Fig. 17.1
Clinical photographs and radiographs showing pre-endodontic restorability and periodontal assessment considerations. Note: (a–c) tooth 17 presented with gross buccal caries extending subgingivally. A crown-lengthening procedure was not possible due to the extent of caries and future crown margin encroaching near the furcal region of the tooth (black arrow). The tooth was extracted. (d–e) A lower left first molar presented with gross secondary caries. The tooth was deemed unrestorable and extraction carried out. The decision to carry out complex endodontic treatment must take into account the long-term restoration and whether or not this is feasible
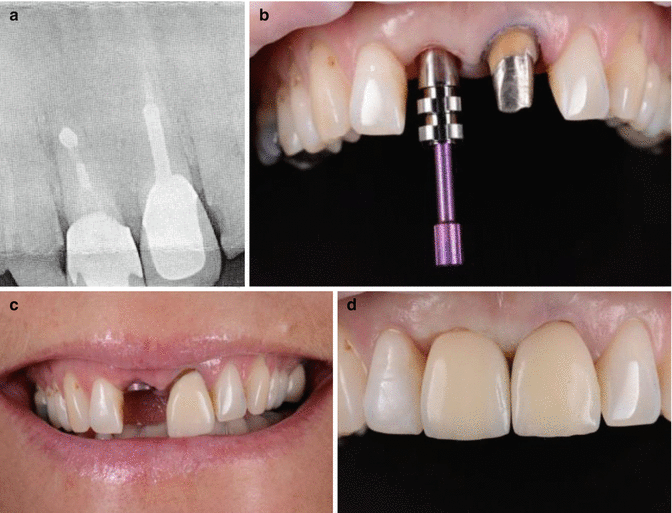
Fig. 17.2
Clinical radiographs and photographs demonstrating (a) failing endodontic treatment associated with tooth 11. The tooth had previously undergone periapical surgery and suboptimal orthograde root canal treatment. Treatment options were discussed with the patient, and a decision to replace the tooth with a single tooth implant was made. (b–d) The tooth was extracted and replaced with a single tooth implant. Tooth 21 had a cast restoration replaced to match the new implant abutment and provide optimal aesthetics
Historically it was thought that the dentine of endodontically treated teeth was significantly different when compared to their vital counterparts with factors such as moisture content and loss of collagen cross-linking being attributed to the demise of root treated teeth and their propensity to fracture [7, 8]. These findings were disputed and did not support the conclusion that endodontically treated teeth are more brittle [9, 10]. It is in fact the loss of both structural integrity associated with access preparations [11] and impairment of neurosensory feedback mechanisms following pulp tissue removal [12] that may lead to a higher occurrence of fractures associated with endodontically treated teeth. The anterior and posterior teeth are subjected to masticatory loads in normal function (laterally and vertically) with increased cuspal deflection when endodontic access cavities have been prepared [5, 13]. Taken together, these studies would suggest that the definitive restoration not only serves to provide an enhanced coronal seal and minimise future risk of micro-leakage and recontamination [14] but more importantly to prevent catastrophic fracture particularly when under heavy masticatory loading during normal function [15].
Endodontically treated teeth with intra-coronal restorations are at higher risk of cuspal fracture [16–18]. In a 20-year retrospective analysis, the cumulative survival rate (retention of both cusps) and fracture pattern of 1639 endodontically treated posterior teeth were assessed. All teeth had an MO/DO or an MOD cavity restored with amalgam without cuspal overlay. The 20-year survival rate of teeth with an MO/DO cavity was markedly higher than teeth with an MOD cavity. Maxillary bicuspids with MOD restorations showed the lowest survival rate overall (28 % fractured within 3 years, 57 % were lost after 10 years and 73 % after 20 years) [17]. The loss of tooth structure in combination with an increased cavity depth due to endodontic access results in greater cuspal deflection compared to a vital tooth [13]. Bicuspid teeth (such as maxillary premolars) can be more prone to longitudinal root fractures where the mesiodistal dimension is narrow [19].
