In 1968, Rowe and Killey, in the second edition of their text on facial fractures, distilled the experience of half a century in the management of facial trauma. The lessons came primarily from an unforgiving teacher—the theater of war. What evolved from this experience was a management protocol that was safe and provided resource-efficient treatment. The largely closed treatment techniques allowed a return to satisfactory function for most patients. Persistent deformity in many was accepted.
The last 4 decades of relative peace and prosperity for much of the developed world have seen major developments in the field of facial trauma, with advances in resuscitation techniques, imaging, other diagnostic tools, anesthesia, and instrumentation. Concomitantly, there has occurred an increase in the available resources to manage the trauma that occurs in peacetime. Innovative surgeons have exploited these changes in an attempt to achieve much improved results in facial form and function after trauma. A paradigm shift has occurred, with the emphasis now placed on adequate exposure with precise, usually “open”, reduction and fixation of fractured segments. The direct antecedent of this change was the experience gained in the management of craniofacial deformity through wide exposure and osteotomy with direct osteosynthesis of mobilized fragments. At the same time and in part as a result of these advances, patient expectations have also steadily risen.
We believe there has been a steady improvement in outcome; however, validation of this belief with objective data has not always been achieved. What has emerged is a treatment protocol that aims to deliver excellent results but is resource expensive. However, the techniques learned in the preceding era must not be lost, because it is evident from the experience of current conflicts that those techniques will still be required in some form by today’s and tomorrow’s surgeons.
This chapter presents a management protocol that is applicable to civilian peacetime practice, where considerable resources are available and can be brought to bear on the management of relatively small numbers of individuals at any one time.
Classification of Midface Fractures and Outcomes
Le Fort’s 1901 classic treatise describing experimentally induced midfacial fracture patterns has remained in use for more than a century and continues to have utility ( Fig. 14-1 ). However, a satisfactory classification schema should accurately describe the major clinical features present and allow the stratification of patients presenting according to severity, for the purposes of measuring outcome. Le Fort’s simple classification has important deficiencies in both respects. It fails to adequately account for fractures at multiple levels — including asymmetrical fracture patterns, separation of major fragments, comminution of vulnerable areas, concurrent anterior cranial fossa (ACF) and mandibular fractures. All of these features have a bearing on management protocols and outcome and are seen in many cases of panfacial trauma (see Fig. 14-1C ).
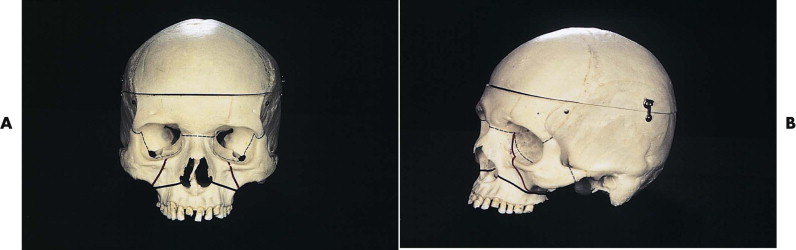
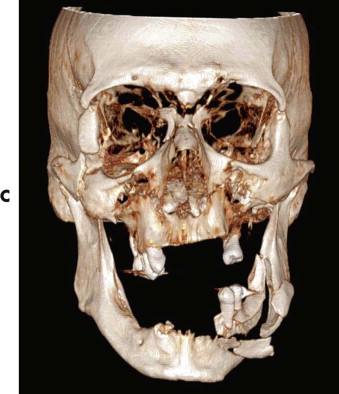
A number of workers have made useful contributions in an attempt to provide more comprehensive classification systems for the mid and upper face. Developments in the 1980s incorporated and recognized the significance of sagittal palatal fractures, naso-orbitoethmoid comminution, and involvement of the ACF. In addition, varying degrees of zygomatic complex involvement have been classified, as have frontal injuries. These descriptions have the virtue of being clinically significant, with classification of fractures of each of the major midfacial subunits facilitating communication among clinicians and planning of surgical intervention. However, if several subunits are involved, it is descriptively cumbersome. For example, a patient with a frontal sinus fracture, a naso-orbitoethmoidal fracture with traumatic telecanthus, pyramidal maxillary fracture, and displaced zygomatic complex would have a number of different classification labels applied.
Guerrissi devised a maxillofacial trauma scoring system that aims to identify patients with potentially life-threatening maxillofacial injuries, allowing appropriate triage as well as quantifying the severity of facial injuries for the purpose of stratification according to functional and esthetic impact. This scoring system has the disadvantage of being descriptive of both bony injuries and soft tissue injuries, which can lead to potential difficulties with interpretation. Furthermore, it has not, to our knowledge, been validated in a prospective study.
