http://evolve.elsevier.com/Haveles/pharmacology
A growing number of older patients who are taking multiple drugs seek dental treatment each year. The demographics of our population, the use of fluorides, and management of periodontal disease have increased the age of the average dental patient. Dental offices are administering more complicated drug regimens; dental appointments are taking longer; and dental patients are on average getting sicker. With these changes, the chance that an emergency will occur in the dental office continues to increase. Both the dentist and the dental hygienist should become familiar with the most common emergency situations, their management, and the drugs used to treat them. When an emergency occurs, the dentist and hygienist working together can increase the chance of producing the best outcome. Many emergency situations can be handled correctly with adequate knowledge. Lack of this knowledge during an emergency may cause panic in a dental office. If the dental office and its personnel are prepared for an emergency, handling one will be easier. Before patients who might be at risk for an emergency arrive for dental care, the treatment of a potential emergency related to their disease should be reviewed. It is the responsibility of each dental health care worker to make sure the members of the team can act in a coordinated manner.
General measures
Steps Indicated
To prepare the dental office for an emergency, the following steps should be taken:
To minimize the chances of an office emergency, the procedures listed in Box 24-1 should be performed for each new dental patient. It is easier to prevent than to treat a dental emergency. If an emergency occurs in the dental office, the steps listed in Box 24-2 should be taken.
Preparation for Treatment
Before any emergency treatment can be administered, investigation of the patient’s signs and symptoms must lead to a diagnosis of the problem. In 2010, the American Heart Association revised its approach to assessing a patient from the traditional “A,B,C—maintenance of the airway (A), respiration (breathing, B), and circulation (C)—to C-A-B: Chest compressions (C) are now performed first, followed by assessment of the airway (A), and then breathing (B). Chest compressions, or hands-on-only CPR, are recommended first because people without training can administer them with guidance via telephone from an emergency medical technician or from a 911 dispatcher (Figure 24-1). The use of drug therapy in these situations is only ancillary to the primary measures of maintaining adequate circulation and respiration. One should remember that drugs are not necessary for the proper management of most emergencies. Whenever there is doubt as to whether to give the drug, it should not be given.

In the dental office, each health care worker should be certified for both CPR and ACLS. The legal implications of lack of CPR training could be serious. ACLS training can be helpful in certain rural situations or if the technique of preoperative sedation or conscious sedation is used in the dental office.
The categories of emergencies are discussed in the next section. The most commonly used drugs and the choice of drugs and equipment for a dental office emergency kit are addressed.
Categories of emergencies
This section discusses the signs, symptoms, and treatment of the most common emergency situations, dividing them into change in consciousness; respiratory, cardiovascular, and other emergencies; and drug-related emergencies.
Lost or Altered Consciousness
Many common dental emergencies involve either unconsciousness or altered consciousness. Dental office personnel should be ready to handle such an emergency and determine the best course of treatment.
Syncope
The emergency most often encountered in the dental office is simple syncope (fainting, also known as vasomotor collapse) or transient unconsciousness. The skin takes on an ashen-gray color, and diaphoresis occurs. The release of excessive epinephrine results in a pooling of the blood in the peripheral muscles (β-adrenergic effect, vasodilation), a decrease in total peripheral resistance, and a sudden fall in blood pressure. A reflex tachycardia follows, but soon, decompensation results in severe bradycardia. These effects are brought about by anxiety, fear, or apprehension, all of which are common in a dental situation. Treatment involves placing the patient in the Trendelenburg position (head down) (Figure 24-2), causing blood to rush to the head, which has the effect of giving the patient a transfusion of whole blood.
