The symptoms may progress to coma and convulsions without intervention.
43. What should the dentist be prepared to do for the patient who has a hypoglycemic reaction?
The dental practitioner should have some form of sugar readily available, such as packets of table sugar, candy, or orange juice. Also available are 4- to 5-gram tablets of glucose. It is recommended that a hypoglycemic patient take 15 grams of fast-acting carbohydates (glucose), which is approximately 3 to 4 tablets. If a patient develops symptoms of hypoglycemia, the dental procedure should be discontinued immediately; if conscious, the patient should be given some form of oral glucose.
If the patient is unconscious, the emergency medical service should be contacted. Glucagon, 1 mg, can be injected IM, or 50 mL of 50% glucose solution can be given by rapid IV infusion. The glucagon injection should restore the patient to a conscious state within 15 minutes, and then some form of oral sugar can be given.
44. Is the diabetic patient at greater risk for infection after an oral surgical procedure?
It is important to minimize the risk of infection in diabetic patients. They should have aggressive treatment of dental caries and periodontal disease and be placed on frequent recall examinations and oral prophylaxis.
After oral surgical procedures, endodontic procedures, and treatment of suppurative periodontitis, diabetic patients should be placed on antibiotics to prevent infection secondary to delayed healing. Antibiotics of choice are amoxicillin, 500 mg 3 times daily, or clindamycin, 300 mg 3 times daily for 7 to 10 days.
45. When is it necessary to increase the dose of corticosteroids in dental patients who have primary or secondary adrenal insufficiency?
Guidelines on the use of supplemental corticosteroids state that only those patients who have primary adrenal insufficiency and who are undergoing surgical procedures require supplementation with additional corticosteroids. They do not require supplementation for routine dental procedures.
Patients who have secondary adrenal insufficiency only require their usual dose of corticosteroid on the morning of the procedure.
If supplementation is needed for those patients with primary adrenal insufficiency, the following guidelines apply:
| Procedure | Target Dose |
| Routine dentistry | None |
| Minor surgery | 25 mg hydrocortisone preoperatively on day of surgery |
| Moderate surgical stress | 50-75 mg hydrocortisone on day of surgery and up to 1 day after |
| Major surgical stress | 100-150 mg/day of hydrocortisone, given for 2 to 3 days |
46. What are the clinical symptoms of hypothyroidism? What dental care can be safely provided?
The clinical symptoms of hypothyroidism are weakness, fatigue, intolerance to cold, changes in weight, constipation, headache, menorrhagia, and dryness of the skin. Dental care should be deferred until after a medical consultation in a patient with or without a history of thyroid disease who experiences a combination of these signs and symptoms. If the patient is myxedematous, he or she should be treated as a medical emergency and referred immediately for medical care. It is important not to prescribe opiates for the palliative treatment of the myxedematous patient, who may be unusually sensitive and die after being given a normal dose of an opiate.
Allergic Reactions
47. What would you prescribe for the patient who develops a mild soft tissue swelling of the lips under the latex rubber dam?
The patient probably has had a contact allergic reaction from the latex. If the reaction is mild (slight swelling, with no extension into the oral cavity) and self-limiting, the patient should be given 50 mg of oral diphenhydramine and observed for at least 2 hours for a possible delayed reaction. If the reaction is moderate to severe, the patient should be given 50 mg of diphenhydramine IM or IV and closely monitored. Emergency services should be contacted to transport the patient to the emergency department for treatment and observation. Allergic patients should be instructed to inform their health care providers of their latex allergy and referred to an allergist. Dentists are encouraged to use nonlatex rubber dams and gloves whenever possible.
48. What should you do if a patient for whom you prescribed the prophylactic antibiotic amoxicillin approximately 1 hour previously reports urticaria, erythema, and pruritus (itching)?
If the reaction is delayed (>1 hour) and limited to the skin, the patient should be given 50 mg of diphenhydramine IM or IV and then observed for 1 to 2 hours before being released. If no further reaction occurs, the patient should be given a prescription for 25 to 50 mg of diphenhydramine to be taken every 6 hours until symptoms are gone.
