Fig. 16.1
Clinical radiographs demonstrating (a, b) external inflammatory root resorption associated with apical pathosis, (c) external replacement resorption, (d) internal root resorption, (e) orthodontic pressure root resorption, and (f) external invasive cervical root resorption
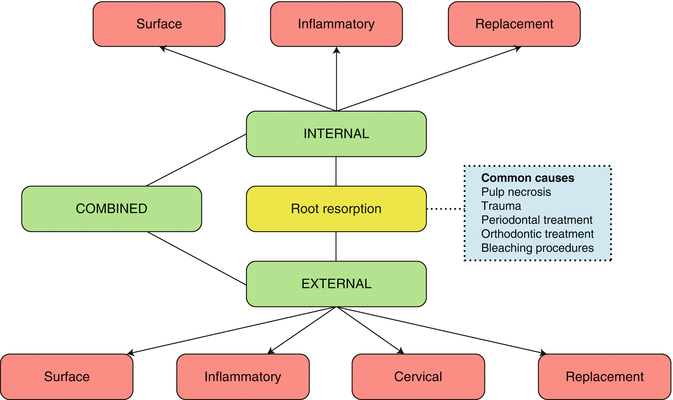
Fig. 16.2
Schematic classification of internal and external root resorption (based on classification proposed by Andreasen)
Internal root resorption is usually asymptomatic and identified by chance on routine radiographic examination. If left untreated, it can result in the progressive destruction of intra-radicular dentine and dentinal tubules along the middle and apical thirds of the canal walls as a result of clastic activities. In the initial stages, this resorption defect is the result of inflamed necrotic coronal pulp tissue with the recruitment of clastic precursor cells through vital blood vessels usually present more apically. Treatment is aimed at severing the blood supply to the resorbing tissues by means of conventional root canal treatment. Extensive resorption can eventually lead to root perforation resulting in the formation of a sinus tract. Such lesions will result in extensive tooth loss and weakened tooth structure resulting in a poorer prognosis that may or may not be amenable to treatment. Radiographically, internal root resorption appears as a ‘ballooning out’ of the root canal. The resorption lesion is an oval or round radiolucency with smooth, well-defined margins that does not change position relative to the root canal when using parallax radiographs [11–13].
Transient apical breakdown can develop as a result of certain traumatic injuries to teeth and their supporting structures. Moderate injuries to the pulp including subluxation, extrusion, lateral luxation, orthodontic treatment and occlusal trauma can result in either a spontaneous periapical radiolucency or persistent progressive expansion of the periodontal ligament space over an extended period of time. In such cases, the injured tissue undergoes a spontaneous process of repair, usually returning to normal within 1 year. Therefore, no endodontic treatment is necessary [14, 15].
External surface resorption is a transient situation in which the root surface undergoes spontaneous destruction and repair as a direct consequence of localized and limited injury to the root surface or surrounding periodontium. Since the process is self-limiting, no treatment intervention is required with resultant superficial resorptive cavities healing with new cementum within 2–3 weeks or in cases of dentine involvement partial restoration of the root surface [2, 10, 16].
External inflammatory root resorption commonly occurs following traumatic injury to the tooth or following the application of pressure due to iatrogenic orthodontic stimulus or pathophysiological stimulus of impacted teeth or tumours. The resultant damage to the periodontal ligament cells on the root surface results in a denuded root surface, whereby loss of cementum allows direct communication with the internal root canal system and external root surface. A necrotic, infected pulp, bacteria and their by-products can then provide the continued stimulus leading to extensive and progressive resorption of the root surface [9, 16].
External invasive cervical root resorption is a relatively uncommon phenomenon whose true aetiology remains obscure and can potentially result in an often destructive and aggressive condition in any permanent tooth. Potential predisposing factors cited as causes include dental trauma, orthodontic treatment, intracoronal bleaching, periodontal therapy and idiopathic origin. The resorptive process is characterized by invasion of the cervical region of the tooth by fibrovascular tissue derived from the periodontal ligament, which will eventually invade the pulp space resulting in extensive destruction of sound tooth structure (see Fig. 16.3). The pulp survives and withstands invasion until late due to inherent protection provided by predentine and odontoblasts making early diagnosis difficult unless there are chances of radiographic findings. Treatment, where indicated, is aimed at inactivation of all resorbing tissue and the reconstitution of the resorptive defect either by placement of a suitable filling material or by the use of biological systems. The radiographic appearance of external cervical root resorption depends on the severity of the lesion. Early lesions may appear as poorly defined borders of mixed radiolucency in the cervical region of the tooth.