Endodontically treated teeth as abutments have also shown to be at greater risk of fracture [12]. In a retrospective clinical investigation comparing 1273 endodontically treated teeth as abutments or crowns, it was found that the greatest failure rate was associated with pulpless teeth without a crown (24.2 %). A comparison also indicated that the failure rate of abutments when used for removable partial dentures (22.6 %) was twice that of fixed bridges (10.2 %). Overall success rate was found to be highest in endodontically treated teeth that had been restored with single crowns (94.8 %). Additional observations concluded that the presence of intra-coronal reinforcement did not appreciably increase the success rate for survival without coronal coverage. Post placement had limited influence on the success rate of fixed partial denture abutments but interestingly significantly improved the success for partial denture abutment endodontically treated teeth. ParaPost and amalgam or resin composite cores had considerably greater success compared to tapered cast post and core restorations [20].
There is strong evidence to support the notion that the clinical longevity of an endodontically treated posterior tooth is significantly improved with a coronal cuspal coverage restoration [18, 20–22]. One retrospective study, using a multivariant model and proportional hazard survival analysis, evaluated the effect of crown placement on endodontically treated teeth and their survival. Endodontically treated teeth without crowns were lost at a six times greater rate than teeth with crowns [22].
All endodontically treated teeth that require extra-coronal cuspal coverage restorations also require a coronal-radicular core restoration. The purpose of the core restoration with or without a post is to replace lost dentine and provide internal support and retention for the crown ensuring resistance against cervical tooth fracture. The presence of a circumferential ring of sound tooth structure (ferrule) at the crown-root interface is critical for the long-term success of the crowned endodontically treated tooth (Fig. 17.3). A minimum ferrule of 1.5–2 mm is required between core and crown margin to provide a bracing or casing action to protect the integrity of the root. When a crown is placed with optimal ferrule, the crown and root function as one integrated unit dissipating occlusal forces to the underlying periodontium without undue stresses resulting in crown/post dislodgement or root/post fracture. In cases where an adequate ferrule is not present then due consideration must be given to either forced orthodontic eruption or surgical crown lengthening or extraction [23, 24].
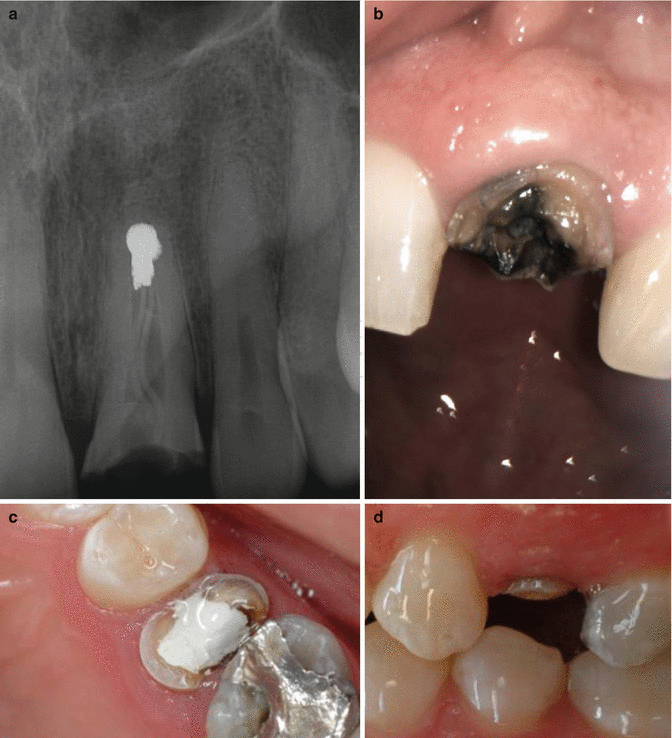

Fig. 17.3
Clinical radiographs and photographs showing limited coronal tooth structure and inadequate ferrule. Note: (a, b) tooth 21 has previously undergone root canal treatment and apicoectomy procedures. (c, d) Tooth 25 shows limited circumferential ring of sound tooth structure (ferrule). Both cases highlight the complexities involved when treatment planning cases for endodontic treatment. The cost/benefit of root canal procedures, crown lengthening, and complex post and core restorations must be outweighed against perhaps more predictable alternative prosthodontic replacement options
The anchorage provided by a well-placed core utilising the pulp chamber can be sufficient to both reinforce and replace the remaining coronal tooth structure. In posterior molar teeth, a coronal-radicular core build-up using amalgam utilising the pulp chamber and 2 mm into each canal space has proved to be successful in clinical studies [25]. Additional retention can also be provided by the use of intra-dentinal pins [26], amalgapins [27] and dentinal slots and grooves [28]. With the advent of modern adhesive techniques, these types of retention methods have been superseded due to concerns of further weakening the tooth as a direct result of further coronal tooth structure loss [29].
