Tongue thrusting and mouth breathing may also play a part in the creation of a malocclusion. An anterior open bite is the most common dental problem associated with the anomalies.
12. Describe intervention therapy for non-nutritional sucking habits.
1. Ideally, the patient should understand the problem and want to correct it.
2. The timing of intervention is controversial. Some authors suggest that therapy should begin around age 4 years to prevent irreversible changes, whereas others suggest waiting until the patient is about 6 to 7 years old to ensure that he or she can understand the intent of therapy.
3. Patients who decide to accept appliance therapy should have support and encouragement from their parents to help them during treatment.
4. The dentist should know the patient well to provide intervention and advice at the correct time.
5. The dentist should be able to evaluate the deformity and extent of its effects so that it can be treated in the best possible manner.
13. What is the current schedule of systemic fluoride supplementation?
See Table 10-1.
14. Summarize the scientific basis for the use of fluoride varnishes in caries management.
1. When used appropriately, varnishes offer a 40% to 65% reduction in the incidence of caries, with a 36% reduction in fissured caries and a 66% reduction in nonfissured surfaces.
2. Varnish results in a 51% reversal of decalcified tooth structure and a reduction in enamel demineralization of 21% to 35%.
3. Varnish application is effective in arresting and reversing active enamel lesions, reducing the need for restorative treatment.
4. Varnishes are as effective as acidulated phosphate fluoride gels in controlling approximal caries.
5. In primary teeth of preschool children, varnishes result in a 44% reduction in caries.
15. Is prenatal fluoride supplementation effective in decreasing caries rates in the primary dentition?
No. No studies to date support the administration of prenatal fluorides to protect the primary dentition against caries.
16. Do home water filtration units have any effect on fluoride content?
Absolutely. For example, reverse osmosis home filtration systems remove 84%, distillation units remove 99%, and carbon filtration systems remove 81% of the fluoride from water.
17. Why has the prevalence of fluorosis increased in the United States?
The increased prevalence is likely because of three factors: (1) inappropriate fluoride supplementation; (2) ingestion of fluoridated toothpaste (most children <5 years ingest all the toothpaste placed on the toothbrush); and (3) high fluoride content of bottled juices. For example, white grape juice may have a fluoride concentration greater than 2 ppm.
18. What are the common signs of acute fluoride toxicity?
Acute fluoride toxicity may result in nausea, vomiting, hypersalivation, abdominal pain, and diarrhea.
19. What is the first step in treating a child who has ingested an amount of fluoride greater than the safely tolerated dose?
In acute toxicity, the goal is to minimize the amount of fluoride absorbed. Therefore, syrup of ipecac is administered to induce vomiting. Calcium-binding products, such as milk or milk of magnesia, decrease the acidity of the stomach, forming insoluble complexes with the fluoride and thereby decreasing its absorption.
20. Are children born with Streptococcus mutans?
Children are not born with Streptococcus mutans. Instead, they acquire this caries-causing organism between the ages of about 1 and 3 years. Mothers tend to be the major source of infection. The well-delineated age range of acquisition is referred to as the window of infectivity.
Transmission of S. mutans may be vertical (e.g., from caregiver to child) or horizontal (e.g., between siblings). Transmission may be decreased by reducing habits such as sharing utensils or foods. Additonally, several studies have demonstrated decreasing maternal levels of S. mutans decreases the transmission rate to the child.
21. What variable is the best predictor of caries risk in children?
Past caries rates are the single best predictor in assessing a child’s future risk.
22. Is milk a contributing factor to early childhood caries?
Several animal and in vitro studies have suggested that milk and milk components are not cariogenic. Similarly, human breast milk by itself does not cause demineralization. However, when mixed with a sucrose-containing substance, cow’s milk and human breast milk promote caries.
23. What food components reduce the caries-inducing effects of carbohydrates?
Phosphates, fats, and cheese decrease caries susceptibility. Phosphates apparently have a topical effect that aids in remineralization and improves the structural integrity of the enamel surface. Although the mechanism is not entirely clear, fats may form a protective barrier on the teeth or coat the carbohydrate. Cheese may contribute through a number of mechanisms, including its fat, phosphorus, and calcium content.
