Chapter 9
Guided Tissue Regeneration
HISTORY
Guided tissue regeneration (GTR) is defined by the American Academy of Periodontology as a procedure attempting to regenerate lost periodontal structures through differential tissue responses (American Academy of Periodontology 1996). It involves the use of resorbable or nonresorbable barriers (membranes) to exclude epithelial and connective tissue cells from the root surface during wound healing. This is believed to facilitate the regeneration of lost cementum, periodontal ligament, and alveolar bone. In theory, this technique should result in reconstructing the attachment apparatus rather than just root coverage.
The membranes used during this procedure are most commonly made of materials such as expanded polytetrafluoroethylene (ePTFE), polyglactic acid, polylactic acid, and collagen. Pini-Prato et al. (1992) and Tinti & Vincenzi (1994) reported the use of an ePTFE membrane to treat gingival recessions. Cortellini et al. (1993) conducted a histological study on a patient, demonstrating that the root coverage obtained with the use of an ePTFE membrane, while treating a gingival recession, led to new connective tissue attachment and new bone formation. In 2001, Harris, while examining the histology of four teeth with gingival recessions treated with GTR, reported healing with a long junctional epithelium attachment without regeneration.
INDICATIONS
- Moderate to severe gingival recessions
- Thin palate
- Patient reluctant to have a second surgery site
ARMAMENTARIUM
This includes the basic surgical kit plus the following:
- Barrier membrane: resorbable (e.g., Resolut (W.L. Gore, Flagstaff, AZ, USA) XT, XTN2, or XTW1 and/or nonresorbable (e.g., Gore-Tex titanium reinforced TRN2, TRW2 or GTN1, GTN2, GTW1, or GTW2)
- Citric acid, pH 1 (40%), or 1 capsule of tetracycline hydrochloride (HCl), 250 mg
GUIDED TISSUE REGENERATION FOR ROOT COVERAGE
Technique
After proper anesthesia (Fig. 9.1), the recession is root planned thoroughly and flattened using a Gracey (Hu-Friedy, Chicago, IL, USA) curette or a back-action chisel (Fig. 9.2). The root is conditioned for 5 min with tetracycline paste. Two vertical releasing incisions are made at the line angles of the tooth with the recession (Fig. 9.3). These releasing incisions must pass the mucogingival junction for the flap to be mobile.
An intrasulcular incision connects the two verticals coronally. A full-thickness flap is raised using a periosteal elevator (24G) (Hu-Friedy) that will enable bone visibility 3 mm apical to the exposed root (Fig. 9.4). The flap is then converted to a partial thickness one apically that will enable coronal mobilization.
Figure 9.1. Tooth 11 with a moderate gingival recession.
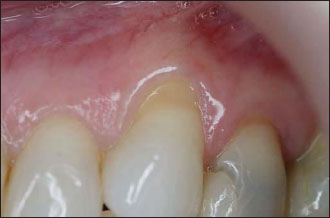
Figure 9.2. The exposed root surface is thoroughly scaled with a back-action chisel.
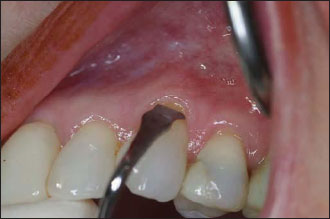
Figure 9.3. Two vertical incisions are placed, avoiding the interproximal papillae.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