More recently, comprehensive scoring systems applicable to facial trauma have been described, some with validation of the proposed system for reproducibility and correlation with complexity of injury. As might be expected, the more severe the scores, the worse the degree of injury; none of these scoring systems can accurately predict outcome from a functional or esthetic point of view.
An alphanumeric scoring system has been devised by Cooter and David, and a prospective evaluation of this method has been reported. This instrument expresses the degree of facial disruption as a percentage. The authors claim that it offers a detailed analysis of fracture pattern and accurately represents the severity of bony injuries. That contention is supported by the published data. In 100 patients studied prospectively, both the maxillary fracture score and the total facial fracture score demonstrated a strong correlation with complications or adverse sequelae.
Although it is hardly surprising that greater degrees of facial disruption are associated with less favorable outcomes, the strong correlation coefficient suggests that Cooter and David’s method provides a useful objective stratification instrument. Accurate stratification of the severity of injury allows comparison of outcomes among centers even if variations exist in treatment methodology. Moreover, the pattern of adverse results observed in this study is revealing. Most of the posttreatment problems were seen in the orbital region (20% of patients) and principally comprised enophthalmos, orbital dystopia, and canthal deformities. Eight percent of the patients had occlusal abnormalities after treatment, 8% had nasal problems, and wound and implant-related problems occurred in 9%. The overall adverse sequelae rate was 36% in this group of patients who, for the most part, had sustained high-energy injuries. These data, from a major craniofacial surgical center, emphasize that residual deformity after treatment of midfacial trauma of more than moderate severity is commonplace.
A publication from two major North American centers also found worse outcomes with respect to physical problems and psychosocial well-being in patients with severe midface injuries. Patients with severe midface disruption were compared to patients with less severe facial disruption and with a second control group of patients who had sustained injuries other than to the facial region. Specifically excluded from all three groups were individuals with severe brain injury, spinal cord injury, major burns, or an extremity requiring amputation. Only 55% of those subjects with more severe Le Fort–type fractures returned to work, compared with 70% of those with less severe midface fractures and those in the age- and sex-matched group with general injuries.
There was a 23% incidence of persistent diplopia (minimum follow-up, 18 months) after Le Fort–type fractures, similar to the 20% incidence of diplopia reported after midface fracture in a sample of 363 patients from the West of Scotland. In the American study, 35% of patients reported epiphora, and the prevalence of this problem increased with severity of facial injury. Difficulty with mastication was reported in 31% (trismus, malocclusion, pain, residual nerve injury). Subjectively reported altered smell and taste occurred in 35%, and one third of patients reported persistent areas of facial numbness. This work emphasizes that the functional and psychosocial costs of midfacial injuries are high. Minimizing long-term disability requires early intervention of the highest standard and follow-up care that seeks to rectify remediable problems, together with appropriate referrals to other health care professionals when necessary.
Haug et al. also reported that more superior levels of midfacial fracture resulted in a higher incidence of adverse sequelae. Their study sought, retrospectively, to compare largely closed management of maxillary fractures with open reduction and internal fixation, using the rate of complications and of adverse sequelae as the outcome measure. No difference was observed between the groups, and the authors concluded that, “given the advantage of airway protection, enhanced nutrition, and a more rapid return to pretraumatic functioning, open reduction with rigid internal fixation may be the preferred modality of treatment.”
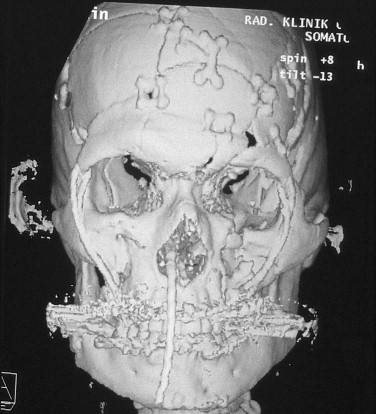
The lack of a demonstrable benefit from techniques that employ wide exposure and direct fixation in Haug’s study is disappointing and surprising. It is clear that less invasive management strategies leave substantial fragments malpositioned ( Fig. 14-2 ), and it has been assumed that more precise reduction and fixation would lead to improved outcomes. There are two possible explanations. Either the method of outcome measurement was insufficiently sensitive to detect a difference, or the extended exposure required to effect precise reduction and fixation of all fragments was associated with adverse effects, nullifying a potential benefit. These explanations are not mutually exclusive, but it is our belief that the former is the more significant factor.
What is currently lacking are objective methods by which to assess both functional and esthetic outcomes. Measurement of complication rates and the requirement for revisional surgery provides only limited information. Adverse outcomes vary from the trivial and transitory to the functionally and esthetically disabling, and thresholds for revision procedures vary widely among patients and among surgeons.
