Fig. 11.1
Of 61 patients with obstructive events, 25 required tracheostomy, of which 11 were syndromic (Stickler syndrome (a group of genetic disorders affecting connective tissue), Treacher Collins (congenital craniofacial syndrome), and others) and other 14 patients had isolated Robin sequence
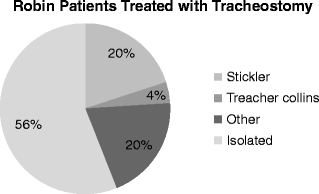
Fig. 11.2
Of 25 patients treated with tracheostomy, 44 % (11 cases) were syndromic, of which 45 % (5 cases) was either Stickler or other syndromes and 10 % (1 case) was Treacher Collins and the other 56 % (14 cases) had isolated RS
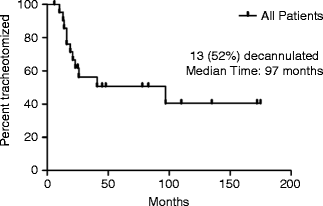
Fig. 11.3
Of 25 infants treated with tracheostomy, 13 infants (52 %) were eventually decannulated with median time to decannulation of 97 months
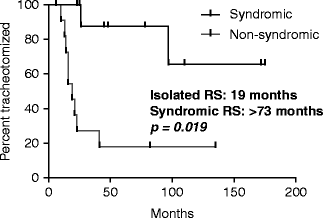
Fig. 11.4
Patients with syndromic RS had a median time to decannulation of >73 months versus patients with isolated RS had a median time to decannulation of 19 months, p = 0.019
At mean follow-up of 4 years, the rate of tracheostomy-specific complications (e.g., cannula obstruction or accidental decannulation, delays in speech and language development, tracheomalacia (flaccidity of the tracheal support cartilage)/tracheitis, pneumonia) was 52 % and tracheostomy-specific mortality was 8 %. Patients with syndromic RS stayed in the hospital significantly longer than patients with isolated RS (50 versus 28 days, respectively). There was one death in each group; however, patients with syndromic RS had significantly more events of end-organ dysfunction (neurogenic, gastrointestinal, and/or cardiopulmonary) per patient than patients with isolated RS (2.08 versus 0.69, p = 0.005).
11.4 Discussion
Based upon the literature, approximately 2/3 of patients with RS can be successfully managed with conservative therapies (Kochel et al. 2011; Gozu et al. 2010; Evans et al. 2006; Horikiri et al. 2010). Prone positioning is often sufficient in less severely affected patients but may result in prolonged hospitalization (Kochel et al. 2011; Sher 1992; Bhat et al. 2006). NPA can be effective in during the early clinical course to avoid emergent tracheostomy, but difficultly maintaining proper position for an extended period of time has limited its use (Chang et al. 2000; Sher 1992; Kochel et al. 2011; Masters et al. 1999; de Buys Roessingh et al. 2007). Lastly, orthopedic devices have been tried with success in a few small studies but these devices are often expensive (Hotz and Gnoinski 1982; Buchenau et al. 2007; Kochel et al. 2011). More recently, Kochel et al. described the usage of newer orthopedic devices as another noninvasive way to treat upper airway obstruction. Three major types (plate with a posterior wire spur, plate with a posterior acrylic extension, and plate with a pharyngeal tube) of orthopedic devices were used in seven patients based on their mechanisms of the obstruction (Sher’s classifications; see Sect. 11.4). All of the seven patients had normal oxygen saturation upon discharge and at the end of study period, five out seven patients tolerated the removal of the orthopedic devices (Kochel et al. 2011).
