Fig. 27.1
An electromechanical digitizer used to extrapolate x, y, and z coordinates from a plaster palatal cast
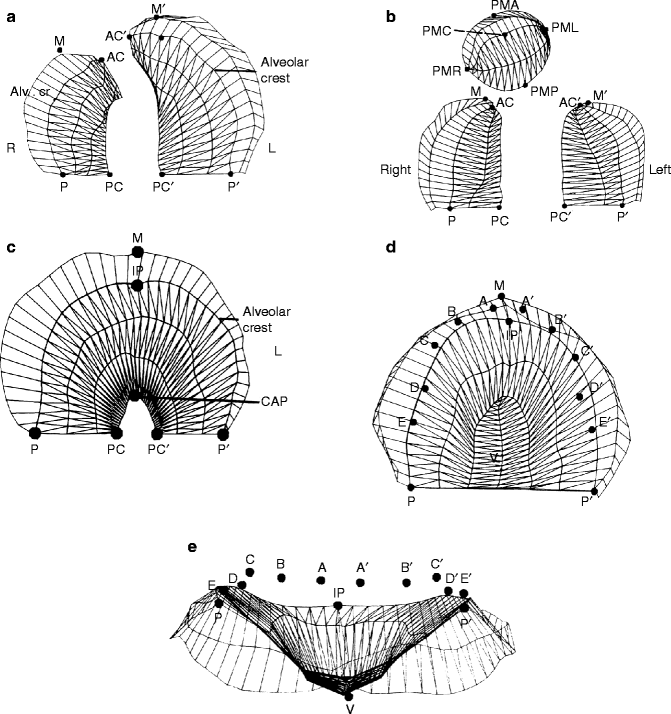
Fig. 27.2
(a–e) Computer-generated images of various cleft palate types. (a) Complete unilateral cleft lip and palate. (b) Complete bilateral cleft lip and palate. PMA premaxilla anterior, PMP premaxilla posterior, PMC premaxilla center, PMR premaxilla right, PML premaxilla left. (c) Isolated cleft palate. (d) Normal palate: occlusal view. (e) Normal palate: posteroanterior view. P postgingivale comparable to PTM (pterygomaxillary fissure on a lateral cephalograph). It is the posterior border of the hard palate, PC landmark on the PP line at the cleft, AC anterior point of the alveolar ridge at the cleft, M the most anterior point of the palatal segment, IP incisal papilla point, V highest vault point, A deciduous central incisor, B deciduous lateral incisor, C deciduous cuspid, D deciduous first molar, E deciduous second molar. Palatal Surface Area. Before cleft closure: Bounded laterally by P to AC, P to Pc and PC9 to P9, P9 to Ac9. After cleft closure: Includes cleft space bounded by AC to AC9 and PC to PC9. Cleft Space Area: Anterior limit AC–AC and posterior boundary PC to PC9. In Bilateral Clefts: Anterior Cleft Space: Bounded anteriorly by the premaxilla’s outer point of the alveolar crest RPM or LPM to AC and posteriorly by line AC to AC9. Posterior Cleft Space: Bounded by AC to AC, AC to PC, and PC to PC9
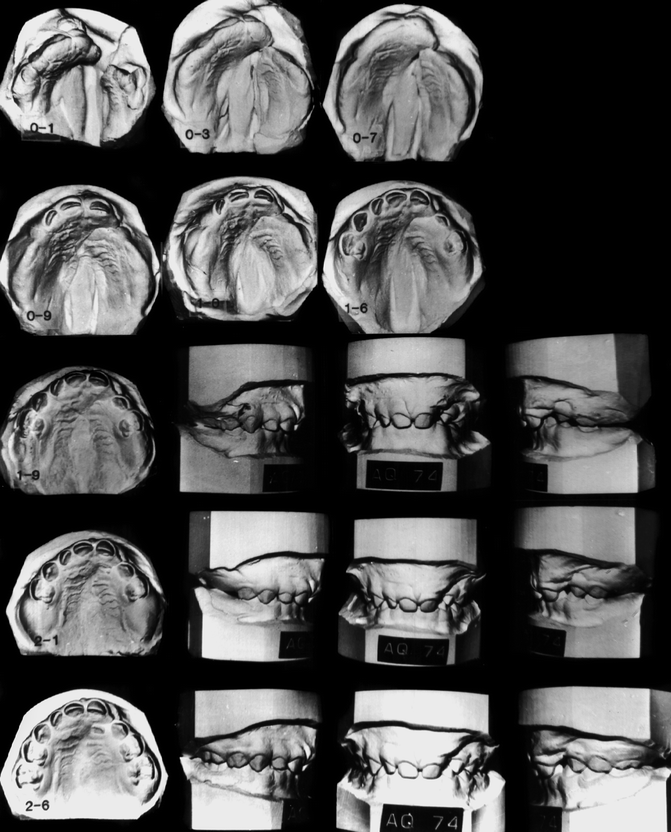
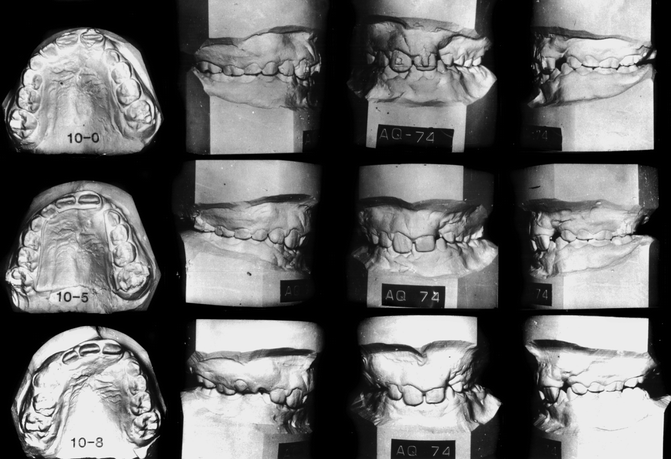
Fig. 27.3
Serial dental casts for case JH (AQ-74) show: 0–1. Separated palatal segments soon after birth. 0–3. Palatal segments move together forming a butt joint relationship 0–7, 0–9, 1–6, and 1–9. What appears to be a “collapsed” state is not so. 2–1 and 2–6. The buccal teeth are in an ideal occlusal relationship 10–0, 10–5. and 10–8. Palatal growth maintains the excellent palatal arch relationship. The central incisors were brought together at 8 years of age prior to secondary alveolar bone grafts
