Chapter 9
Malignant Transformation and Oral Cancer Development
The transformation of precursor potentially malignant lesions into invasive carcinoma must be seen as the ultimate failure in diagnosis and management of oral precancer. Clinical examples of squamous cell carcinoma that have arisen from pre-existing tongue leukoplakias are illustrated in Figures 9.1 and 9.2. The fact that such oral leukoplakias still unpredictably transform into cancers remains a major frustration to clinicians, particularly as we are still unable to predict how quickly or how likely any individual patient or any potentially malignant disorder will proceed towards cancerisation.
Figure 9.1 An infiltrative squamous cell carcinoma arising in a pre-existing non-homogeneous leukoplakia on the ventrolateral tongue.
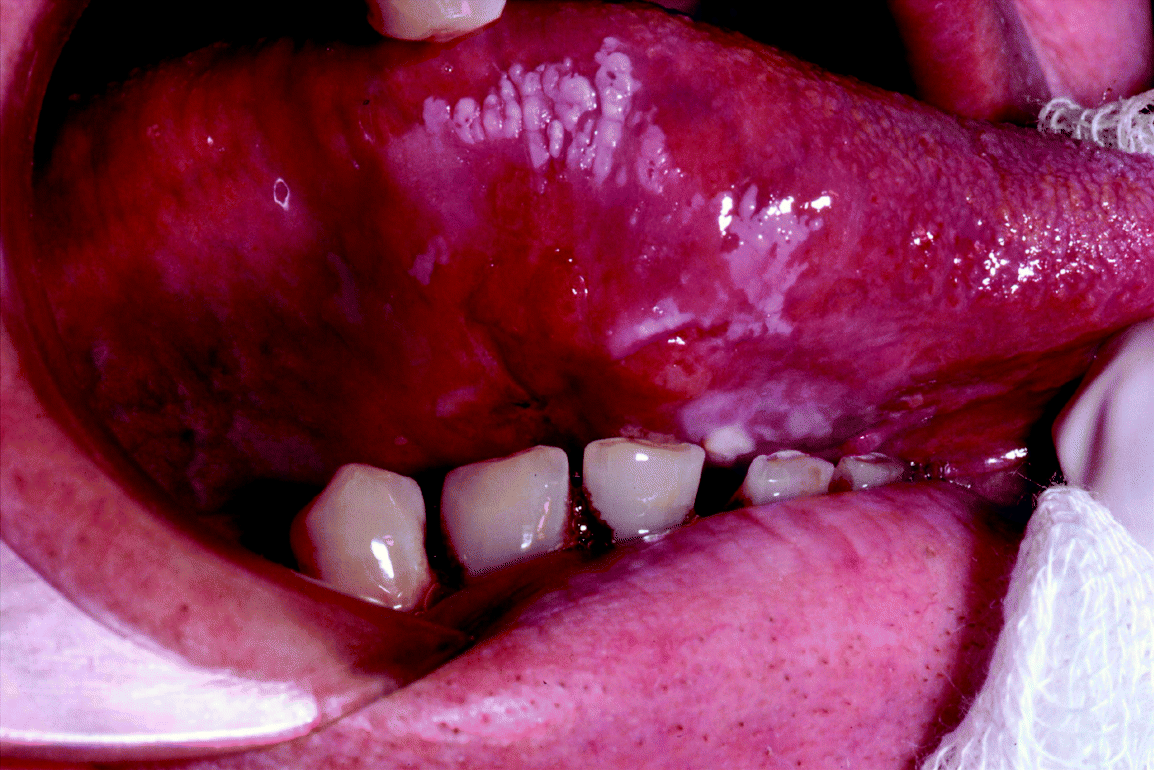
Figure 9.2 An ulcerative squamous cell carcinoma arising from a pre-existing non-homogeneous ventral tongue leukoplakia.
