32. What are the manifestations of fluoride toxicity?
The ingestion of 5 g or more of fluoride in an adult results in death within 2 hours if the person does not receive medical attention. In a child, ingestion of a single dose greater than 400 mg results in death caused by poisoning in about 3 hours. Doses of 100 to 300 mg in children cause nausea and diarrhea.
33. How much fluoride is contained in an average 4.6-ounce tube of toothpaste?
Sodium monofluorophosphate or sodium fluoride toothpaste contains approximately 1.0 mg of fluoride/g of paste. Therefore, a 4.6-oz tube of toothpaste contains 130 mg of fluoride. A level of 435 mg of fluoride consumed in a 3-hour period is considered fatal for a 3-year-old child—only a little over three tubes of toothpaste need to be consumed to reach a fatal level.
34. What is the rationale behind the use of pit and fissure sealants in caries prevention?
Occlusal surfaces, particularly fissures, have not experienced as rapid a decline in the incidence of caries as proximal surfaces because fluoride’s protective effect is confined to smooth surfaces only. It has been observed that sealing the fissures from the oral environment prevents the development of occlusal caries. Sealants should be part of an early preventive program for protecting permanent molars.
35. What proportion of U.S. children has received dental sealants?
Of U.S. children, 30% of those age 6 to 11 years and 38% of adolescents age 12 to 19 years have received dental sealants. In addition, 39 states report having dental sealant programs to extend this service to the neediest children.
36. Describe evidence-based dentistry (EBD) and its three important domains.
Evidence-based dentistry is an approach to practice, an approach to making clinical decisions, and the provision of personalized dental care based on the most current scientific knowledge. The practice of EBD is based on the following:
1. The best available scientific evidence
2. A dentist’s clinical skill and judgment
3. Each individual patient’s needs and preferences.
37. What are the recommended sources when searching for clinical evidence?
• PubMed
• TRIP Database
• DARE (Database of Abstracts of Reviews of Effectiveness)
• National Guideline Clearinghouse
• Cochrane Library
• ADA’s EBD website
38. Do dentists have an obligation to report child abuse?
Yes. Dentists are morally, ethically, and legally obligated to report a suspected case of child abuse. Reports should be made to the local department of social services, although this may vary from state to state.
39. Where is the dentist’s code of ethics found?
The ADA has established a code of ethics that describes dentistry’s responsibility to society. The code is published in the Journal of the American Dental Association. It deals with issues of patient care, fees, practice guidelines, advertising, and referrals. The ADA Principles of Ethics and Code of Professional Conduct can be found at the ADA’s website, http://www.ada.org/en/about-the-ada/principles-of-ethics-code-of-professional-conduct/.
40. What does the ADA Code of Ethics state about the removal of dental amalgam to prevent mercury toxicity?
“The removal of amalgam restorations from the non-allergic patient for the alleged purpose of removing toxic substances from the body, when such treatment is performed solely at the recommendation of the dentist, is improper and unethical.”
41. How does the Americans with Disabilities Act affect dentists?
• Dentists cannot deny anyone care because of a disability.
• Offices must undergo architectural changes to allow access for the disabled.
• Employees are protected against dismissal because of a disability.
• Offices must accommodate disabled workers so they can perform jobs.
Epidemiology and Biostatistics
42. Define epidemiology.
Epidemiology is the study of the distribution and frequency of disease or injury in human populations and the factors that make groups susceptible to disease or injury.
43. Differentiate between incidence and prevalence.
Incidence is the number of new cases of disease occurring within a population during a given period. It is expressed as a rate, (cases)/(population)/(time).
Prevalence is the proportion of a population affected with a disease at a given point in time— (cases)/(population).
Example: A dentist counts the number of patients presenting to the office with newly diagnosed periodontal disease in a 6-month period. Of the 100 people who came to the office, 10 had periodontal disease. The incidence rate is calculated as 10/100 in 6 months, or 0.2/year. The range for incidence rates is from 0 to ∞. The prevalence of periodontal disease may be obtained by counting all patients with periodontal disease in the same period—that is, if 50 of 100 patients have periodontal disease, the prevalence is 50%. Remember, incidence is a rate and requires a unit of time, whereas prevalence is a proportion and is expressed as a percentage of the population.
44. What is meant by test sensitivity and specificity? How are they calculated?
Frequently, dentists wish to know if disease is present and may use some diagnostic test to arrive at an answer. In dentistry, the most frequently used test is radiography. Dental radiographs are imperfect in that they do not distinguish all diseased from disease-free surfaces. Sensitivity and specificity are measures that describe how good the radiograph is in such differentiation.
Sensitivity measures the proportion of persons with the disease who are correctly identified by a positive test (true-positive [TP] rate). Specificity measures the proportion of persons without disease who are correctly identified by a negative test (true-negative [TN] rate). Sensitivity and specificity are inversely proportional; as the specificity of a test increases, the sensitivity decreases. An ideal test would have both high specificity and sensitivity, yet tradeoffs can be made, depending on the condition being tested. Sensitivity and specificity can be calculated from a 2 × 2 table (Table 13-2). Sensitivity = (TP/TP) + FN; specificity = (TN/FP) + TN (FN is false-negative).