Anterior teeth with minimal loss of tooth structure can be restored conservatively with a bonded restoration in the access opening without the use of a post [18]. The use of modern direct composites and resin bonding materials is at the forefront of contemporary minimally invasive aesthetic dentistry and will provide satisfactory aesthetic results restoring function and aesthetics, whilst preserving healthy tooth tissue [30]. Where there has been substantial tooth structure loss or in addition where the tooth is aesthetically displeasing, then crowning may be indicated. The primary disadvantage of using indirect conventional metal-ceramic crowns is the significant buccal surface tooth reduction (approximately 1.5–2 mm) that is required to accommodate both metal and ceramic core [31]. The use of all-ceramic crowns (e.g. Procera, Nobel Biocare, Zurich, Switzerland. Empress, Ivoclar Vivadent, Amherst, NY, USA. In-ceram, H.Rauter GmbH & Co. KG, Bad Säckingen, Germany) as an alternative to metal-ceramic restorations has been driven by both superior aesthetics and increased strength in thin sections resulting in a viable option for anterior and posterior teeth [32].
In posterior teeth, as discussed earlier, the longevity of the root canal therapy is dependent on the quality of the coronal restoration in terms of both tooth survival and potential fracture and prevention of coronal leakage and possible reinfection. Root canal treatment outcomes evaluated in a large-scale epidemiological study of more than one million patients showed that 85 % of teeth that had been extracted had no full coronal restoration. They also found a sixfold increase in failure rate in posterior teeth with no crowns compared with posterior teeth with crown restorations [33]. Prosthetic reconstruction of posterior endodontically treated teeth without adequate cuspal coverage using conventional amalgam has been shown to be not suitable [17]. The use of amalgam crown restorations, with a minimal 2 mm thickness of cuspal coverage, has shown a cumulative survival rate of 88 % after 100 months and a less expensive alternative to cast restorations [34, 35]. Their intended use may be particularly beneficial when the endodontic prognosis is questionable and longer-term follow up is envisaged providing a relatively inexpensive and predictable interim restoration.
The use of tooth coloured direct composite restorations has also been evaluated for use in the restoration of root-filled teeth. Fibre posts with direct composite restorations in root-filled premolars with limited tooth structure loss have been shown to exhibit equivalent survival rates compared with premolars restored with crowns after 3 years [36]. The long-term survival of direct composite restorations, particularly in load-bearing areas, is questionable due to natural wear and tear resulting in either fracture or marginal discrepancies that can lead to reinfection and failure. In a longitudinal outcome study based on a systematic review, root-filled teeth restored with crowns had a 10-year survival rate of 81 %. Teeth restored with direct restorations (such as amalgam or composite) had a survival rate of 63 % [37]. The use of composite restorations in posterior teeth may be best served as a core material in preparation for future cast cuspal coverage restoration.
Cast gold partial restorations (onlay, three-quarter and seven-eighths) and full coverage crowns allow for the most conservative tooth preparation ensuring optimal preservation of residual tooth structure. They are useful in posterior teeth where aesthetic demands are not of paramount importance or where the patient exhibits parafunctional habits (bruxism) or there is limited inter-occlusal space. The reduction required for gold restorations can be as little as 0.7 mm in non-load-bearing areas and up to 1.5 mm in load-bearing areas [6]. Both metal-ceramic restorations and all-ceramic crowns have also been shown to be effective and again useful when aesthetics is of particular importance.
When insufficient coronal tooth structure exists to retain a core, then a post is a universally accepted treatment modality. Previously considered to provide further reinforcement, it is now widely recognised to help retain the core build-up albeit there is a greater risk of significantly weakening the root as result of post preparation [15, 38, 39]. The decision to place a post must be weighed up against the inherent risks associated with post preparation including procedural accidents such as perforations in the apical or mid-root of the tooth, increased risk of root fracture and treatment failure [40] (Fig. 17.4).