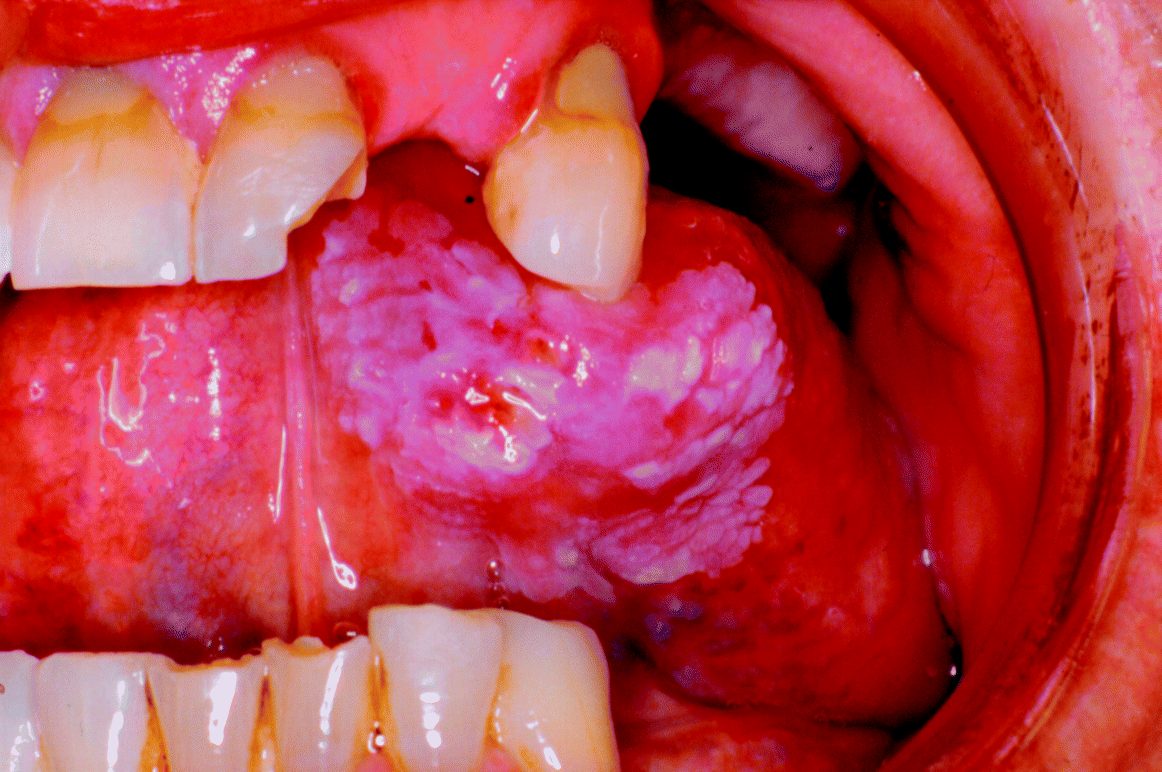
Quoted transformation rates to oral malignancy vary widely in the published literature, from around 0.1% to over 40%. The interpretation of such data is complicated by the heterogeneous clinical and histopathological nature of different precursor lesions studied and the varying length of follow-up periods in different reported series.
In Chapter 8 we considered the overall spectrum of clinical outcomes that may be seen following the diagnosis and management of oral precancer lesions. Unfortunately, many of the difficulties we experienced in interpreting the available scientific literature to enhance our understanding of the natural history of the disease apply equally well to our desire to clarify our knowledge of oral carcinogenesis. In this chapter, therefore, we will review some of the salient concepts surrounding our current understanding of oral precancer transformation to malignancy and, using data obtained from observational studies following cohorts of treated Newcastle patients (see Chapter 8), will make recommendations both for the terminology of disease recognition and for clinical patient management.
Risk of Progression to Oral Carcinoma
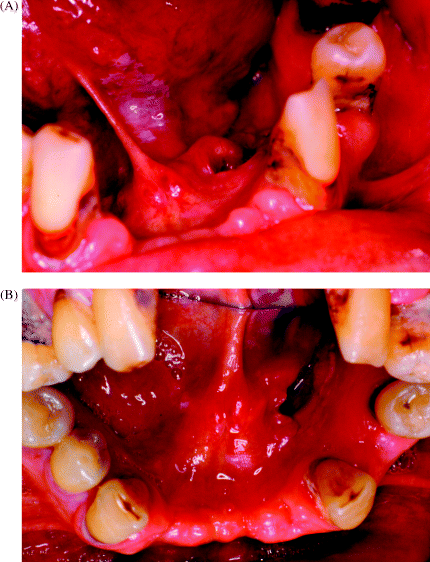
There are, unfortunately, very few reliable data sets available in the literature that help to provide either a consensus or a pragmatic view regarding the risk of cancer development in oral potentially malignant disorder patients. Figure 9.3 summarises the clinical dilemma in predicting the likely clinical outcome in a patient who presented with widespread, multiple foci of ventral tongue and floor of mouth leukoplakia.
