Chapter 10
The Future
Thus far in this book we have tried to concisely review our current understanding of the presentation, diagnosis, management and clinical outcomes for oral potentially malignant disorders. In doing so, it will no longer surprise the reader that it is very clear that there remain many unanswered questions and fundamental problems with our present knowledge base. A list of these limitations and the salient difficulties in our approach to oral precancer diagnosis and management is summarised in Box 10.1, together with a number of potential solutions that may help to address these problems.
Box 10.1 Current problems and potential solutions in oral potentially malignant disorder management.
Current problems
- Non-specific precancer diagnosis with no reliable prediction of clinical behaviour
- No ability to determine future disease progression
- Unpredictable risk of oral malignancy
- Difficulty in determining the efficacy of treatment interventions
Solutions
- Individual patient profiling at the biomolecular level
- Targeted and effective interventional treatment with minimal morbidity
- Reduced risk of malignant transformation and cancer development
In this chapter, therefore, we will attempt to look towards the future to see just how some of these important issues may be resolved. It is highly likely, though, that attempts to establish the true carcinogenic risk for oral potentially malignant lesions will be the subject of epidemiological, diagnostic, pathological, molecular and translational research for many years to come. The precise interplay of these factors is a complex process, and malignant transformation is most probably the result of a combination of intrinsic and extrinsic influences acting both synchronously and metachronously in any individual patient. Undoubtedly, however, it will only be by gaining a better understanding of the mechanisms involved in oral carcinogenesis that we will be able to improve prevention, early diagnosis, treatment and prognosis for both oral precancer and ultimately invasive squamous cell carcinoma itself.
Central to future developments in oral oncology will be the need to advance our knowledge of molecular biology. As our ability to identify molecular alterations associated with various disease states increases, the need to analyse these for diagnostic and therapeutic purposes grows. The human genome, which was first draft sequenced in 2001, contains over 30 000 genes packed into 23 pairs of chromosomes, with around 40 of them involved in the control of cell replication and proliferation. As we discussed in Chapter 3, loss of cell cycle control and abnormal proliferative activity is in many ways a fundamental hallmark of oral carcinogenesis and a more detailed study of these cell cycle progression genes may help in future studies of tumour growth rates and the prediction of aggressive clinical behaviour.
Whilst numerous techniques are now available to study the molecular biology of carcinogenesis at both the genetic (genomic) or protein expression (proteomic) level, it is salutary to note that very few scientific advances have, to date, found routine application in the clinical setting. The ultimate aim of genotype-based predictive tests must be, of course, the ability to stratify risk, determine prognosis and thus personalise therapeutic intervention at an individual patient level [1].
In this chapter we will widen our discussion and look at ways in which both scientific advancement and more generalised approaches to health care may aid in the future prevention, diagnosis and treatment of oral potentially malignant disorders. We will also consider some possible future research directions that may help improve our understanding of oral precancer disease.
Whilst there are still no universally agreed management strategies for treating established potentially malignant lesions, we have presented in this book an interventional management technique based upon excision laser surgery. To date this appears one of the best studied and most efficacious diagnostic and treatment options for oral precancer.
Primary prevention, however, must be considered as the initial and perhaps most important strategy in trying to stop the development of a potentially malignant disorder in the first place, rather than surgical attempts to eliminate the disease once it has become clinically apparent. As seen and emphasised in preceding chapters, we also believe that surgical intervention remains important and retains clear practical benefits in terms of both secondary and tertiary preventive strategies.
In the future, with the rates of new oral cancer cases rising, it will become increasingly important to strengthen our efforts to facilitate primary prevention of oral potentially malignant disease.
Tobacco and Alcohol Use
Tobacco has been shown both in the developing and developed world to be the commonest risk factor for oral cancer and potentially malignant lesions. However, most smokers do not actually develop oral cancer, which not only confounds the advice we give our patients but also, of course, underlines the importance of other, presumably inherent susceptibilities or pre-existing genetic factors.