24. Is there any dental health benefit to chewing gum?
One study found that children of mothers who chewed sugar-free gum sweetened with xylitol (in addition to normal oral hygiene measures) had 70% less dental decay than children of mothers who did not chew the gum.
25. Summarize the mechanisms of xylitol’s effect.
• Xylitol has a five-carbon chemical structure not recognized by oral bacteria.
• Because it is not fermented, no acid production results, and pH levels in the mouth do not decrease (see question 27).
• Chewing xylitol-sweetened gum promotes stimulation of salivary flow, which in turn helps rinse away excessive sucrose residues and neutralize acids from other foods. In addition, saliva contains calcium and phosphate, which promote remineralization of early caries.
• Xylitol is a polyol that inhibits the growth of S. mutans, thereby reducing caries susceptibility. Continued use helps reduce the number of virulent bacteria in the plaque, although xylitol is not bactericidal.
• Xylitol reduces plaque in the oral cavity and enhances the proportion of soluble to insoluble polysaccharides.
• Xylitol complements fluoride in the oral cavity.
26. Who throws a meaner curve, Ryan or Stephan?
Undoubtedly Stephan! The Stephan curve describes the decrease in pH that occurs following a cariogenic challenge. Hall of Fame pitcher Nolan Ryan, on the other hand, is best remembered for his fast ball, although did have a pretty good curve.
27. What is meant by critical pH?
Critical pH is the pH (∼5.5) at which enamel is demineralized.
28. What is the Vipeholm Study? What did it demonstrate?
In the Vipeholm Study (1954), adult institutionalized patients were followed for several years on a variety of controlled diets. The following results were reported:
• Caries increased significantly when sucrose-containing foods were ingested between meals.
• Sucrose in a retentive form produced more caries than forms that were rapidly cleared from the mouth.
• Sucrose consumed with meals was the least detrimental form.
• Caries activity differs among people with the same diet.
29. Why does this CAT not have your tongue?
CAT stands for the Caries Risk Assessment Tool developed by the AAPD to aid in assessing a child’s risk of caries (Table 10-2). Recommendations based on their guidelines are as follows:
1. Dental caries risk assessment, based on a child’s age, biologic and protective factors, and clinical findings, should be a routine component of new and periodic examinations by oral health and medical providers.
2. There is not enough information at present to carry out quantitative caries risk assessment analyses. However, estimating children at low, moderate, and high caries risk via a preponderance of risk and protective factors will enable a more evidence-based approach to medical provider referrals, as well as establish periodicity and intensity of diagnostic, preventive, and restorative services.
3. Clinical management protocols, based on a child’s age, caries risk, and level of patient and parent cooperation, provide health providers with criteria and protocols for determining the types and frequency of diagnostic, preventive, and restorative care for patient-specific management of dental caries.
30. Why might children with asthma be at higher risk of developing dental caries?
The two major classes of medications used to treat asthma are anti-inflammatory agents (e.g., corticosteroids, cromolyn sodium) and bronchodilators (beta-adrenergic agonists, such as ventolin and albuterol). Over the years, numerous studies have shown that all these medications can impair salivary function, causing xerostomia (dry mouth) and thus potentially increasing susceptibility to caries. Evidence suggests that children with asthma may have double the risk of caries in their primary and permanent dentition. Therefore, it is important to implement appropriate preventive measures in asthmatic patients, such as routine fluoride application and giving extra attention to oral hygiene.
31. What is the earliest macroscopic evidence of dental caries on a smooth enamel surface?
A white spot lesion results from acid dissolution of the enamel surface, giving it a chalky white appearance. Optimal exposure to topical fluorides may result in the remineralization of such lesions.
32. Which teeth are often spared in nursing caries?
The mandibular incisors often remain caries-free as a result of protection by the tongue.
33. Does an explorer stick necessarily indicate the presence of caries?
Several studies have demonstrated that an explorer stick may often be caused by the anatomy of the pit and fissure and not the presence of caries (poor sensitivity). However, the lack of a stick is a good indication of lack of caries (good specificity). It has been suggested that sharp eyes are more important than sharp explorers in detecting pit and fissure caries.
