition to periodontal surgery. Following initial therapy, additional treatment may be indicated for residual diseased sites in which periodontal pockets and bleeding persist after scaling and root planing. Before reinstrumentation, reflecting a flap to improve access and increase visibility of deposits may be required. Surgical solutions to noninflammatory periodontal conditions may also be considered for esthetic problems, such as ridge deficiencies, root exposure, or excessive gingival display. Candidates for implant prostheses who possess too little existing bone for implant retention can receive bone augmentation in preparation for implant placement. In addition to surgical treatment, antibiotic therapy delivered locally or systemically may be a useful adjunct. Occlusal therapy (discussed later in this chapter) may be indicated to reduce occlusal trauma and protect the periodontium from damaging forces. The following series of clinical situations relate to the periodontal tissues and structures.
Periodontal Disease and Related Conditions
Periodontitis Not Responsive to Initial Therapy
As discussed in Chapter 7, initial therapy for periodontitis usually consists of meticulous scaling and root planing (often performed under local anesthesia); specific instruction in oral self care; and after a 6- to 8-week period, a detailed reevaluation or post—initial therapy evaluation. Although most patients respond favorably to this regimen, some do not. The causes of failure may include specific aggressive pathogenic microbes, poor oral self care, site-specific impediments to plaque and debris removal, or inadequate host response as a result of systemic factors, such as smoking or poorly controlled diabetes.
Localized Infrabony Defects
Angular or vertical bone loss associated with periodontal disease often results in an infrabony (within the confines of bone) defect and may be classified by the number of remaining bony walls, that is, a one-, two-, or three-walled defect. In general, teeth with untreated, progressive infrabony defects have a poor long-term prognosis.
Furcation Involvement
When progressive bone loss advances to the furcation area of a multirooted tooth, the condition is described as furcation involvement. The presence of bone loss in this area worsens the long-term prognosis for retaining the tooth.
Root Proximity
In some individuals, the roots of two adjacent teeth may have developed in close proximity to one another at the cervical third of the root. This condition can also arise when a significant loss of proximal coronal tooth structure has occurred, usually because of caries or fracture, with the result that the roots move closer together. In either case, root proximity may make the remaining interproximal bone vulnerable to rapid and dramatic destruction. Once the bone is lost, it becomes difficult or impossible to induce bone regeneration unless the teeth are repositioned.
Congenital or Medication-Induced Gingival Overgrowth
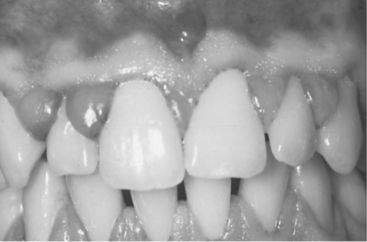
Gingival overgrowth can occur as a result of a genetic predisposition or in response to certain medications, including the anticonvulsant phenytoin (Dilantin); calcium-channel blockers for cardiac conditions (e.g., Procardia); or the immunosuppressant drug cyclosporine. Overgrowth can be unsightly and often inhibits effective oral hygiene (Figure 8-1). In extreme instances, if it extends past the coronal surfaces of the teeth, overgrowth can interfere with mastication.
Mucogingival Conditions
Mucogingival conditions are defined as altered relationships between the gingival margin and mucogingival junction that either do not allow for control of inflammation or are associated with progressive gingival recession. Common examples include gingival recession, minimal or absent keratinized gingiva, and probing depths that extend beyond the mucogingival junction. Mucogingival defects can result from local factors or from mechanical trauma to the tissue, such as toothbrush trauma. Patients with “thin”-profile periodontium are more susceptible to gingival recession than those with a “thick” periodontium. Special attention should be given to sites with thin and narrow bands of keratinized tissue, especially when subgingival margin placement or orthodontic tooth movement is planned.
High Frenal Attachment
If the maxillary labial frenum is coronally positioned, it may contribute to the retention of a diastema that the patient regards as unesthetic. High buccal or facial frenula may complicate denture construction. A coronally positioned lingual frenum (ankyloglossia) can interfere with speech and tongue movement.
Esthetic and Architectural Defects or Problems
Some patients present with periodontal conditions that they perceive to be unesthetic. Examples include the patient with a high lip line, short clinical crowns, or an excessive display of gingival tissue, particularly when smiling. Patients with clefts of the lips and/or ridges will typically seek correction. Similarly, patients with traumatic injuries or oral cancer may require reconstruction of the oral and periodontal tissues. A more recent and now common request is for tissue recontouring or increasing the roundness and size of the papilla (plumping) around implants and other fixed prostheses to create more natural and hygienic papillae and gingival contours.
