http://evolve.elsevier.com/Haveles/pharmacology
This chapter discusses treatment and management of fungal and viral infections commonly encountered in the dental office: the fungus Candida albicans (candidiasis or thrush) and the herpes simplex virus. The viral infection acquired immunodeficiency syndrome (AIDS) and the different types of hepatitis (B, C) are discussed with reference to factors that might affect dental treatment.
Antifungal agents
Fungal infections are not often encountered in dental practice, but when they are present, they are often difficult to treat. In comparison with bacterial infections, fungal infections are more insidious. Fungal infections are more likely to occur in patients who are immunocompromised, and these infections can become chronic. Fungal infections can be divided into those that affect primarily the skin or mucosa (mucocutaneous) and those that affect the whole body (systemic). The dental hygienist usually treats skin or mucosal lesions, most commonly within the mouth. These mucosal lesions may be treated with a topical or systemic antifungal agent.
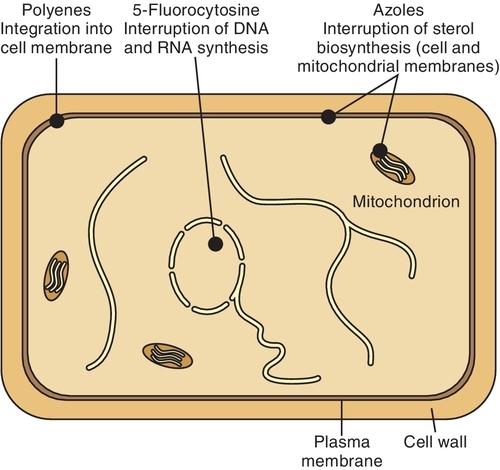
Although there are different groups of fungi, two common groups are candida-like and tinea. Dental hygienists manage oral candidal infections, primarily caused by C. albicans, with nystatin, clotrimazole, ketoconazole, or fluconazole (Table 8-1). Figure 8-1 reviews where these drugs work on the fungal cell.
Table 8-1
Dentally Useful Antifungal Agents for Oral Candidiasis

N/A, not available; qid, four times a day.
* Sucrose.
† 0.4 g sucrose + 0.8 g glucose.
‡ Glucose.
Nystatin
Nystatin (nye-STAT-in) (Mycostatin, Nilstat) is a prescription antifungal agent that is produced by Streptomyces noursei. Its mechanism of action involves binding to sterols in the fungal cell membrane. This binding produces an increase in membrane permeability and allows leakage of potassium and other essential cellular constituents.
Nystatin is not absorbed from the mucous membranes or through intact skin; taken orally, it is poorly absorbed from the gastrointestinal tract. In usual therapeutic doses, its blood levels are not detectable. When administered orally, it is not absorbed but is excreted unchanged in the feces. Nystatin is fungicidal and fungistatic against a variety of yeasts and fungi. In vitro, nystatin inhibits C. albicans and some other species of Candida.
The adverse reactions associated with nystatin are minor and infrequent. Applied topically or taken orally (through the gastrointestinal tract), there is little if any absorption. When higher doses have been used, nausea, vomiting, and diarrhea have occasionally occurred. Rarely, hypersensitivity reactions have been reported.
Nystatin is used for both the treatment and the prevention of oral candidiasis in susceptible patients. Although C. albicans is a frequent inhabitant of the oral cavity, only under unusual conditions does it produce disease. Often, patients affected are immunocompromised.
For the treatment of oral candidiasis, nystatin is available (see Table 8-1) in the form of an aqueous suspension (100,000 U/ml) containing 50% sucrose. The aqueous suspenison should be used as a rinse and expectorated. The aqueous suspension can also be frozen and used as a popsicle. Swallowing the suspension will not cause harm because it is not absorbed by the gastrointestinal tract and it will not eradicate pharyngeal candidiasis either. If diabetic patients swallow the suspension, they must take the sugar content into account (2.5 g sucrose per tsp) when planning their meals and insulin use.
Nystatin pastilles are licorice-flavored, are rubbery, and also contain sugar. The advantage of this preparation is that it takes 15 minutes for the lozenge to dissolve in the mouth, thus bathing lesions in the antifungal agent for a longer period than with the aqueous solution. It is dissolved in the mouth four times daily. The dental hygienist must discuss patients’ oral health habits, especially when patients are ingesting these cariogenic agents over the long term.
Nystatin is available in vaginal tablets for use in vaginal infections. Occasionally, these vaginal tablets can be used orally. They are dissolved in the mouth four times daily. The advantages of the vaginal tablet used as a lozenge are that the drug remains in contact with the infected oral mucosa longer than it does when in the suspension form and it contains no sugar so may be ideal for patients with diabetes. The disadvantage is that it is not flavored for oral use.
Table 8-2 reviews the dosing instructions for the different nystatin preparations. Denture stomatitis can be treated by applying a thin layer of nystatin cream to the tissue side of the denture. Patients should be instructed to use the nystatin product for 10-14 days, depending on the severity of the infection, or for 48 hours after the signs and symptoms of the infection have been eradicated.
