1
Examination and Diagnosis
Case 1: Examination and Documentation
Walter S. Krawczyk, DDS, and Anisha K. Thondukolam, DDS
Case 2: Plaque-Induced Gingivitis
Nadeem Karimbux, DMD, MMSc, and Satheesh Elangovan, BDS, DSc, DMSc
Case 3: Non–Plaque-Induced Gingivitis
N. Joseph Laborde III, DDS, and Mark A. Lerman, DMD
Case 4: Gingival Enlargement
T. Howard Howell, DDS, and Maria Dona, DDS, MSD
Case 5: Aggressive Periodontitis
Nadeem Karimbux, DMD, MMSc, Satheesh Elangovan, BDS, DSc, DMSc, and Martin Ming-Jen Fu, BDS, MS
Case 6: Chronic Periodontitis
Ricardo Teles, DDS, DMSc
Case 7: Local Anatomic Factors Contributing to Periodontal Disease
Daniel Kuan-te Ho, DMD, MSc, and David M. Kim, DDS, DMSc
Case 1
Examination and Documentation
CASE STORY
A 40-year-old African-American male (LD) in no apparent distress presented with a chief complaint of: “My dentist told me I have gum disease and I should see a periodontist.” Figures 1–5 are the patient’s intraoral photographs.
Figure 1: Frontal view.
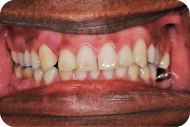
Figure 2: Maxillary view.
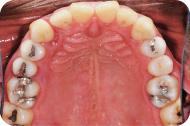
Figure 3: Mandibular view.
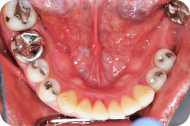
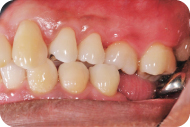
Figure 4: Right occlusal view.
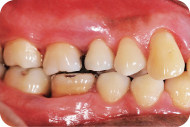
Figure 5: Left occlusal view.
LEARNING GOALS AND OBJECTIVES
- The patient’s chief complaint
- Medical and dental history
- Soft tissue and gingival examination
- Periodontal charting
- Radiographic interpretation and diagnosis of periodontal condition
Past Dental History
This patient denied having bleeding gums during brushing or flossing, he had no loose teeth, and he was not in pain. The patient claimed to brush twice a day and flossed sporadically. His last dental visit was a year ago for a cleaning.
This particular patient presented with a blood pressure of 140/90, a pulse of 70 beats per minute, and a respiration rate of 14 breaths per minute. The patient denied having any significant health problems, had no known allergies, and denied taking any medications.
Soft Tissue and Gingival Examination
The patient had no pathologic masses or lesions upon extraoral and intraoral examination (Figures 1–5). He presented with generalized coral pink gingiva with normal pigmentation, scalloped gingival contour with knife-edged margins, pyramidal papillae with localized areas of blunted papilla, stippling, localized areas of recession, and firm consistency with localized edematous areas. There was mild plaque, with no significant supra/subgingival calculus. There was some normal pigmentation associated with the attached gingiva (Figures 1, 4, and 5).
Periodontal Charting
A thorough periodontal examination was completed. The periodontal chart (Figures 6 and 7) shows that the patient had generalized bleeding on probing, minimal plaque, pocket depths ranging from 2 to 15 mm with the more severe probing depths in the posterior teeth, class 1–2 furcations, class 1–3 mobility, and localized recession.
Figure 6: Maxillary periodontal charting.
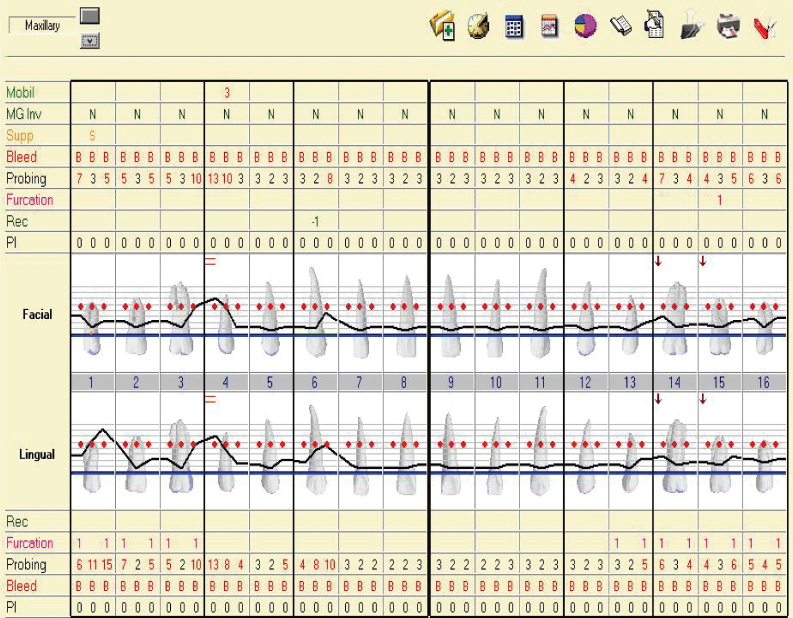
Figure 7: Mandibular periodontal charting.