Figure 9.3 Widespread distribution of leukoplakic foci affecting the ventral tongue (A), and also involving the floor of the mouth and the lingual surface of mandibular alveolar mucosa (B). There is a high risk of malignant transformation in such a case, but it remains impossible to predict which site is most at risk.
An overall malignant transformation rate of approximately 12% over a mean time to malignant transformation of 4.3 years has recently been quoted. How reliable these data are, obtained from 14 non-related studies in a variety of different countries over a 40-year period, in determining a relevant risk calculation remains far from clear [1]. Mehenna et al. [1] had, in fact, actually identified a total of 2837 possible precancer progression papers in the literature over the 40-year search period in their attempt to establish a systematic review and undertake a meta-analysis to try and determine overall risk of cancer development. However, the fact that only 14 publications were ultimately deemed suitable for formal review in this way highlights the practical limitations of this type of research.
It is important to note that Mehanna et al. emphasised that the only effective treatment for oral dysplastic lesions appears to be surgical excision. Although not eliminating the risk of cancer completely, excision does appear to decrease the risk of malignant transformation of potentially malignant lesions by more than a half [1]. These authors also observed a higher malignant transformation rate of 24.1% in severely dysplastic lesions compared with 10.3% for mild to moderately dysplastic ones. They were unable to comment on the relative risk in relation to other factors such as patient gender, smoking status, alcohol use and lesion site [1].
A number of observational, follow-up studies exist in the published literature. These are worth considering in some detail, not only to summarise our current knowledge base, but also to help appreciate the limitations of our real understanding of the risks of oral carcinogenesis in potentially malignant disorder cases.
Silverman et al. in a paper from 1984, reviewed 257 patients with oral leukoplakia who were followed for an average period of 7.2 years. They observed that, overall, 45 patients (or 17.5%) subsequently went on to develop a squamous cell carcinoma, usually within a 2-year observation period. However, only 22 of the 257 patients actually demonstrated dysplasia on initial microscopic examination so that the true transformation rate for dysplastic lesions was actually 36.4% [2]. These authors also noted that high risks for malignant transformation included non-smoking patients, females, lesions with red or erosive characteristics, verrucous hyperplastic lesions, and lesions exhibiting dysplasia on microscopy. In addition, they remarked that an increasing number of cancers were likely to be seen as the length of follow up increased [2].
Hogewind et al. in 1989 similarly observed an increased risk of oral cancer development in older, female patients by following 84 leukoplakia cases for an average period of 5 years. In total, three out of the 84 patients developed cancer, producing a malignant transformation rate of 3.6% [3].
Lumerman et al. in 1995 reported a 16% malignancy transformation rate: seven cases of cancer developed out of 44 patients with oral epithelial dysplasia, within a mean follow-up period of about 34 months. Two of the seven cancer patients in this series developed their tumours at sites distant from the original dysplasia [4]. Interestingly, these authors also combined the results of their study with four previous publications over the preceding 25 years and observed that whilst 6% of 65 patients who had their precancer lesions excised developed carcinoma, the figure rose to over 15% of 91 cases who received no treatment [4]. Clearly, there are significant limitations in combining unrelated studies, but it is interesting to note that Lumerman et al. clearly concluded that surgical intervention should be recommended for all patients presenting with oral dysplastic lesions.
In 1998 in a review of 166 patients with leukoplakia seen over a 24-year period, Schepman et al. observed that 20 patients (or 12% of cases) developed squamous cell carcinoma at a median time of 32 months of follow up, although no distinction was made in this study between same-site malignant transformation and carcinoma development elsewhere in the oral cavity [5]. Parameters associated with an increased risk of malignancy included female patients, non-smokers (especially females) and a non-homogeneous clinical appearance of individual lesions. The authors stated that patients who had ‘any form of intervention’ did not have a significantly lower risk of malignant transformation compared with non-intervention cases [5]. However, this was a highly retrospective study incorporating a variety of different treatment modalities instituted at varying times in the disease history rendering specific observations on the efficacy of treatments somewhat unreliable.
