

Fig. 25.1
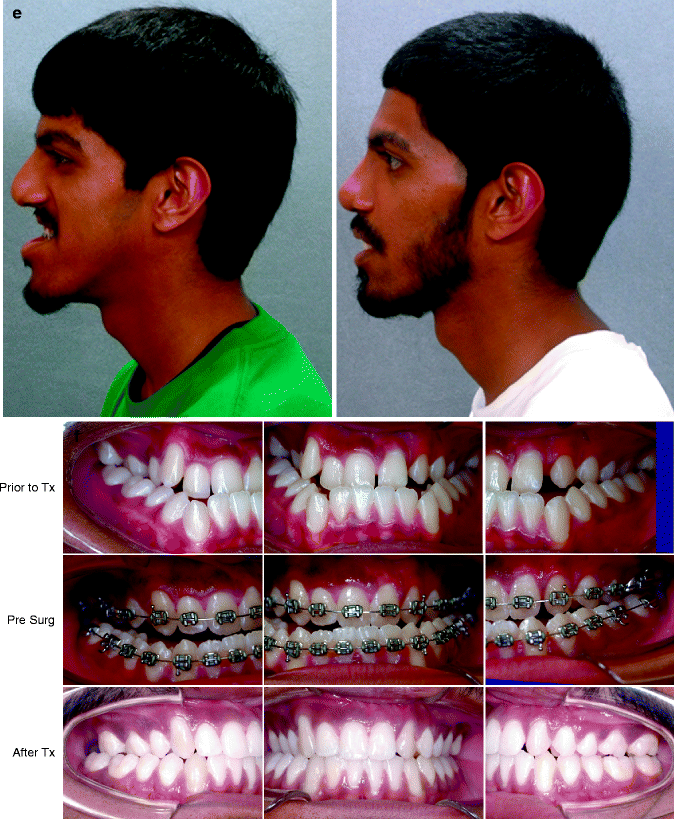
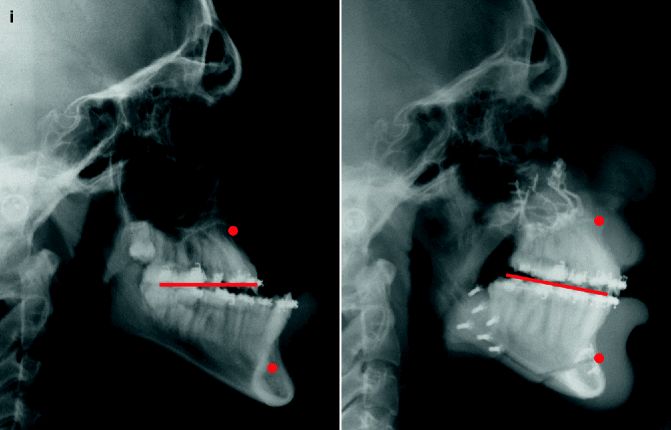
This is a senior high school student who was born with a complete UCLP (left side). He underwent lip and palate repair at another institution. He was then referred to this surgeon and underwent effective bone grafting and fistula closure in the mixed dentition. He developed a jaw deformity characterized by maxillary deficiency and secondary deformities of the mandible and intranasal cavity. He underwent a combined orthodontic and surgical approach. Orthodontic (dental) decompensation included cleft-dental gap (absent lateral incisor) closure. He then underwent reconstruction including maxillary LeFort I osteotomy (horizontal advancement, vertical shortening, midline correction, cant correction, clockwise rotation); sagittal split ramus osteotomies (clockwise rotation, asymmetry correction); osseous genioplasty (vertical shortening); and septoplasty/inferior turbinate reduction/recontouring of floor of nose. Six months after successful orthognathic surgery, he underwent cleft rhinoplasty including rib cartilage (caudal strut) grafting. (a) He is shown in the mixed dentition prior to bone grafting. (b) Frontal views in repose before and after reconstruction (c) Frontal views with smile before and after reconstruction. (d) Oblique facial views before and after reconstruction (e) Profile views before and after reconstruction. (f) Occlusal views prior to orthodontics, with orthodontic dental decompensation in progress, and after reconstruction (g, h) Articulated dental casts before and after reconstruction (i) Lateral Cephalometric radiographs before and after reconstruction
Reconstruction of the alveolar process in UCLP patients is an essential part of cleft care. Accomplishing this goal provides support for the alar base of the nose, the teeth in the cleft region, and the periodontium of those teeth. There are three basic methods described for the closure of the cleft alveolus. The surgical options include: primary bone grafting, secondary bone grafting, and gingival periosteoplasty (GPP). The method of primary bone grafting is now generally recognized to result in severe midface growth disturbance and has therefore been universally abandoned throughout the world (Hathaway et al. 1999; Posnick 1991a, b; Rosenstein 1997). The use of secondary (mixed dentition) bone grafting (Abyholm et al. 1981; Boyne and Sands 1972; Daskalogiannakis and Ross 1997; Hall and Posnick 1984) is generally recognized as an effective method to avoid the problem of midface growth disturbance and is successfully achieved to support the alar base, to provide bone for eruption of the canine through the cleft side, and to establish effective periodontal support. The technique of gingival periosteoplasty (GPP) was first described by Skoog in 1965 as a method to achieve fusion across the cleft alveolus at the time of lip repair (Skoog 1965). The goal was to “remove” the cleft in infancy with the hope that no harm would result. Millard combined the “Latham device” to position the alveolar ridges close to one another before going forward with the GPP procedure at the time of cleft lip repair (Millard et al. 1990, 1999). Grayson and Cutting later proposed the use of a nasoalveolar molding (NAM) device prior to GPP and primary lip repair to accomplish the same alveolar ridge fusion (Grayson and Cutting 2011). Since the late 1970s, clinical studies have been carried out to assess the long-term effects of GPP on midfacial growth in cleft patients. The studies conducted by Millard et al. (1999), Mølsted et al. (2005), Berkowitz and colleagues (2004), Matic and Powers (2008), Renkielska et al. (2005), Henkel and Gundlach (1997), and Tomanova and Mullerova (1994) have all found that patients treated with GPP had poor occlusal relationships with a high need for orthognathic surgery in the teenage years. More recently, Hsin-Yi Hsieh and colleagues completed a retrospective clinical study to evaluate the effects of GPP on facial growth of patients with UCLP (Hsieh et al. 2010). This was a well-done clinical study of a consecutive series of patients that were placed in two study groups, those receiving NAM treatment with GPP and those receiving NAM treatment without GPP. The use of gingival periosteoplasty at the time of lip repair was found to have significant negative effects on the maxillary position (SNA), intermaxillary position (ANB), maxillary length (PMP-ANS), and maxillary alveolar length (PMP-AN) at the age of 5 years. The authors concluded that in patients with an alveolar cleft, the sagittal growth of the maxilla was significantly adversely affected by the gingival periosteoplasty (GPP) procedure.