34. What are the indications for an indirect pulp cap in the primary dentition?
An indirect pulp cap is indicated in a deep carious lesion approximating the pulp but without signs or symptoms of pulp degeneration. Long-term studies have indicated a higher success rate for indirect pulp caps compared to pulpotomies.
Calcium hydroxide is a commonly used medication that is applied to the dentin, followed by a restorative material that provides a complete seal.
35. What are the indications for a direct pulp cap?
A direct pulp cap maybe indicated when there is a small mechanical or traumatic exposure of the pulp. Materials commonly used include calcium hydroxide, glass ionomer and, more recently, mineral trioxide aggregate (MTA). According to one study, successful outcomes are inversely related to the amount of bleeding.
Table 10-2
Caries Risk Assessment Tool (CAT)
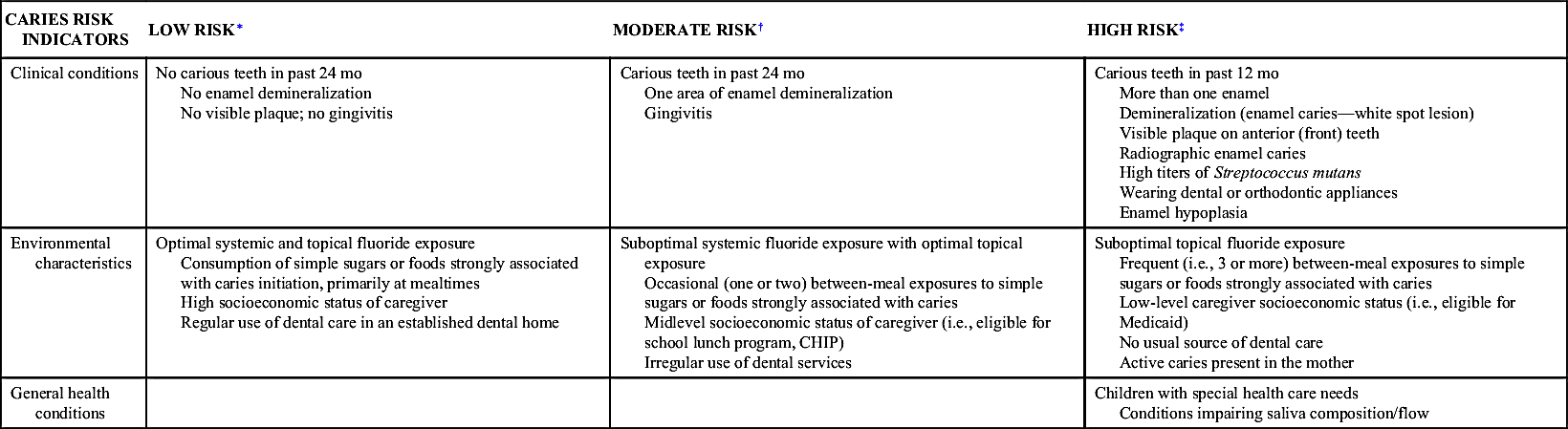
CHIP, Children’s Health Insurance Program.
∗ Low risk: The child does not have moderate-risk or high-risk indicators.
† Moderate risk: The presence of at least one moderate-risk indicator and no high-risk indicators present results in a moderate-risk classification.
‡ High risk: The presence of a single risk indicator in any area of the high-risk category is sufficient to classify a child as being at high risk.
Adapted from American Academy of Pediatric Dentistry: American Academy of Pediatric Dentistry Caries Risk Assessment Tool (CAT). http://www.chcs.org/usr_doc/AAP_CAT.pdf. Accessed May 7, 2014.
36. What medication shows the greatest promise for primary tooth pulpotomies?
Recent studies have suggested that MTA has great potential as a primary tooth pulpotomy medication. It results in less internal root resorption and improved clinical and radiographic outcomes compared with formocresol, ferric sulfate, or sodium hypochloride. (It also smells a lot better than formocresol.)
37. What are the disadvantages of MTA as a primary tooth pulpotomy medication?
They are mainly cost considerations. It is at least 20 times more expensive than formocresol.