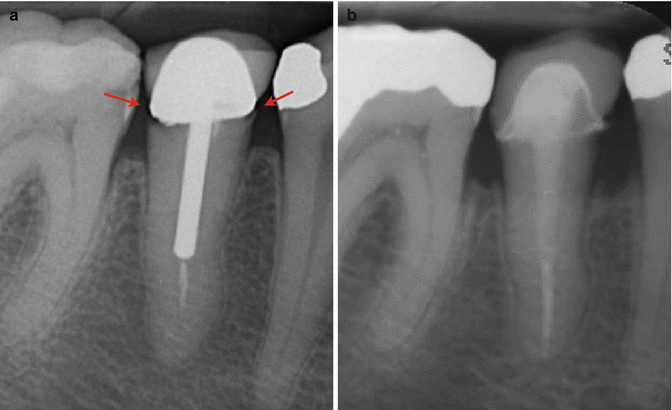

Fig. 17.4
Clinical radiographs demonstrating endodontic re-treatment, crown lengthening, and new post and core crown replacement for tooth 45. Note (a) preoperative radiograph showing parallel post-core restoration with defective margins (red arrows) and coronal microleakage. Clinically minimal ferrule height was confirmed following removal of crown and post. After initial removal of gutta-percha, chemo-mechanical preparation, and patency confirmation, the tooth was dressed with calcium hydroxide. The patient was referred to a periodontist to confirm that crown lengthening was feasible. Following completion of endodontic therapy, the patient returned to the periodontist for crown lengthening, followed by an interim 3-month healing period. (b) The patient was then seen for final fiber post, core, and permanent crown placement. Complex re-treatment occasionally requires a multidisciplinary approach. Provided all stages of treatment are executed correctly, then the long-term prognosis should be good. Careful planning with the patient is crucial from the outset including discussion of alternative prosthodontic replacement options. In this case the patient could have opted for a single-unit implant which would have been of similar expense
Posts can be categorised into metallic posts, prefabricated posts, zirconium and ceramic posts and non-metallic posts (fibre). Metallic and prefabricated post systems are conventionally more rigid in design compared to non-rigid fibre post systems. Metallic custom-cast post and core systems are constructed by making an impression of the post space (direct or indirectly) and fabrication of the post from precious or non-previous casting alloys in the laboratory. A systematic review demonstrated no superiority between cast posts over direct post and core restorations [41]. The disadvantage of a custom-cast post and core system includes increased cost and time involved for the patient. The main advantage of the custom-cast post designed to fit the tooth is the greater potential for tooth conservation. This is of particular importance in teeth with small thin tapered roots such as premolars, maxillary lateral incisors and mandibular molars which could be significantly weakened by further instrumentation necessary to fit a prefabricated post [42].
Prefabricated posts are typically made from stainless steel, nickel-titanium alloy or titanium and come in a variety of designs. They can be divided into tapered or parallel and active or passive. A tapered post is less retentive in comparison to a parallel post but helps to preserve dentine and reduces the amount of dentine that needs to be removed to accommodate the post [43]. Conversely the parallel post provides the greatest retention (particularly if the surface is grooved or roughened) but requires tooth structure to be sacrificed in order to accommodate the post. There has been concern with regard to the wedging effect when using tapered posts that may predispose to root fracture and loss of post retention. Passive posts are retained primarily by the frictional retention of the luting cement and induce less stress into the root compared to active posts, although are less retentive. Active posts imply that the threads of the post engage or screw into the walls of the canal.
Zirconium and ceramic post systems were developed in view of the aesthetic problems associated with metal posts and the possibility of visibility through translucent all-ceramic restorations. Disadvantages of these posts include greater rigidity and brittleness, greater tooth removal required as a consequence of thicker post diameters necessary to compensate for weakness and significantly more root fractures in vitro compared to fibre posts [44, 45]. In addition, retrieval of zirconium and ceramic posts is very difficult if endodontic retreatment is indicated requiring excessive removal of dentine and post removal by grinding the ceramic or zirconium post, which is both risky and tedious. Their use should be avoided if at all possible.
Non-rigid non-metallic prefabricated post systems consist of carbon fibre, glass fibre, quartz fibre and silicon fibre posts. The posts were manufactured for use in conjunction with highly aesthetic restorations whereby the post was bonded utilising resin luting cements incorporating composite cores. The first reinforced fibre posts were made with longitudinally arranged black carbon fibres embedded in an epoxy resin matrix that fell out of favour due to their dark colour. These were rapidly replaced by more aesthetically pleasing tooth coloured/white and translucent glass and quartz fibres. The main advantage of using a fibre post is that the mode of failure is generally more retrievable compared to other post systems. Although the load to failure is greater in metallic posts, they result in significantly greater root fractures [45–47].
