Chapter 5
Diagnostic Methods
Diagnosis refers to the act, or perhaps more appropriately, the art of identifying the precise nature and significance of a disease process presenting in a patient. This is clearly a highly unsatisfactory definition in terms of oral precancer, however, because most potentially malignant lesions are unfortunately asymptomatic for a long period during their evolution and exhibit inconsistent or unpredictable natural histories. Similarly, patients are often totally unaware of their condition and, due to the fact that many patients with risk factors do not attend regularly for dental or oral examination, abnormal mucosal appearance may remain undiscovered for many months or even years.
In most cases, the diagnosis of precancer is based upon the recognition of a suspicious-looking lesion by an experienced clinician during a routine oral examination and then ascribing an appropriate term to the lesion. This is then usually followed by an incisional biopsy of the lesion to facilitate histopathological assessment and thus confirmation of the clinical diagnosis.
Histopathological examination also allows assessesment of any significant tissue disorganisation and dysmaturation changes, which if present are categorised into varying degrees of epithelial dysplasia. We will examine the important and fundamental role of these pathological descriptors of oral precancer disease in some detail in the next chapter of this book.
Unfortunately, however, neither clinical appearance nor histopathological classification offers a reliable prognosis for individual patients or their lesions. Indeed, if clinical examination proves unsuccessful in discovering suspicious lesions, both potentially malignant states and frankly invasive tumours may all go unrecognised.
Oral examination remains the most commonly applied assessment, but there is no doubt that by itself it has limited value as a method for ensuring detection of all suspicious lesions. A number of diagnostic aids have thus been developed to try to improve detection. These include vital tissue-staining techniques, enhanced light-based detection and imaging systems and exfoliative cytology. Whilst still largely in the development phase, they all show potential as screening tools, but their application and accuracy of use requires further research in order that a precise role for each diagnostic test can be identified.
In this chapter we will review the role of population screening for oral precancer, outline the importance and efficacy of conventional visual examination of the oral mucosa, and discuss the potential use of diagnostic aids or adjuncts in precancer diagnosis and management.
Screening is defined as a structured health care intervention that is designed to detect disease at latent or asymptomatic stages, thereby interrupting disease progression or facilitating cure. On the face of it, this would seem highly appropriate for oral precancer but despite the apparent simplicity and appropriateness of a visual oral examination as a screening tool, there is actually little evidence to support oral cancer population screening [1]. This is due to:
- The difficulty in attracting high-risk patients to attend for screening.
- The presence of many benign mucosal abnormalities that confound the diagnostic process.
- The varied clinical appearance of potentially malignant precursor lesions.
- The recognition that many precancer lesions exist in clinically normal-looking mucosa.
It is also problematic that there is a lack of agreed treatment protocols for managing oral precancer lesions following their discovery and a lack of good evidence to show that subsequent preventive and therapeutic approaches markedly improve long-term patient outcomes.
Targeted screening of individuals deemed to be at high risk of carcinogenesis may offer opportunities for risk factor modification and prevention. However, case finding – which is the application of a diagnostic test to a patient who already presents with abnormal signs or symptoms in order to establish a diagnosis – and opportunistic testing of high-risk groups are probably of more greater value as tools in oral precancer diagnosis and in facilitating early interventional strategies [2].
It is well recognised that patients who smoke and drink excessively and who are thus most at risk of oral cancer are also likely to have poor diets, come from lower socioeconomic groups and are least likely to access medical services or to attend their dentist for regular oral examination. The problem therefore remains how to encourage such individuals to attend for clinical assessment. In addition there are real practical questions as to how, when and to whom they should present themselves for examination.
It would seem logical that the clinical responsibility for early identification of oral mucosal changes and the recognition of the potentially malignant nature of suspicious oral lesions should rest ultimately with dental practitioners. However, a recent study involving primary care practitioners in northern England raised concerns about the lack of a rigorous and systematic approach amongst many dentists towards not only the recognition of suspicious oral signs and symptoms, but also to the actual detection and management of established potentially malignant lesions [3]. A similar problem was also noted in relation to the difficulties facing general dental practitioners in identifying early cases of oral cancer and the perceived failure of the conventional axiom that recommends that dentists should screen all their patients for oral cancer at every routine check up [4].
The real dilemma is that public awareness of oral cancer and its associated risk factors remains generally low in most populations. It seems clear that improving public awareness of oral cancer and precancer and targeting education towards ‘at-risk’ individuals to alert them to potential signs and symptoms of early-stage disease together with a greater emphasis on prevention should now be the major priorities for future oral health care.
Clinical Examination Techniques
Careful and thorough mucosal examination by a trained clinician in a good light remains the standard method for identifying suspicious oral lesions. In view of the comments above, all clinicians should be encouraged to improve the quality of their routine oral mucosal examinations. It is also very important that the clinician adheres to a regular routine and is methodical in inspecting every region of the oral cavity to avoid missing abnormalities.
