P
Paget disease Osteitis deformans. Disease of unknown etiology, characterized by enlargement of the cranial bones and often the maxilla and mandible. Cotton-wool appearance of bone on a radiograph may be a diagnostic feature.
Palatal graft See: Free gingival graft.
Palatal implant Endosseous implant placed in the hard palate, which is an anatomic location for an implant in the maxilla, or an anatomic location option for use of an implant as anchorage in orthodontic treatment.
Palatal vault Superior surface of the hard palate.
Panoramic radiograph Tomographic survey radiograph of the maxillofacial complex in two dimensions. Image displays the maxilla and the mandible in its curvature and is produced by conventional tomography. Some x-ray machines allow the image to be obtained in sectors.
Papilla (pl: papillae) Portion of gingiva extending interdentally below the contact points of two adjacent teeth.
Papilla preservation Measure taken to maintain the interdental papillae following tooth extraction to avoid black triangles between an implant and an adjacent tooth or between adjacent implants. This may include an atraumatic extraction, alveolar ridge preservation, and/or respecting certain parameters when placing implants, such as apicocoronal position and inter-implant distance.
Papilla regeneration Creating a papilla between an implant and an adjacent tooth or between adjacent implants. This may involve surgical procedures using small rotational pedicle flaps, use of connective tissue grafts, and/or prosthetic techniques to condition peri-implant soft tissues. The term is a misnomer, since the papillae flatten in the edentulous space following tooth extraction once the transseptal inserting fibers are lost. A flattened papilla cannot be truly regenerated, but the clinician may optimize its appearance by prosthetic means. The appearance of a papilla is mainly determined by the interdental bone height, which has a documented threshold of approximately 5 mm.1-4
Papilla-sparing incision Incision that does not include the papilla and thus avoids the elevation of these tissues.
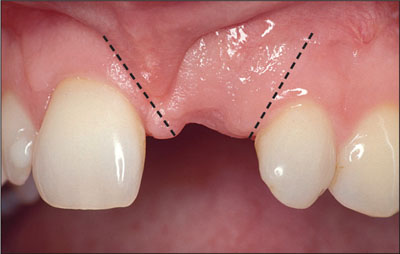
Papilla-sparing incision. (Courtesy of D. Buser).
Paracervical saucerization Progressive bone resorption occurring around the cervical portion of implants. Plausible etiologic factors can include: surgical trauma, peri-implantitis, occlusal overload, microgap, implant crest module, and compromise of the biologic width. Also, the excavation of tissue to form a shallow shelving depression, usually to facilitate drainage from infected areas of bone. Called also craterization.
Paracrine Transfer of chemical compounds such as hormones and growth factors from cell to cell.
Parallel-fibered bone Repair bone deposited onto woven bone and old bone surfaces in a healing situation as parallel layers of bone. The collagen fibers run parallel to the surface but are not organized in a lamellar fashion.
Parallel(ing) pin See: Direction indicator.
Parallel-sided implant Implant with an untapered body when viewed in profile, lengthwise.
Parallel-walled implant See: Parallel-sided implant.
Paresthesia Abnormal sensation of pricking, tingling, or burning related to injury or irritation of a sensory nerve.
Partial denture Fixed or removable dental prosthesis supported and retained by teeth or implants for the replacement of less than a full complement of natural teeth and related hard and soft tissues.5 Called also partial prosthesis.
Implant supported p. d. See: Fixed prosthesis.
Partially edentulous State of being without one or more, but not all, of the natural teeth.5 See also: Edentulous.
Partial-thickness flap Surgical flap that is elevated within connective tissue only, thus leaving the periosteum intact and undisturbed.
Particulate autogenous graft See: Autogenous bone graft.
Particulate graft Graft used in particulate form, which may be an autograft, allograft, alloplast, or xenograft. Particulate grafts differ concerning osteogenic potential, osteoconductivity, hydrophilicity, pore and particle size, and substitution rate.6-8
Particulate marrow cancellous bone (PMCB) Graft material obtained from donor sites, such as the iliac crest, with extensive marrow content. PMCB of an autogenous nature is the most osteogenic graft material; the number of multipotential stems cells is especially high.
Passivated surface oxide Surface treatment of an oxidized implant surface resulting in lower surface energy and increased corrosion resistance. This may be the result of intentional treatment of the surface by the manufacturer or simply by exposure to air over time.
Passivation Formation of an oxide layer on the surface of metal exposed to air- and/or oxygen-containing solutions.
Passive fit Adaptation of one component to another in a manner that does not impart strain. In dental implant prosthodontics, the creation of passively fitting prostheses is desirable.