Post retention is dependent on several factors including post configuration, length, diameter, surface preparation and cementation. Post diameter is the least important factor and should be designed to conform to the pre-existing canal diameter without sacrificing further tooth structure, which further weakens the tooth (Fig. 17.5). Regarding post configuration, the active threaded post is the most retentive, followed by the passive parallel post. The passive tapered post is the least retentive [43, 48]. One must bear in mind that active threaded posts can induce stresses in the root dentine that may lead to crack initiation and predisposition to root fracture at a later time.
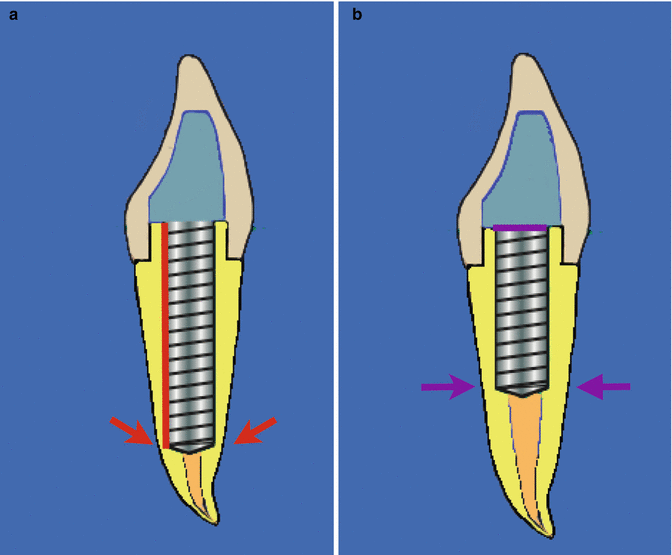

Fig. 17.5
Diagrammatic representation of (a) post length and (b) post diameter and their effect on post retention. Increasing the post length increases the retention of the post and the length should be at least equal to the length of the clinical crown. Post length must be weighed up against anatomical and morphological factors which may increase the risk of perforation (red arrows). Post diameter is the least important factor when designing an ideal post and should conform to the preexisting canal diameter without sacrificing further root structure and predisposing to fracture or perforation (purple arrows)
Increasing the length of the post increases the retention. The length of the post should at least equal the length of the clinical crown [21]. Short posts lead to greater stress in the coronal aspect of the canal increasing susceptibility to dislodgement or root fracture (Figs. 17.5 and 17.6). One study reported that two-thirds of the posts associated with vertically fractured endodontically treated teeth were extremely short, terminating in the cervical third of the root [49]. Ideal post length must be weighed up against anatomical and morphological factors such as apical root structure thickness and furcal concavities which may increase the risk of perforation and weakening of the tooth together with the need to maintain an apical seal (dictated by remaining gutta-percha) [50]. To avoid reinfection of the periapical region following post preparation, at least 4–5 mm of apical gutta-percha should be retained [50, 51]. Once the post has been prepared, the post should be cemented as soon as practically possible to reduce the potential for apical leakage and reinfection [52, 53].
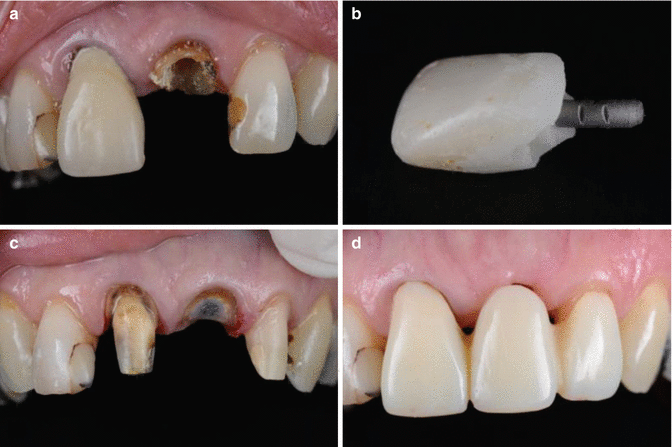

Fig. 17.6
Clinical photographs demonstrating a failed post and core restoration associated with tooth 21. Note: (a) limited coronal tooth structure with adequate ferrule and (b) short post length resulted in prosthodontic failure. (c–d) The 21 was subsequently de-coronated and a temporary fixed-fixed tooth-supported FDP fabricated following its extraction
The long-term success of post retained restorations is also dependent on the resistance form. Resistance refers to the ability of the post and tooth to withstand lateral and rotational forces and is provided by three factors: anti-rotation features, the presence of a ferrule [23, 24] and remaining tooth structure. Anti-rotation features such as slots or pins can be incorporated in the absence of significant vertical tooth height [18, 54]. A minimum crown height of at least 1.5 mm apical to the margin of the core is needed to provide significant resistance to fatigue failure of the cement seal [55].