25.1.2 Bilateral Cleft Lip and Palate
Mulliken and colleagues from Boston Children’s Hospital found that 76.5 % of teenagers with repaired BCLP required maxillary advancement (Good et al. 2007). They showed that the need for orthognathic surgery is dependent on the severity of the cleft type as well as the number and extent of previous operations performed. Results from the Hospital for Sick Children (Toronto, Canada) showed that 65.1 % of their BCLP patients required or underwent orthognathic surgery, while 70 % of BCLP patients referred to their team sometime after cleft lip repair were found to require orthognathic surgery (Daskalogiannakis and Mehta 2009). David et al. from the Cleft Craniofacial Unit in Adelaide, Australia, followed a consecutive group of BCLP patients from birth to maturity and determined the need for orthognathic surgery (David et al. 2006). A skeletal class III malocclusion requiring orthognathic correction was present in 17 of the 19 consecutive patients followed to the age of 18 years (89.5 %) (Figs. 25.2, 25.3, and 25.4). Other earlier research confirms and compliments these findings (Harada et al. 2002; Lisson and Trankmann 1997; Pruzansky 1985).
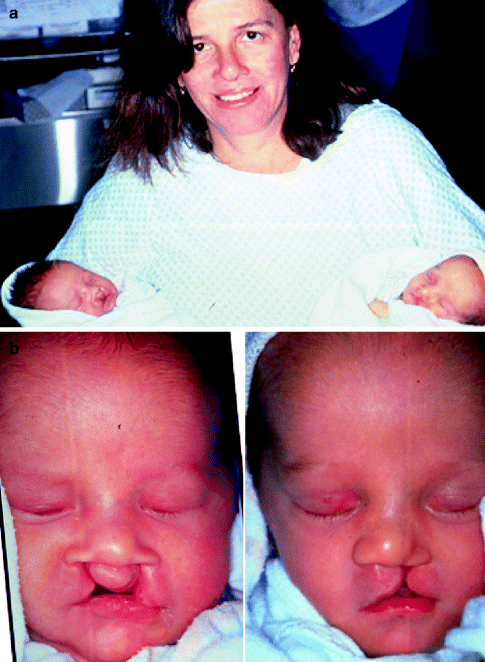
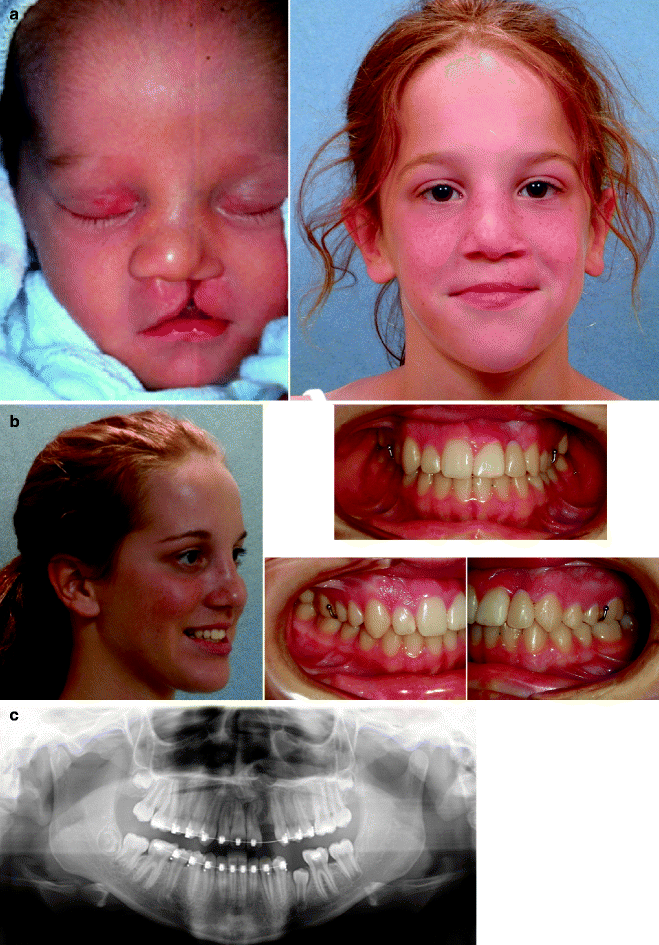
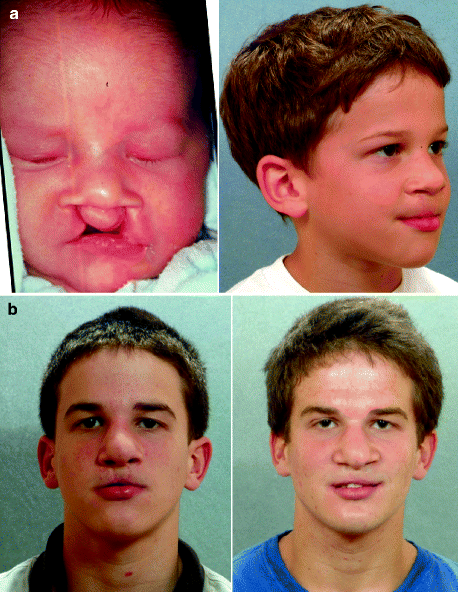
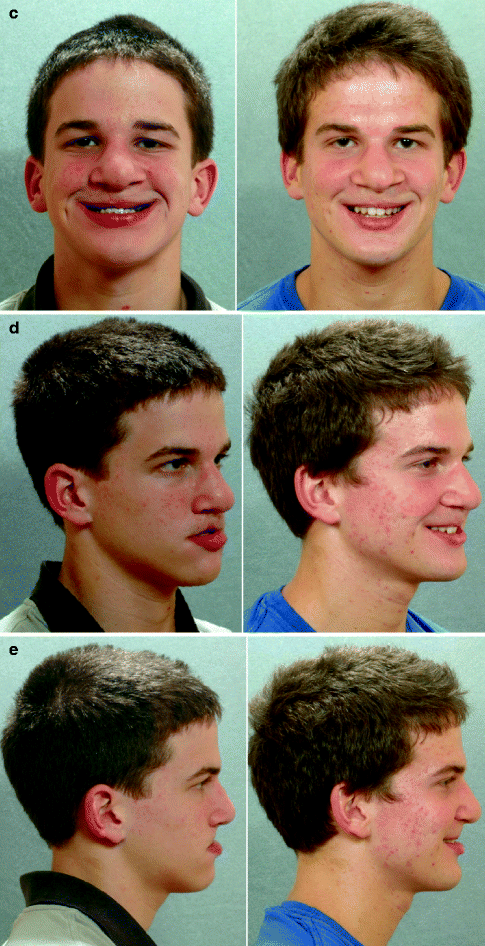
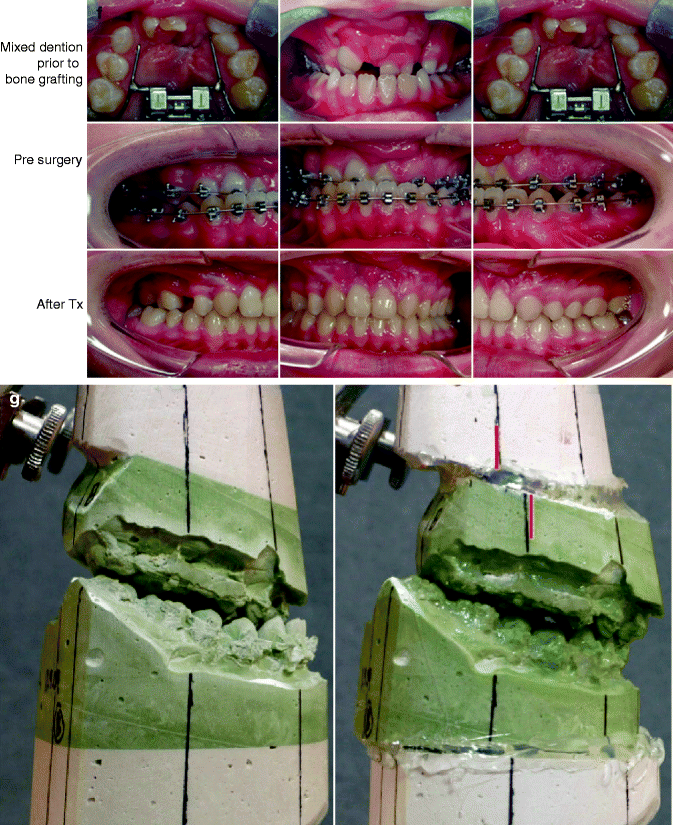
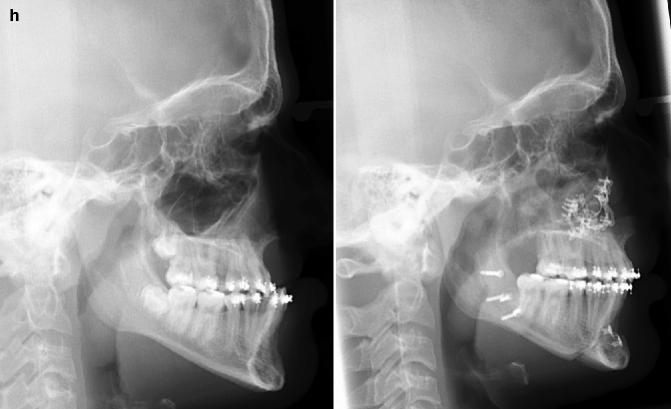

Fig. 25.2
A 40-year-old woman born with BCL and pitting of the lower (central) lip. At the time of pregnancy, ultrasound confirmed twins; one of which was suspected of having BCLP and the other to have UCLP. This was documented at the time of delivery. (a) Family with van der Woude syndrome including mother with repaired BCLP and newborn twins. (b) Twin A with BCLP and twin B with UCLP

Fig. 25.3
A 16-year-old girl born with van der Woude syndrome including UCLP and lower lip pits (see Fig. 25.3). She underwent lip and palate repair in early childhood followed by successful bone grafting and fistula closure in the mixed dentition. She was with normal maxillary growth and underwent standard orthodontic treatment with maintenance of the cleft-dental gap. She underwent an open rhinoplasty including use of a rib cartilage (caudal strut) graft at 15 years of age. There is sufficient bone volume for a dental implant. Implant placement is planned for 18 years of age. (a) Facial views at the time of birth and in the mixed dentition just prior to alveolar bone grafting. (b) Facial and occlusal views as a teenager after rhinoplasty prior to dental implant placement. (c) Panorex as a teenager during orthodontic treatment indicates successful bone grafting of the alveolar cleft




Fig. 25.4
