Chapter 7
Pedicle Grafts: Rotational Flaps and Double-Papilla Procedure
HISTORY
Grupe & Warren were the first to describe the sliding flap as a method to repair isolated gingival defects (1956). They reported elevating a full-thickness flap one tooth away from the defect and rotating it to cover the recession. In 1967, Hattler reported the use of a sliding partial thickness flap to correct mucogingival defects on two or three adjacent teeth.
In 1968, Cohen & Ross, using the interproximal papillae to cover recessions and correct gingival defects in areas of insufficient gingiva not suitable for a lateral sliding flap, described the double-papilla repositioned flap. This technique offers the advantages of dual blood supply and denudation of interdental bone only, which is less susceptible to permanent damage after surgical exposure. A full-thickness or partial thickness flap may be used. The latter is preferable because it offers the advantage of quicker healing in the donor site and reduces the risk of facial bone height loss, particularly if the bone is thin or the presence of a dehiscence or a fenestration is suspected (Wood et al. 1972).
Indeed, Wood et al. (1972) reported increased bone at healing time with a partial thickness flap as opposed to a full-thickness flap (0.98 mm versus 0.62 mm). The advantage of the pedicle graft versus the free gingival autograft is the presence of its own blood supply, in the base, that will nourish the graft and facilitate the reestablishment of vascular anastomoses at the recipient site during the healing phase.
INDICATIONS
- Inadequate amount of attached gingiva
- Single or multiple adjacent recessions that have adequate donor tissue laterally (root coverage)
- Recession next to an edentulous area
PREREQUISITES
- Thick periodontal biotype
- Preferably deep vestibule
ARMAMENTARIUM
This includes the basic surgical kit for the lateral sliding and obliquely rotated flaps. For the double papilla, add:
- Tetracycline hydrochloride 250-mg capsule
- Gracey (Hu-Friedy, Chicago, IL, USA) curette no. 1/2
- Scalpel handle mounted with surgical blade no. 15C
- Wide-field surgical loupes (×4.5)
- Titanium instruments for microsurgery:
- Two straight forceps
- One straight strong forceps
- One curved needle holder with lock
- One straight scissors
- P-1 needle with a 7–0 coated vicryl suture
LATERAL SLIDING FLAP
Technique
After proper anesthesia (Fig. 7.1), the tissue bordering the defect is trimmed free of sulcular epithelium with a blade no. 15 and the root(s) thoroughly planned. When there is enough gingival thickness, a partial thickness flap twice as wide as the defect is reflected beyond the mucogingival junction (Fig. 7.2). The flap is then moved laterally to cover the exposed root, leaving the donor site exposed. The latter is covered by the periosteum/connective tissue (partial thickness flap) or bare bone (full-thickness flap). The flap is then secured using 5–0 single interrupted sutures (Fig. 7.3).
It is sometimes necessary to make a short oblique releasing incision at the base of the flap to avoid any tension that may impair the vascular circulation when the flap is positioned.
Figure 7.1. Recessions on teeth 24 and 25.
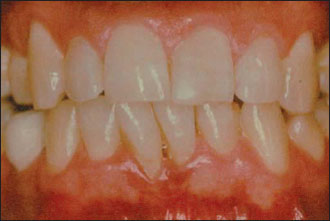
Figure 7.2. Two lateral pedicle flaps are raised adjacent to the receding areas.
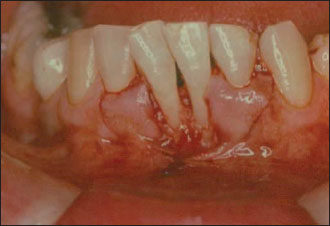
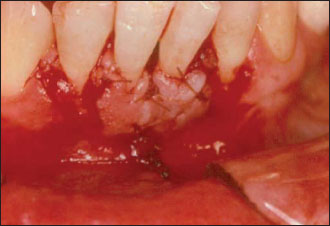
Figure 7.3. The two partial thickness lateral pedicle flaps are sutured covering the exposed root surfaces of teeth 24 and 25.
This enables the flap to lie flat and firm without excess tension at the base. Pressure is exercised on the flap with fingers and wet gauze to minimize blood clot thickness and encourage fibrinous adhesion. A periodontal dressing is applied on the wound and left in place for 1 week.
A word of caution
When operating on the lower mandible in the premolar region, take care not to injure the mental nerve. To avoid />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


