Modern techniques of fracture management allow easy access to the whole craniofacial skeleton, accurate fracture reduction, internal fixation with miniplating and microplating systems, and primary bone grafting where necessary to replace missing bone. The goal of primary treatment is to restore normal anatomy and therefore normal form and function to the craniofacial complex. However, patients may present with posttraumatic deformity for a variety of reasons. They may fail to present in the acute phase, or injuries may go undiagnosed if specialist expertise is not available. Other serious injuries or medical conditions may preclude or compromise immediate treatment of facial injuries, and the results of primary treatment may be unsatisfactory if the extent of the injury is underestimated or in cases of severe comminuted panfacial fractures.
Classification
There is no entirely satisfactory system for classification of posttraumatic facial deformity that incorporates the necessary mix of hard and soft tissue deficits or takes account of resultant esthetic or functional difficulties. Tessier proposed a system based on the major esthetic aspects of the disfigurement and included an orbital syndrome with enophthalmos, a craniofacial syndrome including stigmata of residual frontal and nasoethmoidal fractures, a maxillary syndrome with occlusal abnormalities, and a nasal syndrome characterized by naso-orbital dislocation. Other workers such as Manson and Gruss devised systems related to the previous location of bone fractures comprising frontobasilar fractures; Le Fort I, II, and III fractures of the maxilla; and naso-orbitoethmoid, zygomatic, nasal, mandibular, complex, and panfacial deformities.
Principles of Management
The principles underlying management of secondary posttraumatic skeletal deformity include (1)accurate assessment by history, clinical examination, and special investigations; (2) treatment planning; and (3) surgery, using a variety of techniques for management of soft and hard tissue deficits or deformities, including osteotomies and bone grafting.
Assessment
Assessment of any deformity requires a detailed history, examination, and special investigations.
History
A full history is essential for diagnosis of secondary posttraumatic deformity. Of particular importance is documentation of the patient’s complaints or concerns. A number of potentially correctable deformities may be present, and it is important to assess which of these require correction to address the concerns of the patient. A brief assessment of the psychosocial effect of the deformity may help to highlight important areas, because relatively minor physical abnormalities may give rise to significant psychological, social, or occupational problems. Understanding of the history of the original injury, whether any primary surgery was carried out, and, if so, what this involved are important to plan secondary surgery and anticipate potential difficulties or complications. For example, previous craniotomy with or without dural repair makes subsequent craniotomy more difficult due to dural adhesions, which predispose to increased risk of dural tear and subsequent cerebrospinal fluid (CSF) leak; eye injury or visual loss increases the significance of the risk to vision during operation on the contralateral orbit. The time that has elapsed between the original injury or its primary management and the presentation of secondary deformity may be significant in regard to the timing of secondary surgery. Some problems are better corrected early, whereas in others the timing is less critical (e.g., correction of enophthalmos, orbital and nasal reconstruction).
Examination
A comprehensive clinical examination of the craniofacial complex is mandatory and should include assessment of both hard and soft tissues.
Soft Tissues
Although soft tissues are not directly the subject of this chapter, they deserve mention. The presence of cutaneous scars, soft tissue deficiency, and distortions or subcutaneous fat atrophy may limit the extent of bony movement or the degree of soft tissue response to the underlying bony movement and may leave a persisting esthetic or functional deficit even if a perfect underlying skeletal position can be achieved. This should be appreciated in the planning phase so that soft tissue adjustment can be carried out at the appropriate time, usually after the skeletal reconstruction. In addition, what may seem to be a bony asymmetry may be solely a consequence of soft tissue problems, and surgical technique for correction is likely to be different from that chosen when the underlying problem is truly skeletal in nature. If complaints of orbitozygomatic deformity are being considered, soft tissues of the bony orbit are of paramount importance. Globe displacement in the vertical or anteroposterior (AP) plane needs to be accurately assessed, and the presence of characteristic stigmata of enophthalmos, such as pseudoptosis, implies a degree of displacement of the orbital tissues.
