Fig. 2.1
Example of a computer-based caries risk model (Cariogram). After input, the computer is weighting preselected algorithms on bacteria, oral hygiene, circumstances, and susceptibility toward each other. The green sector indicates that this patient only has 17 % chance to avoid new caries in the near future and that the major cause is a sugar-rich diet (blue sector). The program is interactive for patient education and motivation. It can be downloaded free of charge in many different languages at www.mah.se
2.3 Common Research Designs
There are two principal study designs utilized to investigate the relationship between general diseases and dental caries; case–control and observational studies (Fig. 2.2a, b). The case–control approach is most common and starts with the selection of subjects with a defined disease (cases) and subjects without this disease (controls). The prevalence of caries can be compared in a cross-sectional way, and explanatory variables, or factors related to both the general disease and caries, can be collected retrospectively through a review of medical and dental records. This approach is easy to implement but the quality is strongly dependent on the matching process and the validity of the “historical” registrations. In a trustworthy study, the cases and the controls must be carefully matched for sex, age, socioeconomic and educational background, cultural norms, and lifestyle. The fact that case–control studies many times are presenting conflicting results is likely due to inadequate matching. Other problems that may flaw the conclusions are small sample sizes and diverging disease definitions for the “cases.” From an evidence point of view, the prospective observational study design is more robust and controllable for the researcher but requires a considerable budget and time; a large number of patients must be included and followed for years with periodical reexaminations. The major threat for reliable conclusions is a large attrition rate (lost to follow-up) and/or a low incidence rate of the disease under study. A power calculation must therefore be conducted prior to the study in order to include a proper number of subjects. From an ethical point of view, it is equally problematic to run a project with too few persons as it is to enroll too many in demanding examinations and samplings. A mix of the abovementioned study designs is the nested case–control approach in which only a few defined cases and controls are selected from the full cohort. The main advantage is that not all patients must be sampled or examined over time which keeps down the workload and costs for an otherwise costly and resource-demanding trial.
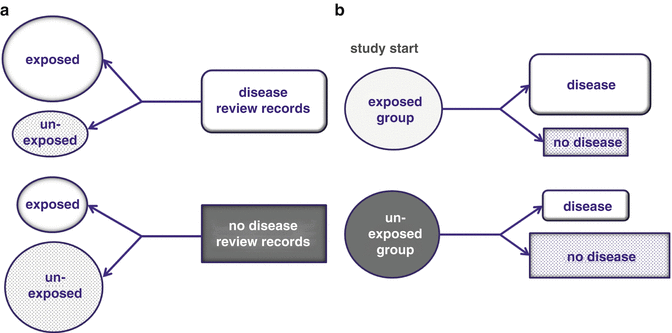

Fig. 2.2
(a) A case-control study begins by selecting subjects with disease (cases) or no disease (controls). (b) An observational study begins with exposure and the outcome is registered by time
2.4 Obesity/Overweight
Obesity and overweight is a growing problem among children and adults worldwide. The etiology is complex but overeating and calorie-rich diets are common compartments. A frequent intake of sucrose-containing food and beverages may be detrimental for the dental health (Arola et al. 2009). The relationship between sugar and caries is however not as strong today as it was decades ago which is commonly explained by the widespread access to fluoride in water and toothpaste. From the evidence perspective, it is beyond doubt that fluoride exposure is the key element in caries prevention and caries arrest at all ages throughout life (Griffin et al. 2007; Twetman and Dhar 2015). The link between caries and overweight in case–control trials is somewhat controversial and highly dependent on inclusion criteria and matching. Even systematic reviews have come to diverging conclusions; one established a significant relationship (OR = 3.7) between obesity and dental caries in children from industrialized, but not from newly industrialized countries (Hayden et al. 2013), while another failed to note any relationship between overweight and caries burden (Silva et al. 2013). A fact that partly can explain the different conclusions is that dental caries may be associated with both high and low body mass index (Hooley et al. 2012). Unfortunately, studies in adults and elderly are largely lacking, but obviously diet recommendations and restrictions in order to reduce weight and prevent caries go hand in hand. Obesity is a part of the metabolic syndrome, and according to the common risk factor approach, dentists, together with all other health professionals, should embrace the current WHO guidelines and motivate their patients to reduce the free sugar intake to less than 10 % of the total energy intake (Moynihan and Kelly 2014). Free sugars include monosaccharides and disaccharides added to foods by the manufacturer, cook, or consumer, and sugars naturally present in honey, syrups, fruit juices, and fruit juice concentrates. A further reduction to below 5 % of total energy intake, or roughly 25 g (six teaspoons) per day, would provide additional health benefits.
2.5 Asthma
Asthma affects 6–8 % of the population and may influence the oral ecology through behavioral and medical pathways. Severe asthma is often associated with dry mouth, thirst, and frequent wake-up periods at night when sugar-rich beverages and fruit juices must be avoided. Furthermore, the steroid-containing inhalators, as well as beta-2 agonists, may have low pH values which favor the growth of acid-tolerating phenotypes in the oral biofilm, and increased levels of mutans streptococci are commonly unveiled in the saliva of asthmatic children (Alaki et al. 2013). Although there are conflicting reports on the relationship between asthma and dental caries in the literature (Maupomé et al. 2010), a meta-analysis has suggested that asthma doubles the risk of caries in both primary and permanent dentition (Alavaikko et al. 2011). Based on 11 studies, the odds ratio was 2.7 in the primary dentition, and the corresponding value in the permanent dentition was 2.0 based on 14 studies (Alavaikko et al. 2011). It was concluded that physicians and dentists should reconsider preventive measures against caries for persons with severe asthma and strongly recommend water rinses immediately after the use of inhalators.