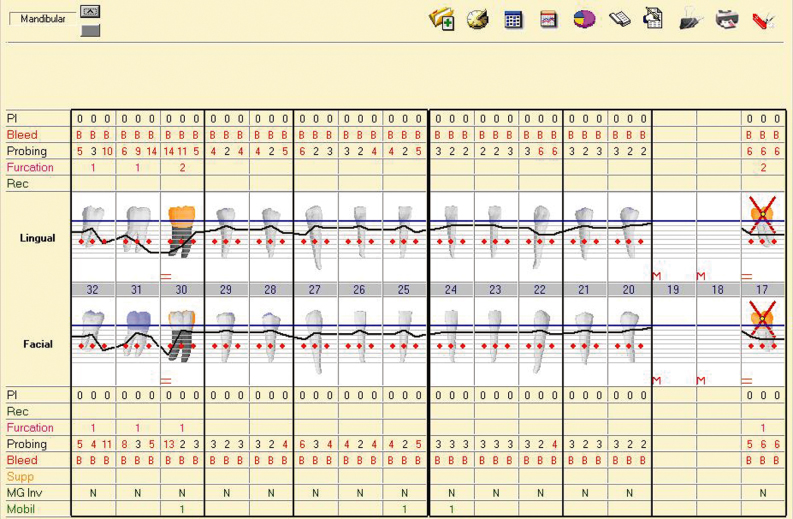
Radiographic Examination
From this full mouth radiograph (Figure 8), generalized bone loss is evident with severe bone loss surrounding #4, #6, #7, and #30. Bone loss in the furcation area is evident for #17 and #30.
Figure 8: Full mouth series radiographs.
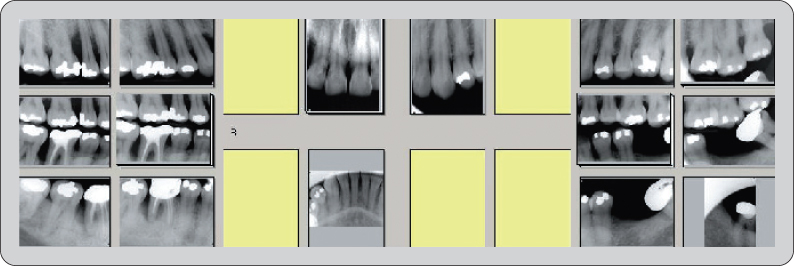
Diagnosis
According to the American Academy of Periodontology (AAP), patient LD would be diagnosed with generalized severe chronic periodontitis, which corresponds to an ADA diagnosis of Case Type IV.
Diagnosis (ADA)
Case Type I. Gingivitis
- No attachment loss
- Bleeding may or may not be present
- Pseudopockets may be present
- Only the gingival tissues have been affected by the inflammatory process
- No radiographic evidence of bone loss
- The crestal lamina dura is present
- The alveolar bone level is within 1–2 mm of the CEJ area
Case Type II. Early Periodontitis
- Bleeding on probing may be present in the active phase
- Pocket depths or attachment loss of 3–4 mm
- Localized areas of recession
- Possible class I furcation invasion areas
- Horizontal type of bone loss is most common
- Slight loss of the interdental septum
- Alveolar bone level is 3–4 mm from the CEJ area
Case Type III. Moderate Periodontitis
- Pocket depths or attachment loss of 4–6 mm
- Bleeding on probing
- Grade I and/or grade II furcation invasion areas
- Tooth mobility of class I
- Horizontal or vertical bone loss may be present
- Alveolar bone level is 4–6 mm from the CEJ area
- Radiographic furcations of grade I and/or grade II
- Crown to root ratio is 1 : 1 (loss of a third of supporting alveolar bone)
Case Type IV. Advanced Periodontitis
- Bleeding on probing
- Pocket depths or attachment loss >6 mm
- Grade II, grade III furcation invasion areas
- Mobility of class II or class III
- Horizontal and vertical bone loss
- Alveolar bone level is ≥6 mm from the CEJ area
- Radiographic furcations
- Crown to root ratio is ≥2 : 1 (loss of more than a third of the supporting alveolar bone)
Source: American Academy of Periodontology: Current Procedural Terminology for Periodontics and Insurance Reporting Manual, 7th ed.
Self-Study Questions
A. What dental history questions are important to consider for a periodontal patient?
B. What medical history questions are important to consider for a periodontal patient?
1. From a medical perspective for medical management of the patient
2. From a perspective of conditions that might affect the gingiva/periodontium
C. What constitutes a thorough periodontal examination?
D. How often and what type of radiographs should be exposed for a periodontal examination?
E. How does one come to a diagnosis for gingival and periodontal diseases?
Answers located at the end of the chapter.
