A. Extrinsic
(i) Chromogenic diet (wine, coffee, tea)
(ii) Tobacco
(iii) Mouthrinses
(iv) Plaque
B. Intrinsic
(i) Systemic causes
Tetracycline staining
Metabolic disorders (fluorosis, dystrophic calcification)
Genetic (congenital erythropoietic porphyria, amelogenesis imperfecta, dentinogenesis imperfecta)
(ii) Local causes
Pulp necrosis
Intrapulpal haemorrhage
Pulp tissue remnants after endodontic treatment
Endodontic materials
Coronal filling materials
Root resorption
Ageing
Trauma (calcific metamorphosis)
The discoloured anterior nonvital tooth has likely been weakened from a combination of previous trauma, endodontic therapy, dental caries and restorative treatment. Destructive alternative prosthodontic treatment options such as veneers or crowns are odds to further weaken the tooth lending it towards possible failure and extraction in the future.
Nonvital tooth bleaching is both useful and less detrimental in the treatment of traumatized discoloured anterior teeth. Different protocols have been advocated for bleaching these teeth including the conventional walking bleach technique [1–3], the chairside power bleaching technique [3] and a modified home bleaching technique [4].
The bleaching agents commonly used for whitening root-filled teeth include hydrogen peroxide (concentrations ranging from 5 to 35 %) [5], carbamide peroxide (10 %) [6] and sodium perborate [1, 7–9].
Sodium perborate is an oxidizing agent available as powder (Bocasan). The walking bleach technique utilizes a paste formed by mixing sodium perborate and distilled water. This technique can lead to successful whitening of nonvital root-filled teeth reducing the risks of side effects [5].
Nonvital bleaching is proposed for endodontically treated teeth which have become discoloured as a result of pulpal necrosis [5], intrapulpal haemorrhage [10], pulp tissue remnants after endodontic treatment [11] and incomplete removal of filling materials and sealer remnants in the coronal access cavity [12].
The occurrence of external cervical root resorption is a serious complication following nonvital bleaching techniques, and its incidence ranges from 1 to 13 % [13–18]. External cervical root resorption can occur more frequently in those cases where higher concentrations of bleach were used, past history of trauma and use of the thermocatalytic method of bleaching (application of heat) [16–18].
The patient must be informed that although the option of nonvital bleaching is a relatively low-risk intervention, from a restorative point of view, it is prone to reversal and reoccurrence of discolouration in the long term [19].
To summarize in the walking bleach technique, the root filling should be completed first, and a cervical seal must be established. The bleaching agent is left in the tooth so that it can function as walking bleach until the next visit. The bleaching agent should be changed every 3–7 days for up to 3–4 visits [20].
18.2 Walking Bleach Technique
- 1.
First the surface of the tooth is cleaned with pumice and the pretreatment tooth shade is recorded. The patient should be informed that the results of bleaching are not predictable and not guaranteed in all cases. Furthermore the patient is instructed as to the number of appointments and possible complications including cervical root resorption. Preoperative clinical photographs are helpful when demonstrating the change following bleaching to the patient.
- 2.
Before commencing bleaching, a preoperative radiograph should be taken to assess the existing quality of the root canal filling and status of the peri-apical tissues. Under no circumstances should bleaching be undertaken if there are any concerns with regard to this. Root canal retreatment should be carried out when in doubt and the filling material allowed to set at least a week prior to commencing intra-coronal bleaching (Figs. 18.1 and 18.2).