If the reaction is immediate (<1 hour) and limited to the skin, 50 mg of diphenhydramine should be given immediately IM or IV. The patient should be monitored and emergency services contacted to transport the patient to the emergency department. If other symptoms of allergic reaction occur, such as conjunctivitis, rhinitis, bronchial constriction, or angioedema, 0.3 mL of aqueous 1:1000 epinephrine should be given by subcutaneous (SC) or IM injection. The patient should be monitored until emergency services arrive. If the patient becomes hypotensive, an IV line should be started with Ringer’s lactate or 5% dextrose in water.
49. What are the signs and symptoms of anaphylaxis? How should it be managed in the dental office?
Anaphylaxis is characterized by bronchospasm, hypotension or shock, and urticaria or angioedema. It is a medical emergency in which death may result from respiratory obstruction, circulatory failure, or both. With the first indication of anaphylaxis, 0.3 to 0.5 mL of 1:1000 aqueous epinephrine should be injected SC or IM, and emergency services should be contacted. The injection of epinephrine may be repeated every 20 to 30 minutes, if necessary, for as many as three doses. Oxygen at a rate of 4 L/min must be delivered with a face mask. The patient must be continuously monitored, and an IV line containing Ringer’s lactate or normal saline should be infused at 100 mL/hr. If the patient becomes hypotensive, the IV infusion should be increased. If airway obstruction occurs because of edema of the larynx or hypopharynx, a cricothyrotomy must be performed. If the airway obstruction is caused by bronchospasm, an albuterol or terbutaline nebulizer should be used or IV aminophylline, 6 mg/kg, infused over 20 to 30 minutes.
Hematology and Oncology
50. What are the normal values for a CBC?
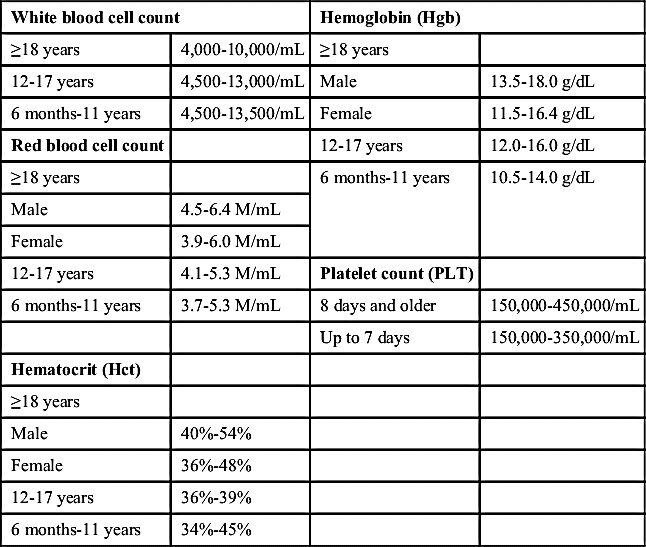
51. What precautions should be taken when providing dental care to a patient with sickle cell anemia?
1. Patients with sickle cell disease should not receive dental treatment during a crisis, except for the relief of dental pain and treatment of acute dental infections. Dental infections should be treated aggressively; if facial cellulitis develops, the patient should be admitted to the hospital for treatment.
2. The patient’s physician should be consulted about the patient’s cardiovascular status. Myocardial damage secondary to infarctions and iron deposits is common.
3. Patients with sickle cell anemia are at increased risk for bacterial infections when surgical procedures are performed. Although there is no evidence to support their use, prophylactic antibiotics are often administered before any dental surgical procedure to prevent the possibility of wound infection and/or osteomyelitis. It is not recommended for routine, nonsurgical procedures. The same prophylactic antibiotic regimen used for the prevention of endocarditis should be followed. After a surgical procedure, antibiotics (amoxicillin, 500 mg three times daily, or clindamycin, 300 mg three times daily) should be considered for 7 to 10 days postoperatively.
