Diagnosis
n
Male
Female
UCL/P
10
6
4
BCL/P
6
5
1
Facial cleft
2
1
1
Total
18
12
6
All patients underwent a thorough history and clinical examination as well as a complete dental and orthodontic examination. Preoperative and postoperative photographic and cephalometric records were obtained as reported previously. Time was spent with the patient and the patient’s family, explaining the distraction process in detail utilizing photographs, video imaging, as well as discussions with other patients and their families who have undergone the procedure. The patient and parents were thoroughly familiarized with the distraction apparatus and its mechanics prior to the procedure.
For this group of patients, a custom-made intraoral orthodontic splint, which acts as the link between the maxillary skeleton and distraction apparatus, was inserted in each patient (Fig. 28.1). This intraoral splint was constructed with rigid 0.045 or 0.050 stainless steel orthodontic wire. The splint was cemented to the first permanent molars or second primary molars and was further secured at the time of surgery with circumdental stainless steel surgical wire. For older children and adults, the splint was inserted in the clinic prior to the surgical procedure. For young children, the splint was placed in the operating room after anesthetic induction and prior to the osteotomy. External traction hooks were bent under and in front of the upper lip with the end of the hook ending at the level of the palatal plane. The splint also included intraoral hooks that were utilized for the required retention phase at the completion of active maxillary distraction. Certain orthodontic tooth movements as well as orthodontic expansion of the upper arch can be performed at the time of maxillary distraction by incorporation of an expansion screw and segmentalizing the intraoral splint into two units. In order to improve rigidity, the splint can be manufactured by using an orthodontic cervical face bow. The external bow is bent to create the external traction hooks. Currently, the intraoral part of the splint utilized at our center is made of heavy 0.045 or 0.050 stainless steel orthodontic wire. In the anterior region, two square tubes are soldered just medial to the oral commissures (Fig. 28.1e). These tubes are used to house removable traction hooks made of heavy rectangular wire (Fig. 28.1f). This design offers the advantage of not having the external traction hooks present at the time of surgery facilitating anesthesia management and intraoral surgical manipulation.
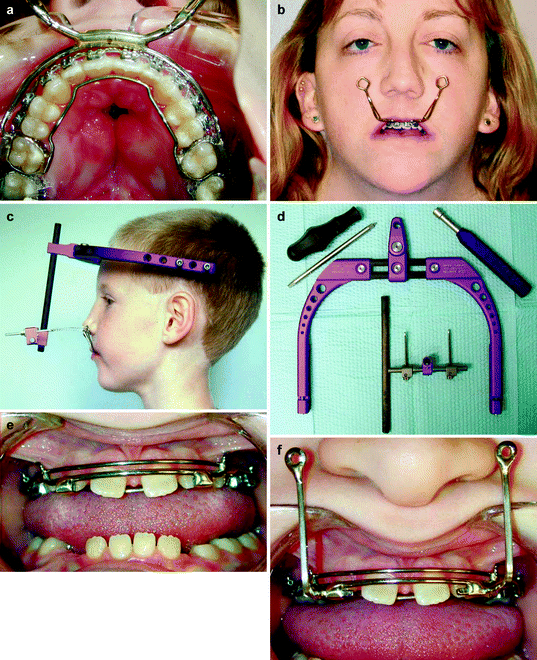

Fig. 28.1
(a) Intraoral view of original design made from an orthodontic face bow for the intraoral splint, anchored to the first molars and further secured with circumdental wires. (b) Facial view of patient wearing the device prior to surgery and demonstrating the external traction hooks. (c) Patient wearing the Rigid External Distraction system, note wires connecting traction hooks from the intraoral splint to the traction screws from the rigid external distraction device. (d) Disassembled distraction device, note posterior screws on the halo, utilized during midfacial advancement to clear the anterior part of the halo from forehead. (e) Intraoral view of newly designed intraoral splint with removable external distraction hooks. Designed in this fashion to avoid the presence of the hooks at surgery. (f) Intraoral splint with removable distraction hooks in place
All 18 patients in this series underwent a LeFort I osteotomy with the height of the transverse osteotomy varying depending on the dental age and aesthetic requirements of each patient. In patients with transitional dentition, a high transverse maxillary osteotomy was performed, just below the level of the inferior orbital rim. The osteotomy circumvents the infraorbital foramen to prevent injury to the infraorbital neurovascular bundle and avoids all permanent tooth buds. Mobilization of the maxillary segments is achieved, including pterygomaxillary and septal disjunction. No intraoperative repositioning of the maxillary segments is performed, and no autogenous or alloplastic bone grafting or internal skeletal fixation hardware is utilized. For the patients in this series who underwent rigid external distraction, the halo portion of the distraction device was placed immediately after closure of the intraoral incision. In the first four consecutive patients with severe cleft maxillary hypoplasia that we elected to treat with maxillary distraction, we performed the distraction with elastic traction as described below. After four consecutive treatment failures in these patients, we abandoned elastic distraction for rigid external distraction.