Examination of eye movement and the forced duction test allow assessment of tethering of the extraocular muscles ( Fig. 24-1 ), and traction on the insertions of the medial and lateral recti (usually with the patient under general anesthesia before surgery) gives an indication of the potential for improvement in AP eye position after enophthalmos correction. On occasion, intraorbital fibrosis may preclude anterior eye repositioning despite good orbital volume correction. The position of the lateral and medial canthi should be assessed, intercanthal distances measured, and note made of any abnormality of eyelid position such as retraction or ectropion.
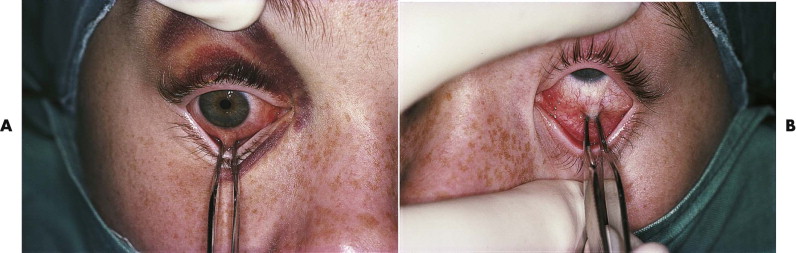
Hard Tissues
A thorough assessment of any bony distortion, deficiencies, or asymmetry must be carried out by inspection and palpation. Techniques used for assessing the bony (and cartilaginous) craniofacial skeleton are well documented in the craniofacial, rhinoplasty, and orthognathic literature. Assessment should be applied in a logical manner and must incorporate all areas of the craniofacial skeleton, including the calvaria and forehead, frontal sinus, orbits, zygomas, external and internal nose, temporomandibular joints (TMJs), mandible, upper and lower dental arches, and dental occlusion. Assessment should be made of displacements in each area examined in the three planes of space (AP, vertical, and transverse) and should include assessment of asymmetries in each of these planes.
Special Investigations
Special investigations may include plain films, dental study models, photographs, and computed tomography (CT) or magnetic resonance imaging (MRI), with three-dimensional (3-D) stereolithographic modeling or virtual planning if appropriate (see Chapter 33 ).
Plain Films
Plain films demonstrate the site and extent of the original injuries and the presence of bone plates and grafts used in primary treatment. Detailed measurements to assess malposition and asymmetries, including AP and lateral cephalometry, may be useful for delineating the underlying problem and for planning surgical correction. This particularly applies to fractures of the mandible, for which plain films can demonstrate a fibrous union or nonunion, the direction and extent of displacements, and major occlusal abnormalities such as an anterior open bite or mandibular asymmetry.
Dental Study Models
Dental study models are mandatory for assessment of posttraumatic deformity involving the tooth-bearing segments of the maxilla or the mandible. If a posttraumatic malocclusion exists, an assessment can be made of the achievable occlusion and whether any secondary dentoalveolar compensatory changes have occurred; the findings may result in a need for orthodontic or restorative correction or segmental surgery. Face bow recording and anatomical articulation may be useful, particularly in cases of bilateral condylar malunion, in which vertical face height changes are planned and mandibular autorotation is anticipated.
Computed Tomography
CT scanning in the axial and coronal planes yields very useful information, particularly in complex midface and orbitozygomatic deformities and calvarial defects. Two-dimensional imaging is useful to delineate areas of deformity or deficiency; as with plain films, accurate measurements taken from stable and unaffected portions of the craniofacial skeleton can provide an assessment of the degree of displacement or deformity. However, an additional benefit of CT scanning is its ability to generate 3-D images that allow the surgeon to visualize all aspects of the deformity at the same time; 3-D images can sometimes reveal the underlying cause of a deformity or discrepancy that is difficult to assess by two-dimensional scans ( Fig. 24-2 ).
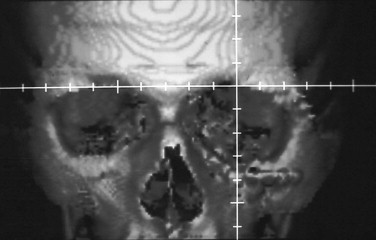
In addition, the recent introduction of stereolithographic modeling and virtual planning allows direct visualization of the defect. Direct measurement of required bony movements or augmentation is possible, and surgical simulation, if necessary, may be carried out. It also facilitates the prefabrication of alloplastic implants and production of templates as a guide for size, shape, and positioning of bone grafts, as well as prebending of plates or mesh for graft fixation. Stereolithographic and virtual modeling has been a major advance in the management of complex posttraumatic bony deformities.
