Chapter 8
Sedation in Special Circumstances
Aim
The aim of this chapter is to describe the impact of medical conditions on sedation in dental practice and to discuss the recognition and management of failed sedation.
Outcome
After reading this chapter you should have an understanding of the medical conditions for which sedation is indicated and contraindicated in general dental practice and other primary dental care settings.
Introduction
Whilst simple dental sedation techniques are appropriate, safe and successful for the majority of fit and cooperative patients, it is important to recognise that some individuals (medically compromised patients, special care patients, paediatric patients) present special problems. This may require a more flexible approach involving management tailored to the particular needs of the individual. Sedation in these circumstances is usually best provided in a specialist centre by practitioners with appropriate training and experience.
Medically Compromised Patients
Not all medical conditions compromise the dental care of patients, but all have an impact on their daily lives. Only those common disorders which might influence sedation will be discussed. The most important of these are those relating to the cardiovascular and respiratory systems, although some musculoskeletal disorders are also significant. It is important to appreciate that, in many cases, it is positively helpful to prescribe sedation, whereas, in others, sedation techniques may require modification. The administration of supplemental oxygen may be indicated in the management of many of these patients.
Conditions in which sedation is beneficial
Sedation is almost certainly beneficial in conditions such as angina, hypertension, asthma, epilepsy and movement disorders.
Angina: Angina may be provoked by anxiety or stress before, during and even after a dental procedure. This often causes tachycardia and increases the work of the heart which may result in the characteristic ischaemic pain of angina. In addition to careful and sensitive patient management, including effective local anaesthesia, the provision of sedation further protects the patient from the effects of stress and so significantly reduces the likelihood of an angina attack.
When considering whether to sedate a patient who suffers from angina in a primary care setting, it is important to differentiate between controlled (stable) angina and uncontrolled (unstable) angina. The former is not usually a contraindication to the use of conscious sedation whereas patients with unstable angina should only be treated in specialist centres.
The emergency management of an angina attack during sedation is no different from that provided for a patient being treated under local anaesthesia alone. It is sometimes appropriate to ask the patient to use their routine rescue medication – for example, glyceryl trinitrate, immediately before the start of treatment (Fig 8-1).
Fig 8-1 Glyceryl trinitrate spray.
Hypertension: Most patients with diagnosed high blood pressure take medication but control may not always be optimal. There are also many patients with hypertension who are undiagnosed and so blood pressure measurement at the assessment visit is essential. It is generally accepted that a persistent diastolic blood pressure in excess of 110 mmHg represents a contraindication to the use of sedation in other than a specialist centre. Remember that blood pressure tends to increase with age and should be reassessed periodically.
Anxiety brought on by the prospect of dental treatment can cause an increase in heart rate and elevation of blood pressure in hypertensive patients. Sedation modifies these responses and protects the patient against sudden changes in blood pressure which can, in extreme cases, precipitate more serious cardiovascular events – for example, cerebrovascular accidents (CVA) or angina. Note that patients with low blood pressure are likely to suffer postural hypotension following sedation.
Asthma: Asthma appears to be an increasing problem within the population at large. Well-controlled asthma is not a contraindication to the use of sedation. Where asthma is poorly controlled, even with medication (brittle asthma), great care must be exercised. Sedation may be helpful, but a detailed assessment of the patient on each day of treatment is essential as asthma is notoriously labile.
Emergency management of an asthma attack during sedation is similar to that necessary for a patient being treated under local anaesthesia. But increased attention must be paid to respiratory function, in particular, if a respiratory depressant drug, such as midazolam, is in use. Rescue treatment usually involves oxygen therapy, inhaling salbutamol (Fig 8-2) and possibly steroids and attention to the positioning of the patient (Fig 8-3). As with angina, it is sometimes appropriate to ask the patient to use their routine rescue medication immediately prior to treatment. Severe (brittle) asthmatics are at risk and must be managed by a specialist team.
Fig 8-2 Salbutamol inhaler.
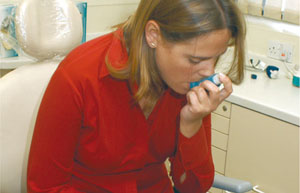
Fig 8-3 Asthma: patient positioned to aid breathing.
Epilepsy: Grand mal epilepsy is often associated with other neurological disorders and in syndromes associated with learning disability. In assessing the advisability of using sedation in a person with epilepsy, the frequency of seizures is probably the most useful index of the severity of the condition. Patients with well-controlled epilepsy usually present few problems, whereas the uncontrolled or poorly controlled patient must be referred for specialist care.
Antiepileptic drugs all depress the central nervous system. As such, they may interact with central nervous system depressant sedation agents. The outcome may be either tolerance to, or potentiation of the sedative effect. Practically speaking, this often produces unpredictable over- or undersedation and a shortened period of effective anxiolysis. Nonetheless, intravenous midazolam usually provides excellent sedation and also reduces the risk of stress-induced seizures.
Emergency supportive management of a patient who fits under sedation is no different from normal. Flumazenil should not be used unless there is also profound respiratory depression or apnoea which cannot be treated with intermittent positive pressure ventilation with oxygen.
Movement disorders: In patients with uncontrolled movements or spasticity, intravenous benzodiazepine sedation will often reduce or suppress excess activity, making treatment easier for both the dentist and the patient.
Conditions where the technique might require modification
Modification of the sedation technique might be required in conditions such as myocardial infarction, heart failure, anaemia, chronic obstructive pulmonary disease, diabetes mellitus and pregnancy.
Myocardial infarction: A patient who has had a myocardial infarct should not receive elective dental treatment under intravenous sedation until at least six months after the heart attack. Nitrous oxide may provide a suitable alternative. A patient whose cardiac condition remains unstable must only be sedated by an appropriately experienced sedationist. Supplemental oxygen through nasal cannulae is mandatory in such cases (Fig 8-4).
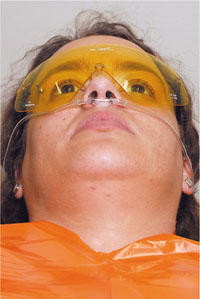
Fig 8-4 Supplemental oxygen via nasal cannulae.
Heart failure: This may be due to right or left ventricular failure. In either case, there may be respiratory distress if the patient is treated in the supine position. Careful questioning of the patient about their sleeping position may serve as a guide for positioning the dental chair. A compromise must be made between the aggravation of dyspnoea and postural hypotension. Liver perfusion may be reduced and drug metabolism therefore delayed. This could result in prolonged recovery from those sedative drugs which undergo metabolism in the liver – for example, midazolam.
Anaemia: Individuals with anaemia are at increased risk of hypoxia because of reduction in oxygen/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