A child born with van der Woude syndrome including BCLP and lower lip pits (see Fig. 25.3). He underwent lip and palate repair including lower lip pit excisions in childhood. He underwent successful mixed dentition grafting and fistula closure. As a teenager, he demonstrates maxillary hypoplasia with secondary deformities of the mandible and chin region. He then underwent a combined orthodontic and orthognathic/intranasal surgical approach. The procedures include standard LeFort I osteotomy (vertical lengthening, horizontal advancement, clockwise rotation with interpositional grafting); bilateral sagittal split ramus osteotomies (clockwise rotation); osseous genioplasty (horizontal advancement); and septoplasty/inferior turbinate reduction/nasal floor recontouring. (a) He is shown at the time of birth and then just prior to mixed dentition grafting. (b) Frontal views in repose before and after reconstruction (c) Frontal views with smile before and after reconstruction. (d) Oblique facial views before and after reconstruction. (e) Profile views before and after reconstruction (f) Occlusal views are shown prior to bone grafting/fistula closure, after orthodontics in preparation for orthognathic surgery and after reconstruction. The congenitally missing right maxillary bicuspid is planned for placement of a dental implant at 18 years of age. (g) Articulated dental casts before and after model planning (h) Cephalometric radiographs before and after reconstruction
25.1.3 Isolated Cleft Palate
Ross documented that at least 20 % of Caucasians with ICP who underwent repair in infancy will experience maxillary hypoplasia resulting in malocclusion that is not responsive to either traditional or compensatory orthodontic maneuvers alone (Abyholm et al. 1981). Chen et al. reported on horizontal maxillary growth in both children and adults of eastern Chinese ethnic background with unoperated and operated isolated cleft palate (Chen et al. 2009). Interestingly, the results of the unoperated mixed dentition individuals with ICP showed almost normal horizontal growth. The operated (repaired cleft palate) mixed dentition patients showed reduced length of both the maxilla and mandible and clockwise rotation of the maxillomandibular complex. Analysis of the permanent dentition groups showed reductions in maxillary length and reduced maxillary and mandibular horizontal projection. The authors concluded that for an individual born with ICP, the high incidence of maxillomandibular deficiency likely results from a combination of factors including the intrinsic primary cleft defect, secondary hypoplasia due to the surgical repair in infancy, and functional factors (e.g., effects of muscles of mastication, respiratory pattern, and mandibular rest posture (Canady et al. 1997)) (Fig. 25.5).
