Factors
Examples
Genetically determined
Amelogenesis imperfecta [3]
Chromosomal anomalies
Down syndrome
Congenital defects
Cardiac defects, unilateral facial hypoplasia or hypertrophy [2]
Inborn errors of metabolism
Galactosemia, phenylketonuria, alkaptonuria, erythropoietic porphyria, primary hyperoxaluria
Neonatal disturbances
Prematurity, hypokalemia
Infectious diseases
Measles, chickenpox
Neurological disturbances
Chronic medical diseases
Hepatic disease, endocrinopathies, renal disease, enteropathies
Maternal health during pregnancy
Hypertension, nutritional deficiency, substance abuse
Nutritional deficiencies
Vit. D deficiency
Unlike genetically determined defects, the effect of developmental factors on enamel formation depends upon the timing, duration, and severity of these factors and is usually referred to as chronological hypoplasia/hypomineralization (Fig. 10.1). For these factors to affect the formation of enamel in primary teeth, they will occur during hard tissue formation of the primary teeth. This starts with central incisor formation at 13–16 weeks after fertilization and ends with the second primary molars at 8–11 months of age [4]. The type of resulting defect will reflect whether the insult occurred during enamel matrix formation (leading to hypoplasia), mineralization (causing hypocalcification defects), or during maturation phase (causing hypomaturation defects). A clinician is likely to encounter two main types of enamel defects: hypoplastic and hypomineralized enamel. Hypoplastic enamel [4, 5] (Fig. 10.2) is caused by incomplete or defective formation of the organic enamel matrix by ameloblasts during tooth formation (secretory stage) resulting in thinner but normally mineralized enamel. Hypomineralization occurs due to a failure in enamel matrix mineralization [4, 5]. This is further divided into hypocalcification (defective mineralization) or hypomaturation (defective removal of proteins from enamel matrix preventing maturation). Clinically, hypocalcified enamel is usually yellow-brown in color with more potential for enamel breakdown, while hypomature enamel may appear normal, mottled, or slightly opaque [4, 5].
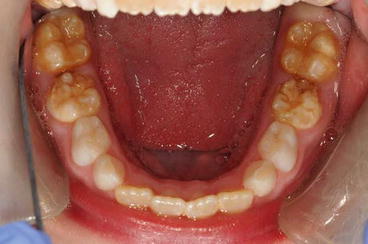
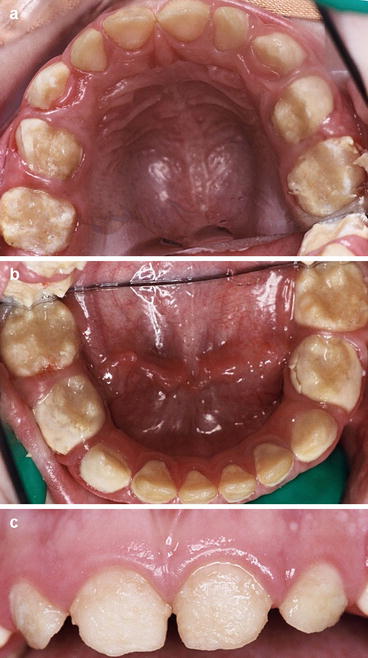

Fig. 10.1
Chronological hypoplasia affecting the lower second primary molars and chronological hypomineralization affecting lower first permanent molars

Fig. 10.2
(a–c) Preoperative images of a 3-year-old child with a hypoplastic form of AI. Note the buildup of calculus associated with the lower primary molars (Courtesy of Nicky Kilpatrick)
Management of DDE in Primary Teeth
The management of enamel defects in generalized conditions or where they are likely to affect the permanent dentition is challenging and usually requires immediate-, short- and long-term planning [6]. Patients with amelogenesis imperfecta (AI), for instance, may have other associated anomalies such as disturbances in eruption, anterior open bite, pulpal calcifications, pathological root or crown resorption, and/ or taurodontism. These anomalies affect the long-term management and usually require an interdisciplinary approach starting in the later primary/early mixed dentition. Patients with primary teeth defects often present at a young age and the parents want immediate treatment to improve the child’s appearance. However, it is important to make a treatment plan which will encompass a stepwise approach that includes a short-, medium-, and a long-term treatment plan. Children with DDE often require several interventions throughout their primary, mixed, and permanent dentition stages [7], and should general anesthesia (GA) be required, it is crucial to plan and provide the necessary management in a timely manner so that the least number of GAs are required throughout the child’s life.
The aims of management, especially at the primary dentition stage, include:
1.
Prevention and maintenance of good oral hygiene
2.
Desensitization and pain management of affected teeth
3.
Restorative management (esthetic management and stabilization of affected teeth)
4.
Behavior management to help children manage the dental care they need
Prevention
The gingival condition and oral hygiene of patients with both generalized defects, such as in AI or isolated defects, are often poor. Figures 10.1 and 10.3 show the presence of calculus in children with hypoplastic and hypomineralized AI. This occurs because many of the teeth are sensitive to thermal and toothbrush stimuli, which prohibits effective toothbrushing. Having enamel defects can also be an additional caries risk factor as the teeth are rough and porous with softer and/or thinner enamel. Therefore, treatment planning should firstly focus on prevention including effective oral hygiene instruction using warm water and very soft brushes, optimizing fluoride exposure both at home and with regular professional application, diet advice and sealants, or temporary restorations where appropriate. A guide is given in the UK Department of Health and British Association for the Study of Community Dentistry toolkit [8]. Comprehensive dietary analysis and advice is essential from both a caries and tooth surface-loss perspective. This will involve identifying fermentable carbohydrates and acidic foods and beverages in the diet and advising on their reduction and timing of use to minimize damage.
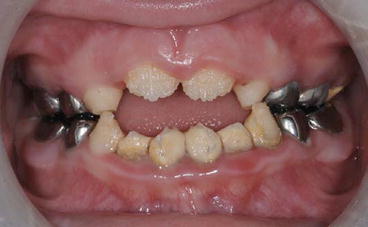

Fig. 10.3
Anterior view of the mixed dentition in a child with AI showing poor oral hygiene, calculus deposits, and gingivitis
It is unrealistic to expect children with DDE to dramatically improve their oral hygiene without some intervention to reduce the sensitivity of the teeth. This might include the use of preventive agents such as topical fluorides or calcium phosphate-containing products or by placing interim restorations (glass ionomer cements or compomers) that will seal the dentine, thereby allowing the child to brush the affected teeth with less discomfort. In younger children, below 6 years-of-age, parents should help with brushing twice daily and should carry out regular flossing if the contact areas are closed.
Reducing Sensitivity
Several strategies are available for the treatment of the sensitivity associated with DDE, although none have been found to be reliable for every case (see Chap. 9). It is important to consider desensitization in order to reduce the discomfort felt by many children with DDE. This sensitivity also makes restorative interventions, especially with adhesive materials, even more challenging. Some of the suggested methods for desensitization include the use of topical fluoride preparations, in particular fluoride varnishes, such as Duraphat® 22,600 ppm F (Colgate Oral Care) or 3M Espe Fluoride Varnish with tricalcium phosphate. Care should be taken to use the recommended amounts on erupting teeth with DDE in preschool-aged children. More recently a combination of casein phosphopeptide and amorphous calcium phosphate (CPP-ACP – GC Tooth Mousse/MI Paste) with and without fluoride has also been advocated to help decrease sensitivity. CPP-ACP helps create, stabilize, and deposit a supersaturated solution of calcium and phosphate at the enamel surface. Therefore, it has been suggested that home application of a CPP-ACP-containing cream especially when combined with fluoride use will help remineralize and desensitize by acting as a source of bioavailable calcium and phosphate. Other topical fluorides may also be useful; among these are stannous fluoride gels, such as Gel-Kam® 1,000 ppm F (Colgate Oral Care) or OMNI Gel 0.4 %/1,000 ppm F (3M). There has also been a suggestion that desensitizing toothpastes may help with some hypomineralized teeth. Currently there is no strong evidence to support the efficacy of these strategies in the management of DDE, though all these products may help reduce sensitivity and enhance mineralization of the hypomineralized areas. However, none of the available products are always effective, and clinicians should consider using products in combination or trying different products in an attempt to alleviate the symptoms in patients.
Pain and Anxiety Management
Pain management in children is an integral part of good pediatric dentistry. Both the technique and choice of local analgesia are important for the provision of high quality, effective restorations in children, particularly if they are to last for the lifetime of the primary teeth (up to 8 years). In particular, teeth that have DDE are more likely to be sensitive and consequently providing effective analgesia is often more difficult than for unaffected teeth.
Behavior Management
Clinicians should evaluate the understanding and coping skills of the child with DDE when the teeth require intervention. One of the commonly encountered problems is that children with DDE present with higher levels of anxiety. This is especially true in cases where the defect is associated with sensitivity or where previous treatment has been attempted without appropriate pain control or behavior management. If such defects are suspected, especially when associated with sensitivity, it is important not to air-dry these teeth during examination but to dry them gently with a cotton pellet. Managing young children requires empathy and some knowledge of behavior management techniques for children. Many pediatric dentistry textbooks cover useful techniques for helping children cope with restorative care. In the center of all the techniques is “tell, show, and do” which will allow most children to be able to cooperate for restorative care when it is presented in age-appropriate language and demonstration. This of course takes a little extra time but is time well spent in preparing a child for more complex care as they grow older.
Local Analgesia
For children who have been sensitized to previous invasive dental treatment, in particular local analgesia, the use of computer-controlled anesthesia (such as the Wand and the Wand STA – controlled dental anesthesia, Dental Practice Systems, Welwyn, Herts, UK) can be an excellent way to administer local analgesia. The Wand provides several advantages over conventional syringes including the fact that it does not look like a conventional syringe; the fine bevel of the needle and the slow speed with which the local analgesic solution can be administered make it a simple way to deliver painless local analgesia. The use of 4 % articaine should be considered in managing older children especially where there is a history of failed local analgesia. For children over 4 years-of-age who are extremely wary of local analgesia, infiltration with 4 % articaine in the lower arch as opposed to an inferior dental block may provide adequate analgesia for restorations to be placed [9]. It is also important to make use of topical anesthesia. The preemptive use of systemic analgesics (in accordance with local guidelines) can also be an effective way of helping children cope with care successfully [10].
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