A useful method commences with examination of the anterior floor of the mouth and ventral tongue and then moves backwards bilaterally along the lateral tongue surfaces, inspecting both the lingual mucosa and then the posterior floor of the mouth. Figure 5.1 shows leukoplakia arising in the floor of mouth, whilst Figure 5.2 demonstrates probable frictional hyperkeratosis extending along lateral tongue surfaces and corresponding to the occlusal line of the teeth.
Figure 5.1 Leukoplakia of the floor of the mouth just extending onto the ventral tongue, as revealed during an anterior oral cavity examination.
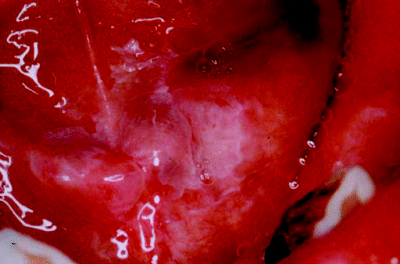
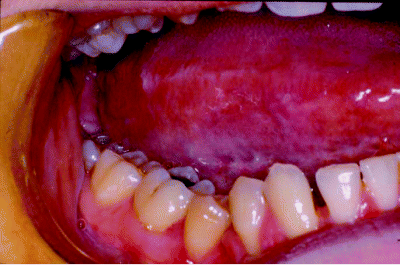
Figure 5.2 Inspection of the lateral tongue mucosa showing frictional hyperkeratosis along the occlusal line.
The patient is then asked to protrude the tongue forwards as far as they can and then to point their tongue tip first to the right and then to the left side to visualise the posterior tongue and tongue base (Figure 5.3). Whilst the tongue dorsum remains an unusual site for potentially malignant disease it is very important to obtain good visualisation of the posterolateral lingual mucosa, where precancer commonly presents. In an alternative technique, the clinician can gently manipulate and manoeuvre the tongue with a damp swab but this is uncomfortable and many patients are intolerant, which can lead ultimately to a poorer quality examination.
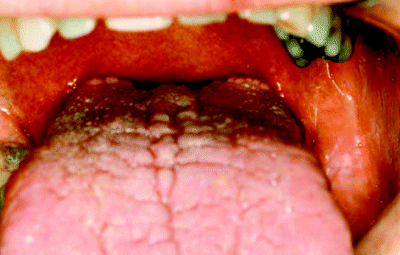
Figure 5.3 Direct visualisation of the posterior third of the tongue is best achieved by asking the patient to protrude their tongue as far forwards as possible.
The lingual mandibular gingiva and retromolar areas are then examined, aided by the use of a dental mirror. This can be a difficult area to visualise but, as illustrated in Figure 5.4, many potentially malignant lesions arise at these sites and can remain hidden unless specifically looked for.
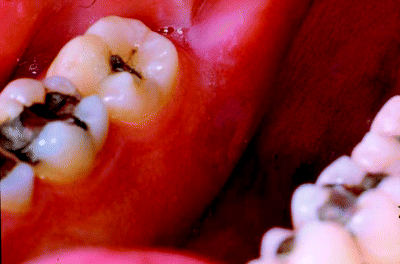
Figure 5.4 The lingual retromolar region, here showing a localised erythroleukoplakia, is best visualised by dental mirror examination.
The patient is then asked to say ‘Ah’ which allows direct visualisation of the faucial pillars, tonsils and soft palate. In many cases tongue depression with a spatula or mirror may improve the view, but some patients are actually quite intolerant of this manoeuvre, resulting in a poorer examination. Figure 5.5 illustrates a diffuse leukoplakia covering most of the soft palate mucosa.
Figure 5.5 The soft palate is usually best visualised by both tongue depression and instructing the patient to say ‘Ah’, here illustrating a diffuse leukoplakia.
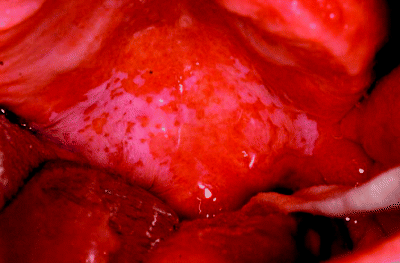
The hard palate and palatal gingiva are best seen by direct visual inspection (Figure 5.6), as is the buccal mucosa. The latter should be examined bilaterally starting posteriorly at the pterygomandibular raphe and finishing anteriorly by careful inspection of both labial commissures and then the upper and lower lip mucosa and vermilion borders. Figure 5.7 demonstrates an extensive buccal mucosal lichenoid lesion and Figure 5.8 illustrates a feint leukoplakia arising at the labial commissure and extending backwards along the buccal mucosa.
