Chapter 4
Clinical Presentation of Oral Precancer
Despite the tremendous advances seen in both molecular biology and also within the related sciences of genetics and epigenetics, the ability of individual clinicians to recognise and identify oral potentially malignant disorders, with their myriad of clinical presentations and subtle changes in mucosal appearance, remains absolutely fundamental to their accurate clinical diagnosis and subsequent management.
The term oral precancer was originally defined to include both discrete oral lesions and more widespread conditions, affecting not only the oral mucosa but also the patient in general, both of which demonstrate a variable and unpredictable potential to transform into invasive squamous cell carcinoma.
The new, preferred definition of oral potentially malignant disorders is probably a more encompassing term as it really implies a spectrum of morphological changes in oral mucosal tissue, many (but not all) observable clinically, which may show not only an increased potential for site-specific malignant transformation but also a risk of cancer development at other apparently clinically normal-looking oral sites.
This chapter is concerned with the clinical appearance of such potentially malignant changes in the mouth and the manner in which individual patients and disorders may present to clinicians. It is important to appreciate that, unfortunately, the vast majority of these conditions are symptomless and usually go unnoticed by patients until they have become quite extensive in size, have developed mucosal thickening or have become irritated in some way.
For practical purposes, therefore, this really means that most potentially malignant disorders will be found initially by dental practitioners during routine oral examinations, dental inspections or via oral health screening. Some patients, however, on eventually noticing symptoms may consult their general medical practitioner for advice regarding oral mucosal lesions. This is less common and can sometimes lead to delays in patient referral due to a lack of medical practitioners’ experience in oral diagnosis.
Similarly problematic are the difficulties in identifying high-risk patients, the limitations of general population screening tests for oral cancer and the problems consequent upon the unpredictable and inconsistent natural history of oral precancer, all of which conspire to confound the diagnostic process. These issues will be explored in some detail in both this chapter and succeeding chapters of this book.
There remains little doubt, however, that a careful and methodical clinical examination by an experienced and alert clinician in an appropriate setting and with good lighting is the most reliable means of identifying oral lesions with the propensity for malignant transformation.
In Chapter 1 we listed a number of definitions relevant to the study of oral precancer. It is useful to review here and expand on some of these definitions, both those that have been used in the past but also and perhaps most importantly those currently favoured in the scientific literature to describe the varied clinical spectrum of oral precancer disease presentation. The wide range of both lesions and conditions that comprise oral potentially malignant disorders are summarised in Box 4.1.
Box 4.1 Clinical presentation of oral precancer disease.
Oral precancerous lesions
- Leukoplakia
- Erythroplakia
- Erythroleukoplakia
Oral precancerous conditions
- Immunosuppression
- Oral submucous fibrosis
- Lichen planus and lichenoid lesions
- Sideropenic dysphagia
- Discoid lupus erythematosus
- Actinic cheilitis
- Chronic hyperplastic candidosis (candidal leukoplakia)
- Syphilis
- Dyskeratosis congenita
The term oral precancerous (or premalignant) lesion remains an extremely useful definition and was originally described by the World Health Organisation (WHO) in 1978 and referred to ‘morphologically altered tissue in which cancer is more likely to occur than in its apparently normal counterpart’. This is very pertinent, as it highlights the significance of the epithelial tissue disorganisation and dysmaturation (encompassed by the histopathological term dysplasia) that is such an integral structural antecedent of neoplastic transformation.
Oral precancerous (or premalignant) conditions, in contrast to their discrete mucosal counterparts, however, are more generalized states associated with a significantly increased risk of cancer and include a range of systemic disorders in which oral manifestations are but one of many important disturbances.
A variety of other terms can be found in different publications through the years, all of which have been used to describe oral precancers, including: oral epithelial dysplastic lesions, epithelial precancer lesions, intraepithelial neoplastic lesions and oral or epithelial precursor lesions. This can lead to confusion for readers, especially when attempting to compare and contrast various clinical observations and analyses in published articles.
Thus, in 2007, a comprehensive review of both nomenclature and classification was undertaken following a workshop of the WHO Collaborating Centre for Oral Cancer and Precancer in the UK, and the new encompassing term, potentially malignant disorders, was proposed [1]. This term was felt to be particularly appropriate not only because not all precursor lesions inevitably transform into malignancy, but perhaps more significantly because of the recognition of field change carcinogenesis. Rather than discrete lesions and widespread conditions existing as separate entities there is a clear spectrum of potentially malignant disease, rendering the whole of the upper aerodigestive tract in such patients susceptible to malignant change.
We must therefore recognise that there exists within potentially malignant disorders a continuum of clinical presentations from discrete mucosal lesions through to more generalised or widespread precancerous conditions. Nonetheless, it remains helpful for the purposes of our description and analysis in this chapter to distinguish these various disorders in terms of lesions and conditions.