Table 8-2
Nystatin Dose Forms
| Dose Form | Instructions for Use |
| Aqueous suspension (100,000/ml) | Children and adults: Swish, swirl (hold in mouth for 5 minutes), expectorate or swallow 4-6 ml 4-5 times daily. Freeze 2.5 ml into popsicle form. Place in the mouth and allow to completely dissolve. This should be done 5 times a day. Infants: Administer 2 ml 4 times daily; place one half dose in each side of the mouth. Avoid feeding infants for 5-10 minutes afterward. |
| Pastille | Suck on 1-2 tablets 4-5 times daily. |
| Cream | Apply to affected area (including the tissue area surrounding dentures). Insert denture. |
| Vaginal tablets | Can be used as an oral lozenge. Dissolve in the mouth 4 times daily. |
Imidazoles
Imidazoles useful in dentistry include clotrimazole, miconazole, and ketoconazole.
Clotrimazole
Clotrimazole (kloe-TRIM-a-zole) (Mycelex) is a synthetic antifungal agent available in the form of a slowly dissolving, sugar-containing lozenge for oral use. It is also available as an over-the-counter (OTC) cream for topical application to the skin or vaginal canal.
Clotrimazole’s mechanism of action involves alteration of cell membrane permeability. It binds with the phospholipids in the cell membrane of the fungus. As a result of the alteration in permeability, the cell membrane loses its function and the cellular constituents are lost.
Clotrimazole oral lozenges or troches dissolve in approximately 15-30 minutes. Patients with xerostomia may have difficulty dissolving this product. Saliva drug concentrations that are sufficient to inhibit most Candida species are maintained in the mouth for about 3 hours. The drug is bound to the oral mucosa, from which it is slowly released. The amount of clotrimazole absorbed systemically by this route is unknown, but some absorption occurs. Each lozenge also contains 0.9 g of glucose. The spectrum of activity of clotrimazole is primarily against the Candida species.
The most common adverse reactions associated with clotrimazole involve the gastrointestinal tract, including abdominal pain, diarrhea, and nausea. Clotrimazole has been reported to produce elevated liver enzyme (aspartate aminotransferase) values in approximately 15% of patients. It is not recommended for use in pregnant women or in children younger than 3 years.
Clotrimazole is indicated for the local treatment of oropharyngeal candidiasis. Patients should be instructed to dissolve the lozenge in the mouth slowly, like a cough drop, to minimize gastrointestinal discomfort. They should also be told to take all of the medication prescribed to minimize relapse. The usual adult dosage is 1 lozenge (10 mg) five times daily for 10-14 days (or longer for immunosuppressed patients) or for 48 hours after the symptoms have cleared. Clotrimazole can be used to treat denture stomatitis. A thin layer of clotrimazole cream should be applied as a thin layer to the tissue side of the denture base.
Ketoconazole
Ketoconazole (kee-toe-KON-a-zole) (Nizoral), another imidazole used in dentistry, alters cellular membranes and interferes with intracellular enzymes. By interfering with the synthesis of ergosterol, a cellular component of fungi, this agent alters membrane permeability and inhibits purine transport. The imidazoles inhibit the C-14 demethylation of lanosterol, an ergosterol precursor. It also inhibits sex steroid biosynthesis, including testosterone, perhaps by blocking several cytochrome P-450 (CYP-450) enzyme steps.
Ketoconazole is indicated in the treatment and management of mucocutaneous and oropharyngeal candidiasis (oral thrush). It can be used prophylactically in chronic mucocutaneous candidiasis. The most frequent adverse reactions (3%-10%) associated with ketoconazole are nausea and vomiting, which can be minimized by taking ketoconazole with food. The most serious adverse reaction associated with ketoconazole is hepatotoxicity. Its incidence is at least 1:10,000. It is usually reversible on discontinuation of the drug, but occasionally it has been fatal. It is thought to be an idiosyncratic reaction that can happen at any time. With extended use, the patient should have periodic liver function tests (LFTs). Patients taking other hepatotoxic agents, those with liver disease (e.g., alcoholic hepatitis), and those on prolonged therapy should be monitored closely because they may be more susceptible to this hepatotoxicity. Because of its adverse reaction profile, ketoconazole should be used only after topical antifungal agents have been ineffective or if there is reason to believe that they will be ineffective.
Ketoconazole has many drug interactions that have been reported in the literature. Because an acidic environment is required for dissolution and absorption of ketoconazole, agents that alter the amount of stomach acid could theoretically reduce the absorption of ketoconazole (H2 receptor blockers, H+-pump inhibitors, anticholinergic agents, and antacids). At least 2 hours should elapse between the ingestion of these agents and ketoconazole’s administration. Also, ketoconazole and the other imidazoles interact with the anticoagulant warfarin, which may increase warfarin blood levels and increase the risk for bleeding.
The usual adult dose of ketoconazole for the treatment of Candida species is 200-400 mg orally (PO) daily (qd). It should be used for at least 2 weeks, and 6-12 months may be required for chronic mucocutaneous candidiasis. Maintenance therapy may be necessary for certain patients.
Other Imidazoles
Other imidazoles, such as fluconazole (floo-KON-a-zole) (Diflucan), an oral triazole antifungal agent, are used to treat certain fungal infections. Fluconazole prevents the synthesis of ergosterol in the fungal cell membranes by inhibiting fungal CYP-450 enzymes. Phospholipids and unsaturated fatty acids accumulate in the fungal cells.
Fluconazole is indicated for treatment of oropharyngeal and esophageal candidiasis and serious systemic candidal infections. One tablet of fluconazole is now indicated to treat vaginal candidiasis. Fluconazole is used prophylactically against candidiasis in immunocompromised patients or for the treatment of candidal infections that do not respond to other agents.
Antiviral agents
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