Treatment Planning
After the concerns of the patient have been identified, treatment goals established, and all areas of anatomical and functional abnormality documented, detailed operative planning is required. If a portion of a craniofacial skeleton is malpositioned or deficient and is giving rise to patient concerns or complaints, it should be restored to its normal anatomical position, shape, or volume. However, correction of one deformity may result in accentuation of another that was not previously noticed by the patient. For example, malar osteotomy may make a previously mild enophthalmos more obvious, or correction of mandibular asymmetry may exaggerate an ipsilateral mild nasal deviation. In this situation, the milder, unnoticed defects may require simultaneous or subsequent correction even if they are not of direct concern to the patient initially.
Detailed planning of surgical interventions and movements depends on the information gathered from the history and examination but in particular on the results of the special investigations. When planning bony surgery, it is essential that an accurate plan of surgery and movements is established before operation. This entails a detailed assessment of the extent of movement required in the three planes of space. If onlay grafts are to be used, the site and extent of augmentation should also be established preoperatively. Intraoperative judgment of the extent of necessary bone movement or augmentation to achieve symmetry is extremely difficult because of distortion of overlying soft tissues due to the surgical access, edema, the presence of an endotracheal tube, and inaccessibility of normal reference points beneath sterile drapes. If 3-D or virtual modeling is available, prebending of plates, preforming of implants, or production of bone graft templates helps to facilitate accurate correction of the deformity and may reduce operating time.
It is important to ensure a coordinated approach to the correction of both bony and soft tissue abnormalities. This usually means correcting the bony abnormality first and then carrying out any necessary soft tissue revision subsequently.
It is essential to discuss with the patient the proposed correction and ensure a realistic expectation of outcome, including both the positive and negative effects of any proposed surgery.
Principles of Management
The principles underlying management of secondary posttraumatic skeletal deformity include (1)accurate assessment by history, clinical examination, and special investigations; (2) treatment planning; and (3) surgery, using a variety of techniques for management of soft and hard tissue deficits or deformities, including osteotomies and bone grafting.
Assessment
Assessment of any deformity requires a detailed history, examination, and special investigations.
History
A full history is essential for diagnosis of secondary posttraumatic deformity. Of particular importance is documentation of the patient’s complaints or concerns. A number of potentially correctable deformities may be present, and it is important to assess which of these require correction to address the concerns of the patient. A brief assessment of the psychosocial effect of the deformity may help to highlight important areas, because relatively minor physical abnormalities may give rise to significant psychological, social, or occupational problems. Understanding of the history of the original injury, whether any primary surgery was carried out, and, if so, what this involved are important to plan secondary surgery and anticipate potential difficulties or complications. For example, previous craniotomy with or without dural repair makes subsequent craniotomy more difficult due to dural adhesions, which predispose to increased risk of dural tear and subsequent cerebrospinal fluid (CSF) leak; eye injury or visual loss increases the significance of the risk to vision during operation on the contralateral orbit. The time that has elapsed between the original injury or its primary management and the presentation of secondary deformity may be significant in regard to the timing of secondary surgery. Some problems are better corrected early, whereas in others the timing is less critical (e.g., correction of enophthalmos, orbital and nasal reconstruction).
Examination
A comprehensive clinical examination of the craniofacial complex is mandatory and should include assessment of both hard and soft tissues.
Soft Tissues
Although soft tissues are not directly the subject of this chapter, they deserve mention. The presence of cutaneous scars, soft tissue deficiency, and distortions or subcutaneous fat atrophy may limit the extent of bony movement or the degree of soft tissue response to the underlying bony movement and may leave a persisting esthetic or functional deficit even if a perfect underlying skeletal position can be achieved. This should be appreciated in the planning phase so that soft tissue adjustment can be carried out at the appropriate time, usually after the skeletal reconstruction. In addition, what may seem to be a bony asymmetry may be solely a consequence of soft tissue problems, and surgical technique for correction is likely to be different from that chosen when the underlying problem is truly skeletal in nature. If complaints of orbitozygomatic deformity are being considered, soft tissues of the bony orbit are of paramount importance. Globe displacement in the vertical or anteroposterior (AP) plane needs to be accurately assessed, and the presence of characteristic stigmata of enophthalmos, such as pseudoptosis, implies a degree of displacement of the orbital tissues.