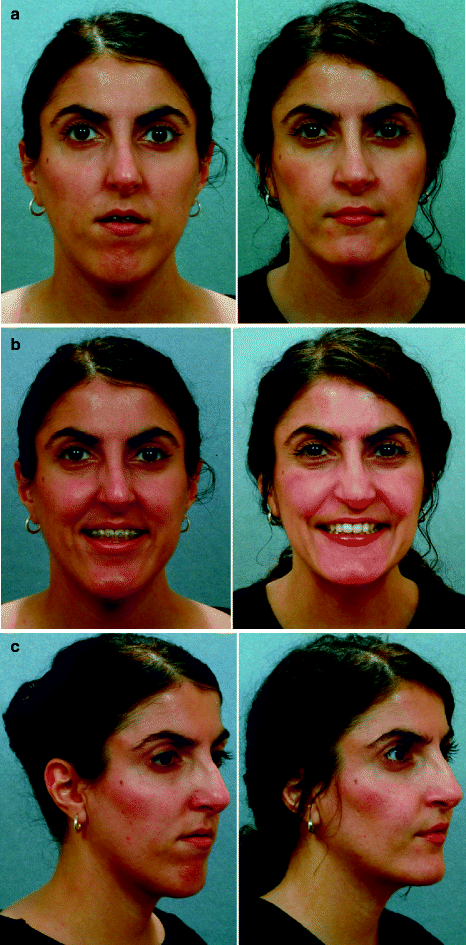
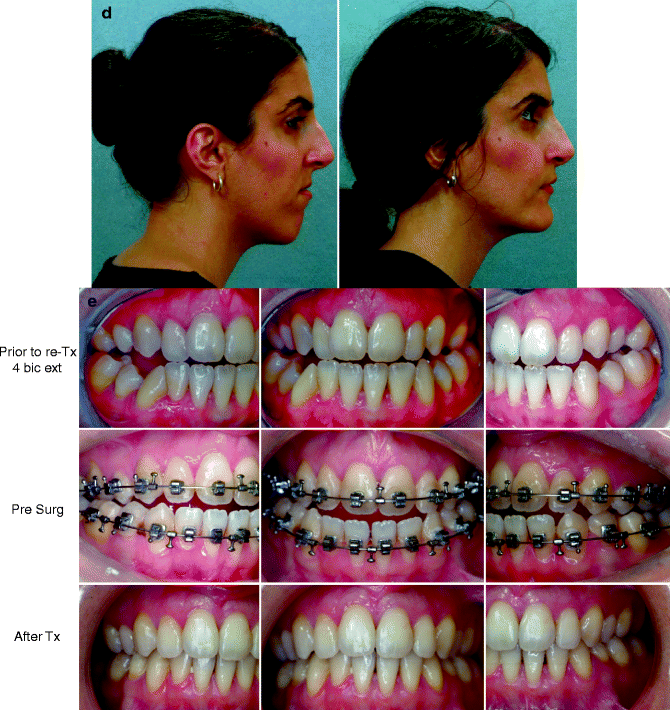
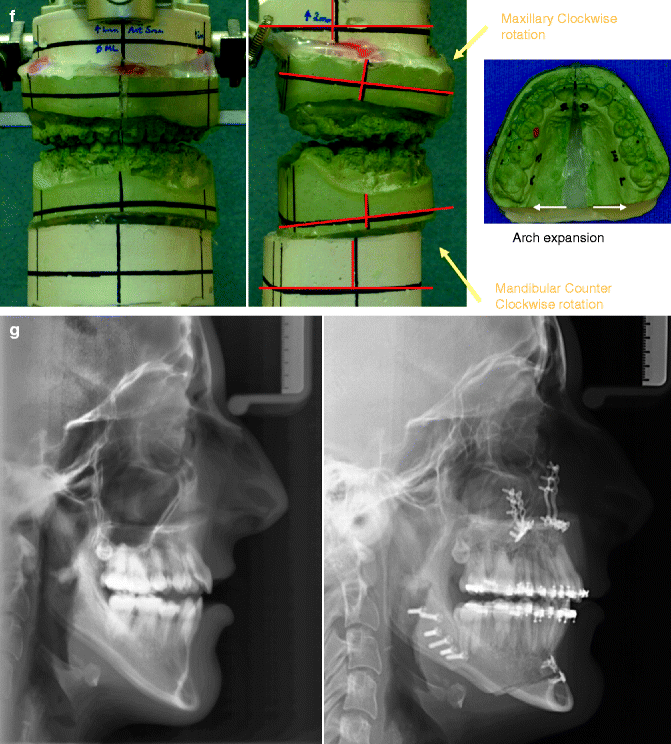



Fig. 25.5
A woman in her late 20s born with isolated cleft palate. She underwent palate repair in infancy. She developed a jaw deformity with malocclusion. Attempts to neutralize the occlusion included four bicuspid extractions and 6 years of growth modification and orthodontic mechanics (from age 11 to 17 years). She was left with generalized labial bone loss and gingival recession, especially of the lower anterior teeth. She presented to this surgeon as an adult with a lifelong history of obstructed nasal breathing and a long face growth pattern involving the maxilla, mandible, and chin region. There was excess lower anterior vertical height and horizontal retrusion (maxilla and mandible). She underwent evaluations including periodontics, prosthodontics, orthodontics, surgery, speech pathology, and ENT. Periodontal treatment and then orthodontic decompensation followed. Surgery includes LeFort I osteotomy (vertical shortening, clockwise rotation, horizontal advancement); bilateral sagittal split ramus osteotomies (horizontal advancement and counter clockwise rotation); osseous genioplasty (vertical shortening, horizontal advancement); and septoplasty/inferior turbinate reduction/recontouring of the nasal floor. (a) Frontal views in repose prior to and after reconstruction. (b) Frontal views with smile before and after reconstruction. (c) Oblique facial views before and after reconstruction (d) Profile views before and after reconstruction. (e) Occlusal views prior to re-treatment, after orthodontic decompensation and 1 year after reconstruction (f) Articulated dental casts after model planning. (g) Lateral cephalometric views before and after reconstruction
25.2 Coordinated Team Approach
Care of the cleft patient (i.e., UCLP, BCLP, and ICP) is best delivered by an integrated group of specialists who evaluate and provide definitive care (Berkowitz 1978; Kapp-Simon 1995; Leonard et al. 1991). It is no longer acceptable for individual practitioners (e.g., surgeons, orthodontists, restorative dentists, speech pathologists, or otolaryngologists) to carry out extended treatment without considering all aspects of the patient’s care and without discussing options with all members of the team (Cohen et al. 1995).
The need for coordinated and efficient cleft care was confirmed by the Eurocleft study which found a lack of association between “high-intensity disjointed treatment” and favorable results. The greater the number of operations and years of orthodontic appliances worn (heavy burden of care), the worst the clinical outcome for the patient (Hathaway et al. 2011; Shaw et al. 1992; Sinko et al. 2008; Tulloch 1993; Williams et al. 2001).
A frequent road block to successful reconstruction and dental rehabilitation of the midface-deficient adolescent born with a cleft is disagreement between clinicians about the indications, most effective surgical techniques, and timing for intervention. The surgeon, orthodontist, dental and medical team, patient, and family must first agree on the dental, occlusal, speech, upper airway, and aesthetic objectives. Only then can effective treatment go forward.
25.3 Treatment Protocol
Patients presenting with a cleft jaw deformity referred for possible orthognathic surgery are at a minimum seen by an orthodontist, orthognathic surgeon, otolaryngologist, and speech pathologist. Additional consultations are held with a prosthodontist, pediatrician/general dentist, periodontist, and other medical specialist (i.e., sleep specialist, geneticist), as indicated. For evaluation of the cleft dentofacial deformity, records and tests should include at a minimum medical-quality photographs with views of the face and occlusion, cephalometric and dental radiographs, dental models and a centric relation (CR) bite, direct facial measurements, nasoendoscopic speech and velopharyngeal assessment, and thorough evaluation of the upper airway.