Fourteen patients underwent rigid external maxillary distraction (Fig. 28.1, Table 28.2) (Polley and Figueroa 1997). These patients had the rigid device placed at the time of surgery and had their distraction performed through mechanical activation of the distraction device. Four patients in this series underwent face mask elastic distraction osteogenesis (Table 28.2). An orthodontic face mask was utilized with elastics placed on the intraoral hooks. Up to 2 lb of elastic force was utilized for each patient through a combination of 8-oz elastics. Patients were instructed to wear the face mask 24 h a day for a period of 3 months. All patients underwent a latency period of 4–5 days following the osteotomy and then began distraction. For the rigid external distraction group, distraction was performed at the rate of 1 mm/day. In this group, the distraction device was kept in place 3–4 weeks following completion of the distraction process for rigid retention. An additional 4–6 weeks of face mask elastic retention at night time only was utilized in this group. For the rigid external distraction group following the period of rigid retention, the external distraction device was removed in an office setting. For the very young patients in this series, the distraction device was removed with mild sedation.
Table 28.2
Treatment groups by diagnosis
|
Distraction
|
UCL/P
|
BCL/P
|
BCL/P + FC
|
Total
|
|---|---|---|---|---|
|
Rigid external
|
9
|
3
|
2
|
14
|
|
Face mask
|
3
|
1
|
–
|
4
|
28.2 Cephalometric Evaluation
The preoperative and postretention lateral cephalometric radiographs were utilized for analysis. The radiographs were traced on 0.003-in acetate paper, and 12 anatomic landmarks were recorded (Fig. 28.2). All tracings were done by a single experienced investigator (A. A. Figueroa). Availability of serial radiographs in all patients permitted landmark verification. All x-rays were corrected to 0 % magnification. Based on the recorded anatomic landmarks, 13 measurements were calculated, 6 angular and 7 linear (4 horizontal and 3 vertical). For the linear measurements, an x-y coordinate system utilizing the S-N plane as the horizontal was employed. Linear horizontal changes were measured relative to a line perpendicular to the S-N plane passing through sella, and vertical changes were measured perpendicular to the S-N plane. The preoperative and postoperative cephalometric values in the rigid external distraction group were statistically analyzed by means of a paired t-test. The numbers in the face mask distraction group were too small for meaningful statistical analysis for intragroup and intergroup comparisons.
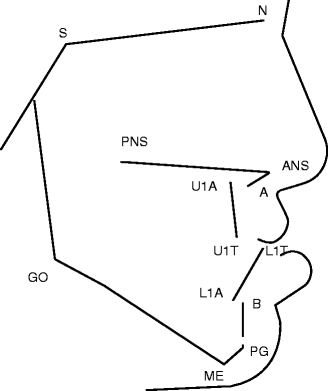

Fig. 28.2
Anatomic landmarks and reference planes. Anatomic landmarks: sella (S), center of sella turcica; nasion (N), most anterior point of the nasal frontal suture; anterior nasal spine (ANS), most anterior point of the spine; A point (A), most anterior limit of the maxillary alveolar bone at the level of the incisor root apex; posterior nasal spine (PNS), intersection between the nasal floor and the posterior contour of the maxilla; apex of maxillary incisor root (U1A), uppermost point of the incisor root; tip of maxillary incisor crown (U1T), maxillary incisor edge; tip of mandibular incisor (L1T), mandibular incisor edge; apex of mandibular incisor root (L1A), lowermost point of the mandibular incisor root; B point (B), most anterior limit of the mandibular alveolar bone at the level of the incisor root apex; pogonion (PG), most anterior limit of the mandibular symphysis; menton (ME), most anterior point of the mandibular symphysis; gonion (GO), the point at the greater convexity of the mandibular gonial region. Reference planes: sella-nasion plane (SN), palatal plane (line through ANS and PNS), maxillary incisor axis (Ul) (line passing through U1A and UIT); and mandibular plane (tangent to the lower border of the mandible through ME and GO)
28.3 Results
Surgery in this series was performed on either an outpatient or a 23-h admission basis by a single experienced surgeon (Polley). No patient in this series was discharged later than the morning after surgery. Perioperative antibiotics were routinely used. All patients began routine oral hygiene and an unrestricted soft diet 24 h postoperatively. No intermaxillary fixation was utilized.