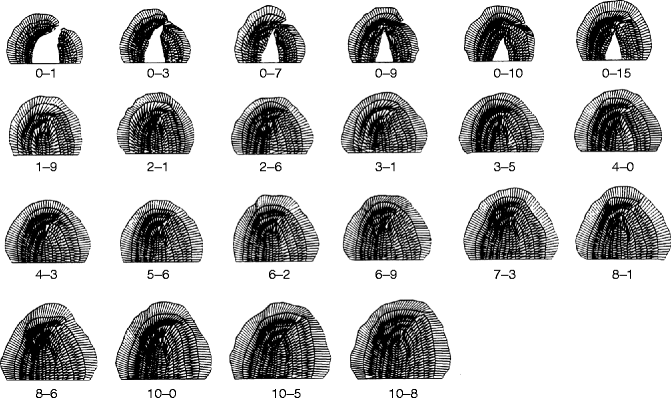
Fig. 27.4
Case JH AQ-74. Computer-generated images of serial casts drawn to scale. This series demonstrates the decrease in cleft spaces associated with an increase in palatal size
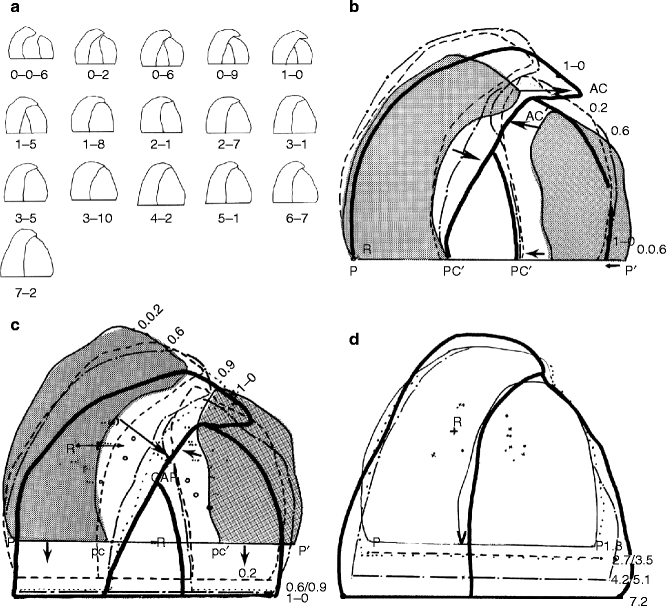
Fig. 27.5
(a) Computer-created serial casts drawn to scale from birth to 7 years and 2 months. (b) Outline tracings at 6 days, 2 months, and 1 year of age superimposed on the baseline P–P1 and registered at midpoint of the line. This illustration shows the medial movement and changes in size of the palatal segments. (c) The same palatal segments are superimposed on the palatal rugae to show the amount and direction of palatal growth and movement brought on by uniting the lip. From 2 days to 1 year of age. (d) Outline of palatal segments from 1 year and 8 months of age to 7 years and 2 months. This illustration shows that most of the palatal growth occurs posteriorly with a slight increase in width with little anterior bony apposition
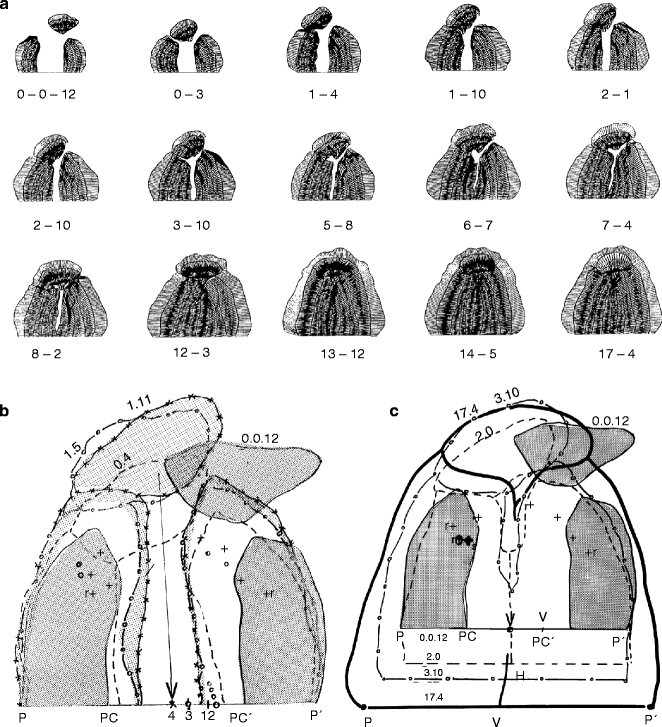
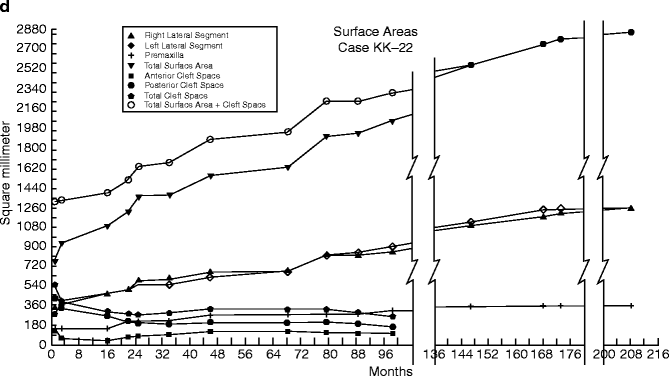
Fig. 27.6
(a–d) Case PM (K-22). (a) Computer-drawn serial casts of a complete bilateral cleft lip and palate drawn to scale showing quantitative and geometric palatal changes as a result of growth and treatment. No presurgical orthopedics. (b) Serial casts superimposed on the base line P to P, registered at V (the point where the vomer meets the baseline). This shows changes in palatal size and palatal relationships. (c) Serial casts from 12 days to 17 years and 4 months. These casts were superimposed on the rugae points with the PP’ line parallel. Most of the palatal growth occurred posteriorly, with only a slight increase in midfacial protrusion compared to the initial premaxillary protrusion. The width increased in proportion to length (d) Time sequence analysis of palatal growth in a complete bilateral cleft of the lip and palate. By 6 years, the palatal growth (including cleft space) more than doubled
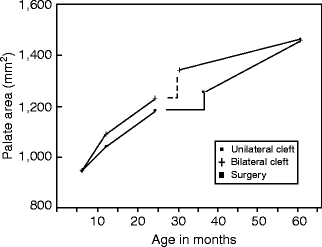
Fig. 27.7