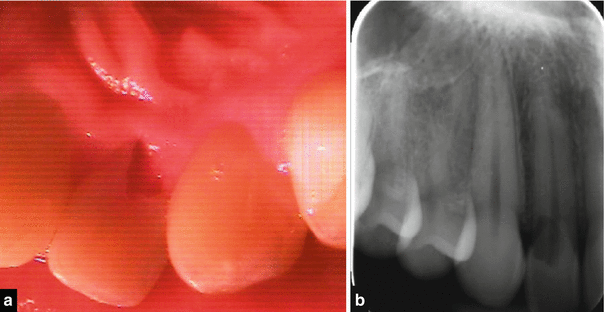
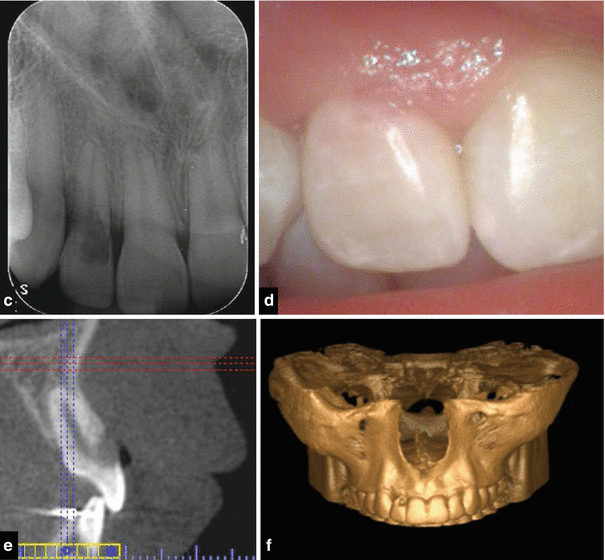


Fig. 16.3
(a) Clinical photograph and (b) radiograph showing extensive cervical root resorption affecting tooth 12. The patient reported a history of orthodontic treatment previously and possible trauma. (c–f) Clinical radiograph, photograph, CBCT scan, and maxillary reconstruction demonstrating external cervical root resorption affecting the labial aspect of tooth 12. This sixteen-year-old patient underwent fixed orthodontic appliance therapy. Following completion of orthodontic treatment and debanding, a pink spot lesion was noted with tooth 12. A parallel periapical radiograph confirmed an irregular lucency in the cervical aspect of tooth 12. CBCT scan confirmed a Heithersay class II/III lesion requiring nonsurgical root canal therapy combined with a surgical approach treating the lesion with 90 % TCA (trichloroacetic acid solution) and repair with glass ionomer cement
The root canal walls should be visible and running vertically through the radiolucent defect, indicating that the lesion lies on the external surface of the root.
The parallax technique may be helpful to detect and determine the location (palatal or labial) of the external cervical root resorption lesions [17–22].
Ankylosis and replacement resorption are commonly seen in teeth associated with luxation injuries and in particular avulsed teeth with an extended extra-oral dry time. Cementum and root dentine are resorbed by osteoclasts with subsequent replacement by alveolar bone deposited by osteoblasts. These teeth are lost usually 3–7 years after initiation of the root resorption process [23–25].
Timely intervention is essential for optimal management of dental resorption based on appropriate diagnosis from both clinical and radiographic findings. Intraoral radiographs do not provide an indication of the true three-dimensional lesion size with potential for underestimation of true extent and risks associated with management thereof. Cone beam computed tomography (CBCT) technology has been specifically designed to produce three-dimensional scans of the maxillofacial skeleton and has been successfully used to evaluate the true nature and severity of resorption lesions in the endodontic literature. Effective management and treatment strategies must be applied according to the type of resorptive process responsible and dependent on lesion size, site and nature. Non-surgical and/or surgical treatment modalities must be weighed up against alternative approaches including extraction for teeth deemed to have poor prognoses (see Figs. 16.3, 16.4 and 16.5) [15, 20, 26, 27].