References
1. Academy Reports position paper: Tobacco use and the periodontal patient. J Periodontol 1999;70:1419–1427.
2. Haber J, Wattles J, et al. Evidence of cigarette smoking as a major risk factor for Periodontitis. J Periodontol 1993;64:16–23.
3. Emrich LJ, Shlossman M, et al. Periodontal disease in non-insulin dependent diabetes mellitus. J Periodontol 1991;62:123–131.
4. Nelson RG, Shlossman M, et al. Periodontal disease and NIDDM in Pima Indians. Diabetes Care 1990;13:836–840.
5. Academy Reports informational paper: Drug associated gingival enlargement. J Periodontol 2004;75:1424–1431.
6. Rose L, Mealey B. Periodontics: Medicine, Surgery, and Implants. St. Louis, MO: Elsevier Mosby, 2004.
7. Association Report: The use of dental radiographs. Update and Recommendations. JADA 2006;137:1304–1312.
8. American Academy of Periodontology. Current procedural terminology for periodontics and insurance reporting manual. 7th ed. Chicago, IL: AAP, 1995.
9. Armitage G. Development of a classification system for periodontal diseases and conditions. Ann Periodontol 1999;4:1–6.
10. Armitage G. Periodontal diagnoses and classification of periodontal disease. Periodontology 2000 2004;34:9–21.
TAKE-HOME POINTS
A. The patient should be asked if he or she has a history of bleeding gums, loose teeth, or if there is a history of periodontal disease in the family. Bleeding of the gums spontaneously or on brushing or flossing can either indicate a systemic problem or a gingival/periodontal problem. Most patients with “bleeding gums” most likely have plaque-associated gingivitis or a form of aggressive/chronic periodontitis. If the bleeding does not resolve after initial phase therapy and home care instructions, the dentist/periodontist should refer the patient for a medical workup. Examples of diseases that may involve bleeding gums include leukemia or hemophilia. Loose teeth can either indicate an advanced stage of periodontitis or trauma from occlusion. A family history of periodontal disease should be considered in cases of localized aggressive periodontitis. Patients should also be asked if they have had prior periodontal therapy and when the last visit to a dentist took place. This history can indicate a past history of treatment for periodontal problems, or it might indicate the patient has had irregular care in the past. One must also ask patients how regularly they brush/floss and if they use any other aids. This can indicate dental neglect or good oral hygiene practices.
For this portion of the examination, it is also important to ask patients if they have a history of smoking or are currently smoking, if they have diabetes or a family history of diabetes, and if they are taking any medications. Smoking and uncontrolled diabetes are both factors that put patients at higher risk for getting periodontitis [1–4]. Because smoking and diabetes are known to affect periodontal health, it is vital that we question patients about these issues. If the patients smoke, they should be given information about how smoking affects oral health and advised to consider smoking cessation. If a patient has diabetes, he or she should be under the care of a physician who regularly monitors the condition.
B. (1) As discussed, a history of smoking and uncontrolled diabetes can reveal risk factors for periodontal disease. Any major systemic conditions or illnesses that a patient has need to be incorporated in the treatment plan. For example, complex medical issues or conditions may need to be treated in a hospital setting. If a patient is hypertensive, the AHA guidelines should be followed before any treatment. If a patient has bleeding disorders or is taking blood thinners (Coumadin, Plavix), a consultation with a physician before any surgeries should be completed. (2) Certain drugs such as nifedipine, cyclosporine, and phenytoin are known to cause gingival hyperplasia [5]. Oral contraceptives can affect the gingiva as well. If patients are taking any medications such as these, they should be informed that their prescription medication may cause changes in their gingiva.
C. A complete periodontal examination involves filling out a periodontal chart. This chart can include information on (1) probing depths (PDs), (2) bleeding on probing (BOP), (3) distance from the gingival margin to the cementoenamel junction (GM-CEJ), (4) clinical attachment loss (CAL), (5) recession, (6) furcation, (7) mobility, (8) ridge defects, and (9) plaque and calculus [6].
1. Probing Depths To obtain probing depths, the periodontal probe is placed in the sulcus in six different locations around each tooth. These locations are the mesiobuccal, straight buccal, distobuccal, distolingual, straight lingual, and mesiolingual. The probe is gently placed to the depth of the gingival sulcus, and the distance from the base of the pocket to the gingival margin is measured in millimeters using the markings on the instrument.
2. Bleeding on Probing Following periodontal probing, bleeding on probing should be noted. Some sites will experience bleeding immediately or a few moments afterward. Bleeding on probing or the lack of bleeding should be recorded on the periodontal chart.
3. Distance from Gingival Margin to Cementoenamel Junction With the use of the periodontal probe, the distance from the CEJ to the gingival margin must be measured in the same locations as the periodontal probing depths. If there is recession, this distance should be measured and recorded as a positive number. If the gingival margin is above the CEJ, which occurs in gingival health or when there is gingival hyperplasia, the probe should be used to feel the CEJ subgingivally, and the measurement should be recorded as a negative number.