Surgical modalities such as glossopexy or TLA, mandibular distraction, mandibular extension, and subperiosteal release of floor of mouth muscle have been studied extensively for their effectiveness in avoiding or delaying tracheostomy, improving polysomnographic results, facilitating feeding, and bypassing or correcting the anomalous anatomy. TLA, subperiosteal release of floor of mouth muscle, and mandibular distraction have been described most frequently in the recent literature. TLA temporarily bypasses the obstruction by creating a stable airway with reported success rates between 70 and 100 % (Denny et al. 2004; Bijnen et al. 2009; Kirschner et al. 2003). Dehiscence (breaking down of the incision) still ranges between 0 and 57 % with a mean of 30 % (Sher 1992; Marques et al. 2001; Bookman et al. 2011). Based on a few studies, the need for a secondary invasive airway procedure such as tracheostomy after subperiosteal release ranges between 10 and 100 % (Delorme et al. 1989; Caouette-Laberge et al. 1996; Breugem et al. 2008; Siddique et al. 2000). Mandibular distraction has been shown to improve polysomnographic outcome, to avoid or delay tracheostomy, and to expedite decannulation of a tracheostomy (Scott et al. 2011; McCarthy et al. 1992; Denny et al. 2001; Lin et al. 2006; Schaefer et al. 2004; Schaefer and Gosain 2003). Nevertheless, complications such as infection, device failure, and nonunion occur from 2.5 to 52 % (Caouette-Laberge et al. 1994; McCarthy et al. 2002; Shetye et al. 2009). One large retrospective review of 141 infants with RS who underwent mandibular distraction reported a 52 % overall complication rate with a 5 % major complication rate – a complication that necessitated a secondary invasive therapy (Shetye et al. 2009).
Indications for surgical airway management are also highly debated. While many clinicians rely on a “gestalt” impression of airway obstruction, some have proposed data-driven clinical parameters for airway management. Caouette-Laberge et al. and Cole and colleagues proposed grading systems based on the settings of respiratory obstruction (Caouette-Laberge et al. 1994; Cole et al. 2008). Caouette-Laberge grouped 125 infants with RS into three categories: (1) adequate respiration in prone position and regular bottle-feeding, (2) adequate respiration in prone position and difficulty with feeding, and (3) endotracheal intubation (Caouette-Laberge et al. 1994). Parsons and Smith provided rule of thumb criteria for TLA in infants with RS; those who had progressive weight/strength gain over a 7-day period did not require TLA, while those infants who needed more than 3 days of endotracheal airway support should receive TLA (Parsons and Smith 1982). Freed et al. reported on the use of bedside monitoring and polysomnography to objectively guide airway management for infants with RS (Freed et al. 1988). Criteria for TLA included (1) an average transcutaneous O2 level below 60 mmHg or transcutaneous CO2 level over 50 mmHg for a minimum of 8 h, (2) obstructive episodes on sleep study, and (3) oxygen saturation below 80 %.
More recently, Rogers et al. described the GILLS scoring system where one point was assigned to each of the five variables: gastroesophageal reflux, intubation preoperatively, late operation, low birth weight, and syndromic diagnosis. TLA was 100 % successful in infants with a GILLS score of 2 or less but failed in 43 % of infants with a score of 3 or more (Rogers et al. 2011). Sher detailed the use of flexible fiber optic endoscopy to guide the form of surgical treatment in infants with RS failing conservative measures. Based upon nasopharyngoscopy and identification of the site of obstruction, infant airways were classified into four groups. Type I represented airway obstruction solely due to glossoptosis, while types II–IV had additional components of obstruction. Regardless of airway classification, all patients were initially treated with NPA placement for up to 8 weeks. If conservative therapy failed, type I patients received TLA and types II–IV underwent tracheostomy (Sher 1992). Schaefer et al. described an algorithm for approaching respiratory and nutritional dysfunction in infants with RS. Management decisions were based upon the ability to maintain progress on the growth curve, continuous pulse oximetry and bedside polysomnography, and the site of airway obstruction (Schaefer et al. 2004). Finally, data from our own institution (Fig. 11.5) from a retrospective review of airway management in patients with RS from 1994 to 2010 found that four clinical factors (MIST criteria) were most associated with surgical airway management: maximum CO2 > 62 mmHg, apnea–hypopnea index (index of sleep apnea severity) > 23.0 events/h, minimum O2 saturation < 79.4 %, and greater than 5.7 % total sleep time with O2 saturation less than 90 %. Each of these parameters identified operative intervention with 75–85 % accuracy (Seruya et al. 2011).