The diverse functions performed by the facial region (e.g., special senses, mastication, verbal and nonverbal communication, humidification) imply a diverse range of potential problems, making the development of good outcome measures difficult. Nevertheless, just as fracture configurations tend to follow certain patterns, so do adverse outcomes. Advances in the measurement of esthetic results in other areas of facial surgery have emerged following the advent of three-dimensional (3-D) and four-dimensional facial imaging modalities. These techniques are applicable to the assessment of esthetic and functional outcomes in trauma cases.
Much of the perceived disfigurement after facial injury is a consequence of asymmetry, which should be quantifiable with digitization of facial form and the use of software algorithms. There are obstacles to the development of such a tool. For example, all individuals have some degree of facial asymmetry, and this cannot be controlled for. It seems probable, however, that asymmetry in some facial subunits has a disproportionate effect in producing perceived disfigurement.
Refinements in technique to produce improved outcomes demand that we look critically and carefully at results and further develop objective outcome measures despite the obstacles that exist.
Assessment
The initial assessment of the patient presenting with panfacial and maxillary fractures is no different from that for any other trauma patient and should follow principles of Advanced Trauma Life Support. Compared with isolated injuries localized to the craniomaxillofacial region, the greater energy imparted in producing panfacial trauma implies a higher probability of associated injury, particular to the brain and cervical spine.
In the primary survey of a patient with panfacial trauma, the airway may well be compromised by orofacial hemorrhage and require active management, or the patient may be obtunded with a decreased Glasgow Coma Scale (GCS) score. The potential for concomitant cervical spine injury in panfacial trauma should be remembered. Problems with breathing not related to loss of the airway are uncommon but can occur as a result of foreign bodies (e.g., avulsed teeth, fractured dentures).
Hemorrhage from panfacial trauma does not usually result in cardiovascular compromise unless it is very profuse or has been on going for a considerable time. Any orofacial hemorrhage should be arrested and can usually be controlled with the application of direct or indirect pressure. It is always wise to presume that cardiovascular compromise in the patient with panfacial trauma is related to a source other than orofacial blood loss unless other causes have been ruled out. Many patients with panfacial injury have some degree of head injury that requires appropriate management.
When assessing the patient with a panfacial injury after completion of the primary survey, it is prudent for the maxillofacial surgeon to consider the following questions:
- 1
Is there an actual or potential airway problem?
- 2
Is there ongoing hemorrhage?
- 3
What is the nature and likely outcome of any accompanying head injury?
- 4
Has a cervical spine injury been diagnosed or definitively excluded?
- 5
Is there an occult life-threatening injury not detected on primary and secondary survey (i.e., is further investigation or consultation required)? A further comprehensive, top-to-toe evaluation is a prudent measure in the 48-hour period after admission and before any major intervention.
- 6
What is the precise extent, location, and nature of all injuries to the craniomaxillofacial region?
- 7
Are there non–life-threatening injuries present that require management by other specialties?
- 8
Is there any comorbidity that will affect treatment and subsequent rehabilitation?
What follows is primarily a discussion of question 6—the extent, location, and nature of injuries to the facial region—but all the questions listed require an answer in the planning of definitive management. Not only the necessity but also the urgency of liaison with additional specialties such as neurosurgery, ophthalmology, vascular surgery, interventional radiology, and orthopedics requires careful consideration based on timely, detailed, and repeated assessment. Early involvement of the required teams and good communication serve to minimize delays and optimize treatment.
The full assessment begins with a detailed history of the injury. This should be taken from the patient, if possible, or from eye witnesses, ambulance personnel, or other emergency team staff. The object of the detailed history taking is to clearly define the mechanism of injury so as to gain an appreciation of the energy involved. This indicates the probable extent of the facial injuries, and highlights probable associated injuries. A past medical history is important with regard to any intervention, and in the multiply injured patient it is often necessary to obtain this history from relatives.
A detailed craniofacial examination should take place as soon as practicable after the patient is admitted. All findings must be described in detail, and diagrams are very useful. A thorough inspection should identify lacerations, incised wounds, abrasions, and contusions. These should all be examined carefully with consideration to underlying structures that may be damaged, particularly the seventh cranial nerve. During inspection, consideration should be given to the possibility of a cerebrosponal fluid (CSF) leak. The bony structures should be palpated for contour, steps, and mobility. The eyes should be examined in detail, including fundoscopy. However, dilatation of the pupils should be carried out only after discussion with the neurosurgical service. The ears should be examined, and blood behind the tympanic membrane, tympanic perforations, and external auditory canal tears should be noted.