4. Clinical Attachment Loss The CAL calculated using the numbers obtained after periodontal probing and after determining the distance from the gingival margin to the CEJ. The probing depth number is added to the GM-CEJ measurement. For example, if the probing depth is 2 mm and there is 2 mm of recession (GM-CEJ = +2), the CAL will be 4 mm. If the probing depth is 3 mm, and the gingival margin is 1 mm above the CEJ (GM-CEJ = −1), the CAL will be 2 mm. The values calculated for CAL are necessary for diagnosing periodontal disease.
5. Recession Recession occurs when the gingival margin is below the CEJ. The Miller classification for recession defects may be used to categorize the recession, as follows:
Miller Class 1: Recession that does not extend to the mucogingival junction with no periodontal bone loss in the interdental areas.
Miller Class 2: Recession that extends to or beyond the mucogingival junction, with no interdental bone loss.
Miller Class 3: Recession that extends to or beyond the mucogingival junction, with some periodontal attachment loss in the interdental area or malpositioning of teeth.
Miller Class 4: Recession that extends to or beyond the mucogingival junction, with severe bone and/or soft tissue loss in the interdental area and/or severe malpositioning of teeth.
6. Furcation Furcation classifications for maxillary molars, maxillary first premolars, and mandibular molars should be recorded. According to the Glickman classification for furcations, it should be recorded as grade 1, 2, 3, or 4.
Grade 1: There is incipient furcation involvement involving mostly soft tissue. Early bone loss may have occurred but is not visible radiographically.
Grade 2: There is a horizontal component to the bone loss in the furcation area resulting in an area that can be probed. Some bone does remain attached to the tooth.
Grade 3: There is no attached bone in the furcation area, resulting in a through-and-through tunnel. Soft tissue may still occlude the furcation.
Grade 4: There is a visible through-and-through tunnel that is easily probed.
7. Mobility The mobility of each tooth should be tested using the blunt ends of two instruments. Depending on the mobility, the tooth should be classified using the Miller classification system as having class 1, 2, or 3 mobility.
Miller Class 1: Tooth can be moved <1 mm in the buccolingual or mesiodistal direction.
Miller Class 2: Tooth can be moved ≤1 mm in the buccolingual or mesiodistal direction but not in the apico-coronal direction.
Miller Class 2: Tooth can be moved ≤1 mm in the buccolingual or mesiodistal direction, and movement in the apico-coronal direction is present as well.
8. Ridge Defects In edentulous areas, the remaining ridge may be classified as a Siebert class 1, 2, or 3 ridge defect if there is bone loss in the area.
Seibert Class 1: Loss of bone in the buccolingual direction with normal adequate bone in the apico-coronal direction.
Seibert Class 2: Loss of bone in the apico-coronal direction with adequate bone in the buccolingual direction.
Seibert Class 3: Loss of bone in both the buccolingual and apico-coronal direction.
9. Plaque and Calculus The presence of plaque and calculus should also be recorded on the periodontal chart as absent, mild, moderate, or abundant.
D. To obtain an accurate picture of a patient’s periodontal health, radiographs should be taken and analyzed as a part of the periodontal examination. Typically a full mouth series of radiographs should be taken every 5 years and a set of bite-wing radiographs should be taken every 2 years [7]. Bite-wing radiographs provide a way to assess the crestal bone and observe bone loss in the posterior. If there is severe bone loss that cannot be seen in a horizontal bite wing, vertical bite-wing radiographs should be taken. Periapical radiographs are useful for viewing the bone level as well, but especially for determining the crown-to-root ratio, which helps in assigning a tooth’s prognosis. Furcation involvement can also be seen in radiographs.
E. Diagnosis (American Academy of Periodontology [8]
If ≤30% of the sites are affected, the disease is localized.
If >30% of sites are affected, the disease is generalized
According to the AAP, patients are diagnosed based on their clinical attachment level.
If CAL = 0 mm, the patient is diagnosed with gingivitis.
If CAL = 1–2 mm, the patient is diagnosed with slight/mild periodontitis.
If CAL = 3–4 mm, the patient is diagnosed with moderate periodontitis.
If CAL = ≥5, the patient is diagnosed with severe periodontitis.
If the clinical attachment loss has occurred gradually for years, the disease is chronic.
If the clinical attachment loss has occurred rapidly, the disease is aggressive.
Figure 9–14 further describe the classification of periodontal diseases and conditions [9,10].
