Impressions and Soft Tissue Management
Tom Giblin
Principles
When fabricating indirect restorations, the fit and accuracy are only as good as the impression that the clinician makes. The principles of making a good impression are the same whether performing traditional impressions or with the latest digital impression technologies: healthy tissues, sufficient tissue retraction, identifiable margins, a dry field, appropriate impression material and good impression technique.
Tooth and Periodontal Health
Good periodontal health aids in restorative success by ensuring that the gingival levels are healthy and stable, the teeth are periodontally sound with minimal movement, and there is no bleeding when attempting to make impressions or cement the final prosthesis.
Subgingival Margins
Traumatising the gingiva during tooth preparation should be avoided. A deep margin may also make it difficult to ensure complete excess cement removal.
Gargiulo et al. described the attachments of bone and soft tissues around teeth in 1961.1 Placement of a subgingival margin may impinge on the biologic width. This has been addressed in Chapter 4.1. If the preparation violates the attachment of the tooth, a phenomenon called biologic width impingement occurs, a chronic inflammatory response that results in the soft tissues around the area being constantly red, inflamed and prone to bleeding. As a general rule, margins should be kept 3 mm from the bony crest to restorative margin, confirmed by bone sounding if necessary.
High, Normal and Low Crest
When assessing periodontal tissues, it is important to establish how stable the tissues are. Kois described the stability of gingival tissues in relation to the underlying bone levels.2 This is measured by bone sounding to the bony crest and measuring the distance to the gingival margin. Normal crest patients (3 mm from gingival margin to the crest of the bone) have normal biologic width, the bone levels are normal and the gingival margins should be stable. In high crest patients (<3 mm from gingival margin to bone), the alveolar bone sits very close to the cemento-enamel junction (CEJ) and may require crown-lengthening surgery to ensure that the biologic width is not invaded. In a low crest patient (>3 mm from gingival margin to bone), the alveolar bone is significantly below the CEJ, which may cause instability of the gingival tissues, and possibly recession even with the lightest of trauma, such as occurs when preparing teeth or placing retraction cord.
Tissue Biotype
Thin tissues may be susceptible to recession associated with the trauma of preparations and impressions more than thicker tissue types. An easy determinant of this was described by Cook et al. and involves the placement of a periodontal probe into the sulcus and assessing whether or not it is visible through the tissues.3
Retraction
The first requirement for a good impression is that the margin be free of soft tissue, blood and moisture. In order to achieve this, the dentist may either prepare the margin supragingivally, so that there is no tissue touching the margin, or use retraction cord or paste to reflect the tissues away from the margin of the tooth to achieve haemostasis and a patent sulcus (Figure 6.4.1).
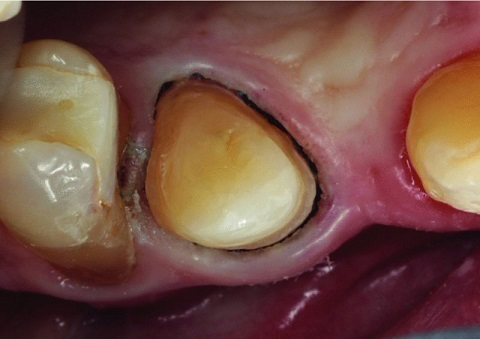
Figure 6.4.1 The aim of retraction is to displace tissues away from the margin and establish a moisture free sulcus to allow impression material to flow freely in
Retraction cord is placed into the sulcus surrounding a tooth to displace the soft tissues physically out of the way. This produces a ‘void’ between the tooth and soft tissue in which the impression material can be placed to ensure capture of the preparation margin. Donovan states that a void of 0.2 mm is required to give an adequate amount of impression material bulk.4 This not only ensures that the material does not tear on retraction due to being too thin, it also allows better definition of the margin in the laboratory, making trimming the die easier and more predictable for the laboratory technician.
There are different types of cord available: twisted, knitted or braided cotton. However, the main characteristics required of them are to be easy to pack, to maintain their volume, not to stick to or tear the tissues and to act as a reservoir for astringent materials. There are different techniques and combinations of cord used depending on preference, but a common one is a two-cord technique.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