Examination of eye movement and the forced duction test allow assessment of tethering of the extraocular muscles ( Fig. 24-1 ), and traction on the insertions of the medial and lateral recti (usually with the patient under general anesthesia before surgery) gives an indication of the potential for improvement in AP eye position after enophthalmos correction. On occasion, intraorbital fibrosis may preclude anterior eye repositioning despite good orbital volume correction. The position of the lateral and medial canthi should be assessed, intercanthal distances measured, and note made of any abnormality of eyelid position such as retraction or ectropion.
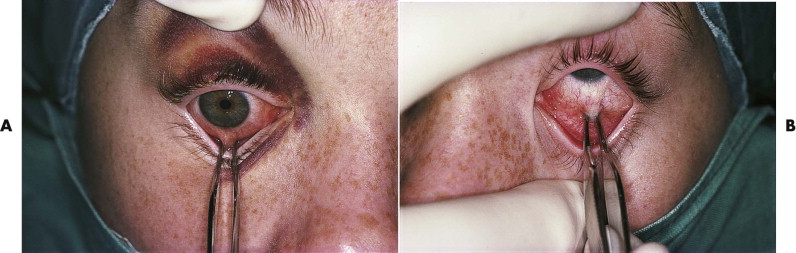
Hard Tissues
A thorough assessment of any bony distortion, deficiencies, or asymmetry must be carried out by inspection and palpation. Techniques used for assessing the bony (and cartilaginous) craniofacial skeleton are well documented in the craniofacial, rhinoplasty, and orthognathic literature. Assessment should be applied in a logical manner and must incorporate all areas of the craniofacial skeleton, including the calvaria and forehead, frontal sinus, orbits, zygomas, external and internal nose, temporomandibular joints (TMJs), mandible, upper and lower dental arches, and dental occlusion. Assessment should be made of displacements in each area examined in the three planes of space (AP, vertical, and transverse) and should include assessment of asymmetries in each of these planes.
Special Investigations
Special investigations may include plain films, dental study models, photographs, and computed tomography (CT) or magnetic resonance imaging (MRI), with three-dimensional (3-D) stereolithographic modeling or virtual planning if appropriate (see Chapter 33 ).
Plain Films
Plain films demonstrate the site and extent of the original injuries and the presence of bone plates and grafts used in primary treatment. Detailed measurements to assess malposition and asymmetries, including AP and lateral cephalometry, may be useful for delineating the underlying problem and for planning surgical correction. This particularly applies to fractures of the mandible, for which plain films can demonstrate a fibrous union or nonunion, the direction and extent of displacements, and major occlusal abnormalities such as an anterior open bite or mandibular asymmetry.
Dental Study Models
Dental study models are mandatory for assessment of posttraumatic deformity involving the tooth-bearing segments of the maxilla or the mandible. If a posttraumatic malocclusion exists, an assessment can be made of the achievable occlusion and whether any secondary dentoalveolar compensatory changes have occurred; the findings may result in a need for orthodontic or restorative correction or segmental surgery. Face bow recording and anatomical articulation may be useful, particularly in cases of bilateral condylar malunion, in which vertical face height changes are planned and mandibular autorotation is anticipated.
Computed Tomography
CT scanning in the axial and coronal planes yields very useful information, particularly in complex midface and orbitozygomatic deformities and calvarial defects. Two-dimensional imaging is useful to delineate areas of deformity or deficiency; as with plain films, accurate measurements taken from stable and unaffected portions of the craniofacial skeleton can provide an assessment of the degree of displacement or deformity. However, an additional benefit of CT scanning is its ability to generate 3-D images that allow the surgeon to visualize all aspects of the deformity at the same time; 3-D images can sometimes reveal the underlying cause of a deformity or discrepancy that is difficult to assess by two-dimensional scans ( Fig. 24-2 ).