Table 1: Classification of periodontal diseases and conditions
Reprinted from Armitage, 1999, with permission from the American Academy of Periodontology.
|
I. Gingival Diseases A. Dental plaque-induced gingival diseases 1. Gingivitis associated with dental plaque only a. without other local contributing factors b. with local contributing factors 2. Gingival diseases modified by systemic factors a. associated with the endocrine system 1) puberty-associated gingivitis 2) menstrual cycle-associated gingivitis 3) pregnancy associated a) gingivitis b) pyogenic granuloma 4) diabetes mellitus-associated gingivitis b. associated with blood-dyscrasias 1) leukemia-associated gingivitis 2) other 3. Gingival diseases modified by medications a. drug-influenced gingival diseases 1) drug-influenced gingival enlargements 2) drug-influenced gingivitis a) oral contraceptive-associated gingivitis b) other 4. Gingival diseases modified by malnutrition a. ascorbic acid-deficiency gingivitis b. other B. Non-plaque-induced gingival lesions 1. Gingival lesions of specific bacterial origin a. Neisseria gonorrhea-associated lesions b. Treponema pallidum-associated lesions c. streptococcal species-associated lesions d. other 2. Gingival diseases of viral origin a. herpesvirus infections 1) primary herpetic gingivostomatitis 2) recurrent oral herpes 3) varicella-zoster infections b. other 3. Gingival diseases of fungal origin a. Candida-species infection 1) generalized gingival candidosis b. linear gingival erythema c. histoplasmosis d. other 4. Gingival lesions of genetic origin a. hereditary gingival fibromatosis b. other 5. Gingival manifestations of systemic conditions a. mucocutaneous disorders 1) lichen planus 2) pemphigoid 3) pemphigus vulgaris 4) erythema multiforme 5) lupus erythematosus 6) drug-induced 7) other b. allergic reactions 1) dental restorative materials a) mercury b) nickel c) acrylic d) other 2) reactions attributable to a) toothpastes/dentifrices b) mouthrinses/mouthwashes c) chewing gum additives d) foods and additives 3) other 6. Traumatic lesions (factitious, iatrogenic, accidental) a. chemical injury b. physical injury c. thermal injury 7. Foreign body reactions 8. Not otherwise specified (NOS) II. Chronic Periodontitis A. Localized B. Generalized |
|
III. Aggressive Periodontitis A. Localized B. Generalized IV. Periodontitis as a Manifestation of Systemic Diseases A. Associated with hematological disorders 1. Acquired neutropenia 2. Leukemias 3. Other B. Associated with genetic disorders 1. Familial and cyclic neutropenia 2. Down Syndrome 3. Leukocyte adhesion deficiency syndromes 4. Papillon-Lefèvre syndrome 5. Chediak-Higashi syndrome 6. Histiocytosis syndromes 7. Glycogen storage disease 8. Infantile genetic agranulocytosis 9. Cohen syndrome 10. Ehlers-Danlos syndrome (Types IV and VIII) 11. Hypophosphatasia 12. Other C. Not otherwise specified (NOS) V. Necrotizing Periodontal Diseases A. Necrotizing ulcerative gingivitis (NUG) B. Necrotizing ulcerative periodontitis (NUP) VI. Abscesses of the Periodontium A. Gingival abscess B. Periodontal abscess C. Pericoronal abscess VII. Periodontitis Associated With Endodontic Lesions A. Combined periodontic-endodontic lesions |
|
VIII. Developmental or Acquired Deformities and Conditions A. Localized tooth-related factors that modify or predispose to plaque-induced gingival diseases/periodontitis 1. Tooth anatomic factors 2. Dental restorations/appliances 3. Root fractures 4. Cervical root resorption and cemental tears B. Mucogingival deformities and conditions around teeth 1. Gingival/soft tissue recession a. facial or lingual surfaces b. interproximal (papillary) 2. Lack of keratinized gingiva 3. Decreased vestibular depth 4. Aberrant frenum/muscle position 5. Gingival excess a. pseudopocket b. inconsistent gingival margin c. excessive gingival display d. gingival enlargement 6. Abnormal color C. Mucogingival deformities and conditions on edentulous ridges 1. Vertical and/or horizontal ridge deficiency 2. Lack of gingiva/keratinized tissue 3. Gingival/soft tissue enlargement 4. Aberrant frenum/muscle position 5. Decreased vestibular depth 6. Abnormal color D. Occlusal trauma 1. Primary occlusal trauma 2. Secondary occlusal trauma |
Table 2: Main clinical features and characteristics of chronic periodontics (1999 Classification)
Reprinted from Armitage, 2004, with permission from the American Academy of Periodontology.
|
* Most prevalent in adults, but can occur in children and adolescents * Amount of destruction is consistent with the presence of local factors * Subgingival calculus is a frequent finding * Associated with a variable microbial pattern * Slow to moderate rate of progression, but may have periods of rapid progression * Can be associated with local predisposing factors (e.g., tooth–related or iatrogenic factors) * May be modified by and/or associated with systemic diseases (e.g., diabetes mellitus) * Can be modified by factors other than systemic disease such as cigarette smoking and emotional stress |
Table 3: Features of aggressive periodontitis that are common to both the localized and generalized forms of the disease (1999 Classification)
Reprinted from Armitage, 2004, with permission from the American Academy of Periodontology.
| Primary features |
|
| Secondary features (often present) |
|
Table 4: Specific features of localized and generalized aggressive periodontitis (1999 Classification)
Reprinted from Armitage, 2004, with permission from the American Academy of Periodontology.
| Localized aggressive periodontitis |
|
| Generalized aggressive periodontitis |
|
Table 5: Comparison of the main clinical characteristics of chronic periodontitis, localized aggressive periodontitis, and generalized aggressive periodontitis.
