Antimicrobials in Pediatric Dentistry
Antimicrobial Classification
Microbial Target
Antimicrobial agents are often categorized according to microbial target group. The principal emphasis of this chapter is on antibacterial agents—the antibiotics. Antibiotics are considered to be either of narrow or wide spectrum. Narrow-spectrum antibiotics are effective primarily against either gram-positive or gram-negative organisms. Broad-spectrum drugs are effective against a wider range of organisms (Table 9-1).
Considerable overlap in effectiveness can exist with the broad-spectrum drugs. Efficacy against a particular microorganism is ideally determined by testing the susceptibility of the actual causative pathogen (obtained by culture) to specific antibiotics. Unfortunately, culture and susceptibility results may take 24 hours to several days and would delay initiation of antimicrobial therapy. This requires that a best guess be made for specific clinical situations as to which pathogen is most likely the causative agent and which antibiotic is usually most effective against it. This antibiotic, or combination of antibiotics, is used until culture and sensitivity results are available. Dental and periodontal infections are most commonly caused by bacteria that normally colonize the mouth, throat, and upper alimentary canal, for example, aerobic and anaerobic streptococci, Micrococcus species, anaerobic gram-negative bacteria (Bacteroides, Fusobacterium, and Veillonella species), and occasionally staphylococci or spirochetes.5 Many of these organisms are sensitive to penicillins; hence penicillins remain the single most useful class of antibiotics for dental and periodontal infections. Occasionally, dental infections are caused by aerobic gram-negative bacteria, Actinomyces, or fungi. In these cases, other antimicrobials are needed for optimal therapy.
Convenient tables listing antimicrobial treatment recommended for various medical and dental clinical syndromes and sites of infection are published and updated periodically. Nelson’s Pocket Book of Pediatric Antimicrobial Therapy2 and the Sanford Guide to Antimicrobial Therapy6 are two publications containing such guidelines. Data from local clinical microbiology laboratories can be consulted for information on local antibiotic susceptibility patterns of common pathogens.
Mode of Action
Antimicrobials may also be categorized according to their mode or site of action.8 Common modes of action for antimicrobial agents are described in Box 9-1 and as follows: (1) inhibition of synthesis of the bacterial cell wall, a structure required for bacterial survival; (2) inhibition of protein synthesis, occurring at one of several possible steps; (3) interference with folic acid metabolism, thereby inhibiting bacterial growth; (4) interference with cell membrane permeability; (5) inhibition of nucleic acid synthesis; (6) inhibition of bacterial topoisomerase enzymes; and (7) inhibition of cytochrome P-450 sterol. By these mechanisms of action, the antimicrobial agents produce toxic effects that selectively interfere with the life cycle of the microbial agent while minimizing significant alterations in the cells of the human host.
Bactericidal Versus Bacteriostatic Antibiotics
Antibiotics may also be classified as bactericidal or bacteriostatic. Bactericidal antibiotics actually kill the microorganisms, whereas bacteriostatic antimicrobials inhibit bacterial growth or multiplication and depend on the normal host defense mechanisms (immune system) to eliminate the microorganism. The same antibiotic may be bactericidal for some pathogens but bacteriostatic for others, or the activity may be concentration dependent. Bactericidal agents are preferable in most situations. Bacteriostatic agents should be avoided if possible in immunocompromised patients, because a compromised immune system may be unable to facilitate clearance of the offending microorganisms. Box 9-2 lists the agents in these categories.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


 Outline
Outline TABLE 9-1
TABLE 9-1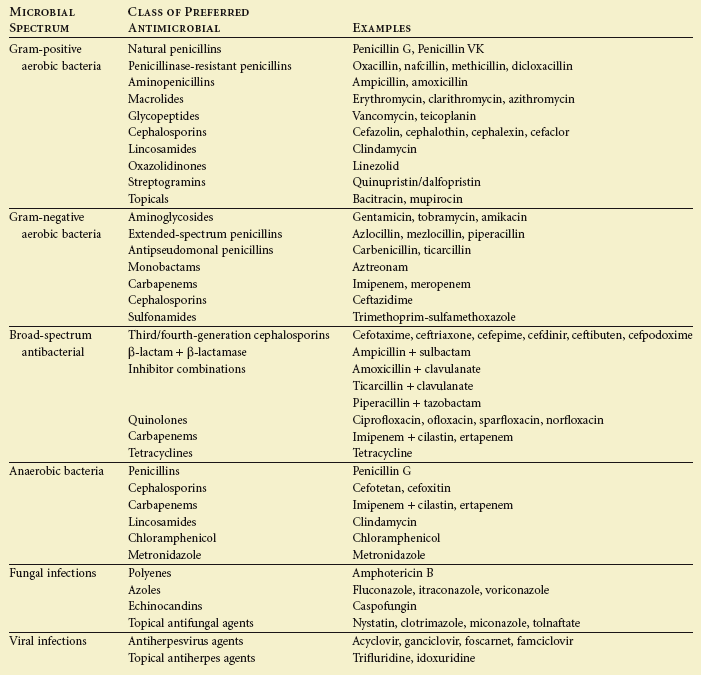
 Box 9-1
Box 9-1 Box 9-2
Box 9-2