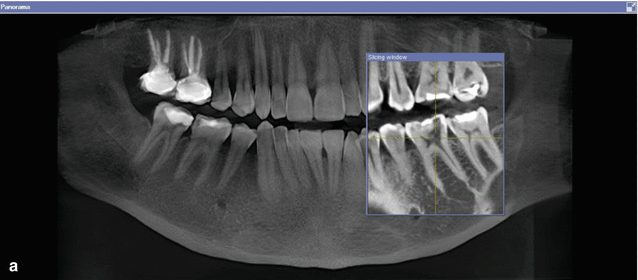
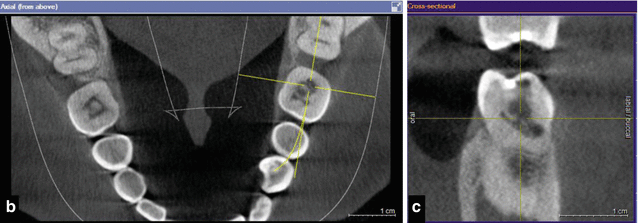
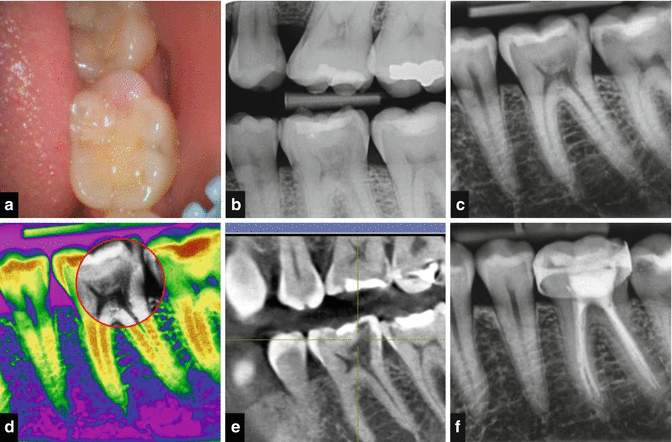


Fig. 16.4
Cone beam CT scans demonstrating external cervical root resorption in tooth 36. Note: (a) panoramic, (b) axial, and (c) cross-sectional views. Intraoral radiographs do not indicate the true dimensions of the lesion. The resorptive defect may spread within the tooth in all directions, and this may not be reflected in either the size or position of the radiolucency seen on standard radiographs. The recent advent of three-dimensional imaging has provided the endodontist with previously unavailable tools providing greater geometric accuracy in diagnosing and managing resorptive lesions. This case demonstrates how the CBCT scan allowed determination of the nature and extent of the resorptive lesion and confirmation that nonsurgical management would suffice

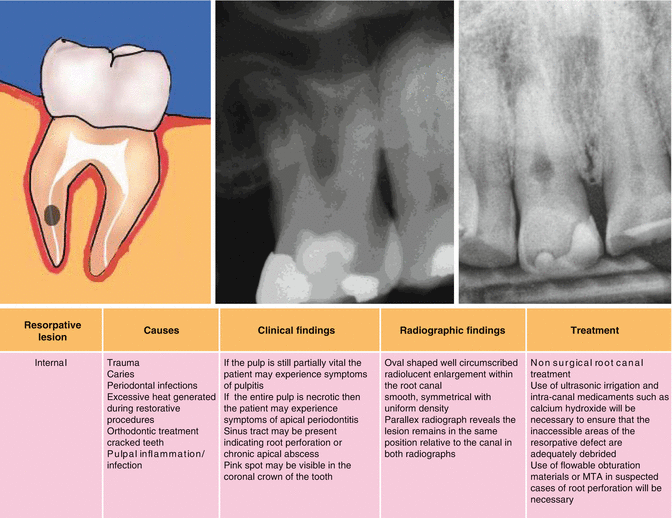
Fig. 16.5
Clinical photograph, radiographs, and cone beam CT scans showing management of external cervical root resorption in tooth 36. Note: (a) clinical intraoral photograph showing “pink spot” visible beneath the crown distally. (b–d) Conventional digital radiography showing irregular radiolucent lesion in cervical aspect of tooth. Cervical resorption lesion (red circle). (e) Cone beam CT scan of tooth 36. (f) Completed nonsurgical root canal treatment and treatment of the resorptive lesion using TCA
16.2 Internal Inflammatory Root Resorption
For internal root resorption to occur, the outermost protective odontoblast layer and predentine of the canal wall must be damaged, resulting in exposure of the underlying mineralized dentine to odontoclasts. Pulp canal necrosis and infection provide the inflammatory stimulus to sustain the process. Various aetiologies including dental trauma, caries, excessive heat generation during restorative procedures, use of cytotoxic materials in vital teeth such as calcium hydroxide pulpotomies and orthodontic tooth movements have been cited in the literature as potentially responsible for potential damage to the internal canal wall. The process has been described as either transient or progressive.