Fig. 11.5
MIST criteria for surgical airway management of patients with Robin sequence (RS)
Despite the various procedures described for surgical airway management, tracheostomy remains the most definitive treatment for infants with severe respiratory obstruction that is not compatible with life. In many cases, tracheostomy is believed to be a temporary measure until “natural” mandibular growth permits decannulation. The topic of mandibular growth in patients with RS has been heavily debated yet remains poorly defined. Some authors have documented diminished mandibular size and proportions compared age-adjusted norms while others have cited evidence to the contrary (Shen et al. 2010; Hermann et al. 2003; Daskalogiannakis et al. 2001; Figueroa et al. 1991). Rogers et al. found that mandibular length was shorter in all patients with RS irrespective of the type of airway management, and the differences in both mandibular length and sagittal position varied significantly among all the syndromic subtypes (Rogers et al. 2009). Maalouf et al. found that 60 % of patients who received bilateral mandibular distraction maintained proportionate facial symmetry at the median follow-up time of 57 months; mandibular size, however, was not evaluated (Maalouf and Lehman 2011). Finally, Pruzansky and Richmond demonstrated the opportunity for “catch-up” growth of the mandible without the need for invasive procedures aside from a temporary tracheostomy (Pruzansky and Richmond 2005). Overall, these studies highlight the phenotypic heterogeneity of patients with RS, which may stem from the dissimilar mandibular growth kinetics of isolated versus syndromic patients.
In our retrospective study of 61 infants with RS, 25 patients required tracheostomy (14 cases of isolated RS and 11 cases syndromic RS). This is one of the largest published cohorts of RS children with tracheostomy that have been followed to analyze rates of eventual decannulation due to mandibular growth without other ancillary surgical interventions. The median time to decannulation in our cohort was longer (97 months) than what other smaller series have reported (Tomaski et al. 1995; Demke et al. 2008). Patients with syndromic RS largely contributed to this extended time course, as most of them could not be decannulated by the completion of the study. Outcomes following tracheostomy were significantly poorer in patients with syndromic RS as compared to those with isolated RS: patients with syndromic RS had longer hospital stay and more long-term complications as compared to patients with isolated RS.
11.5 Summary and Conclusion
Airway management in patients with RS and severe airway obstruction remains controversial. The benefits of various surgical airway procedures, as well as indications for intervention, are unclear and based upon imperfect data. Our experience with these complex patients has documented some factors associated with the need for surgical intervention, but these criteria await validation in a randomized prospective trial. We have also found that although tracheostomy was intended to be a temporary airway for these patients, the time to natural decannulation was longer than expected. This may be partially explained by the mandible’s inability to “catch up” in growth, especially in syndromic patients. We are planning further study into these issues by means of a prospective trial that will incorporate serial lateral cephalograms to document mandibular growth as well as offer mandibular distraction as a surgical modality to patients with severe airway obstruction. Based on our experience, we believe that all potential treatment options should be exhausted before offering tracheostomy to syndromic patients with Robin sequence.
Financial Disclosure Information
The authors have no financial or commercial interests to disclose.
Conflict of Interest
None
References
Bhat RY, Hannam S, Pressler R, Rafferty GF, Peacock JL, Greenough A (2006) Effect of prone and supine position on sleep, apneas, and arousal in preterm infants. Pediatrics 118(1):101–107. doi:118/1/101 [pii] 10.1542/peds.2005-1873 PubMedCrossRef
Bijnen CL, Don Griot PJ, Mulder WJ, Haumann TJ, Van Hagen AJ (2009) Tongue-lip adhesion in the treatment of Pierre Robin sequence. J Craniofac Surg 20(2):315–320. doi:10.1097/SCS.0b013e31819ba5ce PubMed
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