The primary cleft surgeon not only performs repair of the cleft lip and palate and corrects velopharyngeal insufficiency when present but generally plays a role in directing the patient’s overall care. If a cleft surgeon is not trained in skeletal procedures, then a timely and seamless transition to the maxillofacial surgeon should occur. The maxillofacial surgeon caring for the cleft patient with a skeletal deformity should have a fundamental understanding of the patient’s dental, speech, upper airway, and aesthetic needs. He should request consultations with appropriate specialists, evaluate the clinical information, and be prepared to perform orthognathic and intranasal procedures.
The orthodontist provides appropriate interceptive treatment in the mixed dentition, identifies early abnormal skeletal growth patterns, and carries out definitive orthodontic treatment in conjunction with orthognathic surgery when indicated. From the mixed dentition phase, the cleft orthodontist should recognize the patient who may need orthognathic surgery. Instituting extensive camouflage (dental compensatory) treatment is likely to jeopardize periodontal health, lead to dental relapse, and may cause root resorption. Proceeding with a compromised (camouflage) orthodontic approach should only be entered into with full disclosure to the family and other treating clinicians.
Before orthognathic surgery, a speech pathologist experienced in cleft care performs an evaluation to characterize both velopharyngeal function and to identify articulation errors resulting from the cleft jaw deformity and dental malocclusion. A baseline evaluation is important because velopharyngeal function may deteriorate after maxillary advancement. A nasoendoscopic-guided speech assessment is preferred to provide maximum objective data without radiation exposure. Velopharyngeal (VP) closure that was adequate before surgery may become borderline afterward, and VP closure that was borderline may become inadequate. Studies document that only a small percentage of patients require a primary pharyngeal flap or flap revision after maxillary advancement. Articulatory distortions resulting from malocclusion are also identified by the speech pathologist, and cause-and-effect relationships determined. The successful orthodontic and surgical correction of crossbites, open bites, cleft-dental gaps, negative overjet, and residual oronasal fistulas represent the most effective way to correct the identified articulation distortions.
A thorough evaluation of the upper airway in a cleft patient with a jaw deformity is conducted by an otolaryngologist to assess for areas of obstruction. A formal sleep study (attended polysomnogram) is done if there is suggestion of obstructive sleep apnea (OSA). If indicated, simultaneous intranasal procedures including: septoplasty, reduction of the inferior turbinates, and recontouring of the nasal apertures, floor of the nose, and anterior nasal spine should be carried out at the time of orthognathic surgery.
Discussion between the treating medical and dental consultants and patient/family clarifies the need for and extent of orthognathic and intranasal procedures. The overall plan for speech, jaw, upper airway, dental rehabilitation, and the enhancement of facial aesthetics is agreed to prior to initiating treatment.
25.4 Timing of Orthognathic Surgery
Correction of the cleft jaw deformity is best carried out after skeletal maturity and prior to the individual’s finishing high school. Maxillofacial growth is generally complete between the ages of 14 and 16 years in girls and 16 and 18 years in boys. However, skeletal growth is variable and should be documented by knowledge of the pubertal growth spurt and/or sequential cephalometric radiographs taken at intervals. The patient/family’s preferences for timing of the operation based on psychosocial and functional needs (i.e., speech, swallowing, chewing, and breathing) are also taken into account.
25.5 Residual Deformities in the Adolescent Born with a Cleft
25.5.1 Unilateral Cleft Lip and Palate
Correction of residual skeletal, soft tissue, and dental deformities in the UCLP adolescent challenges the ingenuity and skill of the orthognathic surgeon and cleft team (Laspos et al. 1997a, b; Posnick 1997, 2000a, b, c, d, e; Posnick and Ricalde 2004; Posnick and Agnihotri 2011; Sandham and Murray 1993; Stoelinga et al. 1990; Tessier and Tulasne 1984; Turvey et al. 1996). The central deformity is maxillary hypoplasia, but it is often combined with residual oronasal fistula, bony defects, intranasal obstruction, soft tissue scarring, and velopharyngeal dysfunction. In addition, the maxillary lateral incisor at the cleft site is usually congenitally absent or deficient, resulting in cleft-dental gap (Cassolato et al. 2009; Robertsson and Mohlin 2000; Suzuki and Takahama 1992a, b). Secondary deformities of the nose, mandible, and chin region are also common. The prevalence of these residual clefting deformities in mature patients with UCLP varies widely depending on the primary cleft surgeon’s philosophy, available expertise (Nordquist and McNeill 1975), the individual’s intrinsic biologic growth potential, and the family/patient’s interest. Published clinical surveys of individuals born with complete UCLP and treated at established cleft centers indicate that despite best efforts, a number of children will not make themselves available for mixed dentition (prior to eruption of the cleft side canine) grafting (Felstead et al. 2010; McIntyre 2010). Also, some of those that do will fail grafting and require other means of reconstruction/dental rehabilitation. A subgroup of UCLP patients will present at or after adolescence with multiple cleft-related problems that may include:
1.
Maxillary hypoplasia
2.
Residual oronasal fistula
3.
Residual bony defects.
4.
Cleft-dental gap
5.
Chin dysplasia
6.
Mandibular dysplasia
7.
Nasal obstruction and sinus blockage.
8.
Velopharyngeal dysfunction.
25.5.2 Bilateral Cleft Lip and Palate
The adolescent patient with BCLP often has several residual deformities that can be challenging to manage (Posnick 1997, 2000a, b, c, d, e; Posnick and Ricalde 2004; Posnick and Agnihotri 2011; Stoelinga et al. 1990). The central deformity is maxillary hypoplasia, but it is often combined with residual oronasal fistula, bone defects, intranasal obstruction, soft tissue scarring, and velopharyngeal dysfunction. In addition, the maxillary lateral incisors are usually congenitally absent or hypoplastic (93 % of the time), and the patients often have cleft-dental gaps. Secondary deformities of the nose, mandible, and chin region are also common (Cassolato et al. 2009; Robertsson and Mohlin 2000; Suzuki and Takahama 1992a, b). The prevalence of these residual deformities in mature patients varies widely depending on the treating clinician’s philosophy, available expertise, the individual’s intrinsic biologic growth potential, and the family/patient’s interest/motivation. Published clinical studies indicate that a considerable number of children with BCLP will either not make themselves available for mixed dentition grafting or will fail the grafting procedure and require other means of reconstruction/dental rehabilitation (Felstead et al. 2010). For all of these reasons, a subgroup of BCLP individuals continues to present at or after adolescence with multiple cleft-related challenges that may include the following:
1.
Maxillary hypoplasia
2.
Residual oronasal fistula.
3.
Cleft-dental gap
4.
Residual bony defects
5.
Chin dysplasia
6.
Mandibular dysplasia
7.
Nasal obstruction and sinus blockage
8.
Velopharyngeal dysfunction
25.5.3 Isolated Cleft Palate
The ICP adolescent/adult referred for orthognathic evaluation will have an intact alveolar ridge and is generally with a full complement of teeth (Bell and Levy 1971; Posnick 1997, 2000a, b, c, d, e; Posnick and Ruiz 2000; Posnick and Ricalde 2004; Posnick and Agnihotri 2011; Stoelinga et al. 1987). They may, however, present with one or more of the following residual cleft-related problems:
1.