Clinically, the early stages of internal resorption are usually asymptomatic. Partial pulp necrosis may result in signs and symptoms of pulpitis. Eventually, when the entire root canal system becomes necrotic, the patient may develop apical periodontitis and symptoms thereof. Sinus tracts may be present indicating either root perforation or chronic apical abscess. A pink discolouration may be visible within the crown of the tooth although this ‘pink spot’ may be pathognomonic of external invasive cervical root resorption. The radiographic appearance is that of an oval or circular well-circumscribed symmetrical radiolucency associated with the root canal. The radiolucency has a uniform density and will remain in the same position relative to the canal when using the parallax radiographic technique (Fig. 16.6).
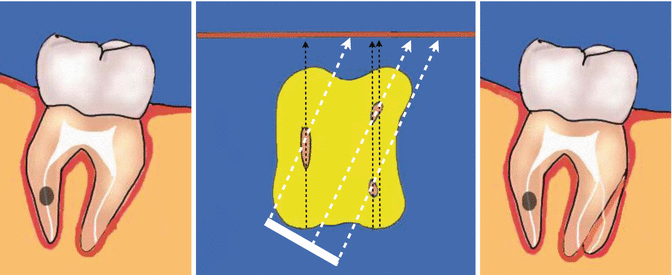

Fig. 16.6
Clinical diagrams demonstrating the parallax radiographic technique used to determine whether the resorptive lesion is internal or external. A second radiograph taken at a different angle often confirms the nature of the resorptive defect. Both external root resorption and external invasive cervical root resorption will move in the same direction as the X-ray tube shift if they are lingually/palatally positioned. They will move in the opposite direction to the tube shift if they are bucally positioned. Internal resorptive lesions on the other hand should remain in the same position relative to the canal in both radiographs
Once internal root resorption has been diagnosed, the prognosis of the tooth is dependent on whether the lesion communicates with the external surface of the root making non-surgical root canal treatment difficult due to risk of extrusion through the perforation between internal and external root surfaces. Non-surgical root canal treatment is recommended in cases where the lesion is confined within the canal, without breaching the external root surface, and where the tooth is deemed restorable.
Root canal systems have complex morphology that can harbour bacteria, by-products and remnants of necrotic pulp tissue in nonvital teeth. Teeth with internal root resorption pose a unique challenge as a result of actively resorbing balloon-sized lesions that contain inflamed bleeding pulpal and granulation tissues that are inaccessible to direct mechanical instrumentation techniques. As a result, adjunctive use of ultrasonic instrumentation and intra-canal antibacterial medicaments should be used to improve disinfection and debridement of the internal resorptive defects. Thermoplastic gutta-percha techniques are ideal when used to seal and fill the resorptive defect provided the root canal wall has not been perforated. In cases of perforation, an alternative technique using mineral trioxide aggregate may need to be utilized due to enhanced biocompatibility important at the restorative-tooth interface (Fig. 16.7).