38. Which branchial arch gives rise to the maxilla and mandible?
The first branchial or mandibular arch gives rise to the maxilla, mandible, Meckel’s cartilage, incus, malleus, muscles of mastication, and anterior belly of the digastric muscle.
39. How does the palate form?
The paired palatal shelves arise from the intraoral maxillary processes. These shelves, originally in a vertical position, reorient to a horizontal position as the tongue assumes a more inferior position. The shelves then fuse anteriorly with the primary palate, which arises from the median nasal process, and posteriorly and with one another. Failure of fusion results in a cleft palate.
40. When do the primary teeth develop?
At approximately 28 days in utero, a continuous plate of epithelium arises in the maxilla and mandible. By 37 days in utero, a well-defined, thickened layer of epithelium overlying the cell-derived mesenchyme of the neural crest delineates the dental lamina. Ten areas in each jaw become identifiable at the location of each of the primary teeth.
41. After the eruption of a tooth, when is root development completed?
In the primary dentition, root development is complete approximately 18 months after eruption; in the permanent dentition, the period of development is approximately 3 years.
42. Define ankylosis. How is it diagnosed?
Ankylosis is the fusion of cementum with alveolar bone and may occur at any time during the course of eruption. Because affected teeth have retarded vertical growth, they appear to be submerged below the occlusal plane. Diagnosis involves visual determination that a tooth may be 1 mm or more below the height of the occlusal plane, radiographic evidence of lack of a periodontal ligament, and/or lack of physiologic mobility. The ankylosed tooth emits an atypical sharp sound on percussion. In addition, children with affected siblings are twice as likely to have submerged teeth compared with the general population. Ankylosis often occurs bilaterally; 67% of affected people have two or more submerged teeth.
43. What causes ankylosis? Which teeth are usually affected?
The definitive cause of ankylosis is unknown. Contributing factors cited in the literature include local mechanical trauma, disturbed local metabolism, localized infection, chemical or thermal irritation, and gaps in the periodontal membrane.
Mandibular first primary molars are usually affected, followed by second mandibular molars, first maxillary molars, and second maxillary molars. The prevalence of infraclusion peaks between 8 and 9 years of age, with a suspected range of 1.3% to 8.9%.
44. How is ankylosis treated?
The severity of submergence dictates the treatment protocol. Therefore, constant vigilance at recall appointments is crucial. The age at which ankylosis begins determines the rate of submergence. The younger the child at onset of ankylosis, the more quickly the tooth submerges because of the increased rate of growth of alveolar bone height. In minor cases, in which the occlusal surface is within 1 mm of the occlusal plane, the tooth needs only monitoring for exfoliation. In rare cases, the ankylosis is severe enough that the occlusal surface meets the interproximal gingival tissue. In such cases, the affected tooth must be extracted, with subsequent space maintenance. For moderate cases, stainless steel crowns or buildup restorations can be used to prevent space loss or supraeruption. With mismanagement or misdiagnosis, the sequelae of infraclusion include space loss, molar tipping, supraeruption of antagonist teeth, and periodontal defects with decreased height of bone.
45. How should dosages of local anesthetic be calculated for a pediatric patient?
Because children’s weights vary dramatically for their chronologic age, dosages of local anesthetic should be calculated according to a child’s weight. A dosage of 4 mg/kg of lidocaine should not be exceeded in pediatric patients.
46. Should the parent be allowed in the operatory with the pediatric patient?
The debate continues. However, some studies have indicated that many pediatric dentists allow the parent to be present in the operatory.
47. What is the treatment for a traumatically intruded primary incisor?
In general, the treatment of choice is to allow the primary tooth to re-erupt. Re-eruption usually occurs in 2 to 4 months. If the primary tooth is displaced into the follicle of the developing permanent incisor, the primary tooth should be extracted.