Precancerous (Premalignant) Lesions
Leukoplakia
Leukoplakia is by far the most common clinical presentation of oral precancer, accounting for 60–70% of all potentially malignant lesions [2, 3]. The abnormal and/or increased keratin production characteristic of leukoplakia enhances tissue hydration by saliva resulting in the white appearance seen clinically in affected mucosa.
The classic definition of leukoplakia is thus of a ‘white patch on the mucosa, which cannot be wiped off and which cannot be ascribed clinically or histologically into any other definable category’. Others have added that the white patch should not be associated with the use of any physical or chemical causative agent except tobacco, helping to emphasise the significance of tobacco in the aetiology of precancer disease [1].
Such an unqualified ‘diagnosis by exclusion’ is somewhat unsatisfactory, however, as it fails to emphasise the significant risk of dysplastic change and its consequent malignant potential within such lesions. The principal distinguishing feature of leukoplakia from other oral keratoses (white patches with thickened keratin layers) is indeed the histopathological recognition of epithelial dysplasia, and these important pathological features of leukoplakia will be discussed in more detail in Chapter 6.
Numerous attempts to refine the diagnosis of leukoplakia have therefore taken place, including the 2005 amended WHO clinical definition of ‘white plaques of questionable risk, having excluded (other) known diseases or disorders that carry no increased risk for cancer’. This is useful as it emphasises the risk of carcinoma development, which is of course the principal concern in diagnosing and managing such lesions.
There are, however, no clear histological requirements for a white mucosal lesion to fulfil this definition and leukoplakia remains, as it always has been, very much a clinical descriptive term.
Oral leukoplakia has a reported prevalence of 2–3% worldwide and is significantly more common in males although, as we have seen, females are also affected [4]. In the developed nations, leukoplakias are usually seen in middle-aged or elderly patients especially between the fifth and seventh decades. However, there is no doubt that in the European setting we have experienced a demonstrable and significant increase in the number of younger patients presenting with leukoplakic lesions.
Leukoplakia is six times more common amongst smokers than non-smokers and can affect any part of the oral cavity and oropharynx. However, the buccal mucosa worldwide and the floor of the mouth and ventrolateral tongue in Western populations are probably the commonest anatomical sites affected [2, 3]. The precise site of leukoplakia development in a population is probably influenced to a large extent by the preferred local tobacco habit. Tobacco smoking is thus associated particularly with leukoplakia on the buccal mucosa, ventral tongue surfaces and the floor of the mouth, whilst buccal lesions alone are commonly seen where tobacco chewing habits predominate, with palatal lesions seen uniquely in reverse smokers. The latter is a particular habit in which the lighted end of a coarse cheroot (or chutta) is held inside the mouth, particularly seen in females from a number of Indian coastal districts.
Schepman et al. (2001) reviewed 166 oral leukoplakia patients in a Netherlands population and noted that whilst the floor of the mouth was the commonest overall site of origin for leukoplakia in smoking patients, male smokers also showed a propensity for lesions to appear at the labial commissure and buccal mucosal regions. In contrast, leukoplakias arising on the lateral borders of the tongue were most commonly seen in non-smoking females. Interestingly, there appeared to be no clear explanations why such specific gender differences should exist [5].
There are a number of factors, however, that are readily defined and identifiable in patients and which may contribute to determining the site of origin of individual leukoplakia lesions. These are summarised in Box 4.2. In addition, Table 4.1 lists the varying clinical appearance and presentation of a number of different leukoplakic lesions that may arise in response to a range of smokeless tobacco habits carried out worldwide. These were discussed in Chapter 3 and include different forms of oral snuff, various tobacco chewing habits and the use of tobacco products mixed with areca nut or lime and applied to the oral mucosa.
Box 4.2 Factors influencing the site of oral leukoplakia presentation.
Oral mucosa
- Type and extent of mucosal keratinsation
- Mucosal permeability
- Epithelial cell proliferative activity
Oral environment
- Salivary pooling
- Mucosal irritation
- Oral hygiene
Tobacco habit
- Tobacco smoking
- Cigarette placement/habitual cigarette holding
- Reverse smoking habits
- Smokeless tobacco use
Table 4.1 Aetiology and clinical presentation of oral smokeless tobacco lesions.