There is definite evidence that once lesions have arisen, cessation of smoking may result in the clinical resolution of oral potentially malignant lesions. Importantly, this may also help prevent further disease arising after treatment. Thus, greater and improved emphasis on smoking cessation techniques and nicotine replacement therapy remains highly pertinent in modern clinical practice. This is probably most effective if provided directly to patients as part of specialist advice in dedicated dysplasia clinics (see Chapter 7).
It is our belief that centralisation of oral potentially malignant disorder patients in a dedicated clinic provides the optimum management strategy. Within such clinics, consistent, continually reinforced, specialist advice and treatment can be available together with multidisciplinary support, particularly for identifying and modifying risk factor behaviour. In the future it would be sensible for dedicated oral precancer clinics to be established to concentrate clinical experience, facilitate rigorous audit, develop research protocols and encourage new treatment trials. This would replace the present arrangement whereby patients attend a variety of different surgical or medical clinics dependent primarily upon local preferences or upon historical clinic arrangements.
Unfortunately, despite increased awareness of smoking as a risk factor and some significant reductions in smoking behaviour, we must recognise that there is a worldwide rise in the incidence of oral cancer. Alarmingly, this seems particularly to be the case for younger patients aged less than 50 years. It is possible that the substantial increases in alcohol consumption reported to be occurring in most developed countries may be partly responsible for this. Separating the carcinogenic effects of tobacco from alcohol remains difficult as most smokers also consume alcohol, so the precise effects of alcohol and tobacco either alone or synergistically are difficult to determine. There is no doubt, however, that opportunities for clinicians to offer advice to patients on reducing alcohol consumption should be taken and may well prove effective in longer term preventive strategies.
There is increasing awareness that all clinicians should become competent in recognising harmful alcohol drinking in their patients and be able to appropriately offer intervention, in much the same way as smoking cessation therapy. For alcohol, these may include cognitive behavioural therapies, effective and assisted alcohol withdrawal protocols and the promotion of abstinence [2]. Similarly, the recognition that harmful alcohol drinking and dependence is perhaps more akin to a drug addition rather than a socially acceptable habit may ultimately help in informing populations. There is no doubt that public awareness campaigns to prevent drink driving, targeting young drinkers to prevent chronic alcohol abuse and government policies to raise the minimum price for alcoholic beverages have been beneficial and have influenced public behaviour in a positive manner in recent years.
Human Papillomavirus
Recent studies have suggested that the human papillomavirus (HPV), especially type 16, may play a causal role in a subgroup of primarily oropharyngeal, especially tonsillar and base of tongue, squamous cell carcinomas. There has been a dramatic rise in this type of oropharyngeal cancer over recent years with HPV-positive cancers occurring in young, non-smoking and non-drinking patients. This may be a new and distinct disease entity, possibly related to high-risk sexual behaviour such as increased numbers of partners and oral–genital sex. Despite the presence of often large cervical nodal metastases, however, HPV-positive cases tend to respond better to chemoradiotherapy treatments than HPV-negative patients, although smoking appears to significantly worsen their clinical outcome [3].
The role of HPV in intra-oral cancer and oral potentially malignant lesions, especially for floor of mouth and ventrolateral tongue lesions, is poorly defined at the present time and will require further research. It may be that HPV plays a role during the early stages of oral carcinogenesis or may simply be a ‘passenger’ in morphologically altered tissues. However, it is very likely that well informed patients will want to know their HPV status in the future and this may have a direct effect on clinical management decisions. Meanwhile, the role of the recently introduced female-only HPV vaccination programme in influencing oral cancer disease presentation remains to be seen [3].
Dietary Factors and Healthy Lifestyle Choices
Epidemiological evidence surrounding the role of diet with regard to the development of oral potentially malignant lesions and oral cancer remains difficult to assess. The literature suggests a causative or contributory role for low fruit and vegetable intake in oral carcinogenesis. Diets vary tremendously around the world, of course, and the many confounding effects – such as high levels of tobacco smoking and the malnutrition consequent upon excessive alcohol consumption – complicate accurate dietary assessments in patient care.