The history and clinical examination guide the use of further investigations. Plain radiographs taken under less than ideal circumstances are usually noncontributory. Furthermore, plain film images frequently fail to provide sufficiently detailed information regarding the nature and extent of skull base fractures, orbital wall injuries, pterygoid plate fractures, and sagittal fractures of the maxilla and condylar process of the mandible. Computed tomographic (CT) scanning is the major diagnostic investigation, with multiplanar and 3-D reconstruction and manipulation of the images on the radiology department workstations or on the surgeon’s own Picture Archiving and Communication System (PACS) being necessary to get the best detail from the information available.
Interpretation of CT scans is first directed toward determining the presence, extent, and location of skull base involvement, as well as underlying brain parenchymal injury and intracranial hemorrhage. The axial images reveal the posterior wall in frontal sinus fractures. The cribriform plate region is often more clearly seen on coronal images, and the orbital roof region is well visualized in axial, coronal, and sagittal planes. Fractures detected in the ACF are often associated with dural tears that communicate with the upper airway. Meningitis is a short- and longer-term risk, although this is not well quantified. ACF repair is frequently indicated, with varying thresholds across neurosurgical units. However, consultation is always indicated in the presence of such injuries.
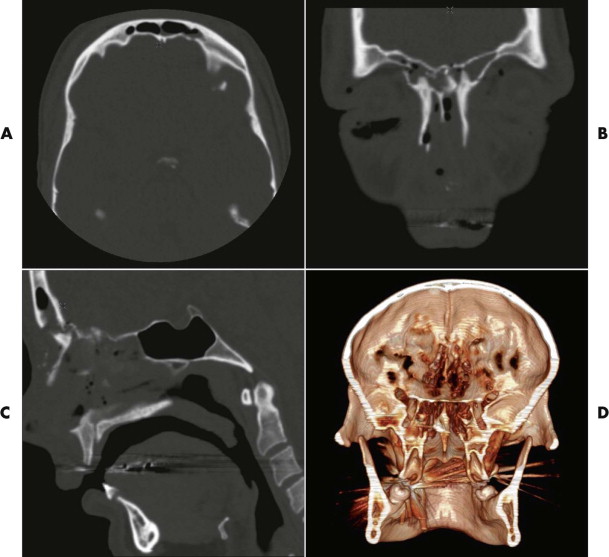
The scans of the middle cranial fossa are next scrutinized. Here, we pay particular attention to the greater wing of the sphenoid in the lateral orbit. If facial fractures extend in continuity with the middle cranial fossa, mobilization and reduction of anterior zygomatico-orbital segments risks production or exacerbation of intracranial hemorrhage, dural tears, and direct brain injury ( Fig. 14-3 ). Fractures involving the orbital apex with potential involvement of the optic foramen are occasionally seen. In the presence of a traumatic optic neuropathy accompanying such injuries, high-dose steroids are recommended. Other workers perform optic nerve decompression procedures in addition (see Chapter 10 ).
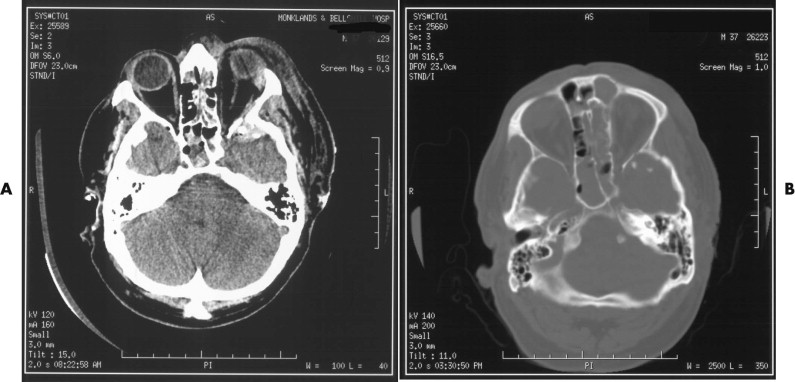
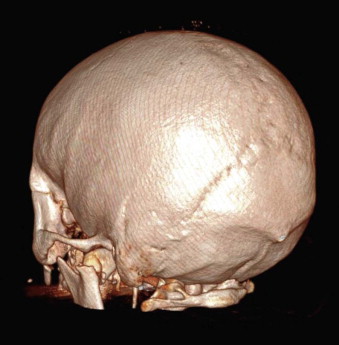
There is little information that cannot be obtained from a careful scrutiny of the axial, coronal, and sagittal images ( Fig. 14-4 ). That said, 3-D CT reconstructions have a role to play in the assessment of facial injuries, because they give a good overview of the injury and make visualization of the relationships of the various fragments easier. However, care needs to be taken in their interpretation, because interpolation of data among images can lead to underestimation of the true extent of injury. Three-dimensional imaging is particularly helpful in the visualization of fracture patterns and displacement of condylar fractures ( Fig. 14-5 ).