The failure of endodontically treated teeth is usually not a consequence of endodontic treatment, but inadequate restorative therapy or periodontal reasons. Prior to the initiation of endodontic treatment, the restorability, occlusal function, periodontal health, biological width and crown-root ratio need to be assessed. Direct adhesive restorations, indirect bonded restorations and traditional full crowns are three therapeutic options for single posterior endodontically treated teeth. Posts may be utilised for retention of core material and to replace missing tooth structure. The amount of remaining sound tooth structure is the most significant factor in determining the most appropriate technique, material and type of restoration employed to restore the functional needs of the patient [56, 57].
17.2 Core Materials
Amalgam
The use of amalgam as a material for core restorations of endodontically treated teeth has been advocated and practised since its earliest use as a conventional restorative material. In addition to its well-documented physical properties, its handling has allowed clinicians to utilise amalgam as a direct core material in situations where bonding would either be difficult or inappropriate for reasons of moisture control. Its inherent compressive strength has made it the material of choice for posterior load-bearing situations; whilst it had been used in anterior teeth prior to the advent of reliable resin bonding techniques, its colour (inherent as well as imparted) has obvious drawbacks in the aesthetic zone. Also worth noting is its low strength in thin sections and under tensile forces; clinicians should therefore ensure that adequate resistance form is present when placing amalgam in smaller sections, and as such, adequate tooth preparation to ensure these parameters are fulfilled may result in further undermining and resultant weakening of residual tooth structure.
The Nayyar core has been the most prevalent application of amalgam as a core material, and this technique has been shown to provide a reliable seal for the endodontic obturation, as well as providing a stable foundation restoration for any overlying indirect restorations. In some cases, where the morphology of the residual tooth dictates (e.g. thin axial walls, inadequate cuspal height), the Nayyar core technique may be employed to build up a direct ‘amalgam crown’ which utilises the canal orifices and pulp chamber morphology to retain a single restoration from orifice to cusp tip. It should be noted, however, as with any technique, that the efficacy of amalgam as a core material is primary derived from the initial seal at the restoration-obturation interface; this is best achieved with a layer of barrier material, such as glass ionomer cement or Cavit, between the obturation material and the amalgam core. Pulp burs or post preparation drills may be utilised to prepare adequate width and depth of space to allow condensation of amalgam into orifices and chambers (Fig. 17.7).
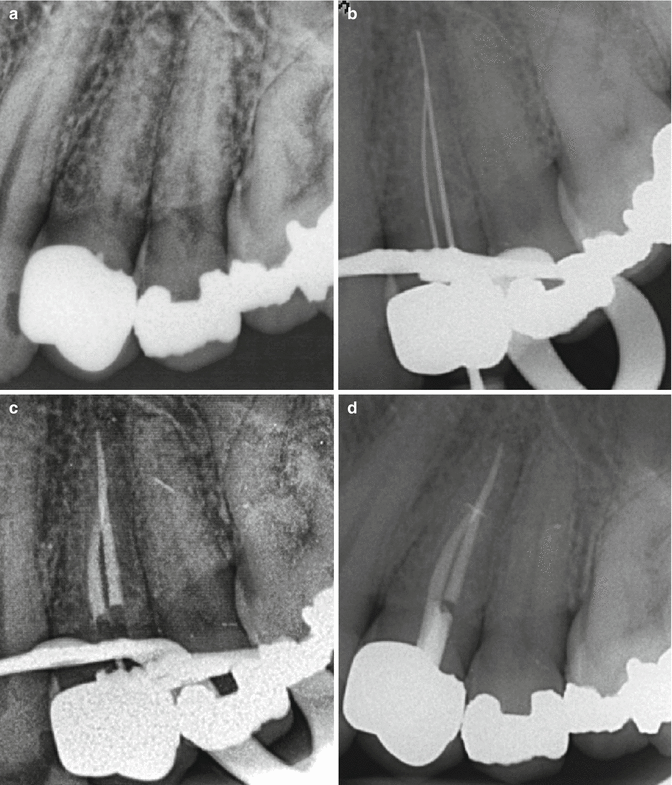

Fig. 17.7
Clinical radiographs demonstrating nonsurgical endodontic treatment of tooth 24 through a metal-ceramic crown restoration. Note: (a) preoperative view of tooth 24 demonstrating periradicular infection and calcified root canal system. (b) Following access cavity preparation through the crown, two canals were located which were confluent in the apical 1/3. Chemo-mechanical preparation was completed using sodium hypochlorite solution (1 %), and an interim calcium hydroxide dressing was placed for 3 weeks. (c) The canals were obturated using AH plus cement and warm vertical compaction technique. (d) The coronal pulp chamber and access cavity is sealed with a Nayyar core technique