48. What are the potential sequelae of trauma to a primary tooth?
Potential sequelae include color changes, necrosis, infection and tooth loss. Color changes include yellow (pulp canal obliteration or metamorphosis), pink (internal resorption), or gray-black (hemosiderin or pulpal necrosis) color changes. Hemosiderin is not uncommon within the first 30 days after the trauma. After 30 days, a gray or gray-black color change in the crown typically indicates pulp necrosis. Necrosis may occur at any time after the injury (weeks, months, years). No treatment is indicated unless other pathologic changes occur (e.g., periapical radiolucency, fistulation, swelling, pain).
Damage to the succedaneous permanent tooth, including hypoplastic defects, dilaceration of the root, or arrest of tooth development, has also been reported.
49. What are the indications for a lingual frenectomy?
Tongue-tie, or ankyloglossia, is relatively rare and usually requires no treatment. Occasionally, however, a short lingual frenum may result in lingual stripping of the periodontium from the lower incisors, which is an indication for frenectomy. A second indication is speech problems secondary to tongue position as diagnosed by a speech pathologist. Inability to latch on or breast-feed has been reported in some infants with a high lingual frenum. Breastfeeding in these patients has been reported to improve following frenectomy.
50. If a child reports a numb lip, can you be certain that the child has a profoundly anesthetized mandibular nerve?
Children, especially young ones, often do not understand what it means to be numb. The mandibular nerve is the only source of sensory innervation to the labia-attached gingiva between the lateral incisor and canine. If probing of this tissue with an explorer evokes no reaction from the patient, a profound mandibular block is present. No other sign can be used to diagnose profound anesthesia of the mandibular nerve.
51. Does slight contact with a healthy approximal surface during preparation of a class II cavity have any significant consequences?
Even slight nicking of the mesial or distal surface of a tooth greatly increases the possibility for future caries. Placement of an interproximal wedge before preparation significantly decreases the likelihood of tooth damage and future pathology.
52. Why bother with restoring posterior primary teeth?
Caries is an infectious disease. As at any location in the body, treatment consists of controlling and eliminating the infection. With teeth, caries infection can be eliminated by removing the caries and restoring or extracting the tooth. However, extraction of primary molars in children may result in loss of space needed for permanent teeth. To ensure arch integrity and reduce the risk of pain, infection, and loss of function, decayed primary teeth should be treated with well-placed restorations.
53. What is the most durable restoration for a primary molar with multisurface caries?
Stainless steel crowns have the greatest longevity and durability. Their 4.5-year survival rate is more than twice that of amalgam (90% vs. 40%).
54. How should a primary tooth be extracted if it is next to a newly placed class II amalgam?
1. The primary tooth to be extracted can be disked to remove bulk from the proximal surface. Care still must be taken to avoid contacting the new restoration.
2. Placing a matrix band (T-band) around the newly restored tooth offers additional protection.
3. When luxating the primary tooth, ensure that the elevator is placed subgingivally so that the forces are against alveolar bone rather than the adjacent amalgam.
55. Can composites be used to restore primary teeth?
If good technique is followed, composite material is not contraindicated. Interproximally, however, it may be difficult to get the type of isolation required for optimal bonding. There is no scientific advantage to using composite instead of amalgam for such restorations, and one has to evaluate whether aesthetic effects justify the additional time required for the composite technique in primary teeth.
56. List the indications and contraindications for pulpectomy in a primary tooth.
Indications
• Teeth with chronic inflammation or necrosis of the radicular pulp
• Often attempted on the primary second molar before eruption of the first permanent molar
Contraindications
• Teeth with advanced resorption (internal or external), loss of root structure, or evidence of periapical infection involving the crypt of the succedaneous tooth
• Primary root canals that are difficult to prepare because of variable and complex morphology
• Proximity of succedaneous tooth bud (unwanted damage may result from instrumentation, medication, or filling materials)
57. How successful is pulpectomy in a primary tooth?
In primary teeth with zinc oxide–eugenol (ZOE) pulpectomies, the success rate is 77.7%. Success rates as high as 100% have been reported with Vitapex (premixed calcium hydroxide and iodoform; Neo Dental International). The most important preoperative predictor of success is amount of tooth root absorption (>23% resorption reduces the success rate to only 23%). If correctly done, pulpectomy does not cause adverse effects on succedaneous tooth formation, but it does involve a 20% chance of altering the eruption path of the permanent tooth.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