52. What hematologic disorders are characterized by a so-called hair-on-end appearance of bone on radiographic surveys?
Thalassemia major and sickle cell anemia are characterized in this way.
53. Can local anesthetic with a vasoconstrictor be used for a patient with sickle cell disease?
Because of the possibility of impairing local circulation, the use of vasoconstrictors in patients with sickle cell disease is controversial. It is recommended that the planned dental procedure dictate the choice of local anesthetic. If the planned procedure is a short routine procedure that can be performed without discomfort by using an anesthetic without a vasoconstrictor, the vasoconstrictor should not be used. However, if the procedure requires long profound anesthesia, 2% lidocaine with 1:100,000 epinephrine is the anesthetic of choice.
54. Can nitrous oxide be used to help manage anxiety in patients with sickle cell anemia?
Nitrous oxide can be safely used in patients with sickle cell anemia as long as the concentration of oxygen is greater than 50%, the flow rate is high, and the patient can ventilate adequately.
55. Can a dental infection cause a crisis in a patient with sickle cell anemia?
Preventive dental care—routine scaling and root planing, topical fluorides, sealants, and treatment of dental caries—is important in patients with sickle cell anemia. Studies have reported some cases of a sickle cell crisis precipitated by a periodontal infection.
56. What are the oral symptoms of acute leukemia?
More than 65% of patients with acute leukemia have oral symptoms. The symptoms result from myelosuppression caused by the overwhelming numbers of malignant cells in the bone marrow and/or large numbers of circulating immature cells (blasts).
1. Symptoms from thrombocytopenia—gingival oozing, petechiae, hematoma, and ecchymosis
2. Symptoms from neutropenia—recurrent or unrelenting bacterial infections, lymphadenopathy, oral ulcerations, pharyngitis, and gingival infection
3. Symptoms from circulating immature cells (blasts)—gingival hyperplasia from blast infiltration
Patients with these signs or symptoms should be evaluated to rule out a hematologic malignancy. The dentist should consider carefully whether the symptoms can be explained by local factors or are disproportionate to these factors. If a hematologic malignancy is suspected, a CBC with a differential white cell count should be ordered.
57. Which leukemia is typically referred to as the leukemia of childhood?
Acute lymphocytic leukemia almost always occurs in children. The condition can be successfully treated, with a 50% to 70% 5-year survival.
58. Is it safe to extract a tooth in a patient who is receiving chemotherapy?
The major organ system affected by cytotoxic chemotherapy is the hematopoietic system. When a patient receives chemotherapy, the white cell count and platelets may be expected to decrease in about 7 to 10 days. If the patient’s absolute neutrophil count (calculated by multiplying the white cell count by the number of neutrophils in the differential count and dividing by 100) drops below 500 neutrophils, the patient is considered neutropenic and at risk for infection. If the platelet count drops below 50,000/μL, the patient is at risk for bleeding.
If possible, dental procedures should be scheduled 2 weeks before planned chemotherapy or after the counts begin to recover, usually 14 days for white cells and 21 days for platelets. Dental treatment should be attempted only after consultation and in coordination with the patient’s physician and after the patient has had a CBC.
59. Which precautions should be taken in treating a patient who has undergone bone marrow transplantation for a hematologic malignancy?
Dental care should be done only in consultation with the patient’s physician. As a rule, elective dental treatment should be postponed for 6 months after transplantation. However, emergency dental treatment can be carried out. If dental care must be done before the recommended postponement, a CBC should be checked, and if the results are acceptable (platelets > 50,000/μL and neutrophils > 500), the patient should be premedicated using the same regimen as for the prevention of endocarditis.
60. What should be done if a patient has enlarged lymph nodes?
Lymphadenopathy may be secondary to a sore throat, upper respiratory infection, or the initial presentation of a malignancy. A thorough history and clinical examination help determine the cause of the lymphadenopathy.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