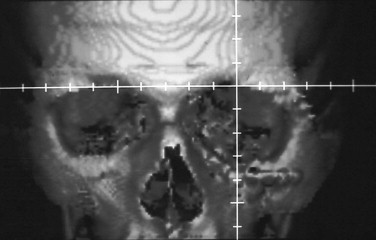
In addition, the recent introduction of stereolithographic modeling and virtual planning allows direct visualization of the defect. Direct measurement of required bony movements or augmentation is possible, and surgical simulation, if necessary, may be carried out. It also facilitates the prefabrication of alloplastic implants and production of templates as a guide for size, shape, and positioning of bone grafts, as well as prebending of plates or mesh for graft fixation. Stereolithographic and virtual modeling has been a major advance in the management of complex posttraumatic bony deformities.
Treatment Planning
After the concerns of the patient have been identified, treatment goals established, and all areas of anatomical and functional abnormality documented, detailed operative planning is required. If a portion of a craniofacial skeleton is malpositioned or deficient and is giving rise to patient concerns or complaints, it should be restored to its normal anatomical position, shape, or volume. However, correction of one deformity may result in accentuation of another that was not previously noticed by the patient. For example, malar osteotomy may make a previously mild enophthalmos more obvious, or correction of mandibular asymmetry may exaggerate an ipsilateral mild nasal deviation. In this situation, the milder, unnoticed defects may require simultaneous or subsequent correction even if they are not of direct concern to the patient initially.
Detailed planning of surgical interventions and movements depends on the information gathered from the history and examination but in particular on the results of the special investigations. When planning bony surgery, it is essential that an accurate plan of surgery and movements is established before operation. This entails a detailed assessment of the extent of movement required in the three planes of space. If onlay grafts are to be used, the site and extent of augmentation should also be established preoperatively. Intraoperative judgment of the extent of necessary bone movement or augmentation to achieve symmetry is extremely difficult because of distortion of overlying soft tissues due to the surgical access, edema, the presence of an endotracheal tube, and inaccessibility of normal reference points beneath sterile drapes. If 3-D or virtual modeling is available, prebending of plates, preforming of implants, or production of bone graft templates helps to facilitate accurate correction of the deformity and may reduce operating time.
It is important to ensure a coordinated approach to the correction of both bony and soft tissue abnormalities. This usually means correcting the bony abnormality first and then carrying out any necessary soft tissue revision subsequently.
It is essential to discuss with the patient the proposed correction and ensure a realistic expectation of outcome, including both the positive and negative effects of any proposed surgery.
Treatment Techniques
Surgical Access
Surgical access to the entire craniofacial skeleton is afforded by bicoronal flap, lower eyelid, or transconjunctival and intraoral buccal sulcus incisions. In addition, a variety of intraoral and extraoral incisions are available for access to the mandible, particularly the vertical ramus and condyle.
Coronal Flap
A coronal flap provides excellent surgical exposure of the upper craniofacial skeleton. Preauricular extension of the incision and dissection in the temporal region immediately adjacent to the deep temporal fascia allow excellent exposure down to and including the zygomatic arches. The dissection in the subgaleal plane is kept on the surface of the deep temporal fascia and may pass deep to the superficial layer where it splits above the zygomatic arch, elevating the frontal branch of the facial nerve with the flap and leaving pericranium attached to the outer table of the skull. Once the flap is raised to within a centimeter of the supraorbital margins, the pericranium can be incised along the temporal crest on each side and across the vertex of the skull posteriorly. The pericranial flap pedicled anteriorly can be raised to expose the underlying skull and is available as vascularized tissue for isolation of the cranial cavity from the nose or for subfrontal dural repair if needed. Freeing of the supraorbital nerves from their foramina can be carried out by means of small osteotomies medial and lateral to the nerves. The calvaria, forehead, supraorbital rim, orbital roof, and lateral orbital rim are exposed, and after mobilization and reflection of the temporalis muscle, access is gained to the lateral wall of the orbit and the temporal fossa.