Cowan et al. in 2001 carried out a retrospective review of histopathology records over a 20-year period and estimated that 14% of 165 identifiable oral dysplastic lesions transformed to squamous cell carcinoma at an average interval from diagnosis of 48 months [6]. Whilst a number of interesting observations and suggestions were made by these authors, this study is clearly limited both by it being based upon histopathology laboratory data and also because of the highly retrospective nature of such data collection.
In reviewing 1458 Taiwanese patients who presented over a 10-year period with a variety of potentially malignant disorders, Hsue et al. reported an overall malignant transformation rate of 3% [7]. On closer inspection of the data, only 166 cases actually exhibited dysplasia and the majority of those showed only mildly dysplastic features; eight of these 166 cases progressed to malignancy, providing a transformation rate of nearer 4.8%. This again emphasises the limitations of such retrospective review studies even in the presence of apparently large numbers of patients.
In a more recent retrospective review of 207 patients presenting with oral epithelial dysplasia over a 16-year period, Arduino et al. in 2009 observed malignant transformation in 7.24% of cases (15 patients) occurring at a median time of about 30 months follow up. The vast majority of lesions studied showed mild dysplasia only, however, and the authors were unable to determine a predictive role for dysplasia severity [8]. A variety of uncoordinated treatment modalities were performed on 133 patients, including scalpel excisions and cryotherapy, whilst the remaining 74 patients underwent a ‘wait and see’ policy. Unfortunately, no clear rationale for any treatment decision appears to have been recorded and there seems to be a conspicuous lack of any cohesive or coordinated treatment protocol for precancer patients [8]. Perhaps unsurprisingly, in view of the above inconsistencies, the authors were unable to predict the risk of malignancy development, noting that neither the clinical type nor site of lesion, nor patient age, gender or risk factor behaviour influenced carcinogenesis, although non-homogeneous lesions were once again thought to be at an increased risk [8].
Ho et al. reviewed malignant transformation of potentially malignant disorders in a further Taiwanese population study of 148 male patients presenting over an 18-year period. There were, however, only 33 patients in this study with biopsy-proven epithelial dysplasia. Eight of these progressed to malignancy so that although the authors quoted an overall 7.6% transformation rate, the real percentage transformation for dyplastic lesions was actually 24% [9]. Whilst these authors noted that the tongue seems to be at particular risk of malignancy and that transformation is more common in the first 2–3 years after diagnosis [9], the heterogeneity of the study group, the lack of any treatment intervention and the small number of true dysplasia cases studied must question the overall relevance of this paper. However, Ho et al. do make an interesting point in their paper regarding the calculation of malignant transformation rates. Criticising the simple mathematical estimate of transformation using the number of malignant cases divided by the total number of study patients, they usefully emphasise that individual person—time malignant transformation rates are more appropriate calculations, particularly as the incidence of cancer is known to increase with the length of follow-up period [9].
Nonetheless, it is clearly important to stress that many published papers have quoted overall malignant transformation rates, varying from 3% to 17%, for heterogeneous patient populations often containing substantial numbers of lesions without dysplastic features. When these malignant transformation rates are recalculated using only dysplastic precursor lesions, the risk of malignancy increases to between 24% and 36%. Whilst it is recognised that lesions apparently without dysplasia may transform this is relatively rare, and most commentators have reported an increasing risk with the more severely dysplastic lesions, as summarised by Mehenna et al. [1].
The fundamental problem remains that all of the above studies are of highly variable quality, with different patient populations presenting with mixed dysplastic and non-dysplastic lesions, and inconsistent treatment and follow-up regimes. Similarly, and of considerable clinical significance, is that the actual site at which oral cancer develops is not clearly defined in many of the studies, thus failing to distinguish between site-specific malignant transformation and new-site cancer development.
Napier and Speight recently published an overview of the natural history of oral potentially malignant disorders. In relation to malignant transformation, they listed a number of possible factors predictive of cancer development [10]. These are summarised in Box 9.1 and include increased patient age, female patients, lesions present for a prolonged time, lesions arising in the floor of mouth, lateral tongue and retromolar regions, non-homogeneous leukoplakias and erythroplakias, d/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