Graph showing growth changes in surface area of 14 CBCLP and CUCLP prior to and after palatal cleft closure surgery. The palatal growth acceleration in the CBCLP was greater the first year, then similar in the two cleft types up to 25 months, just prior to palatal surgery. At the time of surgery, the cleft space in the CBCLP series was greater than in the CUCLP series. After surgery, the palatal growth acceleration curve of the CBCLP series decreased, while that of the CUCLP series increased. A modified von Langenbeck procedure to close the cleft space was used in both cleft types. The sample of cases is being increased to determine the influence of cleft size on future palatal growth and development
Berkowitz (1971) initiated a study to determine the feasibility of using stereophotogrammetry to graphically describe the changing configuration of cleft palates. Data from the study supported the clinical impressions that palatal molding action with palatal growth, which occurred at the palate’s medial border, effectively diminished the width of the cleft space. A second study Berkowitz et al. (1974) was undertaken to further improve the stereometric technology in order to permit the investigation of a larger number of casts. A profile study of nine complete unilateral cleft lip and palate casts demonstrated that the widths of the vault space varied greatly between cases. This was followed by another investigation using an “optical profilometer” (Berkowitz et al. 1982) designed and built by National Aeronautics and Space Administration (NASA) for Berkowitz under a technology utilization transfer grant. This led to the use of an electromechanical digitizer as the instrument of choice for analytical studies of serial casts designed to describe the changing geometry and size of the palatal vault and the geometrical and size relationship between the greater and lesser palatal segments in complete unilateral cleft lip (CUCLP) and palate and the lateral palatal segments and premaxilla in complete bilateral clefts of the lip and palate (CBCLP) (Figs. 27.5 and 27.6).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