At the end of the operation, the temporalis muscle must be anchored to the lateral orbital rim with sutures (after anterior mobilization of the muscle, if necessary) to prevent postoperative retraction and temporal hollowing ( Fig. 24-3 ). Access to the infraorbital margin and orbital floor is possible through a coronal flap but is limited, and fixation of osteotomy cuts or grafts can be difficult from this approach without a lower eyelid incision. In addition, if at the start of the operation the medial canthal ligament is intact and attached to the anterior lacrimal crest, it should never be detached during elevation of the flap, because this would require a transnasal canthopexy on closure, the results of which are often disappointing. The attachment of the medial canthal ligament can therefore limit access to the medial orbital wall. If full access to the medial orbital wall is necessary, a lower eyelid incision is required in addition to access gained via the orbital roof exposure of the bicoronal flap.
Lower Eyelid Incision
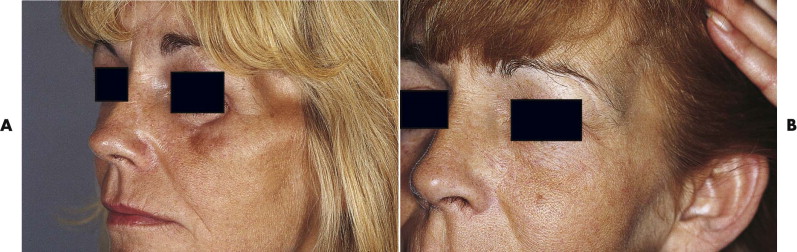
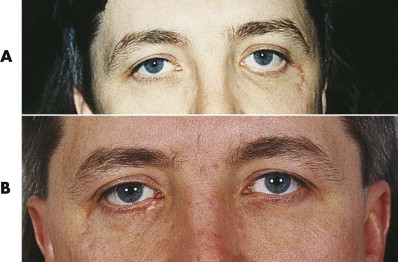
Transconjunctival, subciliary, or midtarsal incisions, with retro-orbicular preseptal dissection, all give excellent access to the infraorbital rim, orbital floor, infraorbital foramen, and anterior surface of the maxilla. We avoid the infraorbital incision for cosmetic reasons. Occasionally, postoperative lower eyelid retraction and increased scleral show may occur, but this is unusual and is amenable to correction if it fails to resolve spontaneously ( Fig. 24-4 ).
Intraoral Buccal Sulcus Incisions
A horseshoe-shaped incision in the upper buccal sulcus provides excellent access to the lower half of the maxilla and zygomatic buttress and limited access to the infraorbital rim. It should be placed at the height of the sulcus, extending from first molar to first molar, and directed out into the cheek posteriorly to avoid tearing and ensure maintenance of a good vascular pedicle to the maxilla. Repair of the paranasal muscles at the end of the procedure may reduce the risk of alar flaring postoperatively.
Extraoral Approach to the Mandible
Whereas lower buccal sulcus incisions give good intraoral access to the horizontal ramus and angle of the mandible, on rare occasions avoidance of the transoral route is necessary. In addition, intraoral access to the vertical ramus and mandibular condyle is poor, and surgical procedures on these areas of the lower jaw often require an extraoral approach. The introduction of endoscopically assisted surgery may on occasion preclude the need for extraoral access.
The submandibular approach provides good access to the horizontal ramus and angle and allows limited access to the vertical ramus of the mandible. The marginal mandibular branch of the facial nerve must be protected, either by dissection deeply on the cervical fascia or by dissection on the deep surface of platysma and formal identification of the nerve in the subplatysma fascial layer. Excessive traction may result in temporary paralysis of the lower lip due to stretching of the marginal mandibular branch of the facial nerve, but permanent weakness should be uncommon with this approach. However, nerve injury is more likely if the submandibular approach has been used previously, causing fibrosis, loss of surgical planes, and distortion of the local anatomy.
Retromandibular incision with blunt dissection between the buccal and marginal mandibular branches of the facial nerve can provide excellent access to the vertical ramus and condylar neck, and a preauricular incision with temporal extension allows access to the condylar head and TMJ. As with the bicoronal flap, dissection on the surface of the temporalis fascia avoids injury to the frontal branch of the facial nerve.
Other Incisions
Other local incisions such as the upper eyelid blepharoplasty incision, lateral eyebrow incision, Lynch incision, or use of existing scars may be indicated in selected cases in which more extensive exposure is not necessary.