Procedures for Treating Periodontal Disease
Periodontal Surgery
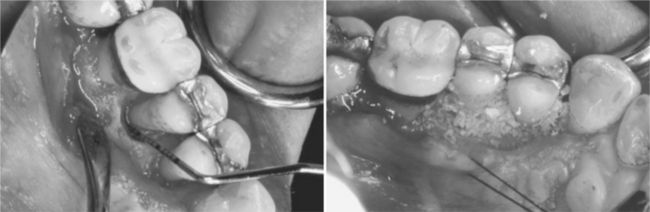
Periodontal surgery performed in the definitive treatment of periodontitis typically involves flap reflection to gain visual access to the root surfaces and bone (Figure 8-2). Following reflection, the dentist removes granulation tissue and performs scaling and root planing. Gingival and osseous tissue heights and contours may be altered. Osseous graft material or a guided tissue regenerative membrane may be placed. Elective periodontal surgery is also strategically used for the correction of gingival overgrowth, mucogingival defects, high frenal attachments, and other esthetic and architectural problems. Although these procedures are still commonly performed using conventional surgical (and in some cases electrosurgical) techniques, laser surgical techniques are gaining wider acceptance.
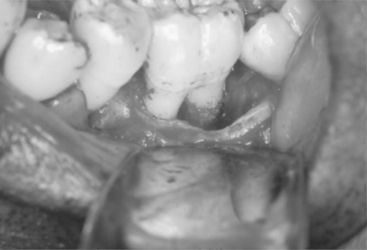
Figure 8-2 Periodontal flap surgery. Note the increased visibility and access for removal of deposits. (Courtesy Dr. J. Moriarty, Chapel Hill, NC.)
Periodontal surgery has a relatively high success rate, especially in patients who do not use tobacco and who have good oral self care or comply with maintenance therapy recommendations. Postoperative complications of surgical therapy can include bleeding, pain, and infection. Long-term negative outcomes may include a loss of periodontal attachment, gingival recession, and tooth sensitivity.
Placement of Antimicrobial-Impregnated Fibers, Cords, or Gels
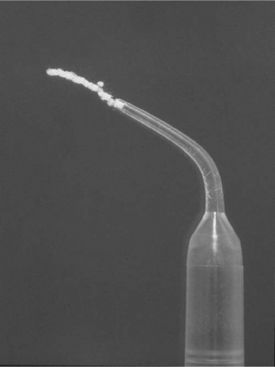
Antimicrobial agents, often impregnated into fibers, cords, or gels, can be placed directly into periodontal pockets to deliver a high concentration of drug to the diseased area (Figure 8-3). The treatment can be effective with proper patient selection and good retention of the agent in the pocket. Patient discomfort is relatively mild. As with other periodontal treatment, inflammation can return to the treated site and relapse can occur. When multiple sites are involved, or in forms of aggressive periodontitis, systemic antibiotics may be considered.
Bone Regenerative and Replacement Therapy
Periodontal regenerative therapy draws on multiple techniques and materials, including placement of freeze-dried demineralized bone or other substances that induce bone formation or provide a substrate for osseous growth (Figure 8-4). Guided tissue regeneration, another form of regenerative therapy, involves placement of a membrane over the osseous defect to encourage new bone and periodontal ligament formation. This procedure may be performed alone or in conjunction with placement of an osseous graft. A growth-promoting agent in a gel delivery system (Emdogain) may also be placed in the bone defect and on the root surface to enhance regeneration. Case selection for any of these procedures is important, and the success rate is best for three-walled infrabony periodontal defects. Complications of placing these materials are similar to those associated with periodontal flap surgery. In addition, material placement increases the cost and the time required for treatment.
Keys to Decision Making
Professional Modifiers
Before considering re-treatment, new surgical therapy, or other adjunctive periodontal procedures, the dentist should evaluate the importance of any relevant systemic factors, tooth-related problems, and localized periodontal conditions. Systemic factors could include patients who are anemic, malnourished, or otherwise immunocompromised. If the patient is a smoker, has smoking cessation been recommended? If drug-induced problems such as phenytoin gingival overgrowth exist, can the drug regimen be altered? If periodontal surgery is considered, will the patient’s general health be a limiting factor?
