Fig. 24.1
(a–f) Instrumentation for the LeFort I osteotomy. (a) Reciprocating saw with irrigation (Aesculap). (b) Guarded septal and nasal osteotomes. (c) Kawamoto osteotome. (d) Rowe forceps with rubber guard on the palatal arm. (e) Nestor (blunt, heavy, periosteal elevator modified by Jack Nestor Engineering, Inc., Miami, Florida). (f) Expansion forceps
Sectioning of the palatine bone, the sole attachment of the maxillary tuberosity to the pterygoid plate of the sphenoid, follows. The lateral osteotomy can be taken a bit farther back by a few taps on a straight osteotome, and the medial antral wall can be further sectioned with a guarded nasal osteotome.
At this point, the only remaining attachment of the lower maxillary segment is the posterior wall of the antrum, and firm, downward finger pressure on the maxilla is usually enough to produce a down-fracture. If not, the forceps can be inserted underneath the nasal mucosa and the maxilla completely mobilized with a downward and side-to-side motion. It can be further mobilized with a blunt elevator used as a lever.
The maxilla is then placed in the desired occlusal relation with the mandible, and both jaws are placed in the desired relationship with the rest of the face. An autogenous iliac or cranial bone graft is used when the face is to be lengthened, when the degree of maxillary advancement is more than 5 mm, or when the patient has a cleft. If the maxilla is shortened, the resected bone is placed over the osteotomy lines.
Sometimes the alveolus is intact, but the maxilla needs to be expanded, as may occur in a cleft patient who has a buccal crossbite and an alveolar cleft. This procedure is easily performed from above the hard palate, and the palatal mucosa is kept intact if possible. The sectioning is performed with the reciprocating saw, and an elevator is inserted to gently pry the two segments apart. Expansion forceps can be used if required. If the palatal mucosa absolutely prevents expansion, it is divided, creating an alveolar and anterior palatal cleft.
If there is an alveolar cleft to begin with, the two maxillary segments are handled independently and brought into proper occlusion with the mandible. The palatal cleft-nasal floor defect is bone-grafted, and if necessary a transportation flap is developed from the buccal sulcus (Burian) to close the palatal defect. In rare instances, a tongue flap is required. The nasal lining, which will have been carefully dissected at the beginning, is closed before the palatal bone graft is inserted.
The procedure has now been refined to the stage that is the same regardless of whether the alveolus was initially intact. Miniplates are placed between the upper and lower portions of the maxilla for rigid fixation. If bone grafts are required, they are placed either between or over the bone cuts.
If the desired maxillary advancement measures more than 6 mm, bone grafts can be wedged into the pterygomaxillary gap. This step is facilitated by using a traction wire placed through the thick bone beneath the nasal spine. The wire is used to pull the maxilla to the opposite side, which opens the gap and allows impaction of the bone graft. Circumzygomatic wires are almost never used, because they pull the maxilla back, they are too long (long wires can “stretch” more than short wires), and they do not prevent the anterior maxilla from rocking downward.
Wolfe (1989) uses an iliac or cranial bone graft on all cleft patients, as these patients are likely to have a maxillary relapse. Generally, the bone can also be used as an onlay to fill out a deficient maxilla. If the advancement is less than 5 mm, bone is placed only over the anterior osteotomies and in the alveolar and palatal cleft, if present.
The use of anything other than a fresh autogenous bone graft is unsafe. It takes about 15 min to harvest the needed amount of iliac or cranial bone. In the former case, the patient will be comfortable as far as the hip is concerned within 1–2 weeks. By this time, the autogenous graft will have consolidated. With cadaver or demineralized bone or with hydroxyapatite, consolidation may require months, or may never occur.
Like the sagittal splitting procedure for the mandible, the LeFort I osteotomy, once mastered, can provide a solution to a number of maxillary problems. After the horizontal osteotomy, down-fracture, and mobilization, the maxilla can be:
1.
Advanced directly with or without a bone graft (in the noncleft class III patient).
2.
Advanced, or advanced and expanded transversely, with a bone graft (in the cleft patient).
3.
Moved superiorly after resection of a measured amount of maxilla above the horizontal osteotomy (in cases of “long face,” resulting from vertical maxillary excess).
4.
Moved inferiorly with a bone graft (in cases of “short face,” or vertical maxillary deficiency).
5.
Sectioned into multiple segments with teeth (Wassmund or Schuchardt procedure, done from above).
6.
Moved directly backward, although this is difficult to do. (The resection should be of the maxillary tuberosity after extraction of the third molars rather than of the pterygoid plate.) The same result can generally be achieved by an associated segmental osteotomy performed more anteriorly.