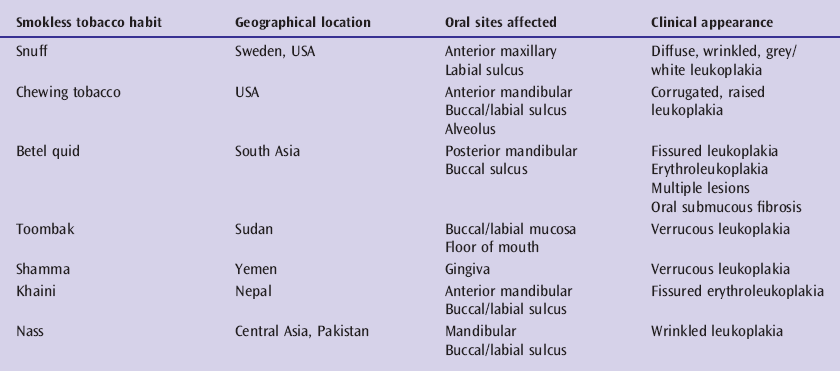
It is clear that site-specific lesion presentation is directly linked to the type of smokeless tobacco used and the preference to habitually place the product at a particular intra-oral location. Lesions tend to evolve with prolonged use of the tobacco product, varying from an initial superficial wrinkling of the mucosa through white/gray discolouration to thickened, white, deeply furrowed or verrucous lesions. Whilst some authors have sought to distinguish smokeless tobacco lesions from their smoking-related leukoplakic counterparts, they are probably all best regarded as part of the overall spectrum of oral potentially malignant disorders [6].
It is also important to appreciate that the many differences seen in quoted figures for overall leukoplakia incidence and prevalence undoubtedly exist not only because of variations in geographic location but also because of differences between types of patients studied. This is especially so for the distinction between general community-based population studies compared with specialist hospital clinic studies. The pattern and presentation of precancer disease in the latter will be highly and selectively influenced by both patient referral patterns and clinician interest and awareness.
Once fully established as a mucosal lesion, leukoplakia may appear clinically in a variety of different forms and it is important that clinicians are aware of these many and often subtle variations (Box 4.3). What remains unclear, however, is how long it takes individual leukoplakic lesions to become clinically apparent, nor is it certain how many lesions may actually change or alter their appearance with time.
Box 4.3 Clinical appearance of leukoplakia.
Homogeneous
- Feint
- Thick
- Ribbed/rippled (ebbing tide)
Non-homogenous
- Warty/thickened
- Nodular
Mixed homogenous/non-homogenous
Verruciform
- Simple verrucous
- Proliferative verrucous leukoplakia
Nonetheless, a number of general observations can be made. Homogeneous leukoplakias are defined as flat and uniformly white throughout the entire lesion, appearing as either feint patches (Figure 4.1) or as much thicker lesions, sometimes resembling a coating of paint (Figure 4.2). On other occasions, whilst remaining uniform, the leukoplakia may exhibit a ribbed or rippled appearance, sometimes compared to the appearance of the ebbing tide at the sea shore. This is shown presenting on the posterior buccal mucosa in Figure 4.3.
Figure 4.1 Feint, homogeneous leukoplakia arising in the anterior floor of the mouth.
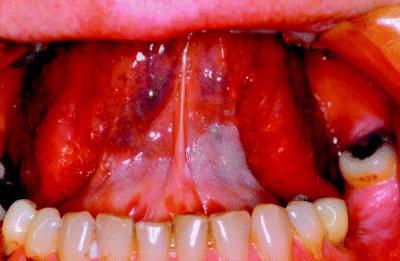
Figure 4.2 Thick, paint-like leukoplakia irregularly distributed on the floor of the mouth.
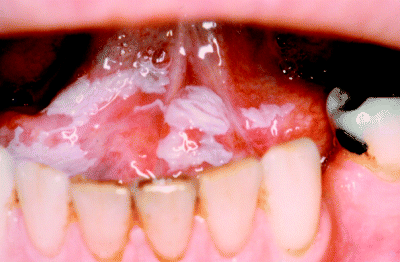
Figure 4.3 Wrinkled or ‘ebbing tide’ leukoplakia arising on the posterior buccal mucosa.
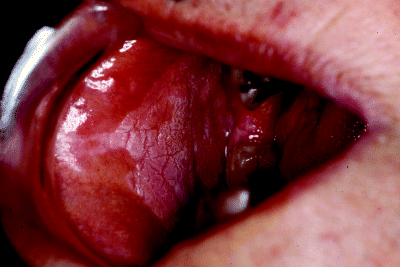
Non-homogeneous leukoplakia can appear as irregular, widespread, thickened areas as seen arising in the floor of the mouth and ventral tongue in Figure 4.4 or as more localised nodular lesions as illustrated on lateral tongue mucosa in Figure 4.5. Mixed patches of homogenous and non-homogenous lesions are also observed, usually when widespread areas of mucosa are affected such as in the buccal mucosa of Figure 4.6.
Figure 4.4 Irregular, widespread and thickened leukoplakia arising in the ventral tongue and spreading onto the floor of the mouth.