Tooth-related issues include an assessment of whether the teeth in question have a good restorative prognosis independent of periodontal problems. Is there a tooth-related cause for the current periodontal problem, such as an open proximal contact, calculus, or a poorly contoured restoration? How important is the retention of the tooth (or teeth) to the patient’s overall oral condition?
Localized periodontal factors that should be assessed include plaque accumulation, bleeding, soft tissue and bone topography, probing depths, clinical attachment levels, furcation invasions, mucogingival relationships, mobility, and occlusal factors (Figure 8-5). In addition to conventional methods of evaluation, the patient’s periodontal status may warrant use of additional diagnostic procedures, such as microbial testing or medical laboratory tests. Other factors that the dentist assesses are the level of overall patient cooperation with and response to previous therapy and oral self-care instructions and the prognosis for any treatment options under consideration, including the option of no treatment.
Patient Modifiers
Some behavioral issues can be pivotal to the decision as to whether and how treatment for the periodontal tissue—related conditions described above is carried out. Does the patient engage in a healthy lifestyle, characterized by good nutrition, regular exercise, and good control of any systemic disease? Does the patient use any tobacco products? Does the patient understand the importance of the proposed treatment and value it? Is the patient motivated to preserve the teeth in question? If not, can he or she be motivated to accept and appreciate the treatment?
Patient-specific issues may affect the planning, timing, and sequencing of definitive periodontal therapy. Is the patient in discomfort or experiencing any symptoms related to the condition? Are there personal reasons motivating the patient to have the treatment (esthetics, halitosis)? If so, the dental team will need to be sure that these concerns are addressed in the course of therapy. Does the patient have a preference for a particular form of therapy? Is he or she willing to undergo the removal of hopeless teeth? The inconvenience, stress, and post-operative discomfort of a surgical procedure? Does the patient accept the proposed therapeutic plan?
Other important questions to ask before proceeding with definitive care include: Does the patient have the necessary financial resources to pay for the treatment? Is the patient willing to follow through with long-term maintenance therapy?
Summary
Not all patients or disease sites respond acceptably or equally to periodontal therapy. When trying to manage periodontitis that has not responded to initial therapy, any of the professional or patient modifiers discussed above may significantly affect the outcome. Successful periodontal therapy requires a sound plan, good execution, and a motivated patient. Long-term success depends on an appropriate maintenance program. Patient noncompliance with maintenance therapy can lead to disease recurrence or progression. A few patients may experience recurrent or progressive disease despite adequate maintenance therapy. For these patients, additional treatment may be indicated.
Table 8-1 summarizes guidelines for the selection of common treatment options for each of the seven periodontal tissue—related conditions discussed.
Table 8-1
Periodontal Treatment Alternatives
| Condition | Treatment Options | Keys to Decision Making |
| Periodontitis not responsive to initial therapy | Reinstrumentation | An option in the presence of calculus or root roughness where access limitation does not preclude the procedure |
| Surgical flap procedure | In locations where access to calculus or root roughness is compromised and instrumentation would be more effective after elevating a full-thickness flap; situations in which bone osteoplasty, removal, or augmentation is indicated; in locations where apical repositioning of the gingival margins will be beneficial | |
| Local and systemic antimicrobial agents | An option when local factors have been removed; local delivery is an option for isolated inflamed sites; systemic antibiotics may be considered in aggressive forms of periodontitis; microbial testing can be of value in selecting an appropriate regimen | |
| Localized infrabony defects | No treatment | Possible approach if the patient is resigned to losing the tooth, but wishes to retain it in the short run for space maintenance or esthetics |
| Extraction | Possible option if patient has an immunocompromising condition or debilitated health (ASA III or IV) and the likelihood for improvement is guarded or if patient has poor compliance with recommended oral self care, or lacks the time, energy, or financial resources necessary to retain the tooth | |
| Closed reinstrumentation | When the patient refuses a surgical approach and the defect can be stabilized in its present condition using nonsurgical therapy | |
| Root resection | May be an option if the defect is isolated to one root and the prognosis for the remaining root or roots is favorable (Note: requires root canal therapy) | |