Correction of Deformity
Correction of bony deformity may be carried out by the use of osteotomy, onlay grafting, or a combination of these techniques. If an individual component of the facial skeleton is of normal morphology but in an abnormal position (displacement), osteotomy is usually the technique of choice. If the bulk of the bone is in a normal position but there is abnormal morphology such as a localized contour deficit (deficiency), onlay grafting may be appropriate. If both displacement and deficiency exist, both techniques may be required. However, the choice of technique must take account of the concerns of the patient as well as the nature and degree of the deformity, the extent of surgery required, potential complications, and a realistic assessment of the likely outcome. These considerations may necessitate a departure from or modification of the basic principles outlined earlier.
Osteotomy
A variety of osteotomies are available and are well documented. These effectively re-create the original fracture pattern in the area of concern. Secondary osteotomies for trauma patients are usually carried out by conventional surgical techniques with the use of interpositional bone grafting, if required, to fill gaps created by the bony movements and to ensure primary bone healing, stability of the bony movement, and support for overlying soft tissues. Osteogenic distraction of the craniofacial skeleton is becoming more widespread and may offer another treatment option in selected cases. However, its role in the correction of posttraumatic deformity has yet to be established.
Onlay Grafting
Onlay grafting to correct bone deficiencies may be carried out using a number of materials. Autografts, homografts, heterografts, and alloplastic materials have been described, and each has its advantages and disadvantages. The ideal characteristics of onlay grafts have been outlined by a number of authors and include the following:
- •
Biocompatible
- •
No risk of disease transmission
- •
Resistant to infection
- •
Dimensionally stable
- •
Easy to shape or mold
- •
Amenable to skeletal fixation
- •
Long shelf life
- •
Cheap
Bone
Autogenous bone may be used as an interpositional graft or for onlay augmentation. It has several advantages over other materials, including its biocompatibility and lack of disease transmission. Resistance to infection is good, particularly if the bone is vascularized. Dimensional stability is variable and depends on several factors:
- •
Vascularity: vascularized is better than nonvascularized bone
- •
Embryological origin: membranous bone is better than cartilaginous bone
- •
Fixation: rigid fixation is better than nonrigid fixation
- •
Graft site: interpositional graft is better than onlay
- •
Functional loading: functional loading is better than no functional loading
A number of donor sites, including tibia, iliac crest, mandible, and calvaria, are available. We prefer iliac crest for cancellous or corticocancellous bone grafting to mandibular nonunion and calvarial bone grafting for almost all other situations, such as where osteotomy gaps or bony deficiency exist, masticatory loading is expected, or dimensional stability is important.
The use of nonvascularized grafts requires a healthy, well-vascularized graft bed. This is usually present in patients with secondary posttraumatic deformity, but occasionally the graft bed is of such poor quality that it requires vascularized bone grafts. Vascularized calvarial bone pedicled on temporalis muscle or on the superficial temporal vessels and temporoparietal fascia provides an excellent source of vascularized bone for midface and mandibular reconstruction. A disadvantage in mandibular reconstruction is the possibility of postoperative restriction in mouth opening. If a large bulk of vascularized bone is required, microvascular free flap transfer is the treatment of choice. There are a variety of potential donor sites, including iliac crest (deep circumflex iliac artery) and fibula. In selected cases, bone regeneration by distraction osteogenesis may be an option, but this has not been widely applied to treatment of posttraumatic deformity.
The disadvantages of autogenous bone grafting include prolongation of operating time and the creation of a graft donor site, with its potential associated morbidity. Variability of calvarial thickness may result in inadvertent cutting into the intracranial space during graft harvesting, but complications are rare.
Cartilage
Autogenous cartilage is an excellent material for reconstruction in some situations. It is biocompatible, maintains its viability, is dimensionally stable, and is easy to carve and shape. It can be fixed with wires or sutures. Although its resistance to infection is limited, it has proved to be a reliable material when implanted into a vascular bed, especially in the orbit and nose. It is an excellent space filler but is not rigid and therefore is unsuitable for load bearing. Potential donor sites are auricular concha and nasal septum, which yield a relatively thin sheet with limited area and volume, or costal cartilage, which has an abundant supply and can provide large volume. As with autogenous bone, prolongation of operating time and donor site morbidity, particularly if costal cartilage is used, are relative disadvantages.