45. What is meant by positive predictive value (PPV)?
The PPV reflects the proportion of persons who have the disease, given that they test positive. It measures how well the test predicts the presence of a given disease. The PPV is calculated from a 2 × 2 table:

This calculation takes into account the prevalence of disease.
46. What is meant by negative predictive value (NPV)?
The NPV indicates the proportion of persons who do not have the disease, given that they test negative. It measures how many of test negatives are true negatives. The NPV is calculated from a 2 × 2 table:
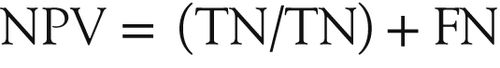
Positive and negative predictive values are directly related to the prevalence of the disease in the population. Assuming that all other factors remain constant, the PPV will increase with increasing prevalence and NPV will decrease with increasing prevalence.
47. What does the P value represent?
It means the probability that the observed result or something more extreme occurred by chance alone. Therefore, a P value of 0.05 indicates that there is only a 5% likelihood that the result observed was caused by chance alone. Traditionally, a P value of 0.05 is considered statistically significant. If the P value is more than 0.05, chance cannot be ruled out as an explanation for the observed effect. It is important to remember that chance can never be ruled out absolutely as an explanation for the observed results. A statistically significant result indicates that chance is not likely.
48. What is relative risk? Odds ratio?
The relative risk measures the association between exposure and disease. It is expressed as a ratio of the rate of disease among exposed persons to the rate among unexposed persons. Relative risk estimates the strength or magnitude of an association. The calculation of relative risk requires incidence rates, which are provided by cohort studies.
The odds ratio provides an estimate of the relative risk in case-control studies; because disease has already occurred, the incidence of disease cannot be determined.
49. How do the mean, median, and mode differ?
The three terms are measures of central tendency and are used to provide a summary measure to characterize a group of people. The mean represents the average. It is calculated by adding together all the observations and then dividing by the total number of measurements. The mean takes into account the magnitude of each observation and, as a result, is easily affected by extreme values. The median is defined as the middlemost measurement (50th percentile)—that is, half the observations are below it and half are above. Therefore, the median is unaffected by extreme measures. The mode is the most frequently used observation.
50. Which of the following is most appropriate to test for differences between the means of two groups—ANOVA, t-test, or chi-square?
A t-test is used to compare the means between two groups. The ANOVA, or analysis of variance, compares the means in more than two groups. The chi-square test is used to show differences in proportions.
51. Confidence intervals are often provided when data are reported. What do they indicate?
Confidence intervals (CIs) represent the range within which the true magnitude of the effect lies with a certain degree of certainty. For example, a relative risk of 2.1 may be reported with a 95% CI (1.5, 2.9). This indicates that the study determined the relative risk to be 2.1 and that we are 95% certain that the true relative risk is not less than 1.5 or more than 2.9. If the 95% CI includes the null value (1.0), the result is not statistically significant.
52. Compare cross-sectional, case-control, and cohort studies.
Cross-sectional studies are a type of descriptive epidemiologic study in which the exposure and disease status of the population are determined at a given point. For example, the caries status of U.S. adults age 45 to 65 years in 1992 may be determined by a national dental survey and examination.
Case-control and cohort studies are analytic epidemiologic studies. In case-control studies, participants are selected on the basis of disease status. The “cases” are persons who have the disease of interest, and the control group consists of persons similar to the case group except that they do not have the disease of interest. Information about exposure status is then obtained from each group to assess whether an association exists between exposure and disease.
In cohort studies, participants are selected on the basis of exposure status. Study participants must be free of the disease of interest at the time the study begins. Exposed and nonexposed participants are then followed over time to assess the association between exposure and specific diseases.
53. Which type of study—cohort, case-control, retrospective, or clinical trial—most closely resembles a true experiment?
In a clinical trial, the investigator allocates the participants to the exposure groups of interest and then follows the groups over time to observe how they differ in outcome. This method most closely resembles an experiment.
54. Define clinical trial, the major types of clinical trials, and their purpose.
Clinical trial is a research study to answer specific questions about vaccines or new therapies or new ways of using known treatments. The National Institutes of Health (NIH) has classified clinical trials into five types:
1. Treatment trials: To test experimental treatments, new combinations of drugs, or new approaches to surgery or radiation therapy. For example, in dentistry, treatment trials are commonly used to test new dental restorative materials, implants, and treatment for dry mouth.
2. Prevention trials: To look for better ways to prevent disease in people who have never had the disease or to prevent a disease from returning. These approaches may include medicines, vaccines, vitamins, minerals, or lifestyle changes. Prevention trials are frequently carried out in dental caries prevention.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