With the maxilla in the down-fractured position, multiple osteotomies can be performed from above, which, coupled with or without dental extractions, permit the dental correction of complex malarrangements of the maxilla in one stage. The circulation of blood to the anterior segment comes entirely through the palatal mucoperiosteum, and one must be certain that there are no protrusive edges from the occlusal splint to impinge on the anterior palate. Any number of transverse sagittal osteotomies can be performed, depending on the requirements of the individual case.
Attempts to treat an anterior open bite by mandibular ramus osteotomies are often unsuccessful due to relapse caused by the predominance of the masticatory muscles. Anterior segmental osteotomies of the mandible are appropriate when there is dental crowding and a downward angulation of the mandibular occlusal plane.
The Schuchardt procedure can be used to shorten posterior maxillary height, but it is rarely used in the USA because it requires either an interdental osteotomy or a tooth extraction (Fig. 24.2).
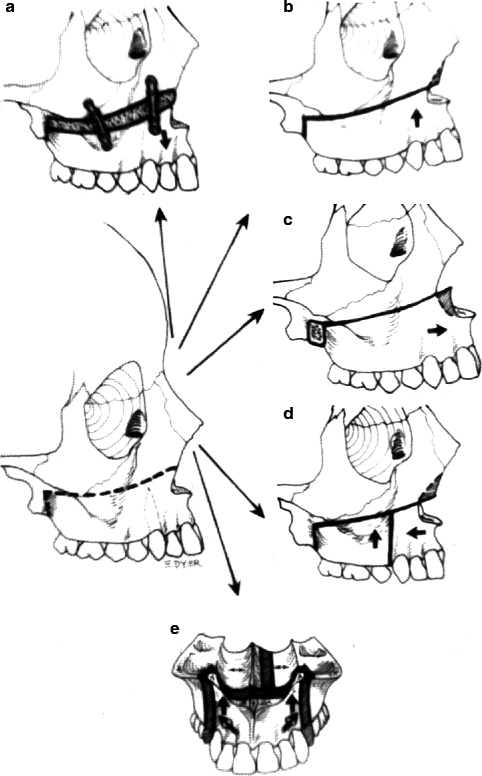

Fig. 24.2
LeFort I surgical procedures: various directions the maxilla can be moved. (a) Inferiorly: requires bone grafts to maintain the new position. (b) Superiorly: no grafts required. (c) Forward: requires a posteriorly supporting bone graft. (d) The posterior segment is moved superiorly while the anterior segment is moved posteriorly. When the premaxilla is retruded it usually needs to be surgically widened through the midpalatal suture between the central incisors to maintain good cuspid interdigitation. (e) The premaxilla moved superiorly
If the orthodontist can level the maxillary occlusal plane, even by accentuating the open bite, the simplest and most stable solution is the LeFort I osteotomy. If the position of the maxillary central incisors relative to the lower vermilion border of the upper lip is satisfactory beforehand, this relationship is preserved. If desired, the maxillary incisors can be raised or lowered relative to the upper lip.
After the maxilla has been completely mobilized, intermaxillary fixation is established and the maxillomandibular complex seated with firm upward and posterior pressure to set the condyles. Appropriate resection of the posterior and, if necessary, the anterior maxilla is performed until the desired anterior maxillary height is obtained. Stabilization of the maxillary osteotomy is then performed with miniplates, and the intermaxillary fixation, if utilized, is temporarily discontinued to evaluate the occlusal relationship with the patient; head in a fixed position. This examination will reveal whether the condyles were inadvertently pulled out of the glenoid fossae. A Class II relationship indicates that the maxilla must be posteriorly repositioned, either by resecting a portion of pterygoid plates (which is difficult) or by extracting the maxillary third molars and resecting a portion of the maxillary tuberosity (which is easier) (Figs. 24.2 and 24.3).