| Guided tissue regeneration or augmentation of the site using osseous grafting materials | Patient and disease site must be a good candidate for regenerative therapy; material and technique selection is determined on a case-by-case basis | |
| Furcal involvement | No treatment except for maintenance procedures | May be appropriate if furca is stable, cleansable, and without inflammation or disease progress; in the presence of progressive disease the “no treatment” option would be permissible only if patient is resigned to losing the tooth but wishes to preserve it temporarily for space maintenance or esthetics |
| Extraction | An option if patient has no desire to save the tooth or if dentist deems the tooth unsalvageable and retention would lead to additional bone loss around the tooth and/or adjacent teeth | |
| Bone regeneration | Patient must be motivated to save the tooth and have the financial resources and desire for optimal treatment; case and site selection is important | |
| Root amputation or hemisection | If the patient has motivation, financial resources, and desire as noted above and augmentation has been tried unsuccessfully, or if augmentation has been ruled out and at least one residual root is thought to have a good prognosis | |
| Root proximity | No treatment | Current periodontal condition is healthy and stable and patient accepts responsibility for possible disease progress and tooth loss |
| Periodontal maintenance treatment with bone augmentation as feasible and appropriate | Preferred option if patient wishes to retain the teeth as long as possible, but is unwilling to undergo orthodontic therapy | |
| Orthodontic correction followed by definitive periodontal therapy | Ideal solution for a motivated, compliant, and consenting patient who wants optimal treatment to save the teeth | |
| Congenital or drug-induced (e.g., phenytoin) gingival overgrowth | No treatment | May be an option if the overgrowth is limited in scope, asymptomatic, not progressive, does not exhibit inflammation, and is maintainable in a healthy state |
| Gingivectomy or gingival flap surgery | Usually necessary if hyperplasia is generalized, symptomatic, progressive, and inflamed, and if tissue cannot be maintained in a healthy state | |
| Mucogingival defects (clefts, recession, absence of attached gingiva) | No treatment except for maintenance procedures | The condition is stable, no active inflammation or infection, and no definitive restoration or orthodontic therapy is planned for that location |
| Pedicle graft | When the above conditions are not met and the defect is isolated to one tooth; adjacent papillae must contain sufficient bulk to reposition into the affected area without detaching the base of the flap | |
| Autogenous graft from separate donor site | An option when defect is progressive or has persistent inflammation, or if a definitive restoration is planned for the area, or when the defect involves multiple adjacent teeth or a pedicle graft would otherwise not be adequate; a subepithelial connective tissue graft is the most popular procedure for esthetic procedures involving root coverage | |
| High frenal attachment | No treatment | In the absence of patient esthetic, phonetic, or functional concerns; no inhibition of desired orthodontic movement or limitation to construction of a prosthesis |
| Frenectomy | When the patient is symptomatic or when the frenectomy would improve the prognosis for orthodontic or prosthodontic treatment |
ORTHODONTIC TREATMENT
Orthodontic treatment usually is thought of as an elective therapy for adolescent patients, most frequently initiated to improve appearance. In addition to esthetic considerations, however, there are many other reasons why limited or comprehensive orthodontic treatment may be recommended to adult patients. For example, it may be advantageous to orthodontically move an impacted tooth into the dental arch, or the vertical dimension of occlusion may need to be increased and an orthodontic approach may be the least invasive and most efficient way to accomplish this goal. Restorative or periodontal therapies may be enhanced by uprighting tipped teeth before fabrication of a fixed partial denture or placement of implants in an edentulous space. No matter what the reason, the patient deserves to be informed when orthodontics is a reasonable treatment option and what the potential benefits of orthodontic treatment may be. Malocclusion and tooth position problems may be treated with orthodontics alone or with orthodontics in combination with restorative and/or surgical procedures.
Malocclusions and Related Conditions
The common thread with this series of clinical problems is the malalignment of the teeth and/or jaws.
Angle’s Class I Malocclusion
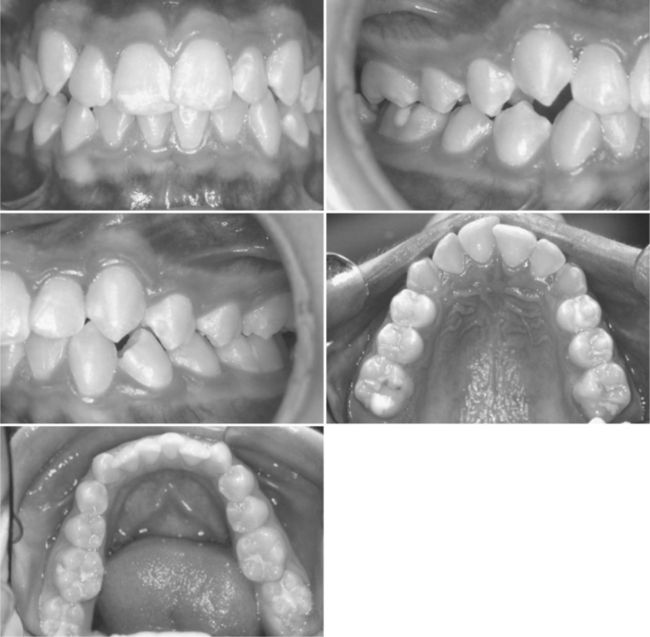
This diagnosis typically involves tooth-arch discrepancies in which the cumulative anteroposterior dimension of the teeth is greater than the length of the available alveolar bone (Figure 8-6). Often the opposing first molars and canines are in normal relationship relative to each other. This type of malocclusion most often is characterized by crowded or malposed teeth, but also may be associated with rotated or tipped teeth, impactions, or isolated cross-bites.