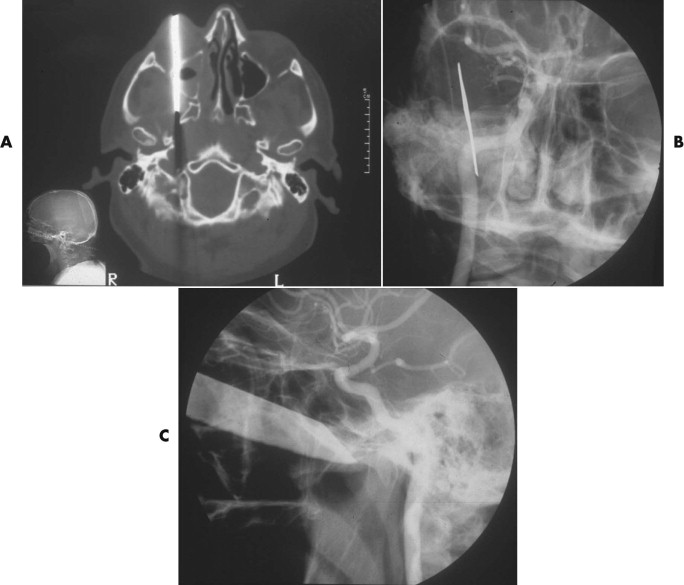
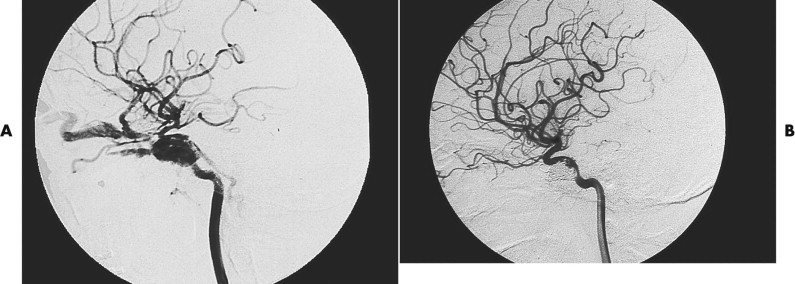
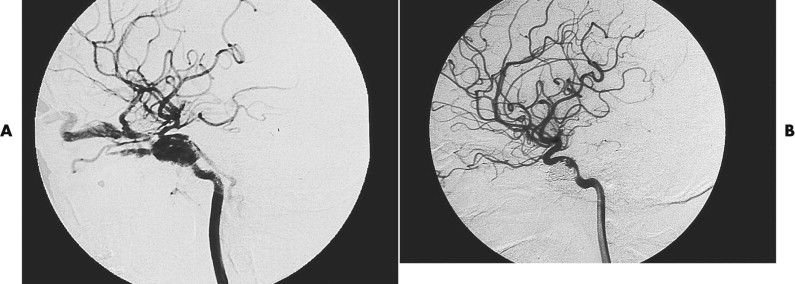
Angiography is not often necessary but can be used both diagnostically and therapeutically. Penetrating wounds can cause injury to important vessels, and angiography should be considered ( Fig. 14-6 ). Interventional techniques are used when other measures to arrest hemorrhage have not been, or are not likely to be, successful ( Fig. 14-7 ).
The use of evoked responses, particularly to assess the optic pathway, has been advocated, but at present this type of investigation is a research tool. In the future it may have a greater role in assessment of the optic pathway in the unconscious patient.
A full dental assessment is important and can be undertaken clincally in all cases. If the patient can cooperate, an orthopantomogram (OPG) is helpful. If there are dento-alveolar fractures or other factors that make the establishment of the pre-injury occlusion difficult, the use of dental models allows assessment of the occlusion and enables the construction of custom-made arch bars and an acrylic interocclusal wafer. It is often necessary to section the models, mimicking the fractures, to allow for an accurate reduction. The inspection of wear facets and the use of pre-injury photographs and orthodontic casts (if available) aid the correct reestablishment of the dental occlusion.
Once the full assessment and targeted investigations have been performed, the following key questions can be answered and, particularly for more complex injuries, a planning meeting for the surgical team convened to formulate an individualized operative strategy. These can be prolonged procedures, and planning optimizes efficiency with respect to both intraoperative decision making and allocation of resources. Treatment planning should considered.
- 1
What is the current airway, and what sort of airway is required for the planned proceedure?
- 2
What is the extent of the bony skeletal injury?
- •
Is the ACF involved?
- •
Is the frontal sinus involved? If so, is there evidence of nasofrontal outflow tract injury and, in particular, obstruction?
- •
What is the extent of naso-orbitoethmoidal injuries?