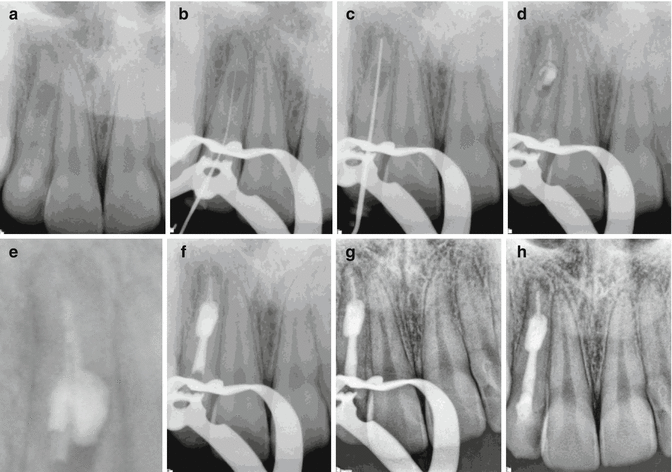

Fig. 16.7
Clinical radiographs demonstrating management of internal root resorption associated with tooth 12. Note: (a) preoperative radiograph demonstrating internal well-circumscribed radiolucency associated with the apical 1/3 of the root. (b, c) IAF and MAF files confirming working lengths. Following chemo-mechanical debridement, use of sodium hypochlorite solution, and adjunctive ultrasonic agitation, a calcium hydroxide dressing was placed for a further two weeks. At the obturation appointment, the patient remained asymptomatic. (d) Cold lateral compaction with gutta-percha and AH plus cement was used in the apical 1/3 followed by warm vertical condensation using System B. Note partial filling of the resorptive lesion (e). (f, g) The remainder of the canal was filled using Obtura. (h) A temporary coronal restoration of IRM and glass ionomer cement was placed to ensure adequate seal prior to permanent restoration with the corresponding general dental practitioner
16.3 Surface Resorption
This type of self-limiting resorption is transient and is often induced following some traumatic injuries or orthodontic treatment. It results in damage to the underlying cementum with shallow resorption of the root contour with involvement of a small amount of underlying dentine that will heal uneventfully with reparative cementum in the absence of underlying infection. Radiographic observations may reveal only subtle changes in the root morphology with no signs of any radiolucency associated with superimposed infections. The lamina dura and periodontal membrane remain intact.
16.4 Pressure Resorption
This type of resorption is commonly induced by the pressure of a crypt of an underlying unerupted/erupting tooth, by some neoplasms and more commonly due to orthodontic treatment. The resorption is often extensive and easily observable radiographically.
Tumours such as cysts, ameloblastomas, giant cell tumours and fibro-osseous lesions are frequently associated with slow growth and expansion whereby the underlying pathological process is responsible for activation of the resorptive process. Usually, the tooth will remain asymptomatic unless the process is close to the apical foramen with the possibility of disturbing the blood supply. Treatment strategies are aimed at removing the underlying cause usually by surgical means, which remove the pressure and arrest the process.
Apical root resorption during tooth movement can result in significant shortening of the roots directly due to continued pressure during orthodontic tooth movements. Teeth will remain asymptomatic, and provided the underlying forces used to tooth movement are not heavy, the pulp remains vital. No treatment is required, and provided the underlying cause is removed, this non-infective resorption will become inactive and uncomplicated repair can occur.
16.5 External Inflammatory Root Resorption
This type of external root resorption is often seen radiographically as an extensive peri-radicular radiolucency associated with an extensive inflammatory response to endodontic pathosis. It is also indicative of an infection superimposed on a traumatic injury commonly seen in both avulsion and luxation injuries. The initiating stimulus for this type of resorption is damage to the underlying protective cementum resulting in surface resorption and exposure of the adjacent dentine with direct communication with the root canal system. Superimposed infection as a result of pulpal necrosis prevents normal reparative cementum to be replaced sustaining the resorptive process due to unimpeded passage of bacteria and bacterial by-products from within the tooth. An inflammatory response persists including the activation of clastic cells resulting in both tooth and bone resorption.