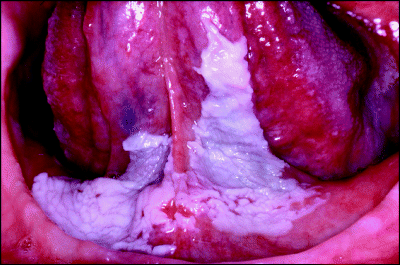
Figure 4.5 Localised, nodular leukoplakia on the lateral border of the tongue.
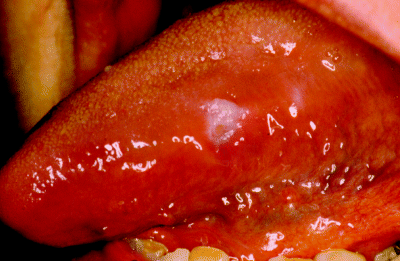
Figure 4.6 Mixed, non-homogeneous leukoplakia arising on the buccal mucosa and comprising feint, wrinkled (‘ebbing tide’) and nodular components.
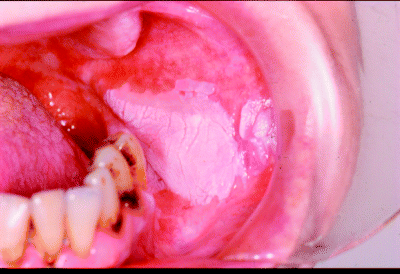
Whilst some leukoplakias present as small, distinct lesions, other patients may exhibit extensive and widespread mucosal disease. These range from large, feint, diffuse leukoplakias to multiple lesions presenting at distinct oral sites separated by normal-looking mucosa. The patient who presents with multiple, synchronous, leukoplakic lesions is probably representative of a specific and distinct precancer disease entity and a detailed description of this will be presented later in this chapter.
The term verrucous leukoplakia has often been applied to a particular clinical presentation of a non-homogeneous lesion that differs from flat homogeneous leukoplakia by its extremely wrinkled, corrugated and warty texture. It may be clinically indistinguishable from verrucous carcinoma, which is a rare, primarily locally invasive variant of oral squamous cell carcinoma [7]. Figure 4.7 demonstrates a particularly florid example of a verrucous leukoplakia extending from the mandibular alveolus into the floor of the mouth in an elderly edentulous patient.
Figure 4.7 Extensive verrucous leukoplakia arising on the mandibular alveolus and extending into the floor of the mouth and buccal sulcus. Note the papillomatous buccal lesion nearby.
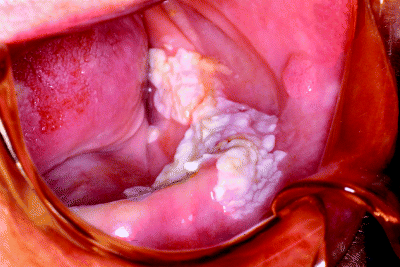
Proliferative verrucous leukoplakia (PVL) is a rare but more recently recognised and important subgroup of leukoplakic lesions. These lesions are slow growing and progressive and appear as expanding, fissured, exophytic and warty-looking white patches, characterised by multifocal presentation, resistance to treatment and a high rate of malignant transformation, often in the absence of identifiable dysplastic features on previous biopsy. Whilst PVL lesions usually present initially as slowly expanding solitary, asymptomatic, white lesions these inevitably progress over time as multiple similar lesions occur, ultimately progressing into large, warty masses. Although lesions may be removed surgically, there is a high rate of both recurrence and new lesion development [8].
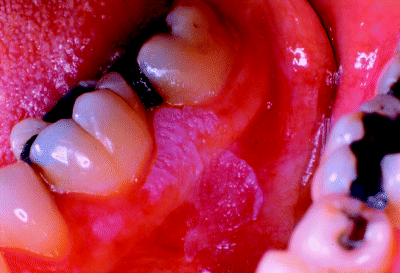
PVL lesions most frequently present on the gingiva, and the alveolar and buccal mucosae, typically arising in patients in their sixth or seventh decades and more commonly in women than men. The precise aetiology of PVL is obscure and, unlike others forms of oral leukoplakia, there appears to be no strong association with the use of tobacco and alcohol. Figure 4.8 shows a relatively localised PVL lesion arising on the mandibular buccal gingiva, whilst Figure 4.9 illustrates a much more widespread presentation involving most of the attached gingiva. The lesions shown in Figure 4.10, however, are more characteristic of the typical multifocal appearance of proliferative verrucous leukoplakia involving both the gingiva and palatal mucosa.
Figure 4.8 Relatively localised, proliferative verrucous leukoplakia involving the mandibular buccal gingiva and alveolar mucosa and extending into the buccal sulcus.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