Composite
The advent of reliable resin bonding techniques by Buonocore has led to the use of resins in various restorative situations, including as a core material. The primary obstacles for all resin restorations are inherent in these situations, as they often involve challenging moisture control and poor access for light penetration to photoactivators. However, improved handling characteristics and physical properties have resulted in composite resins being utilised more widely as a core material, not only in aesthetically sensitive sites but also posterior teeth where access may be more difficult. Enhanced packability (i.e. the ability for composite resin to be condensed by instrumentation) allows clinicians to place resins into smaller and more morphologically complex cavities. Reduced polymerisation shrinkage and smaller accompanying c-factors have also played a significant role in the suitability of composite resin materials for placement into previously inappropriate cavity configurations. In addition, the increased prevalence of dual- or self-curing resins has given clinicians greater flexibility in the range of situations in which these materials may be utilised with greater degrees of success, where light penetration may be less than optimal (e.g. deep orifices, posterior teeth). Despite advances in dentine bonding, clinicians should still be wary of utilising resins at the obturation-restoration interface, as moisture control following preparation can often be difficult in these sites, and the use of a barrier material (such as GIC or Cavit) is still recommended (see Fig. 17.8).
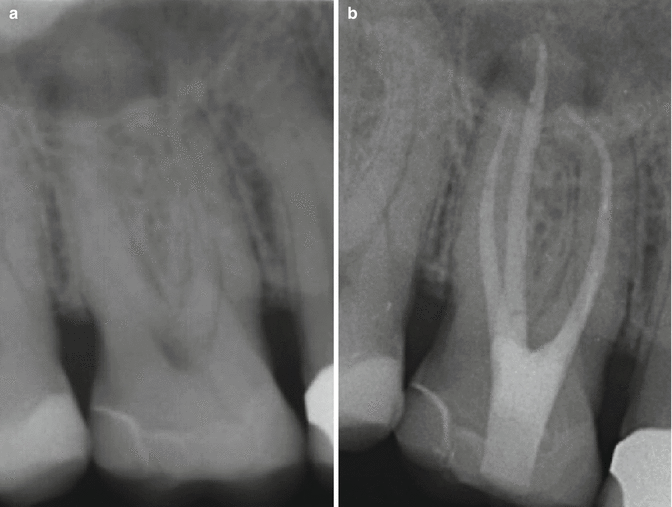

Fig. 17.8
Clinical radiographs demonstrating nonsurgical root canal treatment of tooth 26. Note: (a) preoperative radiograph showing ceramic onlay restoration. The tooth was non-vital with a periradicular radiolucency associated with the palatal root. (b) Completed endodontic treatment with a glass ionomer and composite core buildup
Glass ionomer cement
Various forms of glass ionomer cement (GIC) have become available since the early introduction of the material, which have improved on the handling characteristics and mechanical properties of conventional GIC. These include metal-reinforced GIC, resin-modified (or hybrid) GIC and compomers. As with any core material, however, compressive strength and resistance to fracture under oblique loading situations is highly critical; to date, none of these variations or conventional forms of GIC appear to meet the criteria for satisfactory core restorations. The use of GIC as a lining material under other core materials is recommended due to its tight chemical seal with dentine under moist conditions.
Pins
The use of pins to facilitate the mechanical retention of restorative materials has been widely documented and practised. However, due to advances in the chemical adhesion of resin and glass ionomer materials to tooth structure, their use has been increasingly limited to scenarios in which mechanical retention is lacking for metallic (cast/indirect or condensed/direct) restorations. The use of pins has also been shown to increase susceptibility of surrounding tooth structure to fracture, especially in areas where the morphology of residual tooth structure is thin or undermined. As such, the use of pins should be avoided in canal orifice or peri-radicular areas, as residual dentine walls are often thin and significantly weakened. In addition, the use of amalgam in these situations most often does not require the auxiliary mechanical retention provided by pins as the divergent canal orifices and pulp chamber morphology should provide sufficient retentive form for the core.