Maxillary dysplasia
2.
Residual oronasal (palatal) fistula
3.
Chin dysplasia
4.
Mandibular dysplasia
5.
Nasal obstruction and sinus blockage
6.
Velopharyngeal dysfunction
25.6 Orthodontic Considerations in a Cleft Patient with a Jaw Deformity
25.6.1 Unilateral Cleft Lip and Palate
The adolescent or adult UCLP patient that presents with maxillary hypoplasia and ineffective bone grafting will have two maxillary segments separated by a cleft. Each segment will have a varied degree of dysplasia in all three planes in space. From an orthodontic perspective, each segment is treated individually in anticipation of segmental repositioning. On the other hand, if the individual has undergone effective bone grafting in the mixed dentition, then the maxilla is in one unit and the arch form can be evaluated as an integrated unit.
There is great variability in the number of permanent incisors and the amount of alveolar bone in the anterior aspect of the UCLP maxilla. A lateral incisor-like tooth frequently is found along the edge of the cleft in the lateral segment. When a poorly formed lateral incisor is present, it should be extracted in the interest of long-term function and dental rehabilitation. Cassolato et al. have documented that in patients with complete UCLP, the lateral incisor on the cleft side is normal and maintained in only 7 % of cases.
The decision to extract the fully erupted normally formed tooth (i.e., first bicuspid) depends on the volume and height of available alveolar bone to house the dental roots adjacent to the cleft and the degree of overall dental crowding within the arch. It is preferred to extract a first bicuspid to ensure that there is adequate alveolar bone for leveling and aligning the retained teeth without irreversibly weakening the periodontal support of the teeth adjacent to the cleft and throughout the alveolus. Planning for extractions in the mandibular arch depends on alveolar space requirements and on tooth movements needed to position the incisors ideally over basal bone. Mandibular extractions are generally not required.
The potential disadvantage of closure of a cleft-dental gap (whether carried out orthodontically or surgically) is that it shifts the preoperative anterior dental gap (lateral incisor region) to a posttreatment posterior gap (second molar region). Articulated dental models with the maxilla (maxillary segments) in the proposed postoperative positions are analyzed preoperatively to confirm that the posterior maxillomandibular occlusion will be acceptable. For this reason, the maxillary second molar on the cleft side be orthodontically included in the arch form. Occasionally, there will be a nonimpacted (useful) maxillary wisdom tooth that can be incorporated to oppose the mandibular second molar.
25.6.2 Bilateral Cleft Lip and Palate
The patient who has not had an effective bone graft in the mixed dentition will have three separate maxillary segments, each with a degree of dysplasia in all three planes. If this is the case, each segment should be treated individually by the orthodontist in anticipation of segmental surgical repositioning. Radiographic analysis is essential before any orthodontic movement is initiated. A Panorex film is useful for assessing overall jaw and dental anatomy and tooth angulation. A cone beam CT scan is preferred to assess bone volume at each cleft site.
Both the number of permanent incisors and the amount of dentoalveolar bone in the premaxilla differ widely. Lateral incisor-like teeth are frequently found along the edges of the premaxilla of the lateral segments. These generally are rudimentary with poor root form and are best removed. An erupted supernumerary teeth should be extracted either at the time of bone grafting in the mixed dentition or prior to orthognathic surgery. A useful lateral incisor at the cleft site is only found in 7 % of patients and should be assessed according to root, not crown, morphology.
The decision to extract additional teeth (i.e., bicuspids) should depend on the width and height of available alveolar bone and degree of dental root crowding in the segments (arch). Extractions may be preferred to ensure that there is adequate bone for leveling and aligning teeth without irreversibly weakening the periodontal support of the dental roots next to the clefts. Incorporation of all erupted maxillary teeth including the second molars into the orthodontic mechanics will facilitate development of the desired postoperative arch form and occlusion. Extractions in the mandibular arch are generally not required, but this depends on space requirements and on the tooth movements needed to position the incisors ideally over basal bone.
25.6.3 Isolated Cleft Palate
The primary goal of presurgical orthodontic treatment in the teenager with an ICP jaw deformity is to eliminate all existing dental compensations. Instituting camouflage treatment is likely to jeopardize periodontal health, lead to dental relapse, and may cause resorption. The need to retract the upper incisors, upright the lower incisors, and eliminate crowding, spacing, and rotations are all important orthodontic considerations. The arch form objectives are to achieve a satisfactory occlusion at operation which can be detailed afterward. To eliminate dental compensations, extractions within the maxillary arch may be required. In the ICP patient, compared with the UCLP or BCLP patient, treatment is simplified as the alveolus is intact (no alveolar clefts), and there is generally a full complement of teeth.
25.7 Immediate Presurgical Reassessment
Two to six weeks before the planned operation, the orthodontist places passive surgical wires and confirms that the preoperative orthodontic objectives have been met. The surgeon takes final records including alginate impressions of the teeth, centric relation (CR) bite registration, facebow transfer, and direct facial measurements. Past medical and dental records (e.g., radiographs, reports, photographs, dental models, special studies) are reviewed. CT scan views of the cleft alveolus can be helpful to assess bone volume. Decisions are finalized concerning preferred vector changes (reposition) of the jaw(s) and the precise linear (mm) distances and angles to be accomplished in each jaw for the desired result. Model planning is carried out on the articulated dental casts, and splints are fabricated. The splints assist in achieving the precise occlusion and preferred facial aesthetics which have been decided on preoperatively.
25.8 Orthognathic Surgical Approach
25.8.1 Unilateral Cleft Lip and Palate
Historically, the literature warned of possible complications with maxillary osteotomy in patients with UCLP (Lanigan 1995). Only limited and confusing descriptions of techniques were provided to guide the orthognathic surgeon in the performance of safe, reliable osteotomies to solve these complex problems (Braun and Sotereanos 1980, 1981; Des Prez and Kiehn 1974; Fitzpatrick 1977; Freihofer 1977a, b; Georgiade 1974; Gillies and Rowe 1954; Gillies and Millard 1957; Jackson 1978; James and Brook 1985; Kiehn et al. 1968; Poole et al. 1986; Samman et al. 1994; Skoog 1965; Ward-Booth et al. 1984; Westbrook et al. 1983). As with other aspects of orthognathic surgery, Hugo Obwegeser’s milestone contributions to cleft skeletal reconstruction are important (Drommer 1986; Obwegeser 1966, 1967, 1969a, b, 1971, 2007; Obwegeser et al. 1985). By the late 1960s, he succeeded in advancing the cleft maxilla to the preferred location without the need for a compromised mandibular setback approach. Early on, Obwegeser gained experience to feel comfortable with cleft maxillary advancement of up to 20 mm. He realized that adequate mobilization of the down-fractured maxilla was the key step in advancing the jaw, whether cleft or noncleft. The success of this approach, as initially carried out by Obwegeser, was confirmed by Bell’s demonstration of the blood supply to these maxillary segments in animal studies (Bell and Levy 1971; Bell et al. 1995; Dodson et al. 1994; Dodson and Neuenschwander 1997). By the mid-1980s, Posnick utilized and refined Obwegeser’s techniques of LeFort I osteotomy for treatment of the UCLP deformity (Braun 1992; Posnick 1991a, b, 1996; Posnick et al. 1994; Posnick and Tompson 1992). A key aspect was to use Obwegeser’s circumvestibular incision which permitted direct exposure for dissection, osteotomies, disimpaction, fistula closure, septoplasty, inferior turbinate reduction, piriform aperture recontouring, bone grafting, and application of plate and screw fixation. This was consistently found to be a reliable approach without significant risk of circulation injury to the greater or lesser dento-osseous-musculomucosal segments (flaps). The visibility provided by the circumvestibular incision made possible the incorporation of routine closure of the cleft-dental gap through differential maxillary segmental repositioning without necrosis of bone or loss of teeth. This method also closes the cleft dead space and brings together the labial and palatal flaps without need for subperiosteal undermining which permits closure of recalcitrant oronasal fistulas without tension and the establishment of periodontal health to the cleft-adjacent teeth (Fig. 25.6).