- •
What is the extent of malar-orbital injuries, particularly of the medial orbital wall?
- •
What is the extent and type of maxillary injuries?
- •
What is the extent and type of mandibular injuries (particularly condylar injuries)?
- •
Is there any bone loss (either absolute or effective)?
- •
- 3
What is the extent of any soft tissue injury?
- •
What is the extent and type of lacerations?
- •
Is there any tissue loss?
- •
Is there any injury to cranial nerves?
- •
Is there any injury to the globe or optic tract?
- •
- 4
Is there an actual or potential cervical spine injury?
- 5
Is there potential for exacerbation of a coexisting head injury?
- 6
Is there any potential vascular injury?
- 7
What other injuries exist, and how do plans for their management affect our planning?
- 8
If injuries are unilateral, can intraoperative navigational techniques be employed to assess the bony reductions?
The main aspects of the formulated management plan should be
- •
timing of the interventions
- •
airway management
- •
surgical access
- •
sequencing of repair
- •
bone graft donor sites
- •
soft tissue repair and reconstruction
The need for any particular equipment (e.g., preformed orbital plates, canthal tendon wires) must be anticipated and access to it assured.
These aspects must be considered in relation to the general state of the patient with particular reference to the current and anticipated respiratory status, cardiovascular status, nutritional state, coexisting injury, and comorbid disease.
Assessment
The initial assessment of the patient presenting with panfacial and maxillary fractures is no different from that for any other trauma patient and should follow principles of Advanced Trauma Life Support. Compared with isolated injuries localized to the craniomaxillofacial region, the greater energy imparted in producing panfacial trauma implies a higher probability of associated injury, particular to the brain and cervical spine.
In the primary survey of a patient with panfacial trauma, the airway may well be compromised by orofacial hemorrhage and require active management, or the patient may be obtunded with a decreased Glasgow Coma Scale (GCS) score. The potential for concomitant cervical spine injury in panfacial trauma should be remembered. Problems with breathing not related to loss of the airway are uncommon but can occur as a result of foreign bodies (e.g., avulsed teeth, fractured dentures).
Hemorrhage from panfacial trauma does not usually result in cardiovascular compromise unless it is very profuse or has been on going for a considerable time. Any orofacial hemorrhage should be arrested and can usually be controlled with the application of direct or indirect pressure. It is always wise to presume that cardiovascular compromise in the patient with panfacial trauma is related to a source other than orofacial blood loss unless other causes have been ruled out. Many patients with panfacial injury have some degree of head injury that requires appropriate management.
When assessing the patient with a panfacial injury after completion of the primary survey, it is prudent for the maxillofacial surgeon to consider the following questions:
- 1
Is there an actual or potential airway problem?
- 2
Is there ongoing hemorrhage?
- 3
What is the nature and likely outcome of any accompanying head injury?
- 4
Has a cervical spine injury been diagnosed or definitively excluded?
- 5
Is there an occult life-threatening injury not detected on primary and secondary survey (i.e., is further investigation or consultation required)? A further comprehensive, top-to-toe evaluation is a prudent measure in the 48-hour period after admission and before any major intervention.
- 6
What is the precise extent, location, and nature of all injuries to the craniomaxillofacial region?
- 7
Are there non–life-threatening injuries present that require management by other specialties?
- 8
Is there any comorbidity that will affect treatment and subsequent rehabilitation?
What follows is primarily a discussion of question 6—the extent, location, and nature of injuries to the facial region—but all the questions listed require an answer in the planning of definitive management. Not only the necessity but also the urgency of liaison with additional specialties such as neurosurgery, ophthalmology, vascular surgery, interventional radiology, and orthopedics requires careful consideration based on timely, detailed, and repeated assessment. Early involvement of the required teams and good communication serve to minimize delays and optimize treatment.
The full assessment begins with a detailed history of the injury. This should be taken from the patient, if possible, or from eye witnesses, ambulance personnel, or other emergency team staff. The object of the detailed history taking is to clearly define the mechanism of injury so as to gain an appreciation of the energy involved. This indicates the probable extent of the facial injuries, and highlights probable associated injuries. A past medical history is important with regard to any intervention, and in the multiply injured patient it is often necessary to obtain this history from relatives.
A detailed craniofacial examination should take place as soon as practicable after the patient is admitted. All findings must be described in detail, and diagrams are very useful. A thorough inspection should identify lacerations, incised wounds, abrasions, and contusions. These should all be examined carefully with consideration to underlying structures that may be damaged, particularly the seventh cranial nerve. During inspection, consideration should be given to the possibility of a cerebrosponal fluid (CSF) leak. The bony structures should be palpated for contour, steps, and mobility. The eyes should be examined in detail, including fundoscopy. However, dilatation of the pupils should be carried out only after discussion with the neurosurgical service. The ears should be examined, and blood behind the tympanic membrane, tympanic perforations, and external auditory canal tears should be noted.