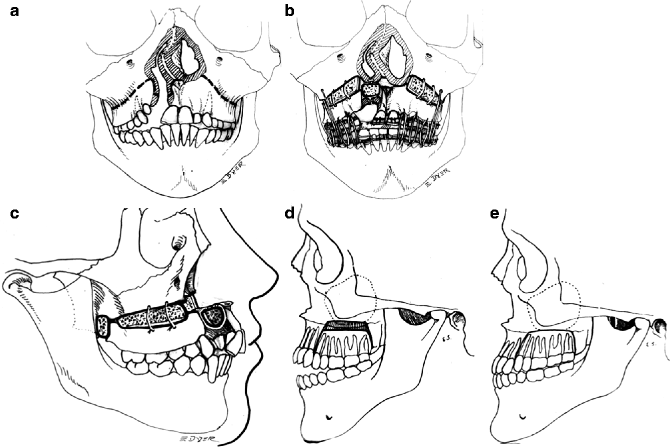

Fig. 24.3
(a) Initial incisions for LeFort I surgery with a secondary alveolar bone grafting to be performed simultaneously. (b) The maxilla is moved inferiorly with bone grafts placed at the surgical cite to support the lengthened maxilla. Alveolar bone graft placed from the nasal aperture to the alveolar crest. Prior to the use of metal plates (rigid fixation) steel sutures were used to stabilized the separated segments. An acrylic surgical wafer is used to position the bony segments according to prior mock surgery performed on plaster casts. Intermaxillary fixation of the maxilla to the mandible using intermaxillary rubber bands for 4–6 weeks is recommended in cases with severe palatal scarring in conjunction with the use of rigid fixation. (c) Lateral view shows a bone block placed between the perpendicular plates of the sphenoid and the maxillary tuberosity with a bone graft to the premaxillary–maxillary junction. (d) Buccal segments are superiorly positioned to permit mandibular auto-rotation and reduction of the anterior open bite. (e) Posterior maxillary impaction to close an open bite (Schuchardt). Buccal segments are superiorly positioned to permit mandibular auto rotation and closure of an anterior open bite
24.2 Stability of Maxillary Advancement
A disappointing yet frequent sequel to orthognathic surgery to advance the maxilla is its partial or complete return to the original state (relapse). The maxillary advancement occurs within a limiting soft tissue envelope (the skin and muscles). Mandibular advancement surgery, especially when it involves the mandibular ligaments, has a great tendency to relapse. The degree of relapse is often judged by measuring occlusal or skeletal landmark changes.
Hochban et al. (Hochban et al. 1993) in a review of the literature reported that the use of miniplates (in rigid fixations) is superior to wire fixation in overcoming the tendency to relapse. Currently, most reports favor the use of miniplates (Ward-Booth et al. 1984; Houston et al. 1989; Champy 1980; Horster 1981; Luyk and Ward-Booth 1985; Rosen 1986). Proffit and Phillips (1987) found a skeletal relapse at 32 % after midface advancement using wire fixation compared with 25 % after miniplate fixation.
Some investigators believe that the amount of relapse is directly related to the amount of advancement (Wolfe and Berkowitz 1989; Houston et al. 1989; Carpenter et al. 1989), whereas others think there is no correlation between displacement of the maxilla and relapse (Rosen 1986; Proffit and Phillips 1987; Iannette et al. 1989). Proffit and Phillips also believe that it is important to achieve excellent occlusion following the operation to reduce the tendency to relapse. Epker (Epker 1981) suggests that interpositioning of bone grafts increases stability by enhancing bony consolidation.
It is generally accepted that the tendency toward relapse starts immediately after surgery and continues for up to about 6 months after the operation. After about 1 year, the correction can be considered stable (Houston et al. 1989; Epker 1981; Teuscher and Sailer 1982; Persson et al. 1986). Hochban et al. (1993), in an excellent review of the subject of postoperative maxillary relapse, reported cephalometric analyses of 31 patients preoperatively, postoperatively, and 1 year later. Fourteen patients had clefts of the lip and palate; the others were noncleft patients with maxillary deficiency. All had maxillary advancement by LeFort I osteotomy and miniplate fixation. Hochban et al. (1993) found that the amount of relapse was between 20 and 25 % in the cleft group and about 10 % in the noncleft group. The degree of relapse was related to the amount of advancement, thus confirming the earlier work by Rosen (1986) and Houston et al. (1989). The authors recommended surgical overtreatment and a good overbite–overjet relationship after orthodontic treatment.
Berkowitz sometime uses very light Class III elastics for 6 months to improve bony consolidation when he notices a maxillary relapse occurring. He believes that the muscular drape to the midface changes very slowly in adapting to skeletal changes, and therefore, some overtreatment is necessary in all instances.
Posnick and Ewing (1990) studied the outcomes in 30 adults and adolescents judged skeletally mature, who had unilateral cleft lip and palate and underwent LeFort I advancement. This group was investigated to determine the amount and timing of relapse, the correlation between advancement and relapse, the effect of performing multiple jaw procedures, the effect of different types of bone grafts, the effect of pharyngoplasty in place at the time of osteotomy, and the effectiveness of various methods of internal fixation. Friehofer (1977), also presented results of maxillary advancement in adolescence.
Tracings of preoperative and serial postoperative lateral cephalograms were digitized to calculate horizontal and vertical maxillary changes. No significant differences in outcomes were seen between patients who had maxillary surgery alone and those who had operations on both upper and lower jaws, nor did the outcomes vary significantly with the type of autogenous bone graft used or the segmentalization of the LeFort I osteotomy. Average “effective” advancement was greater both immediately and 2 years after surgery in patients who did not have a pharyngoplasty in place before the operation.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