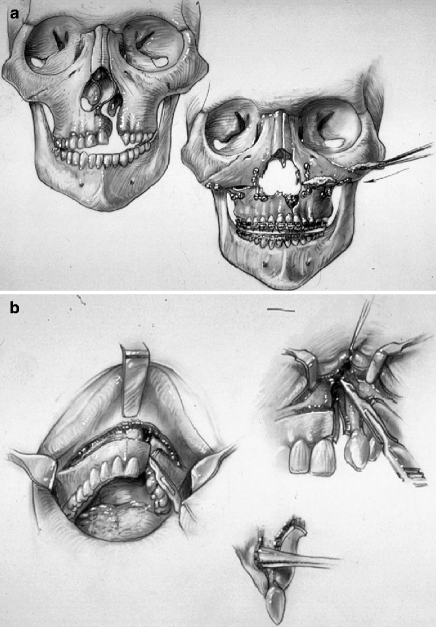
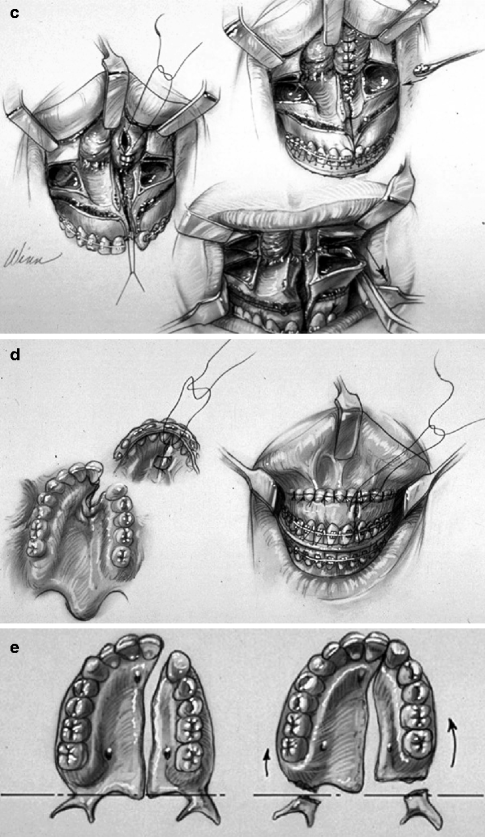


Fig. 25.6
Illustrations of modified LeFort I osteotomy in two segments as carried out in a patient with UCLP who has not undergone successful bone grafting in the mixed dentition. (a) Frontal view of maxillofacial skeleton before and just after LeFort I osteotomy in two segments. The inferior turbinates have been reduced, and a submucous resection of the deviated septum has been performed. The nasal floor has been recontoured with a rotary drill. Cancellous Iliac bone graft has also been placed along the nasal floor. Corticocancellous (iliac) graft is also placed in gaps along the anterior maxilla on each side. (b) Illustration of circumvestibular and perifistula incisions for exposure to complete osteotomies and later fistula closure (c) Illustration of down-fractured LeFort I osteotomy in two segments after submucous resection of septum, reduction of inferior turbinate through the nasal mucosa opening, and watertight nasal-side closure. (d) Illustration indicating wound closure after differential segmental repositioning. (e) Palatal view of bony segments before and after repositioning (From Posnick 1991b)
The extent of maxillary advancement carried out by the surgeon is based on the preferred occlusion, airway needs, and facial aesthetics determined preoperatively. The ideal vertical dimension is also achieved intraoperatively based on the preoperative plan. The maxillary osteotomy sites are fixed in place with titanium plates and screws at each zygomatic buttress and piriform aperture according to the principles originally described by Luhr (Champy 1980; Luhr 1968, 1981). An additional microplate is applied to stabilize each interpositional corticocancellous (iliac) graft. Mandibular and chin osteotomies to correct secondary deformities and facial asymmetries are also frequently required to achieve objectives (Fig. 25.1).
25.8.2 Bilateral Cleft Lip and Palate
Surgical attempts to correct the jaw disharmony seen in patients with BCLP date back to Steinkamm’s descriptions in 1938 (Steinkamm 1938). The early literature mostly warned of possible complications with maxillary osteotomy in patients with BCLP and offered only incomplete descriptions of surgical techniques to guide the surgeon in performing safe and reliable osteotomies (Fitzpatrick 1977; Sinn 1980; Gillies and Rowe 1954; Gillies and Millard 1957; Jackson 1978; Poole et al. 1986; Ward-Booth et al. 1984). Hugo Obwegeser’s early milestone contributions to cleft skeletal reconstruction are important (Drommer 1986; Obwegeser 1966, 1967, 1969a, b, 1971, 2007; Obwegeser et al. 1985). Unfortunately, in the early days, very few clinicians shared his enthusiasm. In 1974, Willmar reported on the complications associated with LeFort I osteotomy in BCLP patients (Willmar 1974). Of the eight patients he treated, one died of airway complications, and the results on the others were not reported favorably. By the mid-1980s, Posnick clarified the safety of the segmental LeFort I osteotomy technique in patients with a BCLP jaw deformity (Fig. 25.7) (Posnick 1996, 2000a, b, c, d, e; Posnick and Tompson 1993; Posnick et al. 1994). The documented favorable results confirmed the importance of following sound biologic principles. For example, preservation of the labial soft-tissue mucosal pedicle to the premaxilla in the unsuccessfully grafted BCLP maxilla is essential. The validity of this flap circulation was proven by Bell et al. in rhesus monkeys (Bell and Levy 1971; Bell et al. 1995).
