Clinical Assessment of Periodontal Tissues
Jorge André Cardoso
Principles
Periodontal tissues play an important role in the appearance of a smile (Figure 4.1.1). While teeth contribute to the ‘white’ aesthetics, the periodontal soft and supporting hard tissues form an important tridimensional architecture that can be referred to as the ‘pink’ aesthetics.
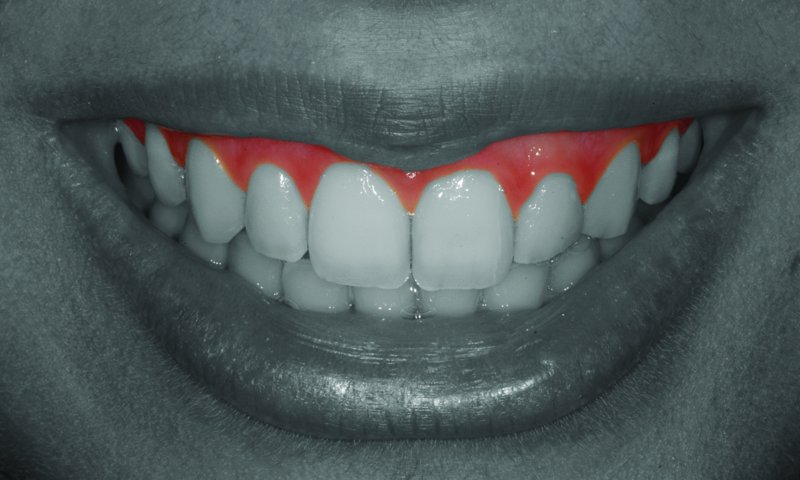
Figure 4.1.1 The periodontal tissues play a major role in the aesthetics of the smile
The periodontal assessment is fundamental for disease diagnosis as well as for recognising some parameters that will largely influence the aesthetic possibilities and treatment plan. A specific appointment for an initial examination that includes periodontal parameters is essential for patient assessment.
Although the main cause of periodontal disease is the presence of dental plaque, several risk factors have been recognised, such as smoking, diabetes and stress.1 Any genetic or systemic condition that affects the host immunological response can also increase a patient´s risk.2 A possible link between periodontal disease and cardiovascular disease has been considered, although this correlation is not entirely clear.3 For all of these reasons, a detailed clinical history is important for a correct assessment.
Additionally to the traditional periodontal assessment, in aesthetic practice the position of pink tissues needs be carefully examined. Since the periodontal tissues surround the dental tissues, any change in soft tissues will have a significant impact on the patient’s smile. The appearance of a tooth’s length is largely dependent on the correct position of soft tissue. If gingival recession is present it can cause a tooth to appear longer. In the same way, if too much soft tissue is covering a tooth, it will appear shorter.
Gingival Exposure during Smile
One of the first parameters to consider in periodontal aesthetics is the overall amount of gingival tissue showing above upper anterior teeth while the patient smiles (Figure 4.1.2). Kokich et al.4 suggest that 1–3 mm of gingival exposure should be present during smile. The gingival level of upper centrals and canines should be approximately the same, while laterals should be about 1 mm shorter. The premolar margin is usually 1 mm shorter than the canine margin and this level is maintained through the posterior maxillary teeth.
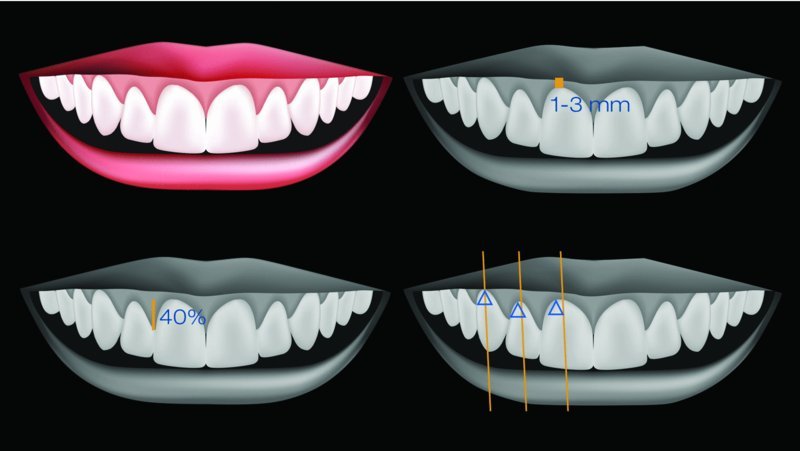
Figure 4.1.2 The main aesthetic parameters in periodontics: gingival exposure during smile, papillae proportions and location of gingival zenith
Gingival Margins and Zenith Points
It may seem obvious, but it is worth remembering that the gingival margins set the tooth´s appearance and size in the apical zone. The gingival zenith can be defined as the most apical position of the gingiva in a tooth. Therefore, it sets the tooth’s apical limits and greatly influences the perceived shape of the tooth. This position should not be the same in every anterior tooth. If we divide each anterior upper tooth in half at its long axis (and these axes are not vertical), the zenith is about 1 mm distal to that line in centrals, 0.5 mm distal in laterals and more or less coincident in canines. This soft-tissue configuration seems to provide a natural and aesthetically pleasing situation.5
Gingival Papillae
According to Chu et al.,6 the papillae tissue occupies 40% of the distance between the zenith and the incisal edge of a tooth. The biological factors that determine the presence of the papillae are directly related to the underlying interproximal bone level.
It is also important to evaluate the relation between the periodontal tissue and any future restorative procedures that are planned. This is usually called the perio-restorative interface and is key for the successful aesthetic and biological integration of any restorative work to be carried out.
Dentogingival Complex (Biologic Width and Gingival Sulcus)
Biologic width is the human body interface that separates the alveolar bone from the oral cavity.7 It is an important area where internal tissues defend themselves from external aggression, just like in every mucosa of the body. Together with the gingival sulcus, it forms the dentogingival complex. Although there are significant variations, the average proportion of this complex is 3 mm,8–10 distributed according to the parameters in Table 4.1.1 and Figure 4.1.3.
Table 4.1.1 Dentogingival complex dimensions in a healthy individual (no presence of periodontal disease)
| Average | Range | ||
| Connective tissue | 1 mm | ||
| Biologic width | 0.5–4 mm | ||
| Junctional epithelium |
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