Impacted Maxillary Canines
The occurrence of this condition presents the dentist with a unique treatment planning challenge. Because of their arrival in the eruption sequence after the incisors and premolars, the maxillary canines are more likely to be impacted or blocked out of the normal dental arch configuration. Maintaining these teeth in a proper alignment has unique and important advantages given their long root length and their pivotal functional and esthetic role.
Anterior Open Bite
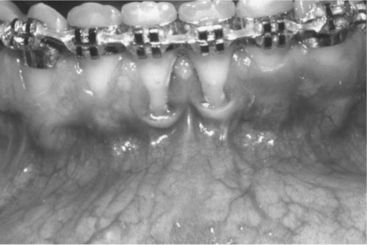
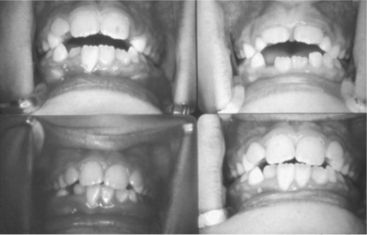
This occurs when the posterior teeth are in maximum intercuspation, and there is vertical space between one or more pairs of maxillary and mandibular anterior teeth. Depending on the size of the open bite, this occurrence may represent a significant esthetic, phonetic, or functional problem for the patient (Figure 8-7).
Procedures for Treating Malocclusion
Comprehensive Orthodontics
Comprehensive or-tho-dontics involves the movement of several teeth, usually in both arches, to improve tooth alignment, function, and esthetics. Usually the practitioner affixes bands and brackets to the teeth, coupled with arch wires and elastic bands. A new form of treatment that has gained considerable popularity with patients and within the profession involves using Visaline functional appliances. The appliances are more esthetic and are tolerated well by patients. Extraction of some teeth may be necessary. The treatment time varies and can range from 1 to more than 3 years, depending on the individual characteristics of the case.
Orthodontic treatment has fairly predictable success rates and outcomes. Potential negative sequelae include root blunting and resorption, gingival recession, increased caries activity, and discomfort to periodontium and other soft tissue during treatment.
Limited Orthodontic Tooth Movement
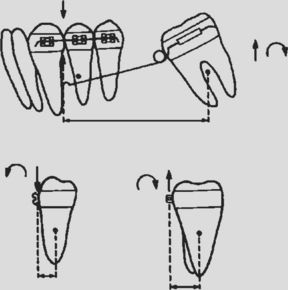
Limited orthodontic tooth movement involves tipping or rotation or bodily movement of a limited number of teeth (usually no more than six), usually in just one arch. Several techniques are available to the dentist and include both fixed and removable appliances. Treatment is usually accomplished in less than a year, with less potential for side effects compared with long-term treatment. A specific example of limited tooth movement is forced eruption of an anterior tooth in which caries or fracture of the crown (and root) has compromised the biologic width. Another common type of minor tooth movement involves uprighting tipped posterior teeth in preparation for use as prosthodontic abutments or to facilitate implant placement (see In Clinical Practice box).
Orthognathic Surgery
Orthognathic surgery may be indicated when the patient has significant skeletal abnormalities in addition to a dental malocclusion. These procedures, usually performed by an oral and maxillofacial surgeon in a hospital setting, involve surgical realignment of the jaws or repositioning of dentoalveolar segments. Surgical treatment may be preceded and/or followed by comprehensive orthodontic treatment.
Orthognathic surgery may be the only satisfactory way to correct a severe skeletal defect, especially for the adult patient. Significant swelling and pain can be associated with the procedure, and it usually requires 1 to 2 days of hospitalization. The patient’s jaws may be immobilized after surgery for 6 to 12 weeks to stabilize the new occlusal relationship. Nerve damage during surgery may result in areas of numbness involving the teeth, lips, tongue, and other surrounding tissues.