The history and clinical examination guide the use of further investigations. Plain radiographs taken under less than ideal circumstances are usually noncontributory. Furthermore, plain film images frequently fail to provide sufficiently detailed information regarding the nature and extent of skull base fractures, orbital wall injuries, pterygoid plate fractures, and sagittal fractures of the maxilla and condylar process of the mandible. Computed tomographic (CT) scanning is the major diagnostic investigation, with multiplanar and 3-D reconstruction and manipulation of the images on the radiology department workstations or on the surgeon’s own Picture Archiving and Communication System (PACS) being necessary to get the best detail from the information available.
Interpretation of CT scans is first directed toward determining the presence, extent, and location of skull base involvement, as well as underlying brain parenchymal injury and intracranial hemorrhage. The axial images reveal the posterior wall in frontal sinus fractures. The cribriform plate region is often more clearly seen on coronal images, and the orbital roof region is well visualized in axial, coronal, and sagittal planes. Fractures detected in the ACF are often associated with dural tears that communicate with the upper airway. Meningitis is a short- and longer-term risk, although this is not well quantified. ACF repair is frequently indicated, with varying thresholds across neurosurgical units. However, consultation is always indicated in the presence of such injuries.
The scans of the middle cranial fossa are next scrutinized. Here, we pay particular attention to the greater wing of the sphenoid in the lateral orbit. If facial fractures extend in continuity with the middle cranial fossa, mobilization and reduction of anterior zygomatico-orbital segments risks production or exacerbation of intracranial hemorrhage, dural tears, and direct brain injury ( Fig. 14-3 ). Fractures involving the orbital apex with potential involvement of the optic foramen are occasionally seen. In the presence of a traumatic optic neuropathy accompanying such injuries, high-dose steroids are recommended. Other workers perform optic nerve decompression procedures in addition (see Chapter 10 ).
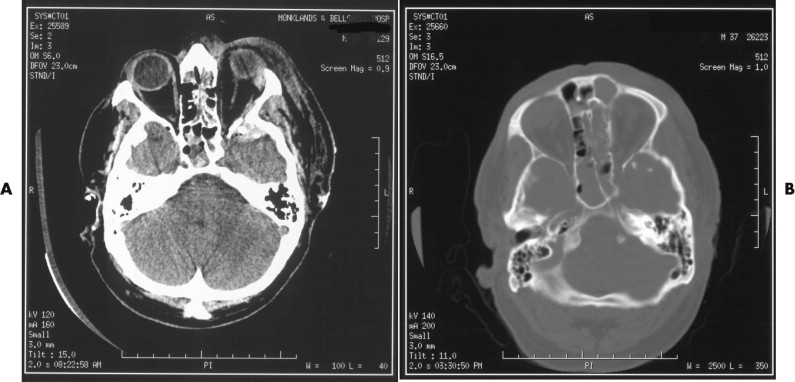
There is little information that cannot be obtained from a careful scrutiny of the axial, coronal, and sagittal images ( Fig. 14-4 ). That said, 3-D CT reconstructions have a role to play in the assessment of facial injuries, because they give a good overview of the injury and make visualization of the relationships of the various fragments easier. However, care needs to be taken in their interpretation, because interpolation of data among images can lead to underestimation of the true extent of injury. Three-dimensional imaging is particularly helpful in the visualization of fracture patterns and displacement of condylar fractures ( Fig. 14-5 ).
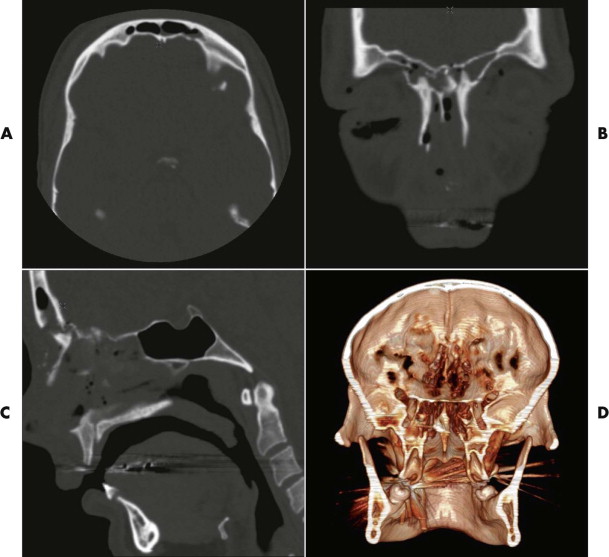
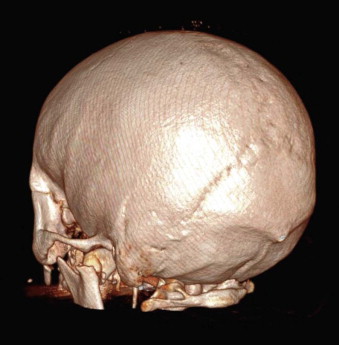
Angiography is not often necessary but can be used both diagnostically and therapeutically. Penetrating wounds can cause injury to important vessels, and angiography should be considered ( Fig. 14-6 ). Interventional techniques are used when other measures to arrest hemorrhage have not been, or are not likely to be, successful ( Fig. 14-7 ).