2.6 Diabetes
Diabetes can affect the stability and profile of the oral biofilm through frequent meals and an increased output and leakage of glucose in saliva and gingival crevicular fluid. In the past, when the management of diabetes mellitus in childhood basically relied on slow-acting insulin and a highly restricted diet, subjects with diabetes exhibited less caries than a non-diseased population. With today’s continuous monitoring of glucose, rapid-acting insulin, or insulin pumps, the type 1 diabetic child can live a more or less normal life with a less restricted diet. Furthermore, the oral health awareness among diabetics has increased in recent years with its close link to periodontal problems. Consequently, the results from case–control studies with diabetic patients have therefore slightly changed over time. According to recent systematic reviews, there is no consistent relationship between type 1 diabetes mellitus (T1DM) and dental caries in childhood (Ismail et al. 2015), although patients with uncontrolled T1DM and poor oral hygiene may present increased prevalence of dental caries (Sampaio et al. 2011). It is therefore important to collect information on the patient’s recent HbA1c status; values above 8 % may indicate a poor compliance and may be associated with active caries development in schoolchildren and adolescents (Twetman et al. 2002). Concerning type 2 diabetes mellitus, no impact on the prevalence of dental caries has been reported (Sampaio et al. 2011).
2.7 Congenital Heart Disease
Congenital heart disease affects around 1 % of all children, and the condition is commonly associated with oral health problems. This has been explained by an increased meal frequency, use of diuretic sucrose-containing medication, and frequent episodes of antibiotic treatment (Hansson et al. 2012). In addition, enamel defects and hypomineralization are prevalent in children with congenital heart disease which may predispose to caries development. Parental anxiety and overcompensation with sweets are psychological and behavioral factors often involved in the management of critically ill children. A case–control study has shown that children with congenital heart disease have three times more caries than healthy controls in spite of more prevention (Stecksén-Blicks et al. 2004). In the same study, a positive relationship between caries and the duration of the digoxin medication was established. Thus, a dental home should be established for children with congenital heart disease at an early age in order to implement individual treatment plans with frequent checkups during childhood.
2.8 Cancers
Long-term survivors of malignant conditions are subjected to long-term effects on oral health due to aggressive treatment protocols based on chemotherapy and radiation (Kaste et al. 2009; Effinger et al. 2014). In particular, the radiation therapy affects the salivary gland functions in a permanent or transient way, depending on location and radiation exposure. Consequently, patients who were post-radiotherapy exhibited higher DMFT values (decayed, missing, filled permanent teeth) compared to those who were post-chemotherapy and healthy controls (Hong et al. 2010). There is also data suggesting that children with leukemia displayed more caries than hospitalized children without cancer (Willershausen et al. 1998). However, among children that were caries-free at the onset of leukemia and displayed a low caries risk, the vast majority (87 %) were still unaffected after 3 years (Pajari et al. 2001). This picture seems to be less clear-cut among adults; a study has suggested an inverse relationship between head and neck squamous cell carcinoma and dental caries in a case–control study, although age and social factors may have played a role (Tezal et al. 2013). Nevertheless, patients with cancers should be considered at risk and candidates for saliva-stimulating measures and high-fluoride supplements.
2.9 Cleft Lip Palate
Children with cleft lip palate are often claimed to be caries prone in their maxillary incisors due to compromised tooth brushing during the infant period (Hasslöf and Twetman 2007; Antonarakis et al. 2013). An elevated prevalence of enamel defects may also contribute to caries susceptibility (Sundell et al. 2015). Consequently, it has recently been reported that children with cleft lip palate have more caries in the primary but not in the young permanent dentition compared to non-cleft controls (Sundell et al. 2015). There was however no clear association to the type or localization of the clefts. The increased caries risk must be taken into account by all members of the multi-professional team involved in the management of children with this syndrome.
2.10 Neuropsychiatric Disorders
Neuropsychiatric disorders in childhood may affect the possibilities to conduct a regular and proper oral hygiene. For example, studies in children with ADHD (attention deficit hyperactivity disorder) have suggested a 12-time increased risk for high DMFT values compared to controls that were matched concerning age, gender, ethnicity, and socio-economy (Broadbent et al. 2004, Blomqvist et al. 2011). The findings were adjusted for fluoride exposure, medical problems, diet, and oral hygiene. The neuropsychiatric disorders are however highly diverse and each family/child is unique, so the caries risk must be assessed individually and followed by targeted preventive measures.
2.11 Aging and Cognitive Impairment
There is no evidence to suggest a link between caries and healthy and vital older persons. However, for those with progressive intellectual disabilities and dementia, oral health can rapidly be jeopardized, and root caries development is an atypical and increasing problem (Fiske et al. 2006; Anders and Davis 2010). This is also true for subjects with mental illnesses (Kisely et al. 2011). The main reasons are difficulties to clean and polypharmacy. Alzheimer’s and Parkinson’s disease are common examples on non-regular or sporadic oral cleaning and loss of ability to clean. Saliva plays a crucial role in maintaining oral health through its mechanical clearance, buffering effect, and being a source of mucins, immunoglobulins, enzymes, and antibacterial agents (Sreebny 2000). Increasing age means an increasing number of prescribed drugs that when combined in a “cocktail” very well can be xerogenic. Even a modest reduction of the unstimulated saliva secretion rate can have a strong impact on root caries development. It is therefore important to assess salivary gland function in elderly people and especially in frail elderly with diminishing autonomy. A sialometry can be helpful for motivating the patient to benefit from saliva-stimulating measures.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