Keys to Decision Making
Professional Modifiers
Before a decision can be made to engage in orthodontic treatment, several important modifiers should be assessed carefully. Individually or collectively, these items may have a bearing on deciding whether to treat, how to treat, and when treatment should take place. For each situation previously discussed, a definitive orthodontic case analysis is in order, such as the “Facial Form Analysis,” developed by Proffit and Fields (see Suggested Readings). At a minimum, panoramic radiographs and a complete mouth series of radiographs and study casts is required. In those cases in which a skeletal component to the malocclusion exists, cephalometric radiographs and a cephalometric analysis also are necessary.
Unless the general dentist has had considerable additional training in orthodontic assessment and treatment, it is usually prudent to enlist the services of an orthodontist during this treatment planning process. Key questions include determining the scope of care (limited vs. comprehensive), whether extractions are necessary or desirable, and whether the option of orthognathic surgery should be pursued. For some adult patients, it may be best to displace teeth relative to the supporting bone to compensate for an underlying jaw discrepancy. This repositioning of teeth primarily for improving facial esthetics is referred to as camouflaging and is often a viable alternative to orthognathic surgery.
Before considering orthodontic treatment, the dentist must be certain that the patient does not have active caries or periodontal disease and is not at significant risk for future disease. The teeth and restorations must be in a stable state, capable of supporting the retention of orthodontic appliances for the duration of treatment. It is also the dentist’s responsibility to identify any apical pathology or root abnormality, such as resorption, before orthodontic treatment is initiated. In addition, the dentist should assess the scope and magnitude of the problem for which orthodontic treatment is considered. If the problem goes untreated, will any significant negative sequelae arise? Is the problem causing, or is it likely to cause, a functional or esthetic problem? In some cases, identifying the specific cause of the problem is critical to the outcome of treatment. For example, if the dentist or orthodontist attempts correction of an anterior open bite without recognizing and addressing the underlying cause, such as a tongue thrust habit, then it is likely that relapse will occur and the treatment will ultimately fail.
Other issues to be considered include the generalist’s training, expertise, and level of comfort with orthodontic treatment. Every general dentist should be able to recognize the clinical problems described in this section and to converse with the patient about them. Some general dentists prefer to refer all orthodontic treatment to specialists. Others can manage limited tooth movement cases. A few generalists who have had extensive training can handle more complex malocclusions. In any case, it is wise for the general dentist to carefully define the limits of his or her knowledge and ability, and treat only those cases that offer a high likelihood of success. It is also advisable for the general dentist to cultivate a close working relationship with an orthodontist and an oral and maxillofacial surgeon so that cases can be discussed and referrals made when appropriate.
Patient Modifiers
A fundamental determinant in orthodontic treatment planning is the patient’s own perceived need for that treatment. For most patients, the willingness to accept orthodontic treatment is motivated by a desire to improve appearance, and a direct correlation can be made between the strength of that desire and the motivation to receive orthodontic treatment. Changes in the patient’s personal life or career can be extremely powerful and effective motivators for initiating orthodontic treatment. Some influences, such as the desire to please a spouse or family member, can be short-lived and if the patient lacks a strong internal motivation to continue, the outcome of treatment may be in jeopardy. The wise practitioner carefully investigates these issues before engaging the patient in orthodontic treatment.
It is important to gain a sense of the patient’s expec-tations about the treatment. Are those expectations realistic? Is the patient interested in limited treatment or comprehensive care? If limited care is preferred, is it technically possible to achieve the patient’s goals? If comprehensive orthodontic care is favored, does he or she have any misperceptions that the treatment can be accomplished in a matter of weeks or by putting braces on a few selected teeth? Does the individual have an aversion to either fixed or removable orthodontic appliances or retainers? If so, will this compromise the treatment?
It is also important to ensure that the patient has a full appreciation of the costs of treatment, in terms of both financial resources and the time and inconvenience that may be required. Is the individual aware of the number of visits that may be required and the number of months over which the treatment will extend? Does he or she recognize that there may be some discomfort to the teeth and soft tissue? Most importantly, can the patient maintain the health of the oral cavity with effective daily oral self care despite the impediments to plaque removal that orthodontic appliances may raise? If orthognathic surgery is recommended or required, is the patient fully aware of the costs, hazards, inconvenience, and discomfort that the procedure may entail?