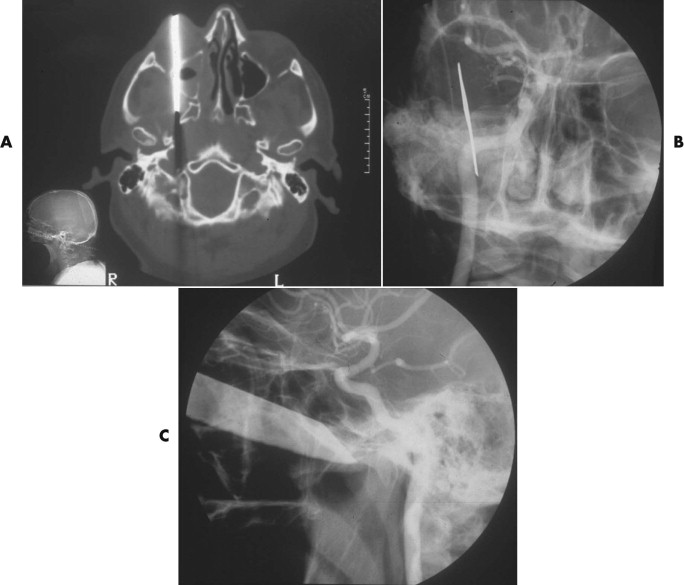
The use of evoked responses, particularly to assess the optic pathway, has been advocated, but at present this type of investigation is a research tool. In the future it may have a greater role in assessment of the optic pathway in the unconscious patient.
A full dental assessment is important and can be undertaken clincally in all cases. If the patient can cooperate, an orthopantomogram (OPG) is helpful. If there are dento-alveolar fractures or other factors that make the establishment of the pre-injury occlusion difficult, the use of dental models allows assessment of the occlusion and enables the construction of custom-made arch bars and an acrylic interocclusal wafer. It is often necessary to section the models, mimicking the fractures, to allow for an accurate reduction. The inspection of wear facets and the use of pre-injury photographs and orthodontic casts (if available) aid the correct reestablishment of the dental occlusion.
Once the full assessment and targeted investigations have been performed, the following key questions can be answered and, particularly for more complex injuries, a planning meeting for the surgical team convened to formulate an individualized operative strategy. These can be prolonged procedures, and planning optimizes efficiency with respect to both intraoperative decision making and allocation of resources. Treatment planning should considered.
- 1
What is the current airway, and what sort of airway is required for the planned proceedure?
- 2
What is the extent of the bony skeletal injury?
- •
Is the ACF involved?
- •
Is the frontal sinus involved? If so, is there evidence of nasofrontal outflow tract injury and, in particular, obstruction?
- •
What is the extent of naso-orbitoethmoidal injuries?
- •
What is the extent of malar-orbital injuries, particularly of the medial orbital wall?
- •
What is the extent and type of maxillary injuries?
- •
What is the extent and type of mandibular injuries (particularly condylar injuries)?
- •
Is there any bone loss (either absolute or effective)?
- •
- 3
What is the extent of any soft tissue injury?
- •
What is the extent and type of lacerations?
- •
Is there any tissue loss?
- •
Is there any injury to cranial nerves?
- •
Is there any injury to the globe or optic tract?
- •
- 4
Is there an actual or potential cervical spine injury?
- 5
Is there potential for exacerbation of a coexisting head injury?
- 6
Is there any potential vascular injury?
- 7
What other injuries exist, and how do plans for their management affect our planning?
- 8
If injuries are unilateral, can intraoperative navigational techniques be employed to assess the bony reductions?
The main aspects of the formulated management plan should be
- •
timing of the interventions
- •
airway management
- •
surgical access
- •
sequencing of repair
- •
bone graft donor sites
- •
soft tissue repair and reconstruction
The need for any particular equipment (e.g., preformed orbital plates, canthal tendon wires) must be anticipated and access to it assured.
These aspects must be considered in relation to the general state of the patient with particular reference to the current and anticipated respiratory status, cardiovascular status, nutritional state, coexisting injury, and comorbid disease.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