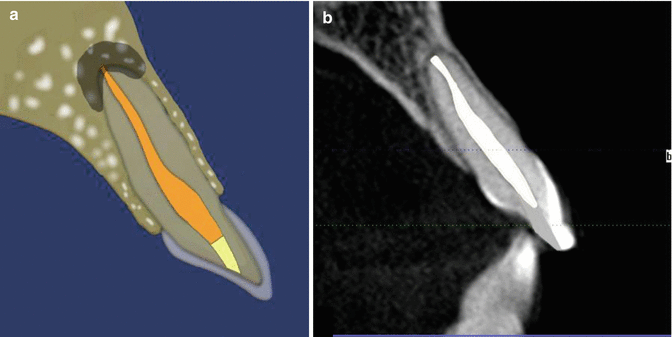 Fig. 18.1Diagrammatic representation showing radiographic contraindications and indications prior to carrying out the non-vital walking bleach technique. Note: (a) obvious preexisting periradicular disease and (b) no preexisting lucency. If there are any clinical and/or radiographic signs and symptoms correlated with apical periodontitis, then endodontic re-treatment should be carried out in the first instance
Fig. 18.1Diagrammatic representation showing radiographic contraindications and indications prior to carrying out the non-vital walking bleach technique. Note: (a) obvious preexisting periradicular disease and (b) no preexisting lucency. If there are any clinical and/or radiographic signs and symptoms correlated with apical periodontitis, then endodontic re-treatment should be carried out in the first instance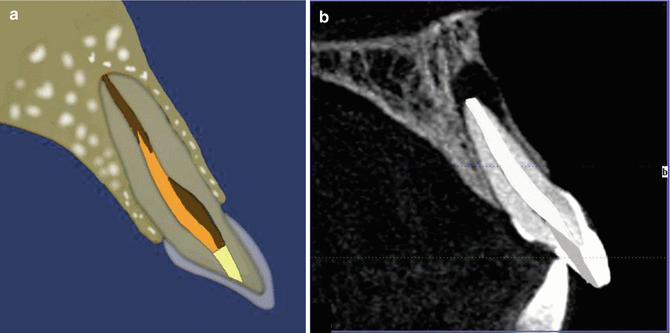 Fig. 18.2Diagrammatic representation showing radiographic indications and contraindications prior to carrying out non-vital walking bleach technique. Note (a) Non-homogenous root filling, poor condensation and voids visible. The root filling terminates >2 mm from the radiographic apex and is deemed ‘unacceptable’ even though no peri-radicular pathology is present. Re-treatment is indicated prior to non vital bleaching procedures. (b) Although a well condensed root filling is present and deemed acceptable peri-radicular pathology is present. Re-treatment should be carried out prior to bleaching procedures
Fig. 18.2Diagrammatic representation showing radiographic indications and contraindications prior to carrying out non-vital walking bleach technique. Note (a) Non-homogenous root filling, poor condensation and voids visible. The root filling terminates >2 mm from the radiographic apex and is deemed ‘unacceptable’ even though no peri-radicular pathology is present. Re-treatment is indicated prior to non vital bleaching procedures. (b) Although a well condensed root filling is present and deemed acceptable peri-radicular pathology is present. Re-treatment should be carried out prior to bleaching procedures - 3.
Rubber dam should be used to isolate the tooth in question. The access cavity is prepared, and all coronal remnants of restorative material, root filling materials and necrotic pulp tissue should be completely removed. In the anterior teeth, it is important to incorporate the mesial and distal pulp horns in the access cavity design and ensure that these areas are ultrasonically prepared to remove any remnants.
- 4.
The root filling should be reduced 1–2 mm below the cement-enamel junction (CEJ). This can be determined by using a periodontal probe placed in the pulp cavity and comparing to external probing depths to the CEJ. The root filling should be sealed with a base (IRM or glass ionomer cement) of at least 2 mm to prevent diffusion of bleaching agents from the pulp chamber to the apical foramen. This sealing material should also reach the level of the CEJ to prevent leakage of bleaching products into the surrounding periodontium resulting in increased risk of external cervical root resorption. A radiograph can be taken to confirm that this step is correct (Figs. 18.3 and 18.4).
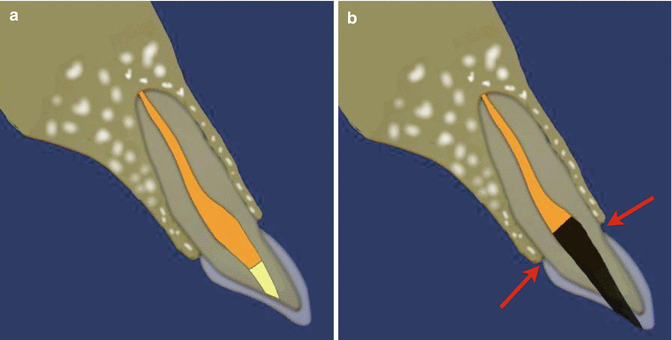 Fig. 18.3Diagrammatic representation of non-vital bleaching procedure showing (a) preoperative view of tooth undergoing non-vital bleaching procedure. There are no signs of any peri-radicular or apical radiolucency and the existing root filling is well obturated. (b) The root filling material is cut back to below the level of the cement-enamel junction (CEJ) (red arrow)
Fig. 18.3Diagrammatic representation of non-vital bleaching procedure showing (a) preoperative view of tooth undergoing non-vital bleaching procedure. There are no signs of any peri-radicular or apical radiolucency and the existing root filling is well obturated. (b) The root filling material is cut back to below the level of the cement-enamel junction (CEJ) (red arrow) - 5.