Typical treatment options for four common problems that can be treated with orthodontics are summarized in Table 8-2 with guidelines for selecting the most appropriate option.
Table 8-2
Treatment Alternatives for Malocclusions and Related Problems
| Condition | Treatment Options | Keys to Decision Making |
| Angle’s Class I malocclusion | No treatment | Patient not interested in correction; limited financial resources or presence of active oral disease precludes treatment |
| Limited tooth movement | Patient wants limited care only; goals of limited tooth movement are feasible and meet patient expectations; no systemic or oral contraindications to treatment are present; no financial, motivational, or other psychosocial barriers to care | |
| Comprehensive orthodontic treatment by generalist | Patient consents to comprehensive care; no contraindications to treatment or barriers to care; generalist has the training, expertise, and desire to provide the care | |
| Comprehensive orthodontic treatment by orthodontist | Same as above except generalist does not have the training, expertise, or desire to provide the care | |
| Impacted or partially erupted maxillary canines | No treatment | Patient has no motivation to correct the problem; systemic disease suggests contraindications to surgery or orthodontics; presence of active caries or periodontal disease precludes orthodontics |
| Surgical removal of canines | Impacted canines and poor prognosis for successful forced eruption; no contraindications to surgery; orthodontic treatment is precluded by lack of financial resources or motivation, or presence of active oral disease; retention of canines may jeopardize the long-term well-being of the adjacent teeth | |
| Extraction of first premolars and comprehensive orthodontics | Patient seeks correction; root form and tooth position of canines conducive to forced eruption; orthodontics without extraction is not a feasible option (insufficient space available for good alignment if all teeth are retained) | |
| Comprehensive orthodontics | Patient seeks correction; canine root form and tooth position conducive to forced eruption; orthodontics without extraction is a feasible option (sufficient arch space exists to allow good alignment when all teeth are retained) | |
| Anterior open bite | No treatment | Patient has no interest in treatment; no phonetic or functional deficiency |
| Correction of tongue thrust habit | Primary tongue thrust must be corrected before initiation of any surgical or orthodontic treatment (management of secondary or acquired tongue thrust can be deferred until after orthodontic or surgical therapy) | |
| Orthodontic correction | Patient seeks correction; skeletal relationship is adequate to support an all-orthodontic solution | |
| Surgical and orthodontic correction | Patient seeks correction; the skeletal relationship is insufficient to support an all-orthodontic correction | |
| Skeletal malocclusion | No treatment | Patient not interested in correction; no significant phonetic or functional problem exists; health, financial resources, or presence of active oral disease preclude treatment |
| Orthodontic treatment alone (camouflage) | Patient seeks esthetic improvement but lack of motivation, presence of systemic disease, or other reasons preclude surgical-orthodontic treatment; camouflage option is feasible, practical, and likely to yield desired result | |
| Comprehensive orthodontics in conjunction with orthognathic surgery | Patient seeks comprehensive, ideal solution; good surgical candidate (ASA I or II); oral disease under control; patient has satisfactory oral hygiene; patient is cooperative, motivated, and has adequate time and financial resources; professional support from competent specialists is available |
NONORTHODONTIC OCCLUSAL THERAPIES
Occlusal therapy incorporates those treatment modalities available to the dentist to manage occlusal abnormalities that can cause damage to the teeth and periodontium. Tooth-related reasons for treatment include severe tooth wear, abnormal occlusal planes, malposed teeth, occlusion-related periodontal attachment loss, and parafunctional habits, such as bruxism, clenching, or nailbiting. Patients with temporomandibular disorders (TMDs) affecting either the muscles of mastication or the TMJ itself may be candidates for occlusal therapy both to diagnose and to treat the problem. Individuals who engage in contact sports or other physical activities that place the teeth at risk for blunt trauma are good candidates for protective occlusal (athletic) guards. Often instituted before pros-thodontic rehabilitation, occlusal therapy may include adjunctive orthodontic treatment. Occlusal therapy may also precipitate the need for additional dental procedures, including root canal therapy, crown lengthening procedures, and/or crown placement.
Procedures for Treating Occlusal Problems
Occlusal Adjustment
Occlusal adjustment, also referred to as occlusal equilibration, involves selective grinding of tooth surfaces with the goal of improving tooth contact patterns. The treatment can be an adjunctive therapy used to alleviate symptoms of temporomandibular dysfunction or, more commonly, to complement comprehensive prosthodontic reconstruction. Treatment goals for selective grinding include developing an acceptable centric relation contact position for the patient, providing for acceptable lateral and protrusive guidance, and establishing an acceptable plane of occlusion with adequate interarch space for any prosthesis replacing missing teeth.