Other Materials
A variety of homografts, heterografts, and alloplastic materials are available, and the reader is referred to Chapter 8 , Chapter 31 for discussion of these. In principle, we prefer to use autogenous materials in most situations to minimize the risk of disease transmission, peri-implant infection, or late extrusion. Exceptions are large calvarial defects, for which sufficient autogenous bone may not be available; temporal or forehead contour defects, for which bone graft substitutes (e.g., tricalcium phosphate) may be used; and minor malar deficiencies, for which alloplastic onlay grafts are an option.
Follow-Up
Postoperative follow-up is essential to monitor the results of treatment and to assess the need for further procedures. It is not uncommon for several reconstructive procedures to be necessary to achieve the best possible result. Cohen and Kawamoto presented a series of complex posttraumatic deformity cases in which an average of 3 to 4 procedures per patient (range, 1-15 procedures) was needed to obtain optimal correction. However, it is important to appreciate the limitations of corrective surgery and to accept that some patients cannot be restored to complete normality. There is a danger that unrealistic expectations of outcome on the part of the patient or the surgeon may result in an increasing number of surgical interventions yielding diminishing returns. If this point is reached, psychological counseling may be appropriate to help the patient accept and cope with any residual deformity.
In the remainder of this chapter, we discuss the application of the principles of secondary correction of posttraumatic deformity in the following areas: cranial vault deformity, orbitozygomatic injuries, nasoethmoidal injuries, posttraumatic malocclusion, and complex cases involving bone deficiency.
Defects and Deformity of the Skull
Cranial vault deformities are discussed under the headings of calvarial defects, frontal sinus fractures, and orbital roof fractures.
Full-Thickness Calvarial Defects
Background
Full-thickness calvarial defects may be seen in a number of situations such as after gunshot wounds, after loss of osteoplastic craniotomy flaps, or as a result of a growing skull fracture.
Growth of a linear or nonlinear skull fracture with time is a specific and unusual variant on the full-thickness calvarial defect. Ninety percent of the cases are seen in children younger than 3 years of age ( Fig. 24-5 ), although the process may also be observed in older children and adults. This delayed complication of skull fracture is rare and occurred in only 0.6% of the cases in one large series. Growing skull fractures manifest with soft swelling in the region of a previous skull fracture and clinical and radiographic evidence of increased width and length of the previous fracture. The predominant factor responsible for the increased size of the fracture seems to be a dural defect with abnormal growth of the underlying cerebral tissues, usually in the form of a leptomeningeal cyst but also from herniated cerebrum or dilated underlying ventricle with porencephalic cyst.
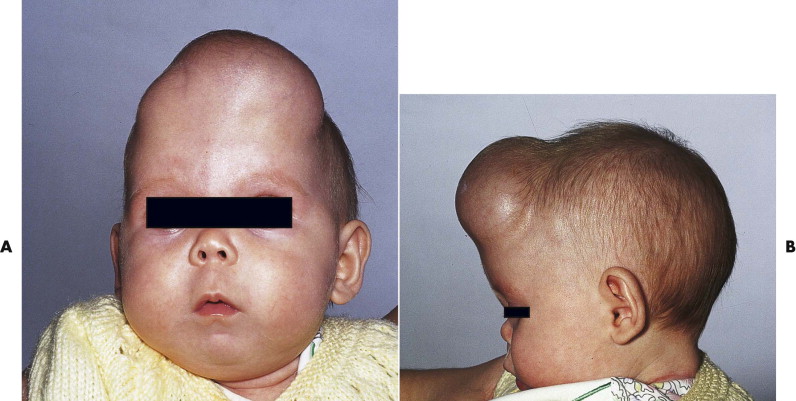
Full-thickness calvarial defects may require treatment for a number of reasons. There may be a risk of further trauma from blunt injury or a penetrating object, and a significant cosmetic defect may be apparent (see Fig. 24-5 ). In addition, infections of the scalp present a significant risk of intracranial spread due to loss of the natural barrier of the calvarial bone, with potentially serious consequences.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