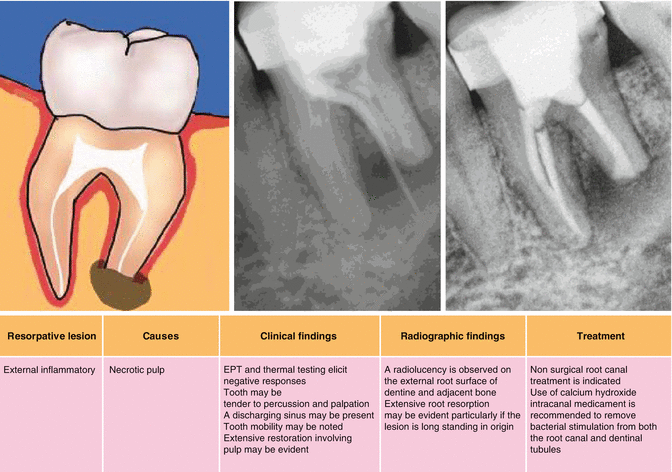

Clinical examination may reveal no abnormalities unless the infection is acute in nature demonstrated by the tooth becoming tender to touch or an overlying swelling or discharging sinus. Radiographic examination may result in bowl-like radiolucencies in both the tooth and adjacent bone that if allowed to progress will result in eventual destruction and replacement. Treatment strategies to halt progression of this type of resorption include provision of effective non-surgical root canal treatment including chemomechanical preparation to remove irritants from within the root canal system. Smear layer removal including the sequential use of 17 % EDTA, 1 % sodium hypochlorite and a final rinse with EDTA has been shown to be an effective treatment modality to ensure diffusion of intra-canal medicaments such as Ledermix paste through the dentine to the external surface of the tooth. The corticosteroid and antibacterial components of Ledermix have been shown to exert beneficial effects on clastic cells responsible for the resorptive processes that occur. Following initial use of this anticlastic agent, conventional calcium hydroxide medicament can be placed to influence hard tissue deposition on the resorbed tooth surface prior to completion of endodontic treatment.
16.6 Ankylosis and Replacement Resorption
Progressive replacement of tooth structure by alveolar bone can ultimately result in tooth loss. This type of process follows the death of viable periodontal ligament cells due to either severe compression or drying of the cells usually seen in severe traumatic injuries such as luxation, intrusion and avulsion. An interface devoid of viable periodontal ligament cells between bone and dentine results in normal remodelling processes associated with skeletal bone turnover at the expense of dentine. Ankylosis occurs with total loss of mobility with a characteristic high-pitched metallic percussion sound. At this stage, there is no loss of root dentine or cementum. Eventually progressive replacement of tooth structure by surrounding bone occurs resulting in the eventual demise of the tooth.
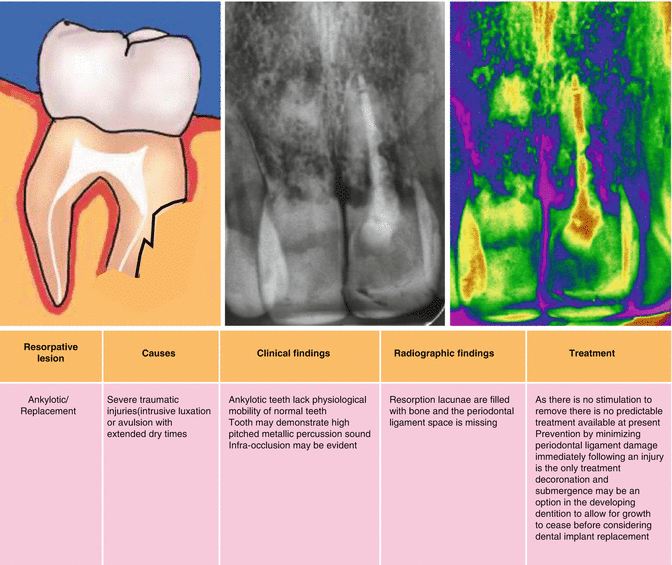

From a clinical management point of view, the replacement resorption process usually proceeds at a slow rate and in some cases taking years to reach a stage where intervention is required. In the mature dentition, alternative prosthodontic replacement options will need to be considered. In the developing dentition, ankylosis can severely disrupt arch integrity with infra-occlusion of the ankylosed tooth that becomes more obvious as skeletal growth continues. In cases of ankylosis with advanced replacement resorption, the procedure of decoronation and submergence has been recommended to allow for continued alveolar growth and uncomplicated transition to implant therapy once growth has stopped.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