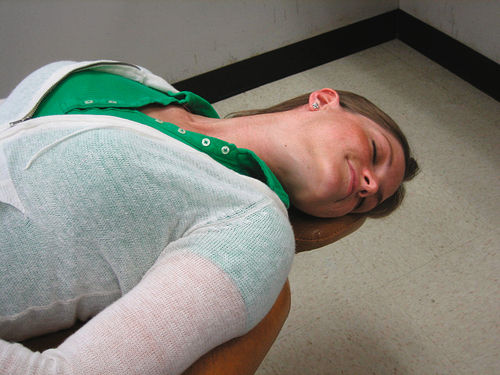
The most important component in the treatment of syncope is for the dental health care worker to exhibit confidence in action and voice. If the hygienist shows control over the situation, the patient will be less anxious and apprehensive and less likely to repeat the syncopal attack.
Spirits of ammonia can be administered by inhalation. The old practice of putting the head between the legs should be avoided because venous return is cut off by the slumped position.
Hypoglycemia
The most common cause of hypoglycemia is an excessive dose of insulin in a patient with diabetes. The medical history in this case is important, so the dental health care worker can determine the dose and type of insulin and food intake before the appointment. Often, patients inject their usual daily dose of insulin but fail to eat before coming to the dental office. If this is the case, then patients should be asked to eat before any dental procedures are begun. The time of the hypoglycemia can be estimated from knowledge of the peak effect of the particular insulins used (see Chapter 21).
The patient with hypoglycemia has a rapid pulse and decreased respiration and is very talkative. Hunger, dizziness, weakness, and occasionally tremor of the hands can occur. Diaphoresis, nausea, and mental confusion are other signs of hypoglycemia. If the signs of hypoglycemia are recognized before they become severe, the patient can be given a sugary drink or oral glucose. If the patient lapses into unconsciousness and has no swallowing reflex, dextrose must be given intravenously.
Diabetic Coma
Less common than hypoglycemia, the diabetic coma is caused by elevated blood sugar. The symptoms frequent urination, loss of appetite, nausea, vomiting, and thirst are seen. Acetone breath, hypercapnia, warm dry skin, rapid pulse, and a decrease in blood pressure can occur. Treatment is undertaken only in a hospital setting and involves administration of insulin after proper laboratory results are obtained (blood glucose).
Seizures
Seizures are most commonly associated with epilepsy, especially the grand mal type (see Chapter 16), but they can also result from a toxic reaction to a local anesthetic agent. Seizures are abnormal movements of parts of the body in clonic and/or tonic contractions and relaxations. The patient may become unconscious. Generally, seizures are self-limiting, and treatment should consist of protecting the patient from self-harm, moving any sharp objects out of the patient’s reach, and turning the patient’s head to the side to prevent aspiration. In some situations, diazepam may be administered intravenously, but observation of the patient is often sufficient.
Respiratory Emergencies
Respiratory emergencies involve difficulty in breathing and exchange of oxygen. They include hyperventilation, asthma, anaphylactic shock, apnea, and acute airway obstruction.
Hyperventilation
Hyperventilation is one of the most common dental emergency situations. The increased respiratory rate is often brought on by emotional upset associated with dental treatment. Tachypnea, tachycardia, and paresthesia (tingling of the fingers and around the mouth) have been reported. Nausea, faintness, perspiration, acute anxiety, lightheadedness, and shortness of breath can also occur. The treatment is calm reassurance. Position the patient upright, loosen tight clothing, and work with the patient to control breathing.
Asthma
Normally, patients who have acute asthmatic attacks have a history of previous attacks and carry their own medication. The most common sign of an asthmatic attack is wheezing with prolonged expiration (squeak). The patient’s own medication (multidose inhalers containing β2-agonist such as albuterol) should be used first. The dose should be repeated two times. If there is no response to these, hospitalization for administration of aminophylline (parenteral or oral) and parenteral corticosteroids and epinephrine should be considered. Oxygen should also be administered.
Anaphylactic Shock
The most common cause of anaphylactic shock is an injection of penicillin, although anaphylactic reactions have also been caused by many other agents. Examples are eating peanuts and being exposed to latex rubber items. The reaction usually begins within 5-30 minutes after ingestion or administration of the antigen. Usually, a weak, rapid pulse and a profound decrease in blood pressure occur. There is dyspnea and severe bronchial constriction.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