17.3 Full Cuspal Coverage Restorations
Amalgam
The use of amalgam as a definitive, cuspal coverage restoration in endodontically treated teeth is well documented. The historical use of amalgam as a conventional restorative material for large posterior restorations has led naturally to its employment in cuspal coverage situations for endodontically treated teeth. This is most conventionally performed as a single amalgam post-core-crown restoration, where amalgam is condensed from the prepared canal orifices all the way to the coronal cuspal aspect. As with all cuspal coverage restorations using amalgam, it is important to follow cavity preparation guidelines, especially with regard to adequate cuspal reduction to allow for sufficient bulk strength of amalgam over these sites. The direct amalgam crown is a particularly useful technique when the morphology of residual tooth structure indicates that further axial preparation will lead to significant weakening of the tooth, or loss of retention or resistance form. Its use should also be considered when previous restorations have deep gingival margins, which may then lead to encroachment of the biologic width with further gingival preparation for indirect restorations. The ability to visualise and prepare a deep gingival margin as well as the potential difficulties associated with tissue management, moisture control and accurate impression taking should also be considered, and in these situations, a direct amalgam crown may be more appropriate.
Gold
The main advantage of the cast gold restoration is its high strength in thin sections, which allows for minimal preparation of underlying teeth. In addition, the finer preparation margins allow for better adaptation and seal with mechanical burnishing of high-gold alloys against preparation margins. As such, in endodontically treated teeth which have already suffered significant loss of tooth structure, especially on the axial aspects, cuspal coverage utilising gold is of great value in preserving the remaining tooth structure. In addition, posterior sites with limited interarch (or inter-occlusal) space also benefit from the minimal occlusal reduction required for placement of cast gold restorations. Conversely, teeth that have minimal loss of existing structure other than the endodontic access cavity may also benefit from the maximal preservation of tooth material afforded by cast gold preparations. These less extensive preparations may take the form of partial onlays, three-quarter or seven-eigth crowns (partial veneers) which seek to provide protection of vulnerable cusps (with flexure widths of under 3 mm) without further preparation of more robust areas of the residual tooth; this in turns allows for less destruction of tooth structure and also preservation of buccal faces for aesthetic purposes. Cast gold restorations can also be luted onto tooth structure with most luting agents, excluding those which require photoactivation for polymerisation. As such, in sites where moisture control may be difficult, the placement of cast gold restorations utilising conventional GIC or zinc phosphate cements may be highly appropriate.
Ceramic
The use of all-ceramic restorations for the restoration of endodontically treated teeth is a relatively contemporary phenomenon, with the advent of stronger ceramic materials allowing clinicians to increase their restorative armamentarium in such situations. The move away from purely feldspathic porcelains to tougher, more resilient ceramic materials has led to the increasing use of these restorations in a wider range of clinical scenarios. More recently, the burgeoning technologies of computer-aided design (CAD) and computer-aided manufacture (CAM) have resulted in a plethora of ceramic materials being available for multiple clinical uses, including cuspal coverage restorations. Leucite-reinforced lithium disilicate, zirconia and alumina are the major material types currently available on the ceramic market. These materials boast physical properties which make their consideration in certain clinical scenarios appropriate; these include high compressive and flexural strength, low coefficient of thermal expansion and favourable optical properties. However, due to this diversity of materials and their properties, clinicians must exercise care in their selection of the appropriate material for each case, as their varying properties will have a significant influence on their success in each scenario. One of the main points to consider is the flexural strength of these restorations, especially in thin sections, which may be required at gingival margins. In addition, the suggested luting materials for these restorations are often resin-based, which requires absolute moisture control, which may be difficult to achieve in certain sites. Wear of opposing materials (restorative or natural tooth) should also be considered when employing ceramic restorations that may or may not be veneered by feldspathic porcelain or treated with glazing layers. The increased use of monolithic materials by clinicians and laboratories employing on-site CAD/CAM fabrication processes requires clinicians to be vigilant about achieving high surface smoothness by appropriate polishing protocols.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