Occlusal adjustment is an irreversible procedure and the dentist must carefully study the patient’s existing occlusion before removing any tooth structure. This includes analyzing mounted diagnostic casts and carefully observing the patient’s occlusion intraorally. Articulating paper and occlusal indicating wax are valuable tools for identifying occlusal patterns. Before performing the procedure, the dentist should inform the patient that grinding the teeth may cause tooth sensitivity in some individuals. The patient also needs to be aware that when gross occlusal reduction is used to correct an occlusal plane discrepancy such as that caused by a hype-r-erupted or extruded tooth root canal treatment, surgical crown lengthening, and/or a crown restoration also may be required.
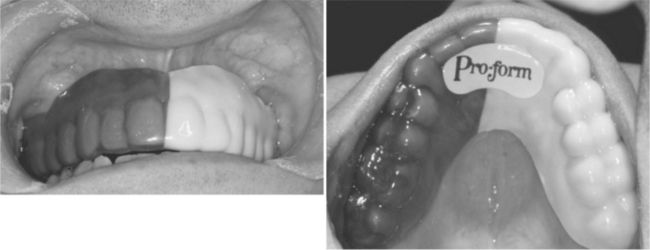
Occlusal Appliance Therapy
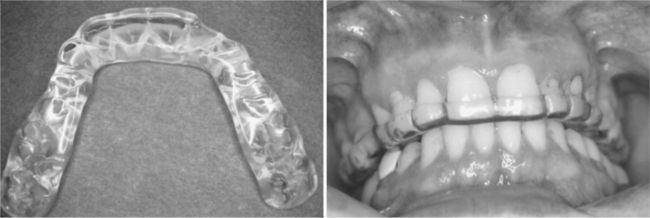
An occlusal appliance, also referred to as a bite guard or bite splint, is a custom-fabricated hard or soft acrylic device that fits over the occlusal and incisal surfaces of either the maxillary or mandibular teeth (Figure 8-9). Occlusal appliances have several uses. For patients with symptoms of TMD, the appliance promotes a more orthopedically stable TMJ position and reorganizes the neuromuscular reflex activity. Along with providing some measure of relief from pain symptoms for the patient, use of the appliance may also confirm the diagnosis of TMD. Occlusal appliances are commonly used to prevent tooth wear caused by bruxism. The dentist also may use the appliance to assess the patient’s tolerance for an increased vertical dimension of occlusion before prosthodontic rehabilitation.
A major advantage to occlusal appliance therapy is that the treatment is reversible and noninvasive. The therapy requires patient cooperation, however, since the splint is only effective when the patient is wearing it. To gain maximum benefit from the therapy, the dentist must carefully adjust the appliance at the time it is delivered and periodically thereafter.
Athletic Guards
A soft, plastic removable appliance, the athletic guard is designed to protect teeth from blunt injury trauma (Figure 8-10). Most frequently prescribed for younger patients who engage in contact sports, such as football and wrestling, the athletic guard can benefit adults too, particularly those who play basketball and racquet sports. If used consistently, the athletic guard effectively protects the teeth from damage. Unfortunately, for many patients compliance can be a problem.
Patients can make their own guards, using kits available in sporting goods stores, or the dentist can fabricate a custom-fitted appliance by vacuum-forming the guard material onto a plaster cast of the patient’s maxillary arch. To maintain an adequate fit for children, the guard may need to be remade periodically as deciduous teeth are lost and new teeth erupt.
RESTORING INDIVIDUAL TEETH
For many years, procedures to restore individual teeth have been the central focus of most general dental practices in the U.S., occupying most of the patient’s and the practitioner’s time. Single tooth restorations replace tooth structure lost because of caries, tooth fracture, abrasion, attrition, abfraction, or erosion (see the What’s the Evidence? box on p. 182). These restorative techniques may also be used to improve the appearance of teeth, establish more normal contours, or close proximal contacts. Some restorative materials are designed to seal areas that have the potential to decay or to desensitize tooth surfaces. Commonly, new restorations are necessary to replace older restorations that have failed because of secondary caries, fracture, material loss, marginal leakage, or stain. Amalgam or composite resin restorations are usually placed into teeth and therefore are considered intracoronal restorations. Extracoronal restorations, such as the gold onlay or porcelain veneer crown, surround the tooth, replacing the entire occlusal or incisal surface.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses