Pink Aesthetics
Brian Chee
Principles
To achieve a natural appearance, the peri-implant soft tissues should closely mimic those of the adjacent dentition. Several key features have been highlighted, including papilla height and the position of the mucosal margin, as well as the texture, colour and contour of the peri-implant mucosa.1–3
Gingival Biotype
Gingival thickness can be broadly categorised into either thin or thick biotype. The thin gingival biotype has been associated with long-narrow teeth and a highly scalloped gingival margin, whereas the thick biotype is associated with short-wide teeth and a flat, low-scalloped gingival margin.4
Appreciation of the gingival biotype is important, since it can influence the aesthetic risk and complexity of treatment. The thick gingival biotype represents robust tissues with a lower risk of mucosal recession. In contrast, a thin gingival biotype is more susceptible to surgical trauma due to reduced vascularisation. This can lead to a greater risk of recession and aesthetic failure.5–7
Papilla
The re-creation of papilla-like tissue is one of the most challenging goals of implant therapy in the aesthetic zone. The principal factor determining the presence of a papilla is the distance of the bone crest to the proximal contact point. A seminal study by Tarnow et al.8 found that when the distance from the contact point to the crestal bone was 5 mm or less, the papilla between teeth was present nearly 100% of the time. However, when this distance was increased to 6 mm and 7 mm, the papilla was only present 56% and 27% of the time, respectively. Similarly, the regeneration of papillae adjacent to single implants is not predictable when the distance from bone crest to contact point is above 5 mm.9 Moreover, the papilla level associated with single-implant restorations is related to the bone crest at the adjacent teeth and is independent of the bone level at the implant.9, 10 A minimum safe lateral distance of 1.5 mm has been suggested to preserve the papilla, as positioning the implant too close to the adjacent tooth can result in loss of the proximal bone.11 Recent studies suggest that a greater potential for complete papilla fill may be achieved if the distance from the adjacent teeth is increased to 3 mm or more.12–14 However, this minimum distance may be less important when using implants with a platform-switched design.15
Even though spontaneous improvement in papilla fill has been observed adjacent to single-implant restorations,1, 14 this is rarely achieved between multiple adjacent implants. Findings by Tarnow et al.16 suggest that a mean soft-tissue height of 3.4 mm can be expected to cover the crestal bone between two implants. Due to this deficiency in papilla height, it may be necessary to modify the shape of the teeth to provide a longer contact areas and smaller embrasure space.17 With severe deficiencies, the papilla can be re-created prosthetically with pink porcelain (Figure 11.6.1), acrylic or composite resin.
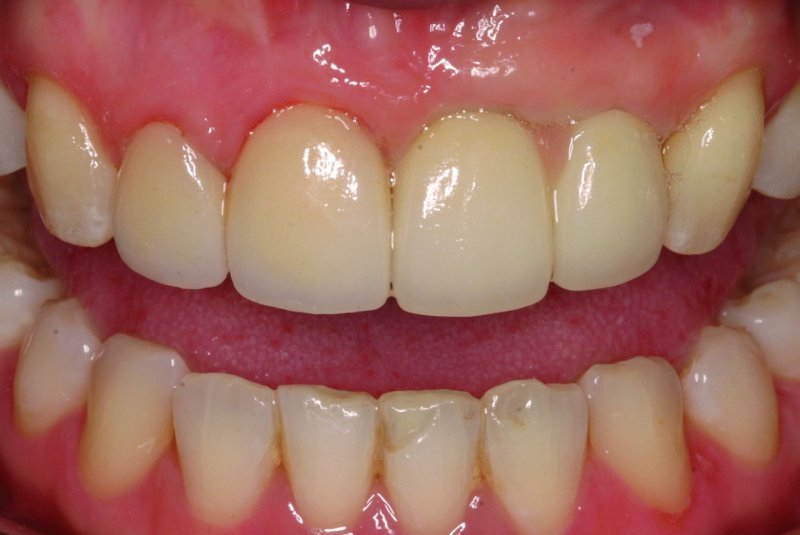
Figure 11.6.1 Pink porcelain between two dental implants in upper left central and lateral incisor to simulate missing papilla. Meticulous attention to oral hygiene is required to maintain the gingival health for this area. Source: Christopher C.K. Ho, BDS MClinDent Prosthodontics. Reproduced with permission from Christopher C.K. Ho.
Implant Position
Incorrect implant position is a major cause of aesthetic failure due to peri-implant soft-tissue defects.18
Apico-coronal Position
Observations in histological studies have confirmed that a consistent soft-tissue dimension occurs at implants similar to the biologic width associated with teeth.19, 20 Furthermore, the bone resorption associated with development of the biologic width is greater if the implant–abutment interface is placed below the bone crest.21, 22 This will also be influenced by the type of connection between the implant and the abutment. Deeper placement can lead to excessive bone remodelling with subsequent recession, short papillae and long clinical crowns, particularly when there is a compromise in the bacterial seal between the implant and abutment connection. The ideal shoulder position for implants in the aesthetic zone should be approximately 3 mm apical to the planned restoration margin.
Mesio-distal Position
Placement of the implant too close to the adjacent tooth can also result in loss of crestal bone to the level of the implant.11 Additionally, the horizontal component of the biologic width means that a minimum distance of 3 mm is required between implants to prevent additional interproximal bone loss.23
Bucco-lingual Position
Buser et al.18 recommend that the implant shoulder is positioned 1–2 mm lingual to the emergence of the adjacent teeth. Implants positioned too buccally are associated with mid-buccal recession and aesthetic failure (Figure 11.6.2).7
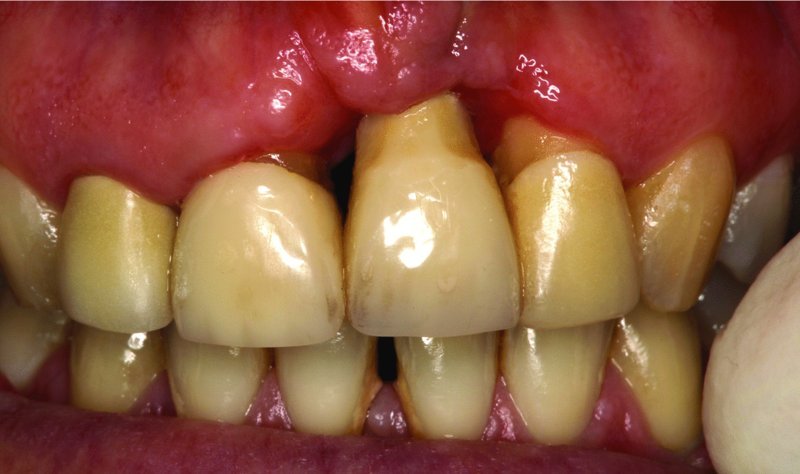
Figure 11.6.2 Implant placed in extreme buccal position leading to severe recession and an aesthetic disaster
Procedures
Papilla reconstruction and recession coverage procedures for implants are currently unpredictable.24 A strong emphasis should therefore be placed on the prevention of soft-tissue defects at implants in the aesthetic zone. Several key principles can be applied in order to reduce the risk of these complications:
- Appropriate flap design, atraumatic handling of the soft tissues and tension-free primary wound closure
- Selection of an appropriate post-extraction timing protocol according to individual aesthetic risk
- Implant placement in the correct prosthetically driven position
- Buccal bone augmentation for long-term tissue stability and prevention of mid-buccal recession
- Consider soft tissue augmentation for patients with a thin biotype
- Support and conditioning of the peri-implant soft tissues prior to definitive restorations.
Flap Design and Wound Closure
Selection of an appropriate flap design and careful handling of the soft tissues are essential in achieving aesthetic wound healing. Flap design should allow good visualisation and access to the bony architecture, while keeping disruption of the blood supply and visible scarring to a minimum.25 Additionally, there should be adequate mobilisation of the flap to allow passive closure over augmented sites. The following principles can be applied to flap design and manipulation:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