Reprinted from Armitage, 2004, with permission from the American Academy of Periodontology.
| Chronic periodontitis |
|
| Localized aggressive periodontitis |
|
| Generalized aggressive periodontitis |
|
Case 2
Plaque-Induced Gingivitis
CASE STORY
A 27-year-old Caucasian male presented with the chief complaint of: “My gums bleed.” The patient noticed blood in the gingiva whenever he brushed (A). He also noted that his gums bled when he flossed (A). There had never been any swelling or pain associated with his gums, and the patient had never had an episode like this before. The patient claimed to brush his teeth once daily, and he flossed two to three times a week (B).
LEARNING GOALS AND OBJECTIVES
- To be able to diagnose gingivitis
- To identify the possible etiology for the same condition and to address them
- To understand the importance of oral hygiene in preventing gingivitis
Medical History
There were no significant medical problems. The patient had no known allergies or medical illnesses. On questioning the patient stated he was taking no medications and he had no allergies.
Review of Systems
- Vital signs
- Blood pressure: 120/65 mm Hg
- Pulse rate: 72 beats/minute (regular)
- Respiration: 15 breaths/minute
Social History
The patient did not drink alcohol. He did smoke (started at age 23 and currently smoked half a pack of cigarettes daily).
Extraoral Examination
No significant findings. The patient had no masses or swelling, and the temporomandibular joint was within normal limits.
Intraoral Examination
- The soft tissues of the mouth (except gingiva) including the tongue appeared normal.
- A gingival examination revealed a mild marginal erythema, with rolled margins and swollen papillae (Figures 1–3).
- A hard tissue and soft tissue examination were completed (Figure 4) (F).
Figure 1: Preoperative presentation.
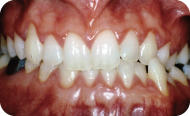
Figure 2: Preoperative maxillary anteriors.
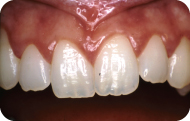
Figure 3: Preoperative mandibular anteriors.
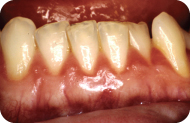
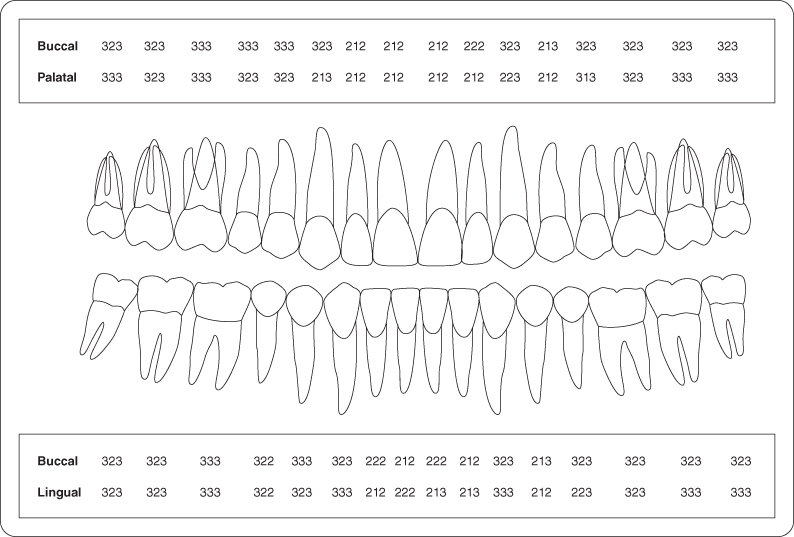
Figure 4: Probing pocket depth measurements.
Occlusion
There were no occlusal discrepancies or interferences.
Radiographic Examination
A full mouth set of radiographs was ordered (G). (See Figure 5 for the patient’s bite-wing radiographs.)
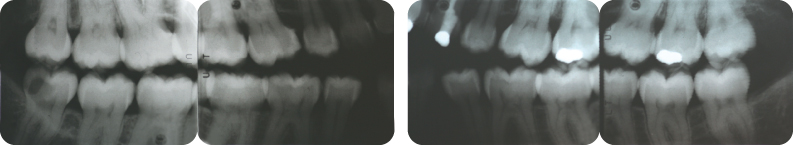
Figure 5: Bite-wing radiographs depicting the interproximal bone levels.
Diagnosis
After reviewing the history and both the clinical and radiographic examinations, a differential diagnosis was generated (H).
Treatment Plan
The treatment plan of the periodontal problems for this patient includes an initial phase of scaling with polishing and a 6-week reevaluation.
Treatment
The patient received a scaling and polishing. At the 6-week reevaluation, the clinical signs and symptoms had not improved, even though the patient claimed to be practicing excellent oral hygiene as per your instructions (I).