Figure 5.6 Direct visualisation of the edentulous maxillary alveolus and hard palate showing bilateral alveolar leukoplakic lesions.
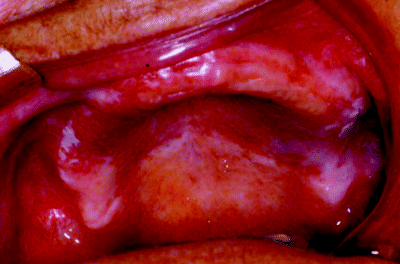
Figure 5.7 Buccal mucosa examination revealing an extensive lichenoid lesion.
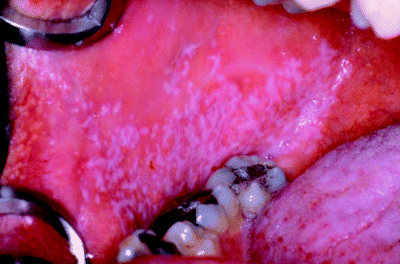
Figure 5.8 Feint leukoplakia arising in the labial commissure region and extending backwards along the buccal mucosa.
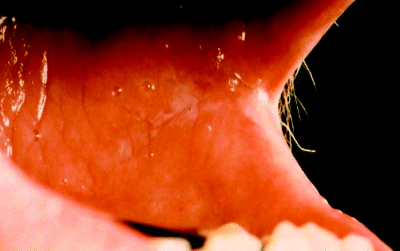
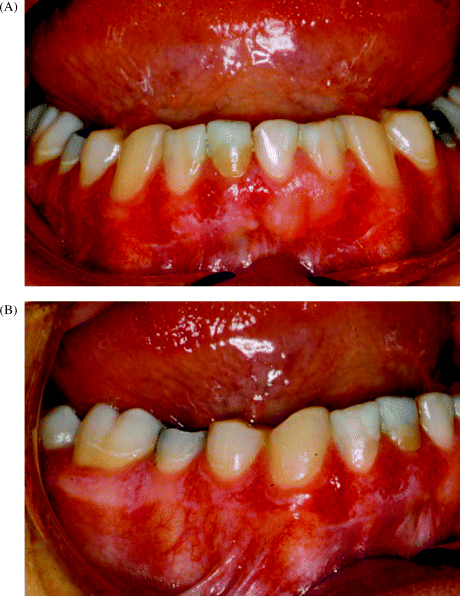
Finally, the patient is asked to close the teeth together and all labial and buccal gingival surfaces are examined. It is surprisingly easy to miss subtle leukoplakic lesions on gingival surfaces, as shown in Figure 5.9, unless careful examination is performed.
Figure 5.9 Mandibular gingiva demonstrating widespread feint leukoplakia at both labial (A) and buccal (B) sites.
If a suspicious mucosal lesion is found, its location, size, morphology and surface characteristics should be recorded. Lesions should then be gently palpated with gloved fingers, which helps determine whether they are soft and mobile or of more sinister nature – appearing firm, indurated, fixed to underlying structures and friable or haemorrhagic. Leukoplakic lesions should be further assessed to see if they can be wiped away by careful use of a damp swab, in which case the diagnosis may well be that of an acute pseudomembranous candidosis. Sometimes, feint or inconsistent lesions can be visualised better and finer details revealed by gentle application of a dry swab to remove overlying moisture on the mucosal surface.
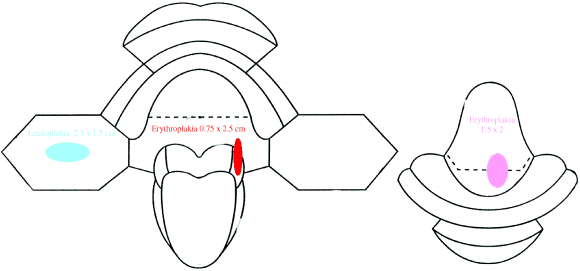
It is important that the findings of clinical examination are recorded accurately and concisely. Some clinicians will record the lesion diagrammatically or enter it on a mouth map (Figure 5.10) to demonstrate both size and location. Others prefer to photograph lesions and include these records in patients’ notes, which is particularly helpful in hospital practice where patients may not always be reviewed by the same clinician at each clinic visit.
Figure 5.10 A mouth map used to record the site, shape, size and clinical description of potentially malignant lesions.
Following thorough visual inspection, the clinician will then have to determine which further investigations are required. Box 5.1 summarises the investigations that may be required to establish a complete diagnosis for a newly presenting oral precancer patient.
Box 5.1 Investigation of the oral precancer patient.
- Patient history:
Identification of risk factors
Recognition of medical conditions predisposing to precancer
- Clinical examination:
Visual inspection of oral mucosa
Palpation of oral lesions
Wiping away pseudomembranous conditions
- Clinical investigations: oral swab for microbiological assessment
- Blood tests:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