Patient assessment See: Patient evaluation.
Patient-based measure Descriptive term referring to the array of questionnaires, interview schedules and other related methods of assessing health, illness, and benefits of healthcare interventions from the patient’s perspective. A patient-based outcome measure that addresses constructs such as health-related quality of life, subjective health status, and functional status; used as primary or secondary end-points in clinical trials.9
Patient evaluation Process by which a patient’s condition is determined. Called also patient assessment.
Patient examination Clinical examination of the patient, including extraoral and intraoral findings. Called also control. See also: Examination.
Patient history Record of the patient’s medical and dental histories.
Patient satisfaction Individual’s perceived fulfillment of a need or a want; can be measured by obtaining reports or ratings from patients about services received from an organization, hospital, physician, or healthcare provider.10
Patient selection Selection of patients who are appropriate candidates for a particular therapy based on risk assessment, including medical, dental, and anatomic factors, as well as smoking habits and psychologic aspects.
Patrix component The part of an attachment system that is designed specifically to insert and engage the matching receptacle or mate component (matrix) for mechanical retention. Attachment systems that use mechanical retention are available in various designs. See also: Attachment system; Ball attachment system; Bar attachment system; Stud-type attachment system; Telescopic coping attachment system.
PDGF Abbreviation for Platelet-derived growth factor.
PDL Abbreviation for Periodontal ligament.
Pedicle flap Rotated or laterally moved flap receiving its blood supply from the original base of the flap. It is used to cover an adjacent surgical site or improve the thickness of soft tissue contours.11 See also: Soft tissue augmentation.
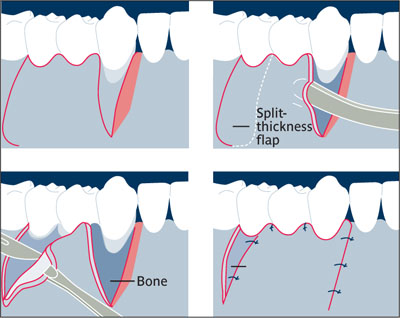
Pedicle flap.
(Redrawn from lto and Johnson12 with permission.)
Peer-reviewed journal Periodical publication for which individuals who are of an academic and/or professional standing equal to that of the author(s) have determined that all articles are of sufficient quality and completeness.
Peer-reviewed literature analysis Analysis of published research reports by individual(s) with expertise similar to that of the author(s).
Penicillin A generic name for a related group of natural or semi-synthetic antibiotics derived directly or indirectly from strains of fungi of the genus Penicillium, which exert a bactericidal as well as a bacteriostatic effect on susceptible bacteria by interfering with the final stages of the synthesis of peptidoglycan, a substance in the bacterial cell wall. The penicillins have relatively low toxicity for the host and are active against multiple organisms, especially gram-positive pathogens (streptococci, staphylococci, pneumococci); clostridia; some gram-negative forms (gonococci, meningococci); some spirochetes and fungi. They are classified as penicillin G and congeners (penicillin V), anti-staphylococcal penicillins (methicillin, dicloxacillin), extended spectrum penicillins (ampicillin and amoxicillin), and extended spectrum penicillins with beta-lactamase inhibitors (amoxicillin and clavulanate, ampicillin and sulbactam).13 See also: Amoxicillin.
Percentage bone-implant contact Area of bone in direct contact with the implant surface; usually measured from histologic specimens.14
Percutaneous implant Implant placed and positioned through the skin, eg, implants placed extraorally for reconstruction of facial structures or those used in the treatment of fractures in buccomaxillofacial and orthopedic areas.
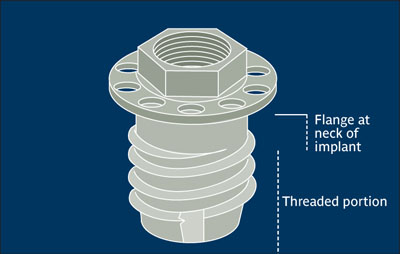
Percutaneous implant.
(Redrawn from Brånemark and Tolman15 with permission.)
Perforation Inadvertent tear or dehiscence within a flap created during surgery, either by overthinning the mucosa, improper blade direction while making periosteal releasing incisions, or excessive flap retraction.
Peri-abutment Region surrounding an implant abutment. Usually refers to the soft or hard tissues surrounding the abutment.
Periapical radiograph Radiograph taken intraorally showing the entire tooth from the occlusal plane to the apex. The radiograph should reach 3 mm beyond the structures of the tooth.