However, it is likely that future preventive strategies will emphasise healthy, well balanced diets for many types of cancer prevention as well as general health promotion advice on losing weight, regular exercise and responsible sexual health. In the future, all health care professionals will be expected to increasingly engage patients in active discussions on personal habits and risk factor behaviour before moving firmly towards encouraging active patient participation in health living schemes [4].
Increasingly, public health promotion schemes such as ‘Mouth Cancer Awareness Week’ and ‘Mouth Cancer Action Month’ in the UK have tried to raise the profile of oral cancer to the general public, whilst also developing a greater public understanding of the links between oral and general health. Whether such campaigns will have an effect on clinical disease presentation in the long term is difficult to say as unfortunately, like many public health screening programmes, the people at most risk of disease rarely access such programmes and almost never present for health advice or preventive oral examination.
Nonetheless, it is likely that these public awareness campaigns will continue and they are, of course, to be encouraged. Current advice to prevent oral cancer and information provided to patients to accompany such programmes are summarised in Box 10.2. There is now a clear emphasis on a healthy diet, exercise and sexual health alongside more traditional advice on tobacco and alcohol use.
Box 10.2 Advice to prevent oral cancer.
- Stop smoking and avoid all forms of tobacco use
- Reduce or avoid alcohol intake, and ensure alcohol-free days every so often
- Eat healthily, with plenty of fresh fruit and vegetables in daily diet
- Maintain a healthy weight and avoid obesity
- Exercise moderately on most days of the week
- Maintain sexual health and practice safe sex using condoms and barriers
Early Diagnosis of Potentially Malignant Disease
We have already discussed the significant limitations inherent in trying to screen the general population for oral disease and the difficulties in identifying and targeting high-risk groups for diagnostic intervention. It is assumed, and not unreasonably, that early diagnosis of oral potentially malignant disorders is desirable. This is based upon the hypothesis that once diagnosed, prompt intervention will stop the disease process and prevent oral cancer development. We have already seen that controversy exists as to whether either of the aforementioned aims can realistically be achieved for every patient. However, when the consequences of squamous cell carcinoma development in the oral cavity are so potentially disastrous, both in terms of patient morbidity and mortality, efforts to improve the prompt identification of precancer and early invasive oral carcinoma must be encouraged.
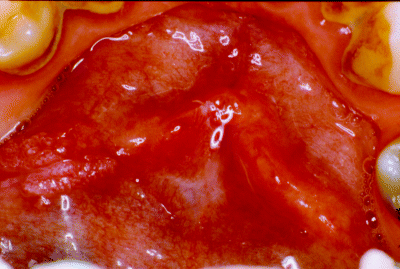
Clinical examination of the oral cavity remains first and foremost amongst the diagnostic techniques undertaken to identify suspicious oral lesions. Figure 10.1 illustrates the sometimes quite subtle mucosal changes, as seen in the floor of the mouth, which may be the first indications of precancer disease. To improve accuracy in distinguishing individuals who do or do not have malignant or potentially malignant disease, however, requires further investigation such as the use of biopsy for histopathological and/or cytological examination.
Figure 10.1 Floor of mouth mucosa demonstrating a small patch of homogeneous leukoplakia anteriorly over the opening of the submandibular duct, together with an irregular, warty, non-homogeneous lesion sited more posteriorly.
It is unlikely that any of the newer diagnostic aids reviewed in Chapter 5 will supplant standard clinical examination and incisional biopsy – which remain fundamental to the diagnosis of any suspicious oral lesion. These newer techniques are, however, proving to be useful adjuncts in specialist dysplasia clinics (see Chapters 4 and 7). Multicentre, randomised controlled clinical trials are needed to further investigate the precise role of, for example, light-based detection systems, exfoliative cytology and molecular biomarker testing.
Interventional Management Strategies in the Future
We have outlined in the preceding chapters the efficacy of interventional laser surgery in the diagnosis and management of oral precancer and early />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