The pulp chamber is etched with 37 % phosphoric acid for 30–60 s, washed and dried. This allows opening of dentinal tubules for penetration of bleaching agent (Fig. 18.4).
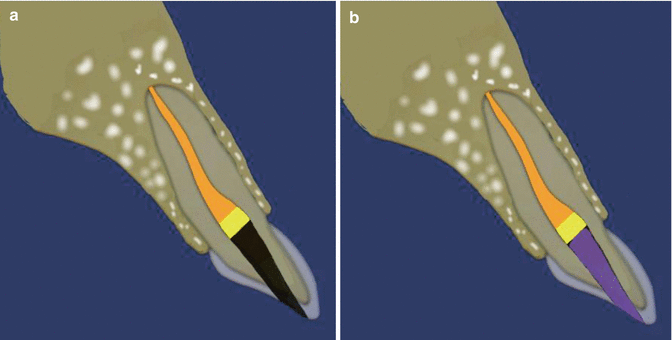 Fig. 18.4Diagrammatic representation of the non-vital bleach technique showing (a) preexisting root filling cut 1–2 mm below the level of the CEJ (orange) with overlying base material (yellow). (b) Placement of etch into coronal pulp chamber (purple) (37 % phosphoric acid) to allow penetration of bleach in to the dentinal tubules
Fig. 18.4Diagrammatic representation of the non-vital bleach technique showing (a) preexisting root filling cut 1–2 mm below the level of the CEJ (orange) with overlying base material (yellow). (b) Placement of etch into coronal pulp chamber (purple) (37 % phosphoric acid) to allow penetration of bleach in to the dentinal tubules - 6.
Sodium perborate (Bocasan) is mixed with distilled water in a ratio of 2:1. The bleaching agent can be applied with a suitable carrier or plugger (Fig. 18.7).
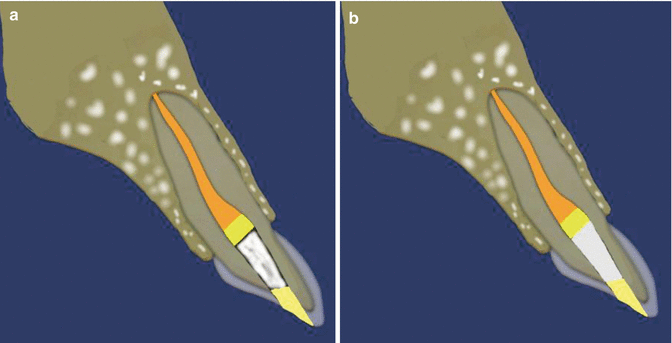 Fig. 18.5Diagrammatic representation of the non-vital bleach technique showing (a) placement of bleach into coronal pulp chamber and overlying temporary restoration. The patient can be reviewed every 3–4 days for replacement of bleach up to 3–4 visits (depending on changes in discoloration). Usually you should aim to over-bleach due to risk of relapse. (b) Placement of calcium hydroxide dressing in the coronal pulp chamber when bleaching procedure has been completed. A final definitive tooth colored restoration can then be placed sealing the coronal pulp chamber permanently
Fig. 18.5Diagrammatic representation of the non-vital bleach technique showing (a) placement of bleach into coronal pulp chamber and overlying temporary restoration. The patient can be reviewed every 3–4 days for replacement of bleach up to 3–4 visits (depending on changes in discoloration). Usually you should aim to over-bleach due to risk of relapse. (b) Placement of calcium hydroxide dressing in the coronal pulp chamber when bleaching procedure has been completed. A final definitive tooth colored restoration can then be placed sealing the coronal pulp chamber permanently - 7.
A small piece of dry cotton wool is placed over the bleach and the cavity sealed with either IRM or glass ionomer cement. The patient is reviewed on a weekly basis and the process repeated until the tooth is slightly overbleached. Usually successful bleaching will become apparent by 2–4 visits.
- 8.
Once bleaching has been completed, the access cavity should be restored with a resin composite which is bonded using an acid etch technique. Optimal time for bonding is usually 3 weeks following completion of bleaching. An interim dressing of calcium hydroxide is recommended during this time period to prevent any bacterial penetration and minimize further the risk of cervical root resorption (Fig. 18.5). A final postoperative clinical photograph should be taken to record colour changes achieved.

Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