Discussion
Most patients who present with these symptoms (bleeding gums) have a plaque-induced gingivitis. A thorough history and periodontal examination must be completed to arrive at a diagnosis. Other characteristic features associated with plaque-induced gingivitis include the presence of plaque at the gingival margin, sulcular temperature change, increased gingival exudate, bleeding on probing. With good plaque control, the condition should resolve [1]. If there is a medical concern, it is typically identified by obtaining a thorough medical history. Conditions such as diabetes and leukemia have a profound effect on gingival health, and therefore the patient must be evaluated accordingly. In women, hormonal changes such as those that occur during the onset of puberty, pregnancy, or menstruation have a transient effect on the inflammatory status of these patients [2], which when combined with poor plaque control will lead to severe gingivitis [3,4]. After a diagnosis is reached, the treatment plan will include oral hygiene instructions, an initial phase of treatment (scaling or scaling and root planing) with a 4- to 6-week reevaluation. If the symptoms persist at this visit, the patient should be referred to a physician to rule out any systemic conditions that might cause bleeding.
Self-Study Questions
A. List the systemic/medical reasons the patient might present with bleeding gums when he flosses. What questions in a dental history might help you start to form a differential diagnosis?
B. What are the “ideal” brushing/flossing habits and techniques for a patient?
C. What effects can smoking have on the periodontium? On the oral cavity?
D. How would you perform an oral cancer examination?
E. What are the components of a periodontal examination?
F. What information should be recorded on a periodontal or soft tissue charting?
G. What kind of radiographs should be ordered for a periodontal examination?
H. What are the components that make one diagnose a case as gingivitis versus periodontitis?
I. What should a practitioner do in the case where gingival/periodontal symptoms have not resolved despite the prescribed dental care?
Answers located at the end of the chapter.
References
1. Mariotti A. Dental plaque-induced gingival diseases. Ann Periodontol 1999;4:7–17.
2. Mariotti A. Sex steroid hormones and cell dynamics in the periodontium. Crt Rev Oral Biol Med 1994;5:27–53.
3. Hugoson A. Gingivitis in pregnant women. A longitudinal clinical study. Odontologisk Revy 1971;22:25–42.
4. Loe H. Periodontal changes in pregnancy. J Periodontol 1965;36:209–216.
5. Moran JM, Addy M, et al. A comparative study of stain removal with electric tooth brushes and a manual tooth brush. J Clin Dent 1995;6:188–193.
6. Tritten CB, Armitage GC. Comparison of a sonic and a manual toothbrush for efficacy in supra gingival plaque removal and reduction of gingivitis. J Clin Periodontol 1996;23:641–648.
7. Grossi SG, Zambon JJ, et al. Assessment of risk for periodontal disease. I. Risk indicators for attachment loss. J Periodontol 1994;65:260–267.
8. Mullally B, Breen B, et al. Smoking and patterns of bone loss in early-onset periodontitis. J Periodontol 1999;70:394–401.
9. Rose LF, Mealy BL, et al. Periodontics: Medicine, Surgery, and Implants. St. Louis, MO: Mosby, 2004. Chapter 34 p871.
10. Blot WJ, McLaughlin JK, et al. Smoking and drinking in relation to oral and pharyngeal cancers. Cancer Res 1988;48:3282–3287.
11. Neville BW, Damm DD, et al. Oral and Maxillofacial Pathology. Philadelphia, PA: Lippincott, 2005. Chapter 10 p356–362.
TAKE-HOME POINTS
A
a. Bleeding disorders
Idiopathic thrombocytopenic purpura
b. Medications
Use of blood thinners
Use of oral contraceptives
c. Systemic conditions
Hormonal changes during pregnancy and puberty
Gingivitis associated with diabetes mellitus
Leukemia
Vitamins C and/or K deficiency
d. Others
Ill-fitting dental appliances or from its components (e.g., clasps)
Questions to help develop a differential diagnosis include the following:
- How often do you brush or floss?
- Do you bruise easily?
- When you wake up do you notice any blood in your mouth?
- When you cut yourself, do you tend to clot within a normal amount of time?
- What medicines are you taking currently?
- Are you pregnant (for female patients)?
- Are you a mouth breather?/Do you have difficulty breathing through your nose?
B. A patient should ideally brush twice daily and floss once daily. Evidence indicates that the use of rotary brushes is better than manual brushes for interproximal plaque removal and stain removal [5,6]. A toothbrush with soft bristles is strongly recommended. The bristles should be positioned at a 45-degree angle to the junction of the tooth and marginal gingiva, and then the brushing should be initiated using short circular gentle motions (Bass method of brushing). The same technique should be repeated for the rest of the mouth. If a patient has gingival recession, coronal sweeping motion of bristles from the gingiva to the teeth is recommended to prevent the progression of recession (modified Stillman’s technique).