Pericrestal incision Incision placed not directly over the crest, but in either a more buccal or lingual location.
Peri-implant Around an implant. Often used to describe soft or hard tissues surrounding an oral implant, eg, peri-implant mucosa or bone.
Peri-implant crevicular epithelium Epithelium of the marginal peri-implant mucosa that bounds the peri-implant mucosal crevice and faces the abutment region of the oral implant.
Peri-implant disease Disease that affects the tissues associated with an oral implant and/or abutment. Bacteria play a major role in the etiology of peri-implant diseases, which can be restricted to soft tissue (mucositis) or progress to the supporting bone and induce its destruction (peri-implantitis).
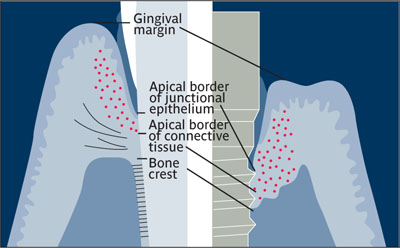
Peri-implant disease (right) compared to periodontal disease (left).
(Redrawn from Grant et al16 with permission.)
Peri-implant mucositis Progressive bone loss and inflammatory tissue pathology resulting from plaque accumulation and bacterial infiltration around implants.17
Peri-implant soft tissue Keratinized or nonkeratinized mucosa around an oral implant.
Peri-implant tissue recession Location of the receding marginal peri-implant tissues apical to the prosthesis-implant interface.
Peri-implantitis Condition of inflamed peri-implant soft tissues, bone loss, and increased probing depth combined with exudation.
Periodontal abscess Localized purulent inflammation of the periodontal tissues. Called also lateral periodontal abscess.
Periodontal biotype Categorization determined by variable biologic or physiologic characteristics of periodontal tissue. To evaluate the periodontal biotype, a periodontal probe can be placed at the facial aspect of the periodontal (or peri-implant) sulcus. It is categorized as thin if the outline of the underlying probe can be seen through the gingiva or mucosa, or thick if the probe cannot be seen.
Thick p. b. Periodontal biotype characterized by a thick and wide keratinized tissue at the facial aspect of teeth and oral implants. This biotype is prone to pocket formation instead of gingival recession in the presence of periodontal disease.
Thin p. b. Periodontal biotype characterized by a thin periodontal tissue at the facial aspect of teeth or oral implants. This biotype is prone to gingival recession following mechanical or surgical manipulation.
Thin-scalloped p. b. Classification of periodontium according to its facial aspects, distinguished by a pronounced disparity between the height of the gingival margin on the direct facial and that found interproximally (ie, noticeable rise and fall of marginal tissue). The underlying bone is usually thin on the facial aspect with dehiscences and fenestrations common.
Periodontal bone regeneration Regeneration of tooth-supporting alveolar bone that includes new cementum and periodontal ligament (PDL) on the root surface of a previously diseased tooth.
Periodontal disease General term that includes all pathologic processes that affect the periodontal tissues. They can be restricted to the soft tissues (gingivitis) or involve all the periodontal support tissues (periodontitis) and induce periodontal attachment loss.
Advanced p. d. Chronic or aggressive periodontitis characterized by clinical attachment loss of 5 mm or more. Teeth with resorption of more than a third of the supporting alveolar bone constitute advanced or severe disease.
Periodontal dressing Protective material applied over the wound created by periodontal surgical procedures.
Periodontal ligament (PDL) Specialized fibrous, richly vascular, cellular connective tissue of the periodontium that surrounds the roots of the teeth and is attached to the root cementum, separating it from and attaching it to the alveolar bone. Main functions are to hold a tooth in its socket and to permit tooth mobility and force distribution and absorption by the alveolar process. Called also periodontal membrane.
Periodontal maintenance Procedure performed at selected intervals to assist the periodontal patient in maintaining oral health. As part of periodontal therapy, this procedure is under the supervision of the dentist and not synonymous with a prophylaxis. Called also supportive periodontal therapy (SPT), preventive maintenance, and recall maintenance.
Periodontal membrane See: Periodontal ligament (PDL).
Periodontal plastic surgery Surgical procedure performed to correct or eliminate anatomic, developmental, or traumatic deformities of the gingiva or alveolar mucosa.18 See: Mucogingival surgery.
Periodontal pocket Pathologic fissure between a tooth and the crevicular epithelium, limited at its apex by the junctional epithelium; caused by migration of the junctional epithelium along the root as the periodontal ligament (PDL) is detached by a disease process. See also: Peri-implant disease.
Periodontal probe
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