There was no surgical morbidity in any of the 18 patients in this series. There were no complications of bleeding or infection. No patients required a blood transfusion, and there were no problems of dental injury, avascular necrosis, or gingival injury. In the patients who underwent rigid external distraction, there were no complications with wearing the external device including pain, discomfort, or loosening of the device during the distraction process. The intraoral splint remained intact in all patients through the active and retention phases. None of the families had difficulty following the guidelines for the distraction, which they carried out at home.
The postdistraction cephalometric radiographs for all patients who underwent either rigid external or face mask distraction were obtained 4 months following distraction. The predistraction and postdistraction angular cephalometric measurements for those patients undergoing rigid external and face mask distraction are given in (Table 28.3). The differences in the linear measurements between the predistraction and postdistraction cephalometric radiographs for each group are given in (Table 28.4). In all of the patients who underwent rigid external distraction, the desired treatment goals were obtained. All patients in the face mask distraction group were undercorrected with residual edge to edge anterior dental relations or remained in anterior crossbite. The results in all patients in the face mask distraction group were considered unsuccessful.
Table 28.3
Predistraction and postdistraction angular cephalometric measurements for rigid external and face mask distraction groups
|
Distraction
|
Measurements (degrees)
|
Predistraction
|
Postdistraction
|
Difference (4 months)
|
Significance
|
|
|---|---|---|---|---|---|---|
|
Rigid external (n = 14)
|
SNA
|
77.6
|
±5.6
|
85.3 ± 5.6
|
7.7 ± 2.9
|
**
|
|
SNB
|
78.8
|
±4.0
|
77.9 ± 4.1
|
–0.8 ± 1.8
|
NS
|
|
|
ANB
|
–1.2
|
±3.5
|
7.3 ± 3.0
|
8.6 ± 3.6
|
**
|
|
|
Convexity (NAPg)
|
–3.5
|
±7.5
|
13.7 ± 6.0
|
17.2 ± 7.3
|
**
|
|
|
Mand. Pl./SN angle
|
39.2
|
±6.7
|
41.4 ± 5.9
|
2.2 ± 2.4
|
*
|
|
|
Ul-P.PL. angle
|
100.7
|
±15.7
|
98.8 ± 14.4
|
–1.2 ± 11.3
|
NS
|
|
|
Face mask (n = 4)
|
SNA
|
77.5
|
±4.3
|
80.3 ± 5.5
|
2.8 ± 4.9
|
|
|
SNB
|
82.9
|
±4.3
|
81.3 ± 3.3
|
–1.6 ± 3.8
|
||
|
ANB
|
–5.4
|
±2
|
–1.0 ± 3.4
|
4.4 ± 2.7
|
||
|
Convexity (NAPg)
|
–12.2
|
±3.5
|
–3.4 ± 7.4
|
8.8 ± 5.5
|
||
|
Mand. P1./SN angle
|
33.2
|
±4.9
|
36.5 ± 3.6
|
3.3 ± 4.3
|
||
|
Ul-P.PL. angle
|
105.1
|
±13.1
|
107.3 ± 10.4
|
2.2 ± 11.8
|
||
Table 28.4
Predistraction and postdistraction linear cephalometric measurements for rigid external and face mask distraction groups
|
Landmark (axis)
|
Pre-post distraction change rigid external (mm)
|
Pre-post distraction change face mask (mm)
|
|---|---|---|
|
ANS-x
|
7.1 ± 3.9*
|
2.9 ± 1.4
|
|
ANS-y
|
–0.4 ± 3.0
|
–1.3 ± 1.8
|
|
A point-x
|
8.3 ± 3.3*
|
2.8 ± 2.1
|
|
A point-y
|
–1.3 ± 3.4
|
–1.7 ± 2.3
|
|
U1-x
|
11.6 ± 4.6*
|
5.2 ± 2.1
|
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