C. Smoking has been identified as a risk factor for periodontitis [7]. The number of cigarettes an individual smokes per day and the number of years an individual has been smoking are two important parameters strongly associated with the degree of attachment loss [8]. It is well established that smoking affects the host immune response, causes local tissue ischemia, and also alters the bacterial profile, shifting the plaque ecology and increasing the periodontal pathogens in the host [9]. This risk factor is “behavioral” and can be modified.
Smoking causes an increased risk for oral and throat cancers [10]. Oral cancer is the sixth most common cancer in males and the twelfth most common cancer in women in the United States [11].
D. A thorough extraoral examination should be conducted. Visualization and palpation of the soft tissues of the head and neck should be completed including palpation of the muscles and lymph nodes.
The intraoral examination should consist of visualization and palpation of the tongue. The tongue represents the most common site (50%) for oral cancer and ventral and lateral surfaces (20%), in particular, have a higher predilection for cancer than the dorsal surface of the tongue (4%) [11]. The floor of the mouth is the second most common site for oral cancer, and therefore careful examination of this area of the mouth should be a part of cancer screening. Other areas that should be examined specifically for oral cancer include the soft palate, gingiva, and buccal and labial mucosa [11].
E. A periodontal examination includes looking at and describing the gingival color, contour, consistency, texture, presence or absence of exudates from sulcus, and bleeding on probing. Six probing depths (mesiobuccal, midbuccal, distobuccal, mesiolingual, midlingual, and distolingual) per tooth should be recorded. Areas of recession, mobility, and furcation involvement are also recorded and graded according to the established classifications for each of these conditions. Radiographs and study models are also important because they offer valuable information that is not obtained from the clinical oral examination.
F. The following are essential components of a periodontal chart:
- Name of the patient and the date of recording
- Missing teeth should be recorded
- Probing pocket depth: measured on six surfaces of each tooth in the mouth using a periodontal probe
- Degree of recession: measured using periodontal probe
- Mobility: measured using two flat ends of dental instruments such as dental mirror and/or periodontal probe and pushing the teeth with one instrument against the second instrument.
- Fremitus: measured by placing the inner pad of the fingers on the gingiva of the teeth in question and asking the patient to tap teeth three or four times. In traumatic occlusion, fremitus is usually felt by the examiner’s fingers, which is then recorded.
- Degree of furcation involvement: examined using Naber’s probe
- Mucogingival complex: the width of the mucogingival complex should be measured from the gingival margin to the apical-most part of the attached gingiva in every tooth, using a periodontal probe, and recorded.
G. Radiographs form an essential component of a periodontal examination. Apart from giving information about the periodontium of the tooth in question, other valuable information such as root length, root form, periapical lesions, and root proximity can be ascertained. The American Dental Association recommends a full mouth set of radiographs should be taken for a full diagnosis (typically every 5 years). A set of four bite wings should be exposed every 2 years. The diagnosis of periodontal disease can be made using periapical radiographs and bite-wing radiographs. Bite-wing radiographs are the most diagnostic for reading bone height because the head of the x-ray tube is perpendicular to the film. Vertical bite wings are recommended for areas with extensive bone loss. In general, paralleling technique is recommended over bisecting angle technique because it reduces the errors associated with film angulations.
H. Clinical attachment loss (CAL) (distance from the cementoenamel junction to the base of a periodontal pocket) and bone loss as seen on a radiograph are the gold standards used to help distinguish a patient with periodontitis versus gingivitis. Patients with gingivitis do not exhibit CAL and bone loss (radiographically), whereas if the diseases progresses to periodontitis, CAL and bone loss are characteristically observed.
I. A referral to physician should be made to rule out any systemic conditions.
Case 3
Non–Plaque-Induced Gingivitis
CASE STORY
A 41-year-old Latin American female presented with a chief complaint of: “My gums and teeth are sensitive.” She had been referred by her general dentist for periodontal treatment. She reported a 5-year history of gingival sensitivity and progressive gingival recession. She experienced lingering pain after drinking hot and cold liquids and also noted sensitivity when brushing.
LEARNING GOALS AND OBJECTIVES
- To be able to distinguish desquamative gingivitis from plaque-induced gingivitis
- To formulate a differential diagnosis for common causes of desquamative gingivitis
- To be able to arrive at a definitive diagnosis and properly manage a patient with desquamative gingivitis
Medical History
There were no significant findings found in the patient’s medical history. The patient saw her physician for an annual physical. She did not currently take any medications and she had no known drug allergies.
Review of Systems
- Vital signs
- Blood pressure: 120/70 mm Hg
- Heart rate: 78 beats/minute
- Respiration: 15 breaths/minute
Dental History
The patient had received sporadic general dental care and orthodontics in Brazil and was unsure if the city water she consumed in her childhood was fluoridated. She had received dental care more regularly since moving to the United States 13 years ago. She had her teeth cleaned twice yearly. She reported that her teeth and gums were very sensitive and that local anesthesia was often needed during her cleanings.
Social History
The patient had been born and raised in Brazil and had moved to the United States when she was 28 years old. She was married and had two daughters. She worked as a ho/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