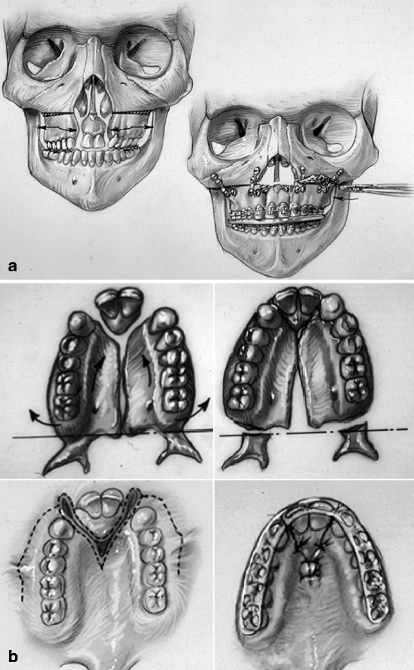
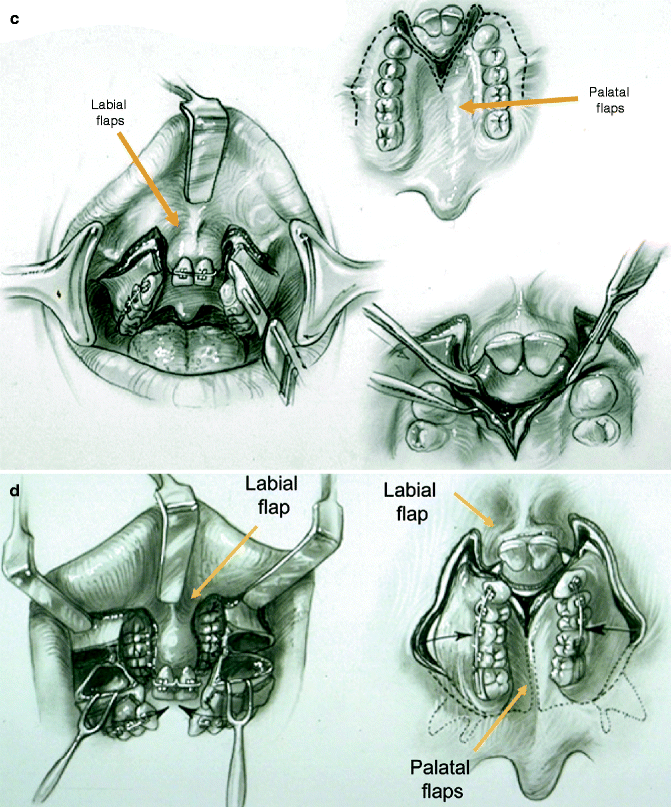
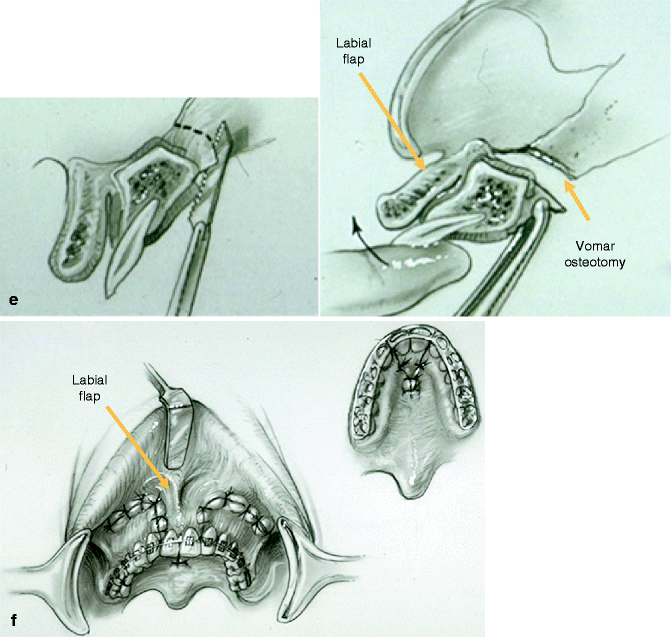



Fig. 25.7
Illustrations of modified LeFort I osteotomy in three segments. This is, as carried out in a patient with BCLP who has not undergone successful bone grafting in the mixed dentition. (a) Illustrations of a patient with BCLP before and after three-part maxillary osteotomies with repositioning of the segments. Septoplasty, inferior turbinate reduction, and recontouring of the nasal floor are also shown. (b) Palatal views of bone segments before and after repositioning for closure of cleft-dental gaps. Both skeletal and soft tissue views are shown (c) Illustrations of incisions for modified LeFort I in three segments. (d) Illustrations of down-fractured lateral segments demonstrating exposure for nasal-side closure of oronasal fistula (e) Illustration of premaxillary osteotomy carried out on palate side (vomer osteotomy) using a reciprocating saw. (f) Illustration demonstrating oral wounds sutured at end of procedure. (From Posnick 1991b)
The BCLP patient with an intact (successfully grafted) alveolar ridge on one side essentially presents to the surgeon with the same anatomy as a nongrafted UCLP patient. The surgical approach to the maxilla for this patient is the same as described for the nongrafted UCLP patient. For the BCLP patient presenting with a “three-segment” maxillary deformity, the modified LeFort I osteotomy (in three segments) should be used. For the BCLP adolescent presenting with an intact (successfully grafted) alveolar ridge on each side, a standard LeFort I down fracture is carried out (Fig. 25.4).
25.8.3 Isolated Cleft Palate
In general, the primary jaw deformity observed in the ICP adolescent is maxillary hypoplasia/dysplasia resulting from the original cleft deformity and the subsequent surgical interventions. The usual reconstructive procedure to consider is a standard LeFort I maxillary osteotomy. Early on, Obwegeser clarified that full mobilization of the down-fractured maxilla was essential to achieving an orthognathic correction on the operating room table and to limit skeletal relapse over time. Bell and others validated that the Obwegeser LeFort I technique allowed adequate blood supply for routine satisfactory bone healing without aseptic necrosis or dental injury (Fig. 25.5).
Any residual palatal oronasal fistula in the ICP patient at the time of orthognathic correction will be difficult to close simultaneously with the LeFort I procedure. This is because elevation of palatal flaps is generally required to do so and this would compromise the blood supply to the down-fractured maxilla. Interestingly, if a watertight nasal-side closure can be achieved through the down-fracture prior to fixing the maxilla in its new location, then the residual palatal-side mucosal separation will frequently heal by secondary intention with fistula closure.
25.9 Clinical Management After Initial Surgical Healing
Managing details of the in-hospital and at-home convalescence during initial healing are essential for a successful outcome. The surgeon is responsible for seeing the patient through this phase of treatment. Cephalometric and dental radiographs and facial and occlusal photographs are obtained at standard postoperative intervals for documentation.
Orthodontic maintenance of the surgical result and detailing of the occlusion are initiated after initial healing (5 weeks after surgery). The seamless transition from the surgeon to the orthodontist for ongoing care is essential.
Speech and VP function can be objectively reassessed 6 months after surgery, and any remaining issues can be addressed at that time. We prefer to evaluate VP function using nasoendoscopic instrumentation when feasible. Further cleft soft tissue procedures (e.g., cleft rhinoplasty, lip scar revision, pharyngeal flap/flap revision, closure of residual palatal fistula) can be carried out as early as 6 months after orthognathic surgery. Once the orthodontic appliances are removed, any planned definitive restorative dental work can also be finalized.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